Lung cancer is an aggressive disease with projections estimating that more than 150,000 Americans will die in 2018 from lung cancer [1]. Mortality is associated with advanced stage of disease and metastatic disease. While the major sites of metastases are the solid organs, the rate of soft tissue metastases has been reported as 0.75-9% [2]. In an asymptomatic patient who is a nonsmoker, there is low likelihood to diagnose early lung cancer unless found incidentally. We present a case of a 66-year-old male non-smoker who presented emergently with recurrent syncopal episodes and dyspnea. Work up revealed long standing chronic lytic soft-tissue mass eroding into the right zygomatic arch and large left pleural effusion with mediastinal shift. Cytology of the fluid was positive for adenocarcinoma and repeat CT scan after drainage showed multiple left lung nodules. Biopsy confirmed lung adenocarcinoma and metastatic adenocarcinoma in the facial mass. Soft tissues remain a notable site for metastases of non-small cell lung cancers and typically confer poor prognosis. This case demonstrates an elusive yet daunting presentation of an otherwise typically indolent disease. Our case posits that for those patients without indication for lung cancer screening, lung cancer may appear as a set of benign-appearing symptoms, further emphasizing the importance of a diligent workup.
We present a 66-year-old non-smoking male with history of ischemic heart disease treated with cardiac stent and Prasugrel who presented emergently in respiratory distress. He stated that since a recent syncopal fall he had experienced worsening dyspnea. Of note, the patient had subtle but noticeable right cheek swelling which was evaluated earlier and was diagnosed as "glandular problem" not warranting further workup at that time.
While being assessed, the patient had an episode of symptomatic bradycardia that quickly progressed to hypotension and altered mental status. He was subsequently intubated. Chest CT revealed a massive left-sided pleural effusion displacing the mediastinum to the right and head CT was significant for a lytic soft-tissue mass eroding the right zygomatic arch (Figure 1). A chest tube was placed, and 3.5 liters of old bloody fluid were drained with subsequent hemodynamic improvement.
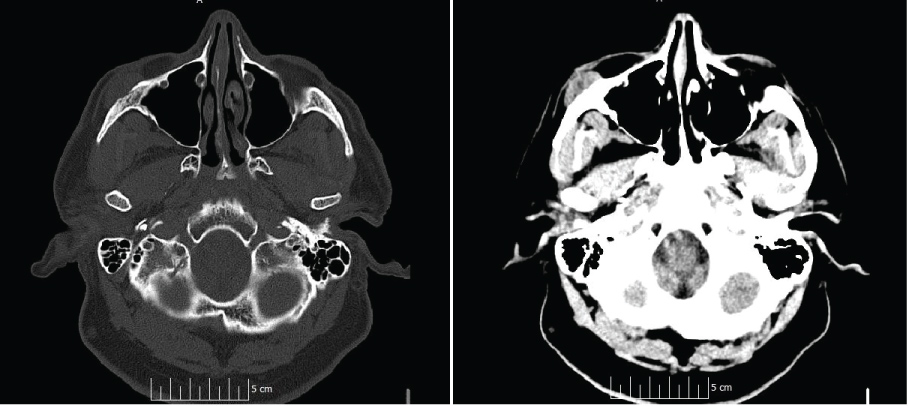 Figure 1: Non-contrast CT images of metastatic facial lesion involving the right zygomatic arch; note the erosion of the lesion into periosteal layer. View Figure 1
Figure 1: Non-contrast CT images of metastatic facial lesion involving the right zygomatic arch; note the erosion of the lesion into periosteal layer. View Figure 1
Cytologic analysis of the bloody effluent revealed atypical cells suspicious for adenocarcinoma. Repeat CT chest showed multiple nodules in the left lung, which were biopsied and found to be adenocarcinoma (Figure 2). The facial lesion was also biopsied and was positive for adenocarcinoma with similar markers found on the lung specimen. Diagnosis of stage IV adenocarcinoma of the lung was made.
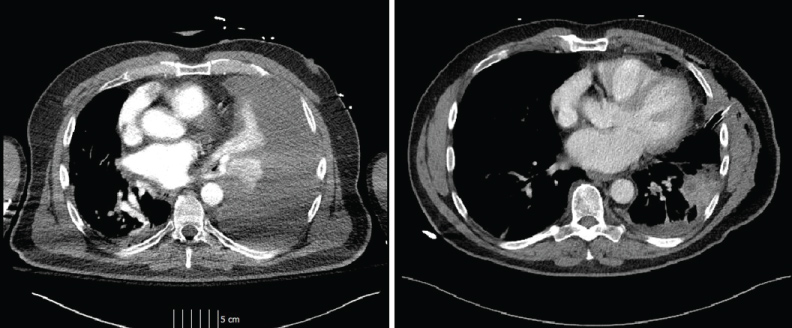 Figure 2: Comparative CT images demonstrating the massive pleural effusion obscuring the tumor and post-drainage where the tumor can be seen in the superior segment of the left lower lobe. View Figure 2
Figure 2: Comparative CT images demonstrating the massive pleural effusion obscuring the tumor and post-drainage where the tumor can be seen in the superior segment of the left lower lobe. View Figure 2
A great deal of focus has been put on screening for lung cancer in smokers, whereas lung cancer in a non-smoking patient, who does not otherwise meet indications for low-dose CT screening may go undiagnosed or present late in the course of the disease. A new finding of a palpable mass or local symptoms such as focal pain in a patient with known lung cancer should raise the suspicion for soft tissue metastasis. In a patient with unknown diagnosis, a soft tissue mass should not be disregarded as an incidental finding. In our case, a grossly benign-appearing lesion may have held the key to diagnosis many months prior to this presentation.
Nearly half of newly diagnosed cases of lung cancer are metastatic at the time of presentation [3]. Cases of lung cancer metastasizing to the soft tissues including skeletal muscle, subcutaneous tissue, and skin are rare [2]. Our report is the first to cite metastatic adenocarcinoma of the lung as a lytic lesion of the zygomatic arch. Our patient, a nonsmoker, also presented in an unusual way: symptomatic bradycardia with cardiovascular collapse prompting urgent work up, including head CT, which drew attention to the destructive nature of an otherwise subtle-appearing facial lesion. Soft tissue masses may not raise initial suspicion unless they are symptomatic (i.e., causing mass effect or local destruction). An incidental facial soft tissue mass, especially in a nonsmoker, would otherwise appear a benign finding.
Next to carcinoma of the lung, carcinomas of the kidney and colon are the most commonly implicated precursors of clinically evident soft tissue metastases [2]. Historically, the presence of cutaneous or soft tissue metastases, confers a particularly poor prognosis. The discovery of metastases to skeletal muscle from a primary non-small cell lung cancer was associated with a mean survival time of 5.6 months [4]. Even following surgical resection, a single metastatic interosseous lesion of the lower limb conferred survival of two years, whereas cutaneous lesions conferred median survival of only 2-4 months [2]. The risk for extra-thoracic metastasis has also been demonstrated to be significantly higher for patients with adenocarcinoma or large-cell lung carcinoma versus squamous cell lung cancer [5].
Taking note of the evidence outlined in the literature, soft tissue metastases from lung cancer remain rare. Still, the incidental finding of a destructive lesion on CT scan in combination with newly diagnosed lung nodules should merit a complete work up for occult malignancy. Despite the lower likelihood of a positive finding in a patient with no smoking history, a differential diagnosis of primary lung cancer cannot be dismissed without diligent investigation. This may include more definitive imaging, monitoring, and multidisciplinary consultation. The comprehensive analysis of pleural fluid, including cytologic analysis, should be completed whenever drainage is indicated. Lung cancer endures a reputation as a silent killer. In the modern era, where more genetic mutations can be targeted, and therapies are more effective than ever, a high level of suspicion is imperative, and establishing a diagnosis as early as possible remains the mainstay for therapeutic success.
Study concept & design: ZB, JP, OW; Acquisition & analysis of data: ZB, JP, OW; Drafting of manuscript: ZB, JP, OW; Critical revision & approval: OW.