(1) Describe a very specific subgroup of patients that we have termed Orphan Heel Syndrome (OHS) characterized by the clinical triad of: Diabetic chronic kidney disease (CKD), posterior tibial and peroneal arterial occlusive disease and an ischemic heel ulcer; and (2) Analyze the applicability of endovascular therapy and its clinical outcomes in a well-delineated cohort of OHS patients.
Retrospective review of 40 consecutive patients treated at the University of Arizona for full thickness diabetic heel ulcers requiring debridement between 1 January 2009 and 31 December 2011.
Over the 3-year study period, among a consecutive series of 40 diabetic heel ulcers, 12 patients (14 limbs) with typical clinical and angiographic findings of OHS were identified. The mean age of this subgroup was 68.3 ± 12.8 years and 75% (n = 9/12) were male. All patients had poorly controlled diabetes with a mean hemoglobin A1C of 9.4 ± 0.9 mg/dl and chronic kidney disease (CKD), with 75% (n = 9/12) on dialysis. Doppler waveform analysis demonstrated acceptable Anterior Tibial Artery flow, but blunted or non-existing Posterior Tibial Artery flow. Diagnostic angiography confirmed the pattern of severe posterior tibial and peroneal artery occlusive disease. All patients were poor open surgical candidates and were managed with a targeted initial endovascular approach with a technical success rate of 78.6% (n = 11/14). At a mean follow-up of 235 days (range 90-956), 50% of the patients had completely healed their wounds and two patients (14%) required major limb amputation at the below knee level.
Orphan heel are difficult to recognize via traditional noninvasive vascular testing and newer techniques to evaluate topographical perfusion warrant investigation. After endovascular-first therapy, limb salvage is acceptable, but wound-healing rates are poor despite application of advanced endovascular therapy.
Orphan heel syndrome, Peripheral artery disease, Diabetic foot, Diabetic foot ulcer, Diabetes complications, Chronic kidney disease, Ischemic heel ulcer, Gangrene, Angioplasty, Endovascular therapy
Diabetic foot ulcers are common, costly, frequently recurrent and chronic. Once infected they all too often are the precursors of major limb amputation. Increased pressure decreased angiogenic response, neuropathy, trauma and deformity all contribute in varying degrees to the pathogenesis of these ulcers. Patients with limited mobility are at higher risk of developing an even more morbid subtype of diabetic foot complication: The heel ulcer [1]. Authors have reported up to 14% prevalence of heel ulcers among patients with threatened limbs and severe ischemia requiring vascular intervention [2,3].
Heel ulcers are generally found among a sicker subset of diabetic foot ulcer patients typically characterised by poor ambulatory status, low albumin levels, high rates of gangrene, a need for revascularization with possible major limb amputation and a low 5-year survival. Conservative, non-operative management for this group using total contact casting has been plagued with substandard results [4]. Debridement and free tissue transfer with or without revascularization have been described in a number of publications with mixed results [5-8]. Additionally, primary amputation has been advocated for those with end stage renal disease or large heel ulcers (> 4 cm) [9,10].
Previously, we described an angiographic classification system for ischemic heel ulcers and proposed a management algorithm for these patients incorporating wound debridement, open revascularization and tissue transfer [7]. In that study, no patients were managed by endovascular therapy (EVT).
The introduction of EVT has greatly expanded revascularization options for patients with threatened limbs and severe ischemia who are poor surgical candidates. Despite a paradigm shift toward EVT for lower extremity peripheral artery disease (PAD), to date, reports evaluating its role in managing patients with heel ulcers are few in number [11,12].
The purpose of this study is two-fold: (1) To describe a very specific subgroup of patients with a condition that we have termed Orphan Heel Syndrome (OHS). These patients manifest the clinical triad of: Diabetic chronic kidney disease (CKD), a unique pattern of isolated heal circulation with ischemia due to Posterior Tibial and Peroneal Artery occlusive disease (lacking and collateral cross coverage from the Anterior Tibial Artery), and heel ulceration (Figure 1). (2) To examine the applicability and clinical outcomes of endovascular revascularization in OHS patients.
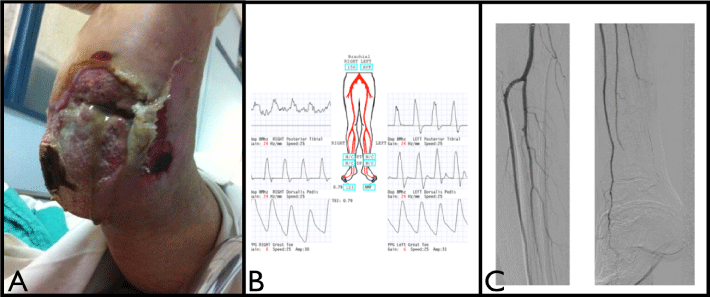 Figure 1: Clinical, non-invasive and invasive testing suggestive of an Orphan Heel Syndrome. A) Complex neuro-ischemic heel ulcer; B) Non-invasive Doppler waveform evaluation demonstrating normal Dorsalis Pedis waveforms with blunted Posterior Tibial waveforms; C) Angiography demonstrating normal forefoot perfusion with intact Anterior Tibial Artery and ischemic hind foot with occlusion of the Posterior Tibial Artery and Posterior Perforating branch of the Peroneal Artery. View Figure 1
Figure 1: Clinical, non-invasive and invasive testing suggestive of an Orphan Heel Syndrome. A) Complex neuro-ischemic heel ulcer; B) Non-invasive Doppler waveform evaluation demonstrating normal Dorsalis Pedis waveforms with blunted Posterior Tibial waveforms; C) Angiography demonstrating normal forefoot perfusion with intact Anterior Tibial Artery and ischemic hind foot with occlusion of the Posterior Tibial Artery and Posterior Perforating branch of the Peroneal Artery. View Figure 1
We performed an IRB-approved, retrospective review of all patients who presented to the Southern Arizona Limb Salvage Alliance (SALSA) clinic, at the University of Arizona Medical Center, with complex multifactorial diabetic heel ulcers from 1 January 2009 to 31 December 2011. Waiver of patient consent was authorised given the retrospective nature of our analysis that did not affect patient care or welfare. A total of 40 patients with 42 ulcers were identified. All 42-heel ulcerations were treated with standard of care including: Offloading, regular sharp debridement and clean dressing changes.
Among this cohort, 12 patients with 14 affected limbs underwent diagnostic angiography and targeted endovascular therapy. This subset was evaluated based on a complete diagnostic angiogram with run off that included magnified views of the foot in both antero-posterior and lateral projections. The OHS subgroup under review in this article was distinguished using these detailed, diagnostic angiographic studies. In many cases, due to the very low velocities, prolonged exposure in digital subtraction mode was used to verify the lack of late collateral perfusion of the heel. It is quite possible that more patients in this study were affected by a similar disease pattern and the diagnosis was missed because our recognition and evaluation of these patients evolved during the study period.
Patient variables extracted included: Age, gender, comorbidities, vascular non-invasive studies, angiographic images, endovascular revascularization technique and results, limb salvage and time to wound healing.
In this study, CKD was defined as a serum creatinine level greater than 1.5 mg/dl (GFR < 60) or as a history of chronic renal insufficiency requiring dialysis or kidney transplantation. Diabetes mellitus (DM) was defined as hemoglobin A1C > 6.5%, fasting plasma glucose level > 126 mg/dl (7.0 mmol/l), or as hyperglycemic symptoms with a random plasma glucose level > 200 mg/dl (11.1 mmol/l). Arterial insufficiency was defined as an ankle/brachial index (ABI) below 0.9 or greater than 1.3 (for patients with non-compressible arteries due to medial calcinosis), abnormal arterial waveforms or diminished pulse-volume recordings at the ankle. Technical success of endovascular intervention was defined as re-establishment of hind foot perfusion via direct in-line flow of at least 1 vessel with residual stenosis less than 30%.
Patients were followed to their last clinic appointment visit or to the time of death. Descriptive statistics were used to report data in this analysis. Data were entered into a computerised spreadsheet (Microsoft Excel 2003, Microsoft corporation, Redmond, WA) and analysed using SPSS for Mac©, version 19.0 (SPSS, Chicago, IL).
Over the 3-year study period, a total of 40 patients with 42 complex heel ulcers were identified. Of this initial group, 57% (n = 24/42) underwent diagnostic angiography. After imaging, 12 patients (14 limbs) were conclusively identified as having typical anatomic findings of OHS. The mean age of this latter subset was 68.3 ± 12.8 years, and 75% were male (n = 9/12). Comorbid conditions were common and significant. All patients exhibited long standing (mean time since diagnosis of 21 ± 13.5 years) poorly controlled diabetes with a mean hemoglobin A1C of 9.4 ± 0.9 mg/dl, and all patients had CKD with 75% (9/12) on dialysis. The mean serum albumin level was 2.8 (range 1.5-3.6) ± 0.4 g/dl.
Among the minority of patients in whom it was measurable, the mean ABI was 0.53 (range 0.21-0.96); however, 8 patients (67%) had non-compressible ankle arteries. Most of the limbs in the series (9/14) had palpable Dorsalis Pedis pulse and none had Posterior Tibial pulse, as noted by a vascular surgeon in electronic medical record notes. Those who did have measurable systolic pressure at the dorsalis pedis level had a mean systolic pressure of 126.5 ± 17.0 mmHg. On analysis of Doppler waveform patterns all 14 limbs had acceptable forefoot patterns with biphasic or pulsatile monophasic waveforms, 9 patients had blunted monophasic waveforms with little to non-diastolic progression and 5 of them had no posterior tibial waveform identifiable.
A total of 14 multilevel endovascular procedures were performed in this cohort. Diagnostic angiography revealed heterogenous distribution of hemodynamically significant occlusive disease in the Superficial Femoral Artery (36%; 5/14 legs), popliteal (14%; 2/14 legs) and anterior tibial artery (57%; 8/14 legs). All patients in the data set had both peroneal and posterior tibial vaso-occlusive disease (defined as greater than 50% stenosis or occlusion) limiting the heel perfusion without any obvious collateral late filling of calcaneal branches after prolonged exposure digital subtraction (Figure 2). The mean lesion length of the peroneal and posterior tibial was 16.4 ± 4.1 cm. The therapeutic approach for all patients is summarized in Table 1.
Table 1: Distribution of endovascular therapy amongst the OHS subgroup. View Table 1
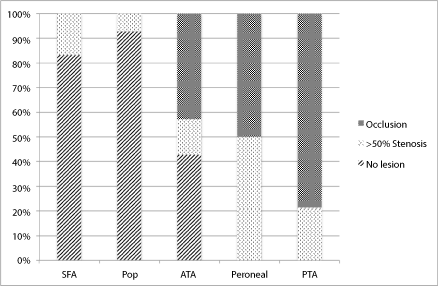 Figure 2: Pattern of disease in Orphan Heel Syndrome patients demonstrate Peroneal and Posterior Tibial Arteries predominance. View Figure 2
Figure 2: Pattern of disease in Orphan Heel Syndrome patients demonstrate Peroneal and Posterior Tibial Arteries predominance. View Figure 2
All patients in the series had successful wire passage to either the Peroneal or the Posterior Tibial Arteries. After balloon angioplasty, technical success (defined earlier as in-line flow to one of these arteries without acute elastic recoil greater than 30%) was accomplished in 78.6% (11/14). Two of the cases had failed passage of the PTA catheter, and one case had recoil greater than 30% after angioplasty-not candidate to stenting due to the extent of the lesion. Only 3 cases required concomitant proximal ilio-femoral inflow therapy, which was established using balloon angioplasty and self-expanding nitinol laser cut stents-at operators discretion. Most of the tibioperoneal therapy was accomplished by low profile (0.018''and/or 0.014'') balloon angioplasty without the need for stenting (Figure 3). Atherectomy was not used in this series. After endovascular intervention, the mean ABI improved by 0.38 (range 0.27-0.79) in those patients in whom it was measurable. All patients required wound debridement, 33.3% (4/12) required tissue transfers and 16.7% (2/12) received open surgical revascularization secondary to failed endovascular therapy.
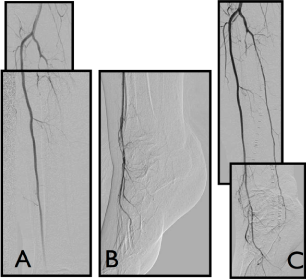 Figure 3: Successful endovascular intervention of an Orphan Heel Syndrome patient. A,B) Pre interventional image: Intact Anterior Tibial down to the foot with severely diseased Peroneal and Posterior Tibial Arteries; C) Post interventional image: Angiogram demonstrating in-line flow to the Posterior Tibial Artery status post successful endovascular therapy with balloon angioplasty. View Figure 3
Figure 3: Successful endovascular intervention of an Orphan Heel Syndrome patient. A,B) Pre interventional image: Intact Anterior Tibial down to the foot with severely diseased Peroneal and Posterior Tibial Arteries; C) Post interventional image: Angiogram demonstrating in-line flow to the Posterior Tibial Artery status post successful endovascular therapy with balloon angioplasty. View Figure 3
As of June 2014, 50% (7/14) of the OHS patients had healed, 22% (3/14) remained with intact index limbs but incompletely healed ulcers, 14% (2/14) had undergone below the knee amputation and 14% (2/14) were lost to follow up. The mean follow-up interval was 235 days (90-956 days). The range of times for complete wound healing was: 90, 103, 278, 290, 412, 465 and 956 days (mean healing time of 304 ± 294 days). Regarding those patients who specifically had technical success and adequate outpatient follow-up (with optimal wound care), the healing rate was 67% (6/9) with a mean time-to-healing of 364 ± 321 days.
The development of an ulcer over the calcaneus is a serious complication in patients with diabetes. When associated with PAD the prognosis is considered poor. Despite aggressive, multi-specialty team protocols, within 2 years nearly half of these patients will demonstrate progression of disease and require major limb amputation [13]. In the present study, a specific subgroup of heel ulcer patients with concomitant CKD, poorly diabetes and a specific anatomic pattern of regional foot ischemia were recognised, identified and characterised. For the purpose of this publication, the condition has been termed Orphan Heel Syndrome.
OHS patients had a mean hemoglobin A1C of 9.4 ± 0.9 mg/dl, mean serum albumin level of 2.8 ± 0.4 g/dl and 100% had renal failure, with 75% being dialysis-dependent. The latter combination of clinical findings has been demonstrated to be associated with such a high risk of limb loss that many authors advocate primary major amputation as the best alternative [12].
Although most patients (57%, n = 8/14) had non-compressible ankle arteries with unmeasurable ankle-brachial indexes, some had a measurable pressure at the dorsalis pedis level (35%, n = 5/14) with a mean systolic pressure of 126 ± 17.0 mmHg. Moreover, 64% (n = 9/14) of the OHS subset had readily palpable dorsalis pedis pulses. Based on the above and acceptable Anterior Tibial waveforms, most diagnostic guidelines would consider these patients to have a normal/acceptable foot perfusion.
The OHS patient population had absent posterior tibial pulses and blunted or absence of Doppler waveforms at this level. The disparity of fore and hind foot perfusion (based mainly on non-invasive waveform analysis and physical exam) supports the observation regarding vascular compartmentalization of the foot. The angiosome theory described by Taylor, et al. [14] has been extensively explained in other publication. This sub-group of patients, rather than defy the concept defines a sub-group of patients with intact forefoot angiosome perfusion, but ischemic calcaneal (medial/lateral) angiosome secondary to a series of clinical conditions that preclude angiosomal cross-coverage.
Although the angiosome theory has recently become a popular area of debate, few authors specifically address the 'choke vessel' or inter-angiosomic small caliber vascular bridges as having a role in the reason for this concept being crucial for dictating therapy (direct vs. indirect revascularization) [14,15]. These vascular bridges posses dynamic adaptability to redirect flow, which serves as the basis for maintenance of viable tissue in the presence of obstructive disease of the axial flow vessels.
Microvascular disease is an entity frequently described in patients with longstanding diabetes and advanced kidney failure [16]. The authors' hypothesis is that the clinical scenario of OHS patients negatively affects the luminal caliber and/or physiologic flow adaptability of the choke vessels hindering any potential angiosomal cross-coverage. Hence, the presence of peroneal, and to an even greater degree, posterior tibial occlusive disease, renders the heel an 'orphan' isolated from the perfusion of the rest of the foot. The heel can thus be mal-perfused even in the presence of a palpable dorsal pedal pulse and fully intact anterior tibial and dorsal pedal vessels. This hypothesis may well explain why in the published work from Azuma, et al. in relation to bypass surgery and target vessel selection, the healing rate for indirect angiosome revascularization was significantly slower than in the direct revascularization group, especially in the ESRD subgroup of patients [17].
Traditional noninvasive vascular testing falls short when it comes to assessing regional foot perfusion in the OHS subgroup of patients with heel ulcers. An assessment of whole foot perfusion based on forefoot perfusion (i.e. toe pressure) fails to detect hindfoot malperfusion. Faglia, et al. support perilesional transcutaneous oximetry of heel ulcers, as described in a recently published analysis of a solitary complex case that fits our much larger series of OHS [18]. Unfortunately, there are multiple well-known shortcomings of TcPO2, and our group favours research of newer techniques to assess regional perfusion such as indocyanine green angiography [19] or other alternatives such as bio-compatible implantable luminescent oxygen microsensors which due to their stable nature might even revolutionise surveillance protocols [20,21].
In previous work, the authors have analysed data on angiographic disease patterns of heel ulcer patients and proposed a clinical classification scheme [7]: Grade - I patent posterior tibial, grade II - occluded posterior tibial reconstituted from peroneal, grade III - occluded posterior tibial reconstituted from dorsalis pedis, grade IV - no visible reconstitution of the posterior tibial and finally grade V - avascular heel. All of OHS patients had either class IV or V grade heel ischemia.
All patients were poor surgical candidates due to comorbid medical conditions, severe frailty, lack of adequate target arteries, insufficient vein conduit or a combination of these situations. As a result, endovascular management was initially attempted in all patients, which resulted in a 78.6% technical success rate. Two of the technical failures were secondary to failure to move the angioplasty catheter into place and one patient had significant acute recoil with suboptimal in line flow patterns to the heel. In the setting of severe medial calcinosis (classically expected in the CKD/advanced diabetes patient subgroup), technical success rate was found to be reasonable. Moreover, the fact that failure to achieve optimal flow was related to recoil or failure of device delivery, and not failure of wire passage; leaves room for improvement as technology for effective tibial intervention is being constantly miniaturised and new debulking tools are a work in progress.
In general terms this specific subset of patients displays poor, extremely delayed wound healing. By the end of our review the ideal subgroup of patients with successful revascularization and adequate outpatient follow up resulted in a healing rate of 67% (6/9) and a mean time-to-heal of 364 ± 321 days. Additionally, two patients required a major below the knee amputation. Other authors describe positive predictors of healing as including normal renal function, palpable pedal pulses and patent posterior tibial arteries past the ankle [22]; unfortunately, all of these conditions are not shared by this particular subgroup. However, in view of our results, our group advocates aggressive revascularization attempts and optimal local management rather than a more radical stand of primary major amputation. Earlier recognition and revascularization when the wound is still small and not infected [23], may also lead to better outcomes. Moreover, due to the limited number of patients involved in this study, no interventional aspect of nonsurgical wound care showed greater efficacy than any other within the OHS subgroup.
Orphan heel syndrome is a condition characterised by the triad of heel ulceration, diabetic end stage renal disease, and an avascular heel due to compartmentalised foot circulation with an isolated heel due to posterior tibial and peroneal occlusive disease, pedal arch disease, and most likely disease progression into choke vessels. In this specific cohort of patients, classic noninvasive vascular testing often fails to detect ischemia, warranting a higher index of suspicion and novel techniques to evaluate topographical foot perfusion. Incorporation of endovascular therapy into management protocols results in acceptable limb salvage and wound healing rates. It is the author's opinion that OHS is not recognised until a wound has reached a late stage of development, delaying attempts at timely intervention. Many patients with heel ulcer and palpable Dorsalis Pedis pulses or normal ABIs never trigger a specialist consultation. Awareness of OHS amongst primary care doctors, nephrologists and other specialists who deal with vascular patients should be raised in the hope that greater familiarity might lead to focused preventive efforts, earlier recognition and more prompt referral to a vascular and endovascular surgery service.
MM, JMiller researched data. MM, JMills, JMiller wrote manuscript. KG, JMills, DA. BB reviewed/edited manuscript.
This research was previously presented at the 28th annual meeting of the Western Vascular Society as a full presentation on September 24th, 2013.