Vitamin D has immunomodulatory properties. Most of the evidence points towards a causal association between low vitamin D levels and the development of asthma and allergy but the results are not conclusive. We studied the vitamin D levels of patients with anaphylaxis and compared them to previously published vitamin D levels in the Saudi population.
This was a retrospective study of patients presenting with anaphylaxis in a large tertiary care hospital in Riyadh, Saudi Arabia. The study included all patients given new adrenaline auto injector (AAs) prescriptions for anaphylaxis for two years. Their medical records were screened for diagnosis of asthma and vitamin D levels.
A total of 238 patients were identified. The mean age was 22.9 years, (2 years to 73 years) SD +/- 18.2. Male to female ratio was 48:52 and 54% of the patients were 18 or older.
Vitamin D data was available for 121 of those patients. Of these, 84 patients also had asthma. There was no difference in vitamin D levels between those with or without asthma presenting with anaphylaxis. There was a lower incidence of vitamin D deficiency in patients with anaphylaxis compared with the general population; patients who presented with anaphylaxis had a higher chance of having a normal vitamin D level compared to the general Saudi population.
There was no difference in vitamin D levels in patients with or without asthma who presented with anaphylaxis. Vitamin D deficiency was not found to be a significant risk factor for anaphylaxis in our patients but there was a higher chance for them to have normal vitamin D level when compared to the general Saudi population.
Vitamin D, Anaphylaxis, Asthma
Anaphylaxis is a serious allergic reaction that is rapid in onset and may cause death [1]. Anaphylaxis is highly likely when any one of the following three criteria is fulfilled:
1. Acute onset of an illness (minutes to hours) with involvement of the skin and/or mucosal tissue and respiratory compromise and/or reduced blood pressure.
2. Symptoms involving two or more organ systems (skin/mucosal, respiratory, cardiovascular, GI) that occur rapidly after exposure to a likely allergen for that patient.
3. Reduced blood pressure following exposure to a known allergen for that patient.
Anaphylactic reactions can be triggered by allergic responses to a wide range of substances including food, medications, insect stings and latex. Lifetime prevalence of anaphylaxis is up to 2% with the most cases being reported among children and adolescents [2]. Anaphylaxis occurs in 30 per 100,000 people annually in the United States with a reported mortality of 1-2% [3]. The rate of occurrence is increasing in industrialized countries [4]. The incidence and prevalence of anaphylaxis in Saudi Arabia is unknown.
Vitamin D deficiency is a global public health problem. Asthma and allergic disorders including anaphylaxis are also a major worldwide public health concern. The prevalence of hypovitaminosis D is significantly higher among the Saudi population [5]. Vitamin D regulates more than 200 human genes in a wide variety of tissues [6]. Aside from skeletal health, vitamin D has been associated with various cancers and autoimmune disorders [7]. There is also evidence for its role in the development and maintenance of lung structure and function [8-10]. This association with immune and airway function provides the basis for the hypothesis that vitamin D may have direct links with asthma and allergic disease [11,12].
Most of the evidence points towards a causal relationship between low vitamin D levels and the development of asthma and allergies but the results are not conclusive [13]. More studies are needed to understand the role of vitamin D in the pathogenesis of anaphylaxis and other allergic diseases. It is important to study the patterns of anaphylaxis in different geographical regions as well as to see if any causal factors can be identified which may help in understanding its pathogenesis.
This will ultimately help us understand various aspects of anaphylaxis and aid ongoing efforts to reduce morbidity and mortality associated with it. It could also provide important clues for its primary prevention [2]. The global agenda for anaphylaxis research according to the World Allergy Organization anaphylaxis guidelines also stresses the importance of research in anaphylaxis [14]. Similar work looking at the role of vitamin D in anaphylaxis, asthma and allergies has already been published from other parts of the world [15,16].
The aim of the study was to analyze the vitamin D levels of patients who presented to our hospital with anaphylaxis with or without a history of asthma and to compare them to previously published vitamin D levels in the Saudi population. The vitamin D levels were also correlated with the diagnosis of asthma.
All patients given new prescriptions of AAs at our hospital for two years were included in this study. Patients prescribed AAs were identified using the hospital pharmacy database and the case records of these patients were retrospectively reviewed. Clinical data was collected using a standardized form that included information on demographics and indications for AA prescriptions. Vitamin D levels were classified as ranging from severe deficiency (less than 25 nmol/liter), moderate deficiency (25-49 nmol/liter), mild deficiency (50-74 nmol/liter), optimum level (75-250 nmol/liter) and toxic (more than 250 nmol/liter). Moreover, 25(OH) D levels were performed by high-performance liquid chromatography (HPLC) assay, as previously described [17].
The data was sub-classified by age, gender, and nationality, as well as by geographical location within the Kingdom of Saudi Arabia.
Data analysis was performed using SPSS (Statistical Package for Social Sciences) version 12.0 for Windows (SPSS, Inc., Chicago, IL) and R version 3.3.2 for Windows (The R Foundation, Vienna, Austria).
Cochran Armitage Trend test, two-sample Z-test, Welch two-sample T-test, and Fisher's exact test were used for analysis.
The protocol was approved by the Research Advisory Committee of the hospital.
This was a retrospective review of our hospital records which did not require any intervention, device or patient interaction and presented no risk to patients. All patients who had received AAs during the study period outlined above were reviewed for descriptive data such as age, gender, and indications. Patients were not contacted during the duration of the chart review. All the data collected was anonymous and patient identifiers such as medical record number and date of birth were deleted once the data was analysed using SPSS and R. Only the principal investigator (PI) had access to the complete data; other co-investigators did not store the data but passed it on to the PI for analyses and filing in SPSS and R.
This study looked at 238 new patients who were prescribed AAs over a period of two years (Table 1).
The mean age at the time of first AA prescription was 22.9 years, (2 years to 73 years) SD +/- 18.2 years.
Female to male ratio was 52: 48 and 54% of the subjects were more than 18 years of age. Most of these prescriptions were given to Saudi patients mainly from the Riyadh area but also from other parts of the Kingdom. However, about 18% were given to non-Saudis living in the Riyadh region. Most of these were employees of the hospital or their dependents. The signs, symptoms and triggers of anaphylaxis from these patients have already been described previously [18].
A two-sample Z-test showed that there was a statistically significant difference in the proportion of Vitamin D Deficiency occurrence between patients presenting with anaphylaxis and the general Saudi population. Patients presenting with anaphylaxis were more likely to have a normal vitamin D level or mild Vitamin D deficiency, whereas the general Saudi population had a higher chance to have moderate to severe Vitamin D deficiency, compared with patients who presented with anaphylaxis. (Figure 1 and Figure 2) This data is also shown as Supplementary Table 1 and Supplementary Table 2 p = 0.047.
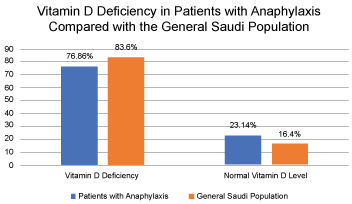 Figure 1: Vitamin D deficiency in patients with anaphylaxis compared with the general Saudi population.
View Figure 1
Figure 1: Vitamin D deficiency in patients with anaphylaxis compared with the general Saudi population.
View Figure 1
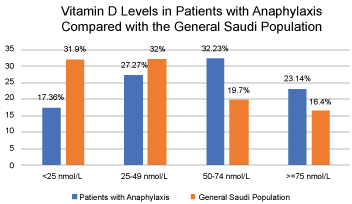 Figure 2: Vitamin D levels in patients with anaphylaxis compared with the general Saudi population.
View Figure 2
Figure 2: Vitamin D levels in patients with anaphylaxis compared with the general Saudi population.
View Figure 2
Supplementary Table 1: Vitamin D deficiency and normal vitamin D level occurrence between patients presenting with anaphylaxis and the general Saudi population. View Supplementary Table 1
Supplementary Table 2: Saudi population had a higher chance to have moderate to severe Vitamin D deficiency, compared with patients who presented with anaphylaxis. View Supplementary Table 2
Despite the apparent differences in the medians, there was no significant difference in the mean vitamin D levels between patients with different asthma severities who presented with anaphylaxis (p = 0.1382) (Figure 3).
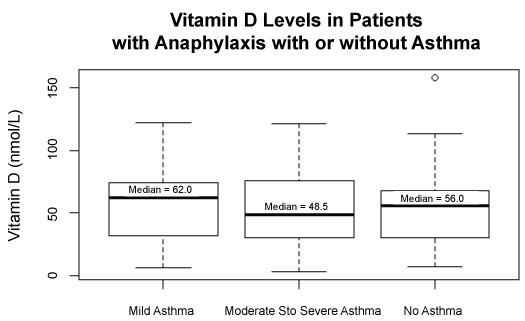 Figure 3: Vitamin D levels in patients with anaphylaxis with or without asthma. One-way analysis of Vitamin D by asthma. View Figure 3
Figure 3: Vitamin D levels in patients with anaphylaxis with or without asthma. One-way analysis of Vitamin D by asthma. View Figure 3
Table 1: Characteristics of these demographics. View Table 1
There was no evidence of a difference in the mean vitamin D levels of males and females (p = 0.1648), presenting with anaphylaxis, despite the difference in medians (Figure 4).
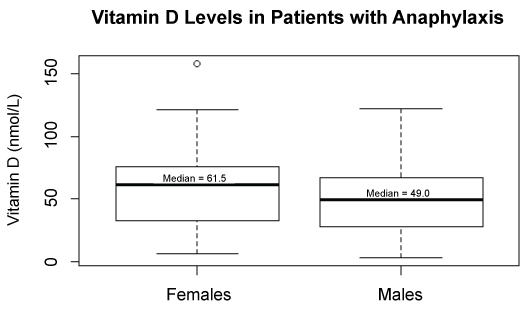 Figure 4: Vitamin D levels in patients with anaphylaxis between females and males. View Figure 4
Figure 4: Vitamin D levels in patients with anaphylaxis between females and males. View Figure 4
There was a significant difference in medians but it did not translate into a statistically significant difference in the means (p = 0.1426) (Figure 5).
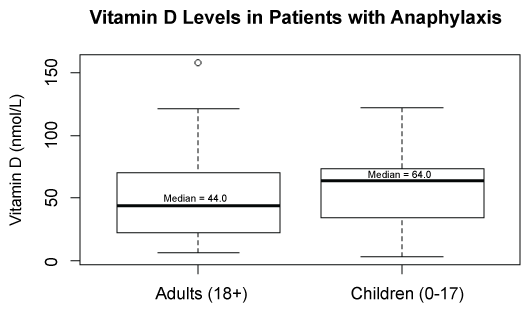 Figure 5: Vitamin D levels in patients with anaphylaxis between adults and children. View Figure 5
Figure 5: Vitamin D levels in patients with anaphylaxis between adults and children. View Figure 5
64.7% of patients presenting with anaphylaxis, were tested for vitamin D deficiency before getting an AA prescription, and 35.3% were tested for vitamin D deficiency after getting an AA prescription. Of those tested before getting an AA prescription, 79.4% were vitamin D deficient (Figure 6).
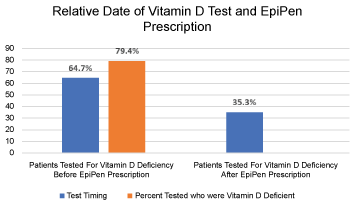 Figure 6: Relative date of Vitamin D Test and EpiPen Prescription. View Figure 6
Figure 6: Relative date of Vitamin D Test and EpiPen Prescription. View Figure 6
A possible role of vitamin D in anaphylaxis, allergies and asthma is being reported from many areas around the world. It is also observed that the incidence of allergies and anaphylaxis is on the rise. It is therefore important to understand more about this life-threatening condition in our region.
There are numerous studies which indicate that there may be an association between low vitamin D levels and anaphylaxis, allergies and asthma [19-21]. While there are other studies that have not found any association between vitamin D and atopy or asthma [15]. Taking together the available literature, it is not yet possible to confirm or refute the direct role of vitamin D in the development/worsening of allergic diseases, or to assign a role to Vitamin D use in an immunological therapy setting [2].
Our data showed that the mean age at the time of the first AA prescription was 22.9 years. This may be higher than populations in the west. No clear-cut explanation was available for this observation. It is possible that the patients presented late to a tertiary care hospital where AA prescriptions are available.
Even though vitamin D deficiency is quite common in Saudi Arabia, it is interesting to note that the patients who presented with anaphylaxis were less likely to have vitamin D deficiency. Since vitamin D is also available over the counter, it is difficult to know the exact usage pattern for vitamin D among patients who may not have reported if they had been taking it. However, vitamin D deficiency does not seem to be causally related to the development of anaphylaxis in the Saudi population, as the general Saudi population has a higher chance of moderate to severe vitamin D deficiency.
Our data did not show any significant difference in vitamin D levels between those with or without asthma who presented with anaphylaxis. This also strengthens our observation that Vitamin D deficiency may not be causally related even in patient populations who may be prone to more than one diseases with underlying allergic pathogenesis.
Similarly, no significant difference was observed in the Vitamin D levels in males vs. females or adults vs. children.
Even though, 64.7% patients had Vitamin D level checked before requiring an AA prescription and 79.4% of them had Vitamin D deficiency, it is difficult to draw any conclusions from them, as overall, the general Saudi population had a higher chance of having Vitamin D deficiency.
There was no difference in vitamin D levels in patients with or without asthma who presented with anaphylaxis. When compared with the general population, patients with anaphylaxis have more chance to have a normal vitamin D level. Vitamin D deficiency was not found to be a significant risk factor for anaphylaxis in our patients compared with the general Saudi population.
The only approved indication for AAs is anaphylaxis. It is only available at a few centers in Saudi Arabia. In a large tertiary care hospital, it should provide us with a good estimate of the anaphylaxis patterns in our population. However, as the AAs are also available at a few other hospitals in the country, we may not be able to completely ascertain vitamin D levels or their role in anaphylaxis in our region.
It is assumed that the vitamin D consumption level would be similar between patients with anaphylaxis and the general Saudi population, however the conclusion that vitamin D was normal in majority patients with anaphylaxis should be interpreted with caution as the exact vitamin D supplementations are unknown in patients with anaphylaxis.
The authors declare no competing financial interests.