Endoscopic decompression has been recently suggested as the first line treatment of ureterocele in children, including laser transurethral incision. We report a case of a unique but very serious complication after simple ureterocele puncture using a holmium laser in an infant. A 6-week-old male with a history of laser treatment of right simple ureterocele (procedure performed at the other institution 2 days earlier) was admitted because of sepsis. Imaging studies revealed urine leak around the bladder. Destroyed right bladder wall with perforation (locally coagulated and buried tissue) and damaged distal part of the right ureter along the distance of 3-4 cm were found during cystoscopy and laparotomy. Bladder was closed wall after removal of damaged tissues and then end right ureterocutaneostomy was done. The presented case shows that one has to be very careful using new techniques for endoscopic treatment, especially in very young patients and complications may overweight the advantages.
Ureterocele, Laser therapy, Endoscopic incision, Children.
General principles of ureterocele management in children have evolved in recent years. Endoscopic puncture/incision is currently suggested as the first line treatment for ureteroceles, especially those associated with single system and intravesical ureteroceles. The timing of endoscopic intervention toward earlier periods has been noted [1-8]. Recently transurethral laser incision of ureterocele has been proposed as a safe and efficacious option [9-11]. The aim of this report is to present a unique but very serious complication after ureterocele puncture using a holmium laser in an infant.
A 6-week-old male after laser incision of a simple right ureterocele performed at the other hospital two days before admission to our institution, was admitted because of general bad condition and signs and symptoms of sepsis. Endoscopic incision was done as an outpatient procedure and a boy was discharged home immediately after cystoscopy.
Ultrasound (US) showed mild distention of the right collecting system and upper part of the right ureter and fluid collection around the bladder. The results of Voiding Cystourethrography (VCUG) suggested contrast leak localized paravesically (Figure 1). Computed Tomographic Urography (CTU) showed dilatation of the right collecting system, only partially visible right ureter and contrast leak from its distal end above the bladder (Figure 2a and Figure 2b).
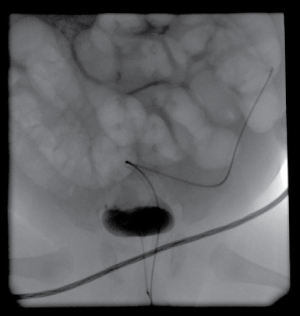 Figure 1: Voiding cystourethrography: contrast leak around the bladder on the right side. View Figure 1
Figure 1: Voiding cystourethrography: contrast leak around the bladder on the right side. View Figure 1
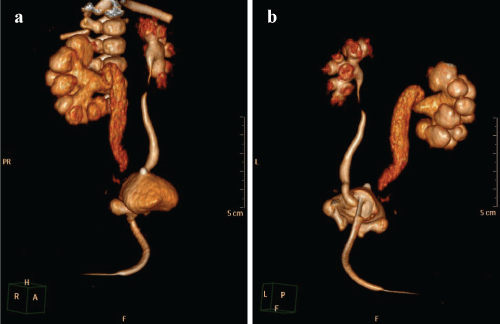 Figure 2: a) Computed tomographic urography; b) Dilatation of the right collecting system, no visible distal part of the right ureter, contrast leak at the end of the right ureter. View Figure 2
Figure 2: a) Computed tomographic urography; b) Dilatation of the right collecting system, no visible distal part of the right ureter, contrast leak at the end of the right ureter. View Figure 2
Cystoscopy revealed necrotic right bladder wall (Figure 3a and Figure 3b). During laparotomy completely destroyed bladder wall on the right side with perforation (locally coagulated and buried tissues) together with damage of the distal 3-4 cm of the right ureter was found. Healthy appearing ureter was present 4-5 cm above the bladder. Also, anterior wall of the rectum was involved, but without perforation (Figure 4a, Figure 4b and Figure 4c). After removal of damaged tissues the bladder was closed in layers and finally end right ureterocutaneostomy was done.
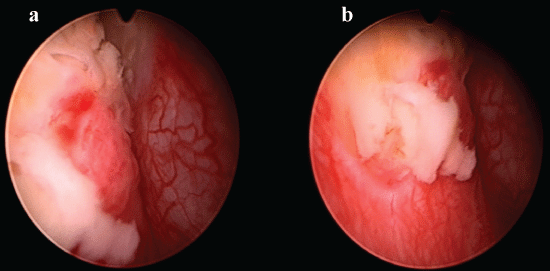 Figure 3: Cystoscopy: necrotic right bladder wall. View Figure 3
Figure 3: Cystoscopy: necrotic right bladder wall. View Figure 3
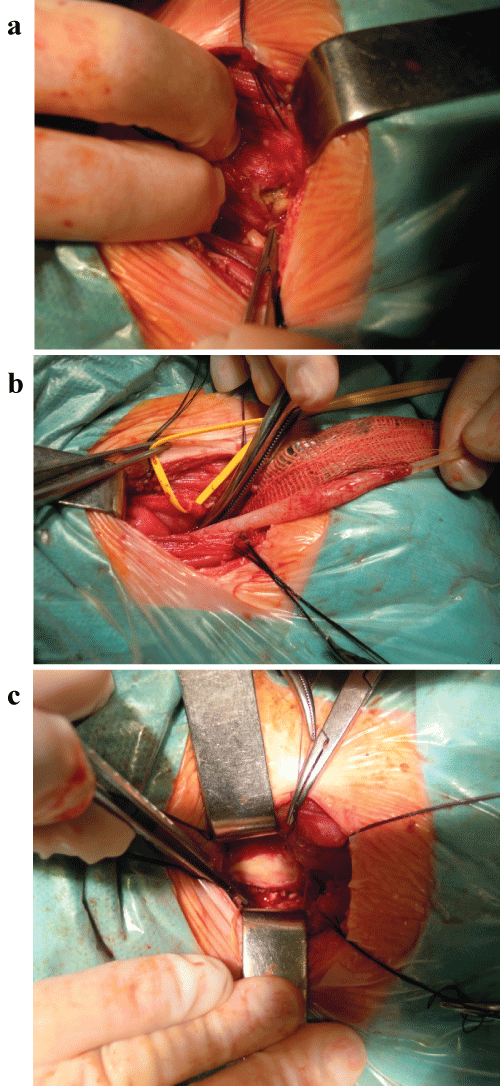 Figure 4: a) Intraoperative view: destroyed bladder wall on the right side with perforation; b) Intraoperative view: damaged distal part of the right ureter, healthy appearing ureter 4-5 cm above the bladder; c) Intraoperative view: buried anterior wall of the rectum. View Figure 4
Figure 4: a) Intraoperative view: destroyed bladder wall on the right side with perforation; b) Intraoperative view: damaged distal part of the right ureter, healthy appearing ureter 4-5 cm above the bladder; c) Intraoperative view: buried anterior wall of the rectum. View Figure 4
Immediate postoperative period was uneventful. Control CTU showed no urinary tract leak. Radionuclide examination showed right renal parenchyma scarring with slightly diminished function (45% ERPF). Recurrent Urinary Tract Infections (UTI) were observed during first two months together with progressing stenosis of cutaneous orifice of end ureterocutaneostomy (Figure 5). This stenosis required reoperation with further excision of distal part of scarred ureter and more proximal localization of stomy (Figure 6).
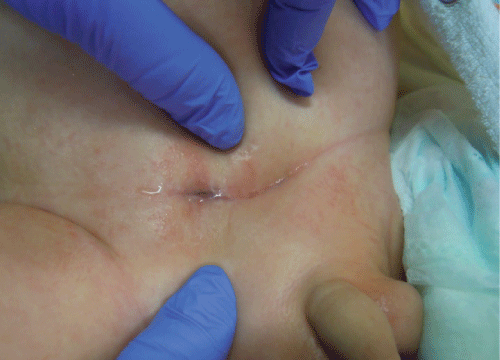 Figure 5: Stenosis of cutaneous orifice of the end ureterocutaneostomy. View Figure 5
Figure 5: Stenosis of cutaneous orifice of the end ureterocutaneostomy. View Figure 5
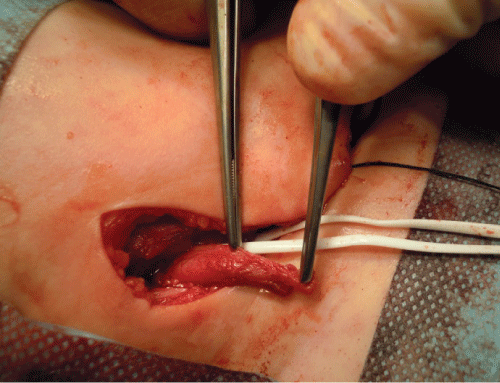 Figure 6: Intraoperative view: scarred distal part of the ureter. View Figure 6
Figure 6: Intraoperative view: scarred distal part of the ureter. View Figure 6
Good function of the ureterostomy, no dilatation of the right collecting system and no UTIs were noted during almost 4 years observation.
Several techniques for endoscopic ureterocele decompression in children have been previously used, including incision with electrocautery, cold knife incision, puncture with a stylet [3,4,8,10]. Regardless the technique used, the only encountered and described complication, was new-onset Vesicoureteral Reflux (VUR) into the punctured system. Reported rates of postoperative VUR ranged from 18 to 27% [1-4,6,8].
The use of holmium: YAG laser to incise ureterocele has been proposed in older children and also in neonates [9-11]. Also, fetoscopic laser surgery to decompress ureterocele prenatally is reported [12-15]. Up to date the largest series of laser treatment of ureterocele using holmium: YAG laser in neonates, including 8 cases, was published in 2015. No intraoperative complications were observed [11].
All authors who presented the results of laser ureterocele treatment in children underline the advantages of laser procedures. They conclude that holmium: YAG laser puncture or incision is a safe, efficacious option and even should be considered as the initial treatment in most patients. The main described advantage is that the use of laser allows for more precise, controlled and accurate incision of ureterocele with the very short penetration of the holmium laser. Also, additional, but theoretical benefit is that laser fibres do not have the local thermal effect, as compared with standard electrocautery.
To our knowledge our report is perhaps the first to present the serious side effect of laser therapy. According to our observation it can be clearly stressed that one have to be very careful using new techniques for endoscopic treatment and have to take into consideration that possible complications may overweight the advantages.