Mycobacterium tuberculosis is one of the most common diseases in the world, with a prevalence of approximately one-third of the global population and nine million new cases per year globally. In the USA, it is more common in immune suppressed conditions such as HIV or if there is a significant history of travel to tuberculosis-endemic regions. Tuberculosis generally affects the lungs, but can also affect other parts of the body. Mycobacterial cervical lymphadenitis, also known as scrofula refers to lymphadenitis of the cervical lymph nodes associated with tuberculosis as well as atypical mycobacteria. We report a case of a 20-year-old HIV negative, immunocompetent female, who was previously treated for latent tuberculosis, now presented with tuberculous lymphadenitis without pulmonary symptoms.
A 20-year-old female with no co-morbidities presented with a progressively worsening painful right sided neck mass of two months duration. She also complained of loss of appetite and five pounds of unintentional weight loss in one month. She denied cough, hemoptysis, breathing difficulty or wheezing. She also denied history of fever, night sweats, chills, difficulty swallowing or change in voice. She denied history of bleeding, bruising, axillary/groin swellings, abdominal pain/swelling, symptoms of hyperthyroidism like heat intolerance, palpitations, or diarrhea and symptoms of hypothyroidism like weight gain, fatigue, menstrual problems, cold intolerance. Pat medical and surgical history were not significant. She never had similar symptoms in the past. Her social history was not significant for any travel outside United States, homelessness, incarceration, animal exposure or tick bites. On further questioning, the patient revealed that she was treated for latent tuberculosis five years ago, with Isoniazid for six months by local public health department after confirming absence of signs, symptoms, or radiographic evidence of TB disease. She reported that she completed the course successfully without any side effects. Her family history was significant with patient's grandfather having a history of tuberculosis (TB) in 1970s and her mother having had tuberculosis in 1990s. Both were treated with four drug therapy for nine months at that time. She had gone to the Emergency Department one week prior to the current admission and was given a seven-day course of macrolide with no improvement in symptoms. On current admission, she was hemodynamically stable and afebrile. Physical exam revealed a right-sided neck mass which was multi-lobular, circumscribed 7 × 5 cm tender, firm in consistency in the anterior part and fluctuant in the posterior part with no erythema or active discharge. Overlying skin was smooth, the mass was not attached to the skin, not reducible, and no bruit or venous hum were heard (Figure 1). On chest exam, bilateral normal vesicular breath sounds were heard with no rales or wheeze.
 Figure 1: Showing the right sided neck mass which was multi-lobular, circumscribed 7 × 5 cm tender, soft to firm in consistency with no active discharge.
View Figure 1
Figure 1: Showing the right sided neck mass which was multi-lobular, circumscribed 7 × 5 cm tender, soft to firm in consistency with no active discharge.
View Figure 1
We ordered sputum Acid Fast Bacillus (AFB) smears, urine Histoplasma antigen which is endemic in this region and placed her in respiratory isolation. Chest X-ray showed minimal infiltrate in the right peri-hilar region. The left lung field is clear. No pneumothorax or pleural effusion. Trachea is midline. The cardiac silhouette is within normal limits. We consulted hematology and oncology as malignancy is one of the differentials in this case. Contrast Tomography (CT) scan of the neck with intravenous contrast revealed irregular, ill-defined peripherally enhancing collection in the right posterolateral neck with increasing liquefaction and mass effect, and Necrotic, peripherally enhancing bilateral cervical lymph nodes (Figure 2). Otolaryngology team performed Fine Needle Aspiration Cytology (FNAC) of the lesion which revealed abundant acute inflammation on pathology, and AFB smear was positive (Figure 3). Aspirate cultures were inoculated to Lowenstein Jensen-Gruft and Middlebrook 7H11 slants, incubated for 42 days at 35-37 degree Celsius at 6-8% CO2. Cultures were positive for Mycobacterium Tuberculosis Complex after 14 days. Identification was confirmed by the Hologics GenProbe Accuprobe, RNA/DNA hybridization and susceptibility test was performed by Quest Diagnostics Infectious Disease by Agar methodology for Ethambutol, Isoniazid, Rifampin, and Streptomycin and broth method used for Pyrazinamide (Table 1).
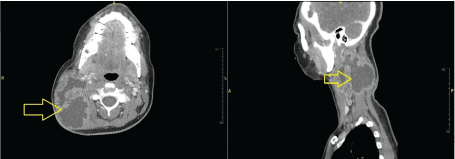 Figure 2: Irregular, ill-defined peripherally enhancing collection with increasing liquefaction and mass effect. Necrotic, peripherally enhancing cervical lymph nodes.
View Figure 2
Figure 2: Irregular, ill-defined peripherally enhancing collection with increasing liquefaction and mass effect. Necrotic, peripherally enhancing cervical lymph nodes.
View Figure 2
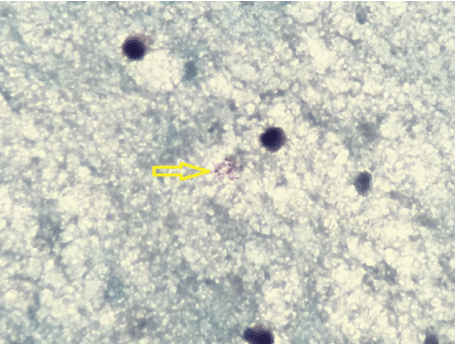 Figure 3: Positive for few Acid Fast Bacilli from the aspirate of the right cervical lymph node mass.
View Figure 3
Figure 3: Positive for few Acid Fast Bacilli from the aspirate of the right cervical lymph node mass.
View Figure 3
Table 1: Antimycobacterial susceptibilities by Agar method for Mycobacterium tuberculosis complex including minimal inhibitory concentration (MIC). View Table 1
Labs significant for White blood cell count: 4.68 [Reference range: 3.6 - 11.2 kilounit per microliter (K/uL)], Neutrophils Absolute: 3.03 (Reference range: 1.8 - 7.8 K/uL), Serum Creatinine: 0.65 [Reference range: 0.70 - 1.30 milligrams per deciliter (mg/dL)], Procalcitonin: 0.12 nanograms per milliliter (more than 1.9 represents a high risk of severe sepsis or septic shock).
Infectious work up: Human immunodeficiency virus 1 (HIV 1) + HIV 2 antibody were Negative. EBV VCA IgG: > 8.0 Arbitrary Index (AI), EBV Heterophile Ab < 0.2 AI, Quantiferon-Tb Gold: Positive, CMV IgG: 60 arbitrary unit/Liter (AU/L), CMV IgM: Negative, B henselae IgG < 1:64, B henselae IgM < 1:16, B Quintana IgM < 1:16, Toxoplasma IgG and IgM were Negative, Urine histoplasma Ag negative.
With her significant exposure to tuberculosis, with high suspicion of Tubercular adenitis, she was initiated on four-drug therapy empirically with Rifampin 600 mg PO daily (10 mg/kg), Pyrazinamide 1500 mg orally daily, Isoniazid 300 mg orally daily (5 mg/kg) along with Pyridoxine 50 mg orally daily, Ethambutol 800 mg orally daily. She did not have any pulmonary symptoms, was not able to produce sputum even on induction and her neck mass had no active drainage. We discussed with Infection Control and agreed that she did not require any airborne precautions. She was discharged in stable condition with a follow-up appointment. Her Mycobacterium tuberculosis complex Polymerase chain reaction (MTB-PCR) came back positive and susceptibility test by agar method revealed sensitive to all the first line drugs. She was seen in our clinic after two months and was tolerating treatment well with no side effects. Her neck mass was non-tender on exam and reduced in size. After 9 month follow up, swelling was completely resolved.
According to Yi Jeon [1], there were 36,089 reported cases of TB (71.4 cases per 100,000 people) in Korea in 2013. Of these, 7,369 cases were Extra-Pulmonary Tuberculosis (EPTB) (14.6 cases per 100,000) which comprised 20.4% of all cases of TB. The most commonly affected sites of EPTB in Korea were pleura, followed by lymph nodes, being the neck one of the most common sites of lymph node enlargement. This trend is similar in developing countries. In a cross-sectional study in Calcutta National Medical College and Hospital, India; Tubercular lymphadenitis was the most common diagnosis (45.4%) who presented with cervical lymphadenopathy [2].
As illustrated by our patient, the most common factors associated with EPTB that have been reported in the literature are: Young age, female gender, Asian and African origin, and human immunodeficiency virus (HIV) infection, been this last one factor the most important when developing EPTB, but negative in our patient [3,4]. Interestingly from this case, our patient received treatment for LTBI, and still got infected by EPTB being an immunocompetent patient. There have been different studies that talk about the effectiveness of latent treatment and recurrence of the disease, reaching over 60% of protectiveness in HIV patients with CD4 cell counts above 200 cells/mm3, and for the other 40% of this study population who had progression from latent to active tuberculosis who had low CD4 cell count, high quantity of alcohol consumption, large size of TST induration or high viral load [5].
Another factor that can be related to the effectiveness of LTBI treatment is compliance of the medication, which has been reported up to 63% of completed medications in infected individuals. There are different risk factors for the non-compliance. Race was found to be the most common risk factor; Hispanics, people born outside the US and Canadians had lower rates of medication compliance, whereas blacks had the highest compliance [6].
In a prospective study on 65 cervical tuberculous lymphadenitis patients performed in Shaheed Shamsuddin Ahmed Hospital, Sylhet, Bangladesh; Systemic features were found in 41 (63.07%) cases. Fever (87.8%; 36), Weight loss (63.4%; 26), Night sweat (63.4%; 26) and Loss of appetite (80.5%; 33) were the common systemic features [7], interestingly, our patient was asymptomatic and with a previous history of TB prophylaxis treatment, needing a wider approach to her condition.
The differential diagnosis for cervical lymphadenopathy includes infectious causes such as acute human immunodeficiency virus, infectious mononucleosis, cytomegalovirus, tuberculosis, toxoplasmosis, cat-scratch disease, tularemia, measles, rubella and non-infectious causes like lymphoma, leukemia, serum sickness, sarcoidosis and Kawasaki disease. Kikuchi disease is another differential to consider in this case. Kikuchi disease is a benign condition of unknown cause. It is most often seen in young adults, mostly women and characterized by fever and cervical adenopathy. Diagnosis is made by seeing the lymph node histology showing preserved architecture with necrotizing histiocytic infiltrate and fragments of nuclear debris.
A significant number of cases of FNAC diagnosed granulomatous lymphadenitis have an identifiable underlying causal pathology. It is suggested that FNAC combined with clinical correlation is useful as a first line investigation. The high specificity of the technique helps to single out those that need further investigation or biopsy [8]. The criteria for considering lymph nodes to be aspirated is 1.5 cm or more for inguinal lymph nodes and about 1 cm for extra inguinal lymph nodes [9].
Using culture as the reference method, the statistical values of ZN, ARS, and AF were as follows: Sensitivity 80.0%, 88.0%, 96.0%; specificity 93.85%, 86.15%, 78.46%; positive predictive values 83.33%, 70.97%, 63.16%; and negative predictive values 92.42%, 94.92%, 98.08%, respectively. There is a definite advantage of autofluorescence over Ziehl-Neelsen and auramine rhodamine which is to detect Mycobacteria, being more sensitive as well as an inexpensive technique. Autofluorescence can be a useful addition to routine cytology for early diagnosis and effective treatment. Directed treatment may decrease morbidity and prolong life expectancy. That's why FNAC has assumed an important role in the evaluation of peripheral adenopathy as a possible noninvasive alternative to excisional biopsy [10].
PCR can be effectively used to achieve a maximum sensitivity in the early and rapid diagnosis of TB lymphadenitis particularly in light of possible false positive or inconclusive histopathology results. A positive PCR result to support the histopathological finding of granulomatous inflammation suggestive of tuberculosis increases its positive-predictive value [11]. However, culture in Lowenstein Jensen media still remains the gold standard [12].
Anti-tuberculosis treatment is the mainstay of the management of TB lymphadenitis. Surgery increases the cure rate with an excellent cosmetic result and a low complication rate. This patient is a category I on the DOTS (directly observed treatment, short-course) guideline. Treatment for Category I includes Intensive Phase with four drugs; Isoniazid, Rifampin, Ethambutol, and Pyrazinamide for two months followed by Continuation Phase with Isoniazid, Rifampin for four months. Lymph node excision usually is not indicated, while the benefit of the usage of steroids is still unknown [13,14]. Surgical management is indicated when there is failure of previous treatment.
Full recovery is expected by the end of the treatment. Nevertheless, is important to keep in mind that paradoxical upgrading reactions could be experienced while on treatment, including enlargement of the lymph node or a new draining sinus in patients who have received at least ten days of treatment. This is expected in 20% - 23% of non-HIV patients. It occurred at a median of 1.5 months after initiation of treatment [15,16].
The global increase of EPTB is believed to be fueled by HIV related immunosuppression. Peripheral lymph node involvement is the commonest form of extra-pulmonary mycobacterial disease and the cervical region is the most frequently affected. Fine Needle Aspiration Cytology (FNAC) provides an inexpensive, quick and safe alternative to histopathology for the diagnosis of tuberculosis, to detect the presence of acid-fast organism on these aspirates using Neelsen stain as well as correlate the cytomorphological findings with Ziehl-Neelsen staining [17]. This is a case that definitely needs further consideration, as it could change the belief that even after being treated for TB, which does not exclude the patient to develop EPTB; drug resistance and medication compliance must be confirmed during LTBI treatment. LTBI have a 10% lifetime risk of developing active TB and 50% of those cases occur within the first 2 years following TB exposure [18].
The most commonly affected group are 20-40-year-old females and in the United States, it is most common in women and immigrants. prophylactic treatment months ago for TBC does not rule out the subsequent development of extrapulmonary TB, there is a lack of support for many epidemiological data after prophylactic treatment, that's why having tuberculosis in our differential diagnosis and the proper workup such as FNAC for lymph node enlargement is essential for a successful treatment.