Cervical and parapharyngeal teratomas are rare but possible causes for respiratory distress in neonates. They can also present as cystic masses in the neck and can be clinically indistinguishable from lymphatic malformations. Physicians must be cognizant of teratoma as an alternate diagnosis when faced with a cystic neck lesion that responds poorly to injection sclerotherapy. We present a case of a parapharyngeal teratoma which was initially diagnosed and treated as a lymphatic malformation.
Teratomas are the most common congenital tumours with elements derived from all three germ cell lineages in various degrees of differentiation. They can be found in different locations throughout the body but are uncommon in the head and neck region [1]. Cervico-facial teratomas can present in different manners depending on the exact site. They can present as neck or oropharyngeal mass, resulting in airway obstruction.
A full term neonate, with unremarkable antenatal scans, presented with respiratory distress immediately after delivery. Clinical examination revealed a distorted palate that was more prominently swollen on the right, and a vague lump on the right side of the neck. An oro-tracheal intubation was performed in view of the respiratory distress. He was referred to the otorhinolaryngology unit. Endoscopic examination showed a patent left choana, but the right posterior choana was narrowed by the mass that extended from the nasopharynx to the oropharynx. The initial Magnetic Resonance Imaging (MRI) scan showed a large cystic mass extending from the skull base to cricoid suggestive of a lymphatic malformation (Figure 1). The patient was referred to a second institution where the scans were reviewed and the diagnosis of a possible lymphatic malformation was confirmed. The patient was then planned for injection sclerotherapy.
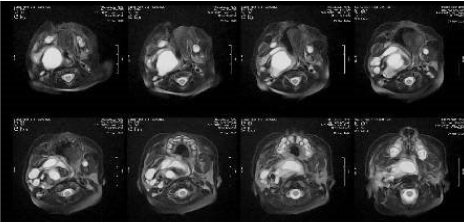 Figure 1: T2-weighted images showing a large mass occupying the parapharyngeal space with largely cystic components. View Figure 1
Figure 1: T2-weighted images showing a large mass occupying the parapharyngeal space with largely cystic components. View Figure 1
The child underwent sclerotherapy injection without tissue biopsy in 2 stages with minimal clinical and radiological resolution of the mass over 6 weeks. Initial cytology from aspiration and histology from a postnasal mass biopsy showed non-malignant cells and mucinous material respectively. At one month of age, after a second unsuccessful sclerotherapy injection, he underwent a second postnasal space biopsy, debulking of the nasopharyngeal and oropharyngeal components of the mass and a tracheostomy. Histology was suggestive of nasal glial heterotropia. Surgical excision was then planned. A repeat MRI scan was performed, again showing a large multi-cystic parapharyngeal lesion causing mass effect but without intracranial extension (Figure 2). At this stage, diagnosis of teratoma was also considered as a high possibility. A formal excision was then carried out using a cervical incision at 4 months of age (Figure 3). Final histology showed a mature teratoma. In addition to glial tissue, the specimen sections showed mature adipose tissue, bone with marrow elements, stratified squamous epithelium and skin adnexal structures, respiratory mucosa and focal choroid plexus and cerebellar tissue-features not seen in the previous biopsy.
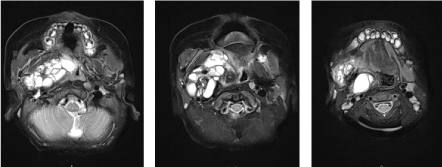 Figure 2: T2- weighted images showing a large mass occupying the parapharyngeal space and narrowing the airway. View Figure 2
Figure 2: T2- weighted images showing a large mass occupying the parapharyngeal space and narrowing the airway. View Figure 2
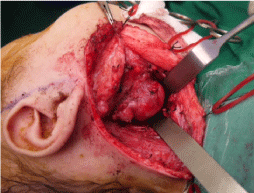 Figure 3: Intraoperative photo showing the parapharyngeal/cervical mass. View Figure 3
Figure 3: Intraoperative photo showing the parapharyngeal/cervical mass. View Figure 3
Head and neck teratomas can present in many ways from neck masses, nasopharyngeal or oropharyngeal masses to airway obstructive lesions with respiratory distress. They may not always be seen on antenatal scans and only diagnosed in the postnatal period [2]. Cervical teratomas are more likely to cause significant airway compromise compared to lymphatic malformations [3], and may require emergency intervention. Apart from teratomas and cystic hygromas, other considerations of congenital cervical masses are hemangiomas, dermoids, lymphomas, branchial cleft cysts, thyroglossal cysts and congenital goiter [4]. Parapharyngeal teratomas are uncommon. Newborns with these lesions can present with respiratory distress [5].
Imaging studies for a teratoma usually demonstrate a heterogeneous mass with both solid and cystic components. On Computed Tomography (CT), teratomas can appear heterogeneous, well circumscribed with both solid and cystic components. MRIs are a useful tool to assess soft tissue detail and to demonstrate any intracranial extension or skull base involvement [6]. The cystic components are often hypointense to isointense on T1-weighted images and hyperintense on T2-weighted images [7]. Other differential diagnoses for cystic lesions with septae include that of multiloculated cystic hygromas or branchial cleft cysts. In this case, with a disproportionately larger cystic component, the presumptive diagnosis was that of a cystic hygroma and was treated accordingly.
With heterogeneous histological characteristics in an uneven distribution, teratomas can also provide a histopathological diagnostic dilemma. A fully resected specimen may show numerous histological features not seen during sampling from incision biopsy specimens as seen in this case. In these instances, a formal excision will then be necessary to obtain a diagnosis.
While cervical and parapharyngeal tetratomas are rare, they can present similarly to cystic hygromas and must be considered as a differential diagnosis [8,9]. Further imaging studies should be carried out to plan subsequent intervention. Tissue biopsy with histology should always be obtained whenever possible in addition to imaging studies.
Distinguishing a cystic hygroma and teratoma in the head and neck region can be challenging as they may present at a similar anatomical locations and in young infants, as well as both having cystic elements on imaging studies. Teratomas also have numerous histological characteristics which may only be seen in a fully resected specimen. While tetratomas are less common than cystic hygromas, they must be considered as an alternative diagnosis especially when there is poor resolution with sclerotherapy treatment of a suspected lymphatic malformation.
None.
None.