Blunt traumatic injury to the subclavian, axillary or brachial artery is uncommon and could have devastating consequences. Historically open repair is performed however reports of successful endovascular treatments are increasing. A case is described of a seventy one-year-old patient with a blunt injury to his right arm after being crushed in a closing hydraulic door of a truck. He sustained a traumatic dissection of his right brachial artery with associated nerve injury to the brachial plexus. After trauma resuscitation he was successfully treated in the hybrid operation room. Through the common femoral artery a helical stent (Supera) was placed in the injured brachial artery. Postoperative recovery was without complications. Additional treatment for the nerve injury was performed several months after trauma by the neurosurgeon. Functional recovery of his right arm was good except for fine motoric functioning which is still recovering.
A review of the literature was performed to identify endovascular repair of blunt traumatic injury to the upper extremity. A total of 28 papers described 55 patients who underwent 56 procedures for subclavian, axillary and brachial injuries. The subclavian artery was affected and treated in 36 patients, in 16 patients axillary injury was treated and only 4 brachial arteries received endovascular repair. Technical success rate of endovascular treatment is good and stent graft patency rates are sufficient. Type of injury which was treated, the follow up technique, anticoagulant therapy and follow up duration varied extensively in the literature.
Endovascular treatment of blunt arterial trauma to the upper extremity appears to be feasible. No definite conclusion can be drawn concerning best type of stent graft, best follow up regime or post-operative medical treatment. Treating a patient in a hybrid operation room seems advisable to facilitate conversion to open treatment or treat associated traumatic injuries if necessary.
Endovascular treatment, Brachial artery, Trauma
In less than 10% of trauma patients an associated arterial injury is reported. The prevalence is low however morbidity and mortality in these cases are substantial [1]. Vascular injury in trauma is usually caused by blunt forces. In developing countries the majority of lesions are caused by penetrating injuries. All patients with vascular injuries should be treated using the same Advanced Trauma Life Support (ATLS) principles as any other trauma patients. A good coordination between trauma and vascular specialist during resuscitation and the planning of treatment is essential. The traditional approach to vascular trauma is open surgical repair however endovascular techniques are gaining terrain [2,3]. In surgically demanding areas like the thoracic aorta and its branches the endovascular repair has proven its effectiveness [4,5]. Other ways to use endovascular techniques in trauma are: haemostasis (plugs or coiling), temporary control (occlusion balloons) and vascular repair (stents, covered stents). The use of stenting in peripheral arteries in trauma is upcoming and initial reports are promising. The series on repair of subclavian, axillary, femoral and popliteal arteries have favourable results in short time follow up [3,6]. The potential benefits of endovascular versus open repair consist of: shorter operative duration, less blood loss and less surgical trauma to the patient [7]. The most important technical requirement is safe passage of a guidewire through the injured vessel to restore distal perfusion. A lesion with a total transection, much intraluminal thrombus, or external compression therefore seems less suitable for transluminal repair. A primary open repair or quick conversion to open repair should prevent prolonged ischemia of the injured extremity. A hybrid approach (direct site endovascular repair) to these demanding cases also seems as a good alternative [8]. We describe a recent case in which an endovascular repair of a blunt brachial artery was highly effective. We conducted a systematic review concerning endovascular repair of blunt vascular trauma to gain more knowledge in its application in the upper extremity.
A seventy one-year-old man was presented to the emergency department in October 2016. He was working on the farm of his son when he got trapped between hydraulic closing doors of a truck. He sustained trauma to his head and to his right arm. His medical history consisted of a transient ischemic attack and chronic obstructive pulmonary disease (GOLD classification 2). He was using pulmonary medication and a combination of carbaspirin calcium (100 mg once a day) and dipyridamole (200 mg twice a day). Trauma care was conform advanced trauma life support principles. Initial presentation showed a hemodynamically stable patient with full consciousness with a laceration of his head and bruising to the right arm. The X-ray imaging of thorax and pelvis, the focussed assessment with sonography for trauma, blood analyses and electrocardiogram were normal. A secondary survey showed a laceration on the medial aspect of the right upper arm with bruising and swelling. The capillary refill of his right arm was delayed and peripheral pulses were absent. A pulse oximetry measurement on the right index finger showed 95% saturation. The arterial pressure on the right could not be measured and on the left measured 144/72 millimetres of mercury. His right arm had diminished motoric functioning and sensibility was severely impaired. A regular X-ray of his right arm showed no fractures but did show air configurations in the subcutaneous tissue (Figure 1). An additional computed tomography of cerebrum and cervical vertebrae showed no abnormalities. In the same session a CT-angiography of the right arm was performed. The Ct showed subcutaneous air surrounding the brachial artery with a dissection and segmental thrombosis (Figure 2 and Figure 3). The neurologist made a careful neurological examination while the trauma surgeon cleared the patient for the operation. Directly after the trauma resuscitation he was brought to the hybrid operation room to perform surgery. General anaesthesia was given to the patient to facilitate a direct conversion to open surgery if necessary. A sterile exposure was made for both groins and the right arm and cervical area. A duplex ultrasound guided retrograde puncture of the right common femoral artery and placement of a 6 French sheath gave access. After gaining arterial access systemic heparin was administered (5000 international units). With a Terumo guidewire (0.035") [Terumo Europe NV, Belgium] and a SIM1 catheter [Cordis Corporation, USA] the axillary artery was reached through the brachiocephalic trunk. A digital subtraction angiography showed a traumatic dissection of the proximal brachial artery (Figure 4). In a gentle twisting fashion the 0.035 guide wire was advanced through the lesion follow by the catheter. An angiography through the catheter, distal to the lesion, confirmed intraluminal positioning of the catheter. After this recanalization the SIM1 catheter was exchanges for a Multi-purpose catheter [Cordis Corporation, USA]. A smaller guidewire (0.018") was placed and a 6 mm balloon angioplasty was performed. After angioplasty two 5 mm × 100 mm Supera [Abbot, USA] stent grafts were deployed in telescopic fashion with the distal stent being deployed first (Figure 5). The control angiography showed a good positioning of the stent grafts (Figure 6). The puncture site was closed with a Star close closure device [Abbot, USA]. After surgery distal pulsations at the wrist had restored and the sensory impairment was recovering. During the first 2 post-operative days the motoric disability markedly improved to nearly normal. Postoperative recovery was without complications. Patient received dual platelet anticoagulation (carbasparin calcium 100 mg once a day and clopidogrel 75 mg once a day) for the first 3 months. After three months his own pre-trauma anticoagulation therapy was restarted (carbaspirin calcium and dipyridamole). A control CT-angiography at 4 months post-operatively showed patent stent grafts with good deployment. Duplex-ultrasound imaging of the stent grafts showed patent stents at 6 months follow up. Unfortunately the patient did sustain concomitant neurological damage to the brachial nerves plexus at trauma. At 4 months post-operatively the neurosurgeon planned a decompression of the ulnar nerve. To date nearly all motoric functioning of his arm recovered except for fine motoric functioning.
 Figure 1: Subcutaneous air on regular X-ray. View Figure 1
Figure 1: Subcutaneous air on regular X-ray. View Figure 1
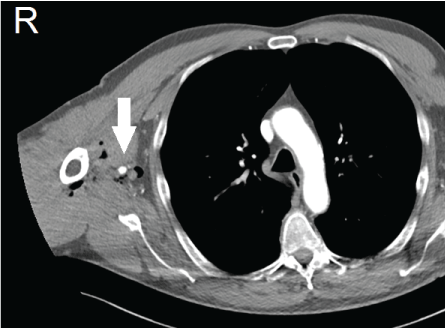 Figure 2: Subcutaneous air on CT surrounding right arteria brachialis. View Figure 2
Figure 2: Subcutaneous air on CT surrounding right arteria brachialis. View Figure 2
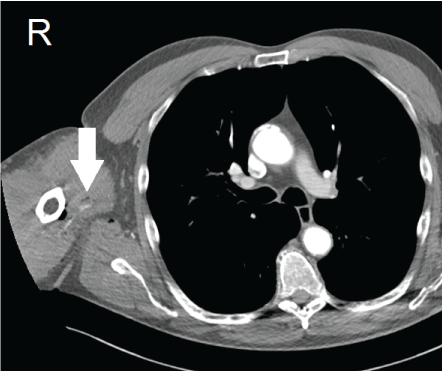 Figure 3: Thrombosed brachial artery at site of dissection. View Figure 3
Figure 3: Thrombosed brachial artery at site of dissection. View Figure 3
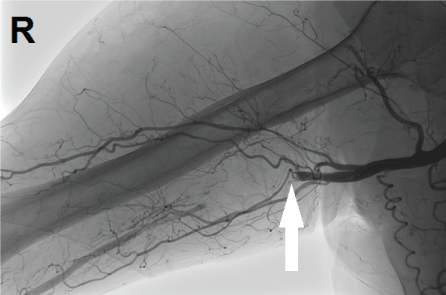 Figure 4: Traumatic dissection of right arteria brachialis. View Figure 4
Figure 4: Traumatic dissection of right arteria brachialis. View Figure 4
 Figure 5: Placement of two 5 × 100 mm Supera stent grafts. View Figure 5
Figure 5: Placement of two 5 × 100 mm Supera stent grafts. View Figure 5
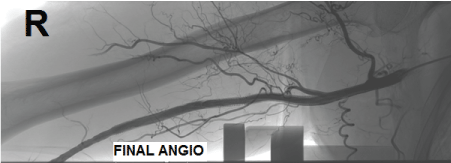 Figure 6: Control angiography. View Figure 6
Figure 6: Control angiography. View Figure 6
Two researchers (RRS & AR) conducted a independent review using Pubmed (www.pubmed.gov) and Embase (www.embase.com) in order to identify all cases of endovascular treatment of blunt vascular trauma to the upper extremity. We used the following search terms "subclavian" or "axillary" or "brachial" combined with "artery" and "blunt" and "trauma" and "endovascular" and "treatment". All publications of English language published after the year 2000 were eligible for selection. Article types included all original articles, case studies, case reports and retrospective analysis reporting blunt arterial trauma to the upper extremity. Excluded were all traumatic injuries to the central thoracic and abdominal arteries, carotid artery, vertebral artery and the lower extremity. Furthermore we ignored all publications of endovascular repair of arterial trauma with iatrogenic or penetrating aetiology. All papers lacking sufficient data on trauma mechanism (blunt/sharp or iatrogenic) and type of therapy (endovascular or open) were excluded from analysis. On initial search a total of 131 papers were identified. An additional 15 papers were added on cross-reference base to be screened. Applying the exclusion criteria 68 out of 146 papers were selected for full text screening after abstract analysis. By full text analysis another 40 articles met exclusion criteria reducing the appropriate papers to a total of 28. All of the selected studies are case reports and retrospective case series. No prospective studies or randomised trials are available in this subject. This review consists of 8 retrospective studies or large case series and 20 case reports describing endovascular repair of blunt trauma to the subclavian, axillary or brachial artery. In total 55 patients were described receiving a total of 56 endovascular procedures. One case reported by Chander, et al. describes a patient who receives a stent graft in both right and left axillary artery. In a total of 36 subclavian, 16 axillary and 4 brachial arteries an endovascular repair was performed. Trauma mechanism consisted of a Motor Vehicle Collisions (MVC), falling from height, shoulder luxation, clavicular fracture and mechanical compression of the thorax. Diverse types of vascular lesions were repaired: pseudoaneurysms, active haemorrhage, occlusions, transections, and dissections. The types of stent grafts which were used are: Luminexx stents [Bard, USA], Fluency endografts [Bard, USA], Strecker [Boston Scientific, USA], Wallstent [Boston Scientific, USA], Wallgraft [Boston Scientific, USA], Hemobahn stent grafts [W.L. Gore and Associates, USA], Jostent stent-grafts [Jomed AB, Germany], Viabahn stent grafts [W.L. Gore and Associates, USA], S.M.A.R.T [Cordis Corporation, USA], Zilver [COOK medical, USA] and Atrium iCAST, [Atrium Medical Corporation, USA].
The overall reporting of post-operative medical treatment which was prescribed was poor. In only 11 of 28 studies a description of therapy was given at all. In the reported papers treatment regimens varied in the following: carbaspirin calcium (3), dual platelet (n = 6), vitamin K antagonist (n = 1) and no anticoagulation due to spontaneous elevated activated platelet activation time (n = 1). In some trials an initial post stent graft therapeutic dose of low weight heparin was given for 1 to 9 days followed by dual platelet anticoagulation.
Patency follow up of the treated artery or stent graft was performed in 24 studies however in 5 of these studies authors did not specify on how follow up was performed. Of the remainder of 19 studies the follow up consisted of duplex scanning (n = 10) clinical check-up (n = 5) or CT-angiogram (n = 4). The overall follow up duration ranged from 0.5 month to 84 months.
Complications related to the transluminal procedure of blunt traumatic lesions were seen in 4 out of 56 treated vessels. Two early complications consisted of: a distal embolectomy after stent placement and one endoleak after treatment of a pseudoaneurysm. The last mentioned endoleak was without therapeutic consequences with stable aneurysm diameter in CT follow up for 3 years. Two late complications were seen and consisted of a stent thrombosis at 1 month and 12 months after placement. The first was successfully treated with thrombolysis and remained patent for the remainder of follow up. The second was without clinical symptoms and was treated conservatively. No severe access related complications were described: one pseudoaneurysm of a brachial access site was treated with a thrombin injection.
Table 1: Published studies on blunt traumatic injury to the subclavian artery. View Table 1
Table 2: Table two published studies on blunt traumatic injury to the axillary artery. View Table 2
A concomitant nerve injury to the brachial plexus was seen in 7 patients after trauma. Six of these patients had an axillary artery injury and only 1 of the 36 subclavian injuries had a plexus injury. A detailed description of all patients is found in Table 1, Table 2 and Table 3. The patient characteristics are described in Table 4.
Table 3: Published studies on blunt traumatic injury to the brachial artery. View Table 3
Table 4: Patient characteristics. View Table 4
Early identification and treatment of concomitant vascular injury in trauma patients is essential. The advantages of an endovascular approach compared to open surgery have increased its use in traumatology [36]. One example is the use of selective coiling which has significantly reduced the need for emergent splenectomy or nephrectomy. Currently the transluminal approach of trauma related injuries to central arteries such as the thoracic aorta and its branches is an accepted strategy. Recent literature suggests that these favourable outcomes in central vascular trauma might also apply to peripheral arteries but long term follow up is lacking. The potential of publication bias and patient selection in these data is high. Furthermore there is heterogeneity in anatomical location and aetiology of the lesions. Description varies from outcome after iatrogenic, blunt or sharp trauma. We should be aware during analysis of outcome after endovascular treatment of peripheral traumatic lesions that its aetiology has an important impact on success. For instance, iatrogenic injuries during endovascular procedures can be identified and treated immediately making feasibility and outcome favourable. In the contrast, mortality rates after sharp injury to the subclavian and axillary artery are high. Demtriades, et al. described an overall mortality of 34.2% of 79 patients in 1999 [37]. Nevertheless reports of successful endovascular repair in penetrating injuries to the subclavian or axillary artery are increasing. A retrospective analysis of 46 cases by Danetz, et al. showed that in almost 50% of penetrating vascular traumas an endovascular treatment was possible but was performed in only 2 cases. The surgeon's preference to open surgery or lack of endovascular services probably accounted for the low incidence of endovascular treatment [38].
Blunt vascular trauma to the upper extremity is rare but seen in high velocity trauma to the thorax, clavicle fractures and luxation's of the shoulder. Knowledge of performance and patency of endovascular treatment in these selected cases is limited. This current review was performed specifically to analyse performance of endovascular techniques in this patient category. We saw that the majority of the reports are descriptions of subclavian artery repair. This is probably due to its partly intrathoracic anatomical position which makes an endovascular approach more appealing than a thoracotomy. Endovascular repair of axillary arteries but especially brachial arteries in blunt trauma is scarce. This might be due to reluctance to place stent grafts on flexible parts of the body. At present however multiple stent grafts are available which are suitable for these conditions making an endovascular approach more appealing. With these new stent grafts and technological improvements more challenging lesions can be treated transluminal than before. Additionally with accumulated endovascular experience, procedures are performed in trauma like hybrid and rendezvous techniques to traverse challenging lesions or complete transections [34]. This review shows that reports of endovascular treatment in blunt trauma to the subclavian, axillary and brachial injuries are increasing. After successful stent placement, patency appears to be good. The good performance of these stents might be attributed to the fact that they are deployed in otherwise healthy non atherosclerotic arteries. However, the reported follow up duration is still fairly limited compared to studies reporting patency of stents in atherosclerotic lesions.
The overall reported complication rates are low, minor and easily treated. The reported incidence of stent thrombosis is low and such late occlusion can be treated with a minor re-intervention. The benefit of the endovascular approach first is that if needed a re-intervention can be planned on a more favourable moment.
Concerning the reported type of treated lesion and type of stent graft which was used we identified great heterogeneity. Additionally the post-operative medical treatment and follow up terms and technique were poorly reported and varied extensively.
One major limitation of this review is the limited information provided on publication bias and patient selection to open and endovascular treatment. Nonetheless successful endovascular treatment is described in hemodynamically unstable patients and even in complete arterial transections. This suggests that with increasing experience and rapid development of new flexible stent grafts the amount of lesions suitable for endovascular repair is expanding. Ganapathy, et al. describe that during their study period from 2009 until 2015 the endovascular treatment of peripheral vascular trauma in their hospital increased from 7% to 50% [3].
As a result of the wide range of used stents, this review cannot advise which type of stent graft one should use. Also one cannot give any recommendation on post-operative anticoagulation. Although a randomised trial would be a modality to answer these questions, the limited incidence of these types of injuries makes such a solution not feasible. However, overall data suggest that endovascular treatment for this indication is feasible when equipped with an adequate endovascular service. Endovascular treatment of these trauma patients can reduce procedural time, reduce blood loss and reduce operative trauma to the patient. Furthermore in case of inability to safely pass the lesion with a guide wire the application of an occlusion balloon can limit blood loss and facilitate controlled open repair. Treatment of blunt vascular trauma in a hybrid room seems advisable to treat concomitant injuries, convert to open surgery or perform a fasciotomy if necessary. Obviously extensive experience in endovascular treatment and knowledge of type of stent grafts and its application is imperative.
Endovascular treatment of blunt vascular trauma to the upper extremity is technically feasible. An endovascular first approach seems recommendable with the concept of damage control in mind. Furthermore the long term patency of endovascular treatment is no longer a threshold. Treatment of these patients in an adequately equipped hybrid rooms seems advisable in order to be able to convert when necessary and treat associated injuries as well.
None.
None.