A 57-year-old hypertensive, obese woman presented with several weeks of a febrile flu-like illness, facial and extremity flushing, and laboratory findings of polycythemia. A workup revealed no evidence of polycythemia rubra vera or a secondary cause of her polycythemia (her erythropoietin level was normal, she had no splenomegaly, and a test for JAK2 v617F mutation was negative). Over the next two weeks, her fever subsided, and her hematological profile returned to normal, pre-illness levels. We conclude that this patient had Gaisbock's syndrome, a relative polycythemia that occurs when there is clinically evident contraction of the intravascular fluid space (plasma volume).
Polycythemia, Hypertension, Plasma volume, Packed cell volume, Venesection, Erythromelalgia
First described in 1905, Gaisbock's syndrome refers to a symptom complex associated with polycythemia that cannot be attributed to a diagnosis of polycythemia rubra vera or to a secondary erythrocytosis that has occurred in response to hypoxemia. In order of decreasing importance, risk factors for the development of Gaisbock's syndrome include male sex, hypertension, smoking, diuretic therapy, obesity, and emotional or physical stress. The polycythemia has been attributed to decreases in plasma volume, and may be associated with increases in blood viscosity and peripheral vascular resistance and a propensity to develop arterial and/or venous thromboses [1-3].
We describe the case of obese women with poorly controlled diastolic hypertension who presented with a febrile flu-like illness and new-onset polycythemia that resolved over a two-week period as she recovered from her illness. Studies for primary and secondary causes of polycythemia were negative, supporting the diagnosis of Gaisbock's syndrome.
The patient, a 57-year-old Caucasian woman, was seen because of a two-week history of fever and a flu-like illness. Her illness began with mild upper airway symptoms (coryza, sore throat), accompanied by myalgias, arthralgias, malaise, fatigue, and anorexia followed by an intermittent non-productive cough and exacerbation of her migraine headaches. She also noted the occurrence of flushing of her face and swelling and flushing of the soles of her feet. Her past medical history was notable for hypertension, a multinodular thyroid, and mild IgM deficiency. She was taking hydrochlorothiazide and triamterene for her hypertension, but was on no other medications. She was a non-smoker, had no history of sleep apnea, and kept herself well hydrated during the illness. Her husband had experienced a flu-like illness 2-3 weeks earlier, and she had recently been immunized to influenza, but the vaccine did not cover 40% of the prevalent strains.
Physical examination revealed a temperature of 102 ℉, a blood pressure of 138/100, a regular pulse of 74 beats/minute, a respiratory rate of 14 breaths/minute, and a BMI of 41. Facial flushing, which increased in the recumbent position, was present, and the soles of both feet had increased warmth, diaphoresis, and erythema characteristic of erythromelalgia (Figure 1). Her oropharynx was mildly injected without exudates. She had no adenopathy, and the examination of her heart, lungs, and abdomen was unremarkable. Her skin turgor was normal.
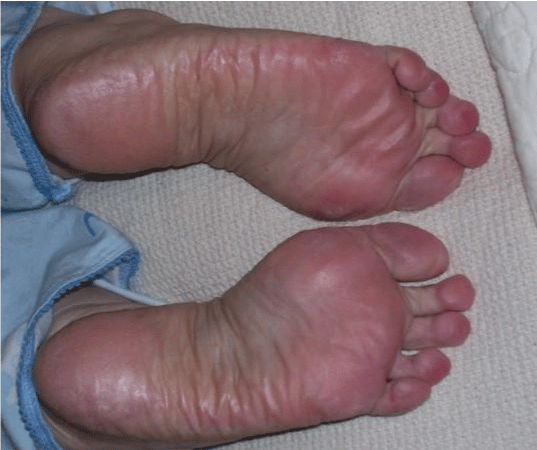 Figure 1: On presentation our patient had erythema, swelling, and perspiration of the soles of her feet. These findings are characteristic of erythromelalgia, which can occur de novo or in association with several medical conditions, including hypertension and polycythemia. The erythromelalgia resolved as her fever subsided and her hematologic parameters returned to normal. View Figure 1
Figure 1: On presentation our patient had erythema, swelling, and perspiration of the soles of her feet. These findings are characteristic of erythromelalgia, which can occur de novo or in association with several medical conditions, including hypertension and polycythemia. The erythromelalgia resolved as her fever subsided and her hematologic parameters returned to normal. View Figure 1
A complete blood count revealed elevations in her hematocrit (packed cell volume, PCV), hemoglobin, and red blood cell count (Table 1). Her erythropoietin level was normal at 7.4 MIU/mL and testing for a JAK v617F mutation was negative. Other blood studies, including blood urea nitrogen, creatinine, electrolytes, liver chemistries, uric acid, thyroid stimulating hormone, B12 level, and leukocyte alkaline phosphatase were within normal limits. An abdominal CT scan was normal with no evidence of splenomegaly, and a chest x-ray was unremarkable.
Table 1: Patient’s hematologic parameters. View Table 1
Over the next several weeks, her fever and respiratory symptoms resolved, and her hematologic parameters incrementally returned to normal, pre-illness values (Figure 2). The patient’s diuretic therapy was discontinued and she was placed on a combination of a beta blocker (metoprolol), a short acting calcium channel blocker (amlodipine) and an angiotensin converting enzyme receptor inhibitor (Losartan) for treatment of her hypertension. Since then, she has had better control of her blood pressure, and no further episodes of Gaisbock's syndrome.
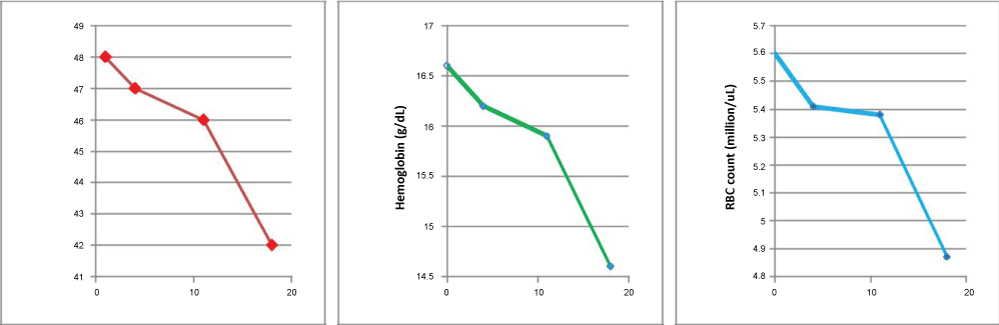 Figure 2: The patient’s hematologic parameters returned to normal as she recovered from her flu-like illness and her blood pressure normalized. The x-axis values represent the number of days since she was first seen. PCV (Packed Cell Volume). View Figure 2
Figure 2: The patient’s hematologic parameters returned to normal as she recovered from her flu-like illness and her blood pressure normalized. The x-axis values represent the number of days since she was first seen. PCV (Packed Cell Volume). View Figure 2
Polycythemia is a disease state in which the PCV in mL/dL is more than 52 in males and 47 in females. It may occur as a result of overproduction of red blood cells in the setting of a myeloproliferative disorder, such as polycythemia vera, or in lung diseases and conditions such as sleep apnea that cause sustained or intermittent levels of hypoxemia with consequent increases in erythropoietin-mediated erythropoiesis. Our patient had normal erythropoietin, leukocyte alkaline phosphatase, and B12 levels, an absence of splenomegaly, and a negative test for a JAK2 V617F mutation, which mediates strongly against a primary or secondary cause of her polycythemia [4,5]. Although we were unable to measure her plasma volume and red cell mass, her hematologic and clinical parameters and her course are in keeping with Gaisbock's syndrome, in which the polycythemia is ascribed to a contraction in the plasma volume [1].
Our patient had four risk factors for Gaisbock's syndrome - hypertension, diuretic therapy, physical and emotional stress, and obesity; of these, hypertension (particularly diastolic hypertension) appears to be the most significant contributor to the polycythemia of Gaisbock's syndrome [2]. In this regard, Emamian and associates studied 9,808 individuals with essential hypertension and found that they had spurious elevations in their hematocrits, hemoglobin levels, red cell counts, and mean corpuscular hemoglobin values [6]. Their finding is in keeping with the fact that plasma volumes are usually (but not always) decreased in patients with hypertension and that, as a group, hypertensives have low plasma to interstitial fluid volume ratios, indicating that extracellular fluid distribution between the intravascular and interstitial compartments is shifted toward the latter. This shift is thought to be related to altered capillary filtration pressure due to increased venous resistance [7].
Our patient experienced considerable physical and emotional stress during her illness. Stress related activation of the sympathetic nervous system has historically been linked with relative polycythemia [8]; in experimental animals, infusion of adrenalin and noradrenaline increases venous tone and causes mild reductions in plasma volume and small increases in PCV [9]. Although the evidence for an association of stress with relative polycythemia is somewhat tenuous [2], we suspect that it played a significant causative role in our patient’s polycythemia.
Patients with a history of Gaisbock's syndrome should be monitored closely for the possibility of recurrence. Messinezy and Pearson found that the PCV returns to normal in one-third of patients with relative polycythemia, in one-third the PCV stays elevated, and in the remaining third the PCV is intermittently elevated [10]. Management should include tight control of hypertension, avoidance of diuretic therapy, smoking cessation, and, in obese individuals, institution of a vigorous weight loss regimen, which will have the added benefit of reducing the patient’s risk for cancer, type 2 diabetes mellitus, ischemic heart disease, cerebrovascular disease, osteoarthritis of the hip and knees, and the metabolic syndrome. Venesection is rarely necessary, but should be considered if PCV levels are sufficiently elevated to place the patient at risk of thrombotic events (i.e., > 54 mL/dL) or if the patient is experiencing symptoms of cardiovascular ischemia [2,11].
We have documented a case of Gaisbock's syndrome in an obese 57-year-old woman that occurred in the setting of a flu-like illness and persistent diastolic hypertension. In addition to facial rubor, as originally described by Gaisbock, she had the unique finding of erythromelalgia involving the soles of her feet. Her polycythemia resolved incrementally over a 2 week period as her blood pressure was brought under better control and her respiratory illness resolved. Gaisbock's syndrome is best categorized under the heading of a relative polycythemia, components of which are commonly seen in persons with essential hypertension.
The patient gave her approval to publish this case report.