We report two cases of an unusual technical complication, arising during percutaneous coronary intervention, and its management.
The first patient, a 65-year-old male, presented to our emergency department with unstable angina without troponin elevation for the first time in January 2015. A calcified culprit lesion in the Right Coronary Artery (RCA) was managed by stenting. Staged Percutaneous Coronary Intervention (PCI) of a significant proximal stenosis of the Left Anterior Descending (LAD) was scheduled for March 2015. During this procedure, two drug-eluting stents were implanted in a highly calcified and tight stenosis of the LAD (Figure 1). Significant residual stenosis was observed, which could not be resolved by high-pressure angioplasty at 26 atm with a non-compliant balloon catheter, or even at 35 atm with an ultra-high pressure balloon (OPN NC balloon, SIS Medical, Switzerland) (Figure 2). The stable patient was transferred the next day to a high-volume center for definitive treatment of the lesion by repeat angioplasty or alternatively rotablation of the implanted stent as a bail-out option. During this second procedure, a shorter ultra-high pressure balloon was inflated in the stent to optimize focussed pressure delivery to the resistant area. Pressure was increased slowly into the off-label range > 35 atm, as reported previously [1]. At 40 atm rupture of the balloon catheter occurred, as evidenced by an abrupt drop in pressure in the indeflator (device to in- and deflate PCI balloons). Unusually, the balloon itself remained inflated within the coronary artery, i.e. filled with contrast medium (Figure 3), whereas the rupture had obviously taken place in a more proximal part of the catheter. As the inflated balloon fully occluded the LAD, ST segment elevations were noted on the monitor ECG and the patient began to suffer from angina. When gentle pull was applied to remove the still inflated balloon from the coronary artery, the proximal shaft completely detached from the distal part at the rupture site (Figure 4 and Figure 5). An attempt to puncture the inflated balloon inside the LAD with the stiff end of a coronary wire that was advanced through a microcatheter failed. Removal of the detached and still partially inflated balloon from the calcified lesion was eventually achieved by "jailing" the remaining balloon shaft in the guiding catheter with another balloon inflated at high pressure inside the guide and then carefully retracting the catheter together with the balloon (Video 1). Total ischemia time until successful retrieval was 30 min. Patient recovery was uneventful and without residual wall motion abnormalities at discharge, although the complication led to a significant increase in necrosis markers and stent deployment was still suboptimal.
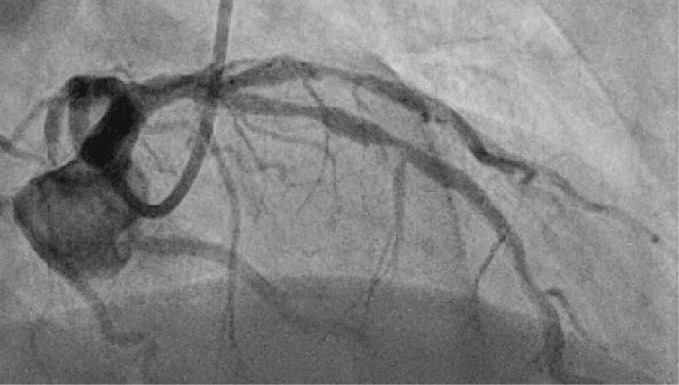 Figure 1: Right anterior oblique cranial projection showing suboptimally expanded stents in the proximal LAD. View Figure 1
Figure 1: Right anterior oblique cranial projection showing suboptimally expanded stents in the proximal LAD. View Figure 1
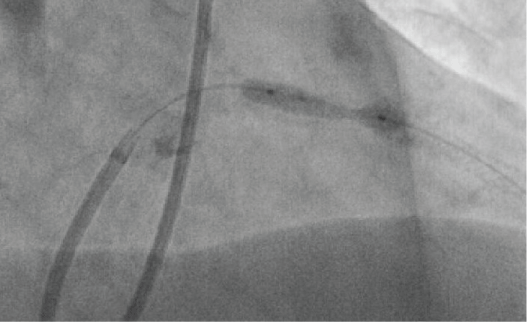 Figure 2: "Dog-boning" of ultra-high pressure balloon inflated inside the stent at 35 atm. View Figure 2
Figure 2: "Dog-boning" of ultra-high pressure balloon inflated inside the stent at 35 atm. View Figure 2
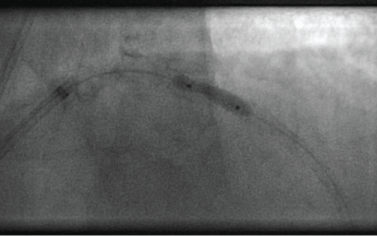 Figure 3: Ultra-high pressure balloon that remains inflated even after pressure-drop in the indeflator, indicating rupture. Balloon is still underexpanded in the proximal part. View Figure 3
Figure 3: Ultra-high pressure balloon that remains inflated even after pressure-drop in the indeflator, indicating rupture. Balloon is still underexpanded in the proximal part. View Figure 3
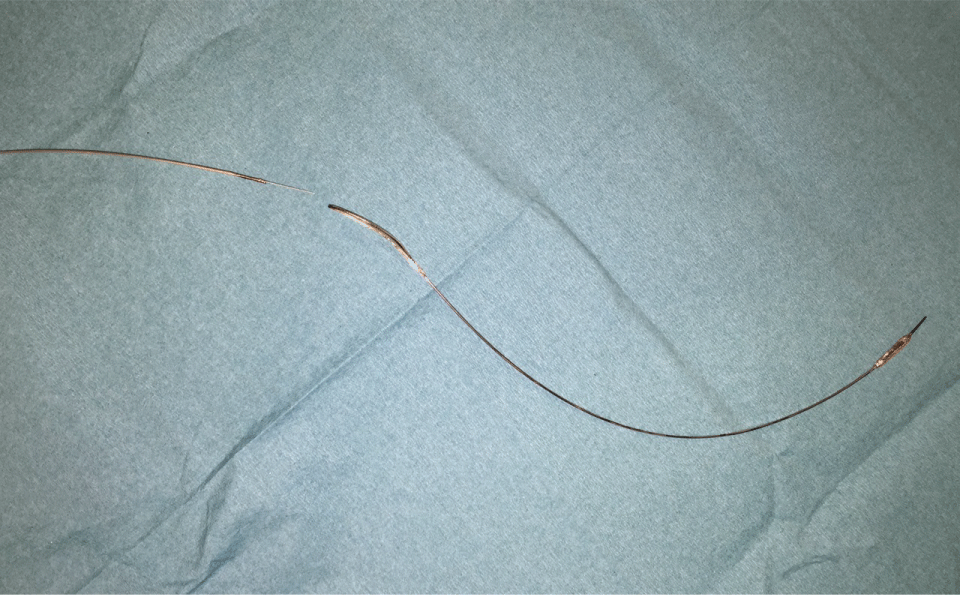 Figure 4: Ruptured balloon after successful removal. View Figure4
Figure 4: Ruptured balloon after successful removal. View Figure4
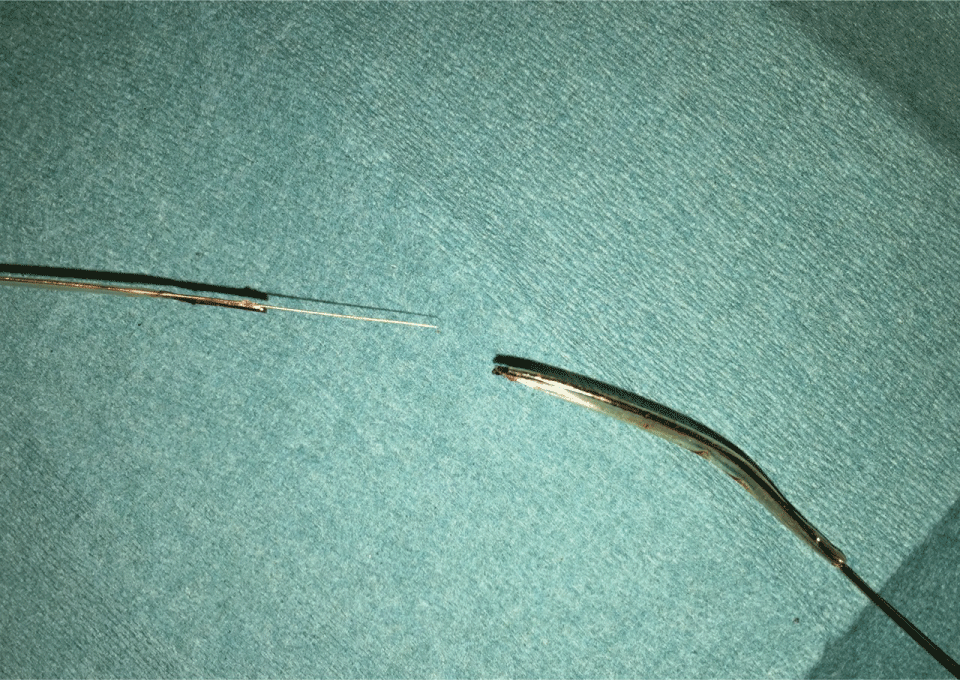 Figure 5: Closeup of the site of rupture and detachment. View Figure 5
Figure 5: Closeup of the site of rupture and detachment. View Figure 5
Video 1: Successful removal of balloon after caging detached distal shaft in the guiding catheter through trapping with non-compliant balloon. View Video 1
Shortly thereafter, a second case of shaft rupture of an ultra-high pressure balloon occurred in our catheterization laboratory at the Helios Albert-Schweitzer-Hospital, Northeim, Germany. This patient presented in May 2015 with a non ST-elevation acute coronary syndrome with troponin elevation. Coronary angiography showed 3-vessel disease with a 90% stenosis in the RCA. Our strong recommendation to undergo urgent surgical bypass grafting was vehemently and repeatedly rejected by the patient. Therefore, PCI of the culprit lesion in the distal RCA was attempted. As a 2.5 mm non-compliant balloon catheter still displayed significant "dog-boning" in the calcified lesion at 26 atms (Figure 6), ultra-high pressure angioplasty was performed with a 2.5 mm OPN balloon. Rupture occurred at an inflation pressure of 36 atm, just above "rated burst pressure". Again, it was not the balloon itself that teared open but the distal catheter shaft (Figure 7). In this second case however, the distal part remained attached to the catheter shaft, contrast medium drained retrogradely into the ascending aorta and removal of the partially inflated balloon could be safely performed without complications.
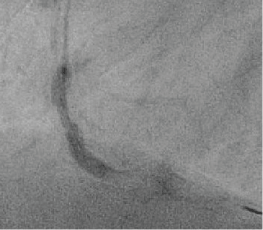 Figure 6: "Dog-boning" of ultra-high pressure balloon in RCA at 35 atm in patient 2. View Figure 6
Figure 6: "Dog-boning" of ultra-high pressure balloon in RCA at 35 atm in patient 2. View Figure 6
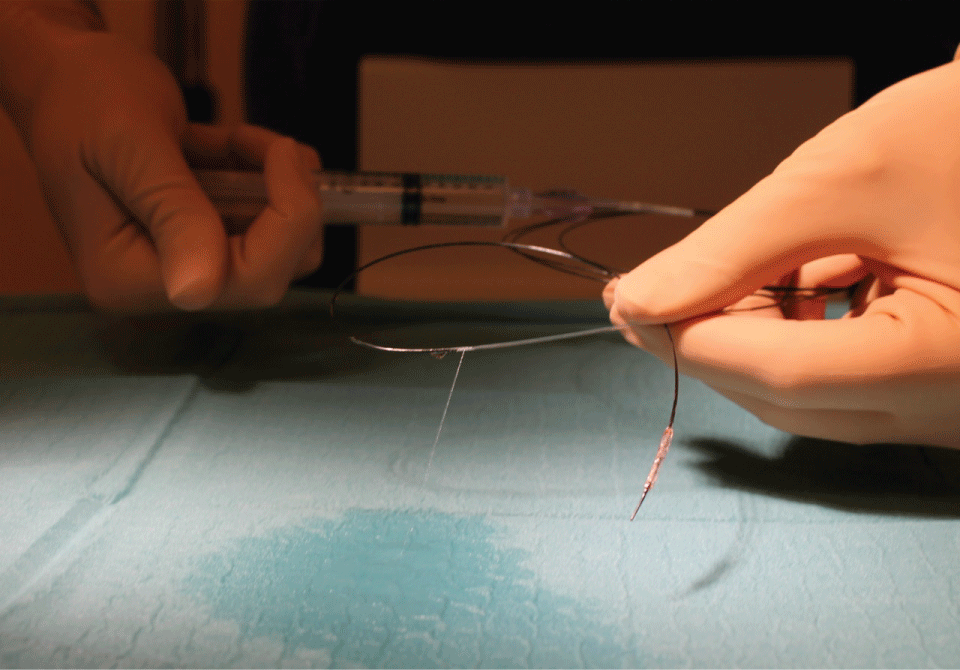 Figure 7: Flushing with saline indicates site of rupture in balloon catheter from case 2. View Figure 7
Figure 7: Flushing with saline indicates site of rupture in balloon catheter from case 2. View Figure 7
While modern interventional cardiology provides a broad technological toolkit to treat even the most complex lesions in the coronary circulation, calcified stenoses remain one of the bigger challenges to the interventionalist with often suboptimal stent expansion [2], leading to higher rates of stent-associated complications [3]. Our cases highlight the fact that optimal preparation is of utmost importance in treating such lesions. Rotablation is the most frequently applied method to deal with this problem [4], but is not available in all centers. As an alternative, ultra-high pressure balloons have been developed to deliver pressures up to 35 atm to crack even the hardest circular calcifications found in the human coronary system. These are also a useful tool to correct stent-under expansion, a situation in which rotablation is controversial and not without risks. A specifically designed double-layer outer hull provides for pressure resistance and form stability, i.e. minimal compliance. They have also been described to rupture "atraumatically" in a two-stepped manner and with a coaxially directed pressure release into the artery lumen (instead of the artery wall) due to this double-layer.
Pressures above the manufacturer-recommended "rated burst pressure" are frequently employed with non-compliant and even ultra-high pressure balloon catheters by interventionalists to treat resistant lesions under full acceptance of a certain risk of intracoronary balloon rupture in an individualised risk-benefit consideration [5]. Rupture of balloons inside the coronary artery is not an unusual phenomenon and it happens even in the recommended pressure range, as sharp calcified edges or spiculae can cut and damage angioplasty balloons during inflation, predisposing them to rupture even at pressures normally well tolerated [2].
We have, however, never observed this phenomenon in the shaft of the balloon catheter. Both balloons were introduced fully intact and undamaged into the guiding catheter. We speculate that ultra-high pressure balloons are more prone to bending inside the guide, as their crossing profile is significantly higher than for lower pressure balloons and as they are often used for difficult-to-cross lesions, necessitating forceful delivery. While a designated breaking point in the shaft part of the balloon catheter could theoretically prevent intracoronary pressure release in case of rupture, and might therefore actually be a safety feature to consider, the shaft was almost fully severed in our first case, while at the same time being so deformed that it did not allow for retrograde drainage of contrast medium. This led to a life-threatening situation for the patient which could be resolved only with major difficulties even by a very experienced interventionalist in a tertiary care setting.
We therefore believe that recognition of this potentially dangerous complication and the described strategies to resolve it are of great importance to the interventional cardiological community. Recognition of this apparently device-specific complication is important for interventionalists when making decisions about the best technical approach to treat calcified coronary lesions.