We present the case of a 52-year-old lady affected with cortico dependent minimal change disease who developed a blue pigmentation of her fingernails during a 3-months treatment with cyclophosphamide for cortico dependent minimal change disease.
The typical manifestation of onset of Minimal Change Disease (MCD) is a pure nephrotic syndrome.
The nephropathy may respond rapidly to corticosteroids [1], but may also show frequent relapses, which occur in 25%-30% of patients during corticosteroid tapering [1]. In these cortico dependent adult patients K-DIGO guidelines recommend a 8-12 weeks course treatment with cyclophosphamide (CyF) 1 mg/kg/day [2].
CyF is a nitrogen mustard belonging to alkylating drugs' group, which is known to have common early side effects, such as leukopenia and thrombocytopenia, bladder and mucosal toxicity, and also common late side effects, such as infertility or carcinogenesis.
A blue pigmentation of fingernail is not specifically reported in company product characteristics, even if nail discoloration and nail disorders are listed among the numerous side effects, and have only anecdotally been reported in the literature [3-5].
A 52-year-old Malagasy woman presented to our observation because of leg edema. She had no previous history of disease, except an episode of malaria. She had been living in Italy for a few months. Proteinuria at dipstix was +++ and renal function was normal.
A few days after the visit in our center she presented to the Emergency Department because of acute renal failure (Serum Creatinine-SCr- was 1.8 mg/dl).
She was hospitalized in our Nephrology Department. Physical examination showed bilateral leg edema.
Laboratory examinations confirmed a severe nephrotic syndrome (proteinuria 16.8 g/day, serum albumin 2.3 g/dl, total serum proteins 4.8 g/dl). Renal function was worsening (SCr increased in few days from 1.8 mg/dl to 5.8 mg/dl). No monoclonal components were detected neither in serum nor in urine. IgA were 110 mg/dl, IgG 650 mg/dl, IgM 45 mg/dl.
Leukocytes were 8830/mm3, hemoglobin 16.4 g/dl, platelets 342000/mm3, coagulation and liver enzymes were normal. Electrocardiogram, abdominal Ultrasound, Chest X-Ray were normal.
The patient underwent a renal biopsy, which showed 22 glomeruli, one with global sclerosis. Glomerular basement membranes were thin, as were the mesangial axes. No pathologic alterations could be detected as regards the interstitium and the vessels. Immunohistochemical examination was negative. Search for anti-phospholipase A2 receptors on renal tissue resulted negative at immunofluorescence.
Minimal change disease was diagnosed and a regimen of 3 methylprednisolone 750 mg pulses followed by corticosteroid 1 mg/kg/day (50 mg/day) was started.
Renal function normalized in 30 days. Proteinuria was 0.3 g/day at the 6th week. Corticosteroid tapering was started after the 8th week. Fourteen days later proteinuria was again 21 g/day and corticosteroids were increased to 1 mg/kg/day; full dose was maintained for a longer time (6 months). Proteinuria completely disappeared a few days after the increase in corticosteroid doses. Six months later, slower tapering of corticosteroids was started. Four months later, at a dose of prednisone 25/5 mg every other day, proteinuria relapsed again (2.1 g/day).
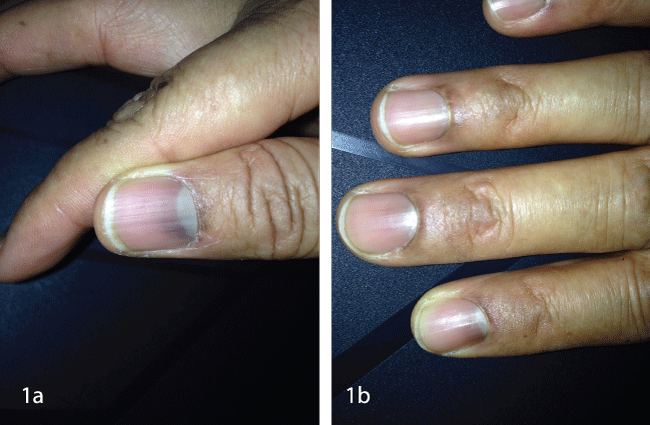 Figure 1: The first picture of the patient's nails was taken at day 15th after the beginning of CyF treatment. View Figure 1
Figure 1: The first picture of the patient's nails was taken at day 15th after the beginning of CyF treatment. View Figure 1
The patient was then given CyF 2 mg/kg/day (100 mg/day). At day 15th after the beginning of CyF she complained of her nails turning to a blue color (Figure 1a and Figure 1b), which became complete and diffuse at day 30th (Figure 2a and Figure 2b). CyF was discontinued after 90 days. The discoloration of the patient's nails progressively disappeared and 5 months later her nails were normal again (Figure 3).
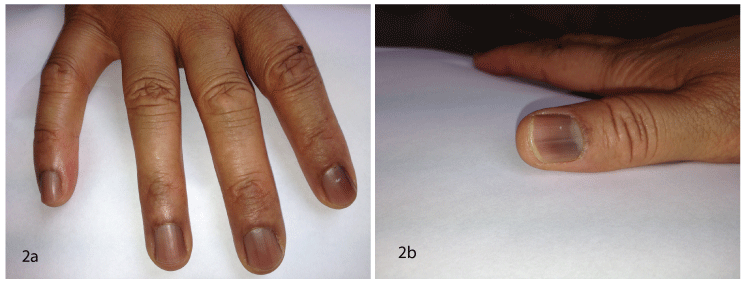 Figure 2: The picture was taken at day 30th of CyF therapy. View Figure 2
Figure 2: The picture was taken at day 30th of CyF therapy. View Figure 2
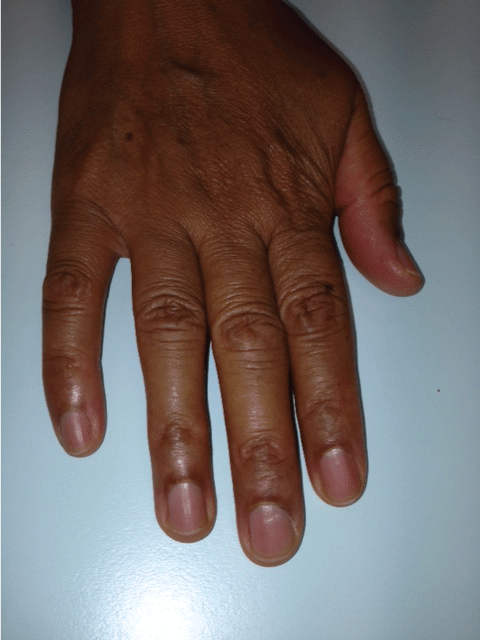 Figure 3: The last picture was taken when the blue color completely disappeared at the 5th months after CyF discontinuation. View Figure 3
Figure 3: The last picture was taken when the blue color completely disappeared at the 5th months after CyF discontinuation. View Figure 3
The change of nail color with appearance of a blue-gray pigmentation is reported in some clinical conditions, such as HIV [6,7], but it is much more frequently associated to some drugs, such as gefitinib [8], sparfloxacin [9], azidothymidine [10], hydroxyurea [11], imipramine [12], minocycline [13,14].
The coloration of fingernails is an extremely rare side effect of cyclophosphamide. Only a few reports are found in a literature search [3-5], regarding oncologic patients treated with high doses of this drug.
Dave [3] reported the case of a woman who developed a pigmentation involving only the nails of the thumb, index finger and half the middle finger of both hands 8 months after a regimen with monthly pulses of 500 mg CyF i.v. plus dexamethasone for pemphigus vulgaris.
Kumar, et al. [4] reported a patient who developed a pigmentation of his nails after six cycles of CyF, methotrexate, and 5-flourouracil chemotherapy for breast cancer. The nail pigmentation involved all the nails of both hands and feet except the second and third toenails of her right foot.
Harrison, et al. [5] observed the same effect in a 3-year-old boy given CyF at a dosage of 80 mg/day, and discontinued the drug because of acute hemorrhagic cystitis after one month. The pigmentation developed at the base of the finger and toe nails, and there was also a brown line on the teeth at the junction with the gums. The changes in the teeth persisted, but those in the nails grew out.
In our patient the blue pigmentation appeared progressively starting at day 15th after the start of CyF treatment, and diffusing from the proximal to the distal part of the nail. It became diffuse to all fingernails in one month, and progressively disappeared after the discontinuation of the drug, being completely solved after 5 months.
The causes of this pigmentation are still unknown. The mechanisms proposed are genetic predisposition, toxic effect on the nail bed and matrix, photosensitization and focal stimulation of melanocytes in the matrix [3]. Melanogenesis in the nail matrix melanocytes varies with the intensity of the cutaneous pigmentation, and is more common in dark people (our patient had mild dark skin color).
In conclusion, pigmentation of the nails is a side effect of CyF which may arise in short time and may completely disappear leaving no signs.