Silver-Russell syndrome is characterized by decreased intrauterine and postnatal growth, facial dysmorphia (triangular face), clinodactyly of the fifth finger, eating problems and body asymmetry, with a frequency of 1:50,000 to 1:100,000 live births [1-3].
There are reports of rare familial cases with dominant autosomal, recessive autosomal and/or linked to the X and also of unknown etiology. It is observed that 10% of the cases have identified maternal disomy of chromosome 7 and the loss of methylation in imprinting region of chromosome 11p15 [1-3].
For most affected individuals, it represents a phenotype rather than a specific disorder. The diagnosis is therefore mainly based on the identification of consistent clinical features, especially prenatal and postnatal growth retardation with normal head circumference. Facial characteristics are detected from birth and the delay in the closure of the anterior fontanelle is common. Usually, patients are small for gestational age, remaining below the 3rd percentile of the growth curve. In some cases, hypoglycemia, excessive sweating, variation in the sexual development pattern, including elevated levels of serum and urinary chorionic gonadotrophin, may occur in the pre-pubertal phase. Therefore, pubertal development may appear before psychological maturity, especially in females. In addition, there is a delay in motor development, but most of the children affected by the syndromes have normal intelligence, although there are reports of learning difficulties. The growth rate is normal, but the average adult height is 151.2 cm (male) and 139.9 cm (female). Other symptoms are associated with gastrointestinal symptoms and include gastroesophageal reflux disease, esophagitis, food aversion and inability to progress food. Reflux esophagitis should be suspected in food aversion or aspiration. Furthermore, there are hypospadias and cryptorchidism. Renal anomalies, including hydronephrosis, renal tubular acidosis, posterior urethral valves and horseshoe kidney have been already reported [3,4].
Considering the morphological characteristics of the syndrome, it could be assumed that obstetric problems may be common in these patients, such as preterm labor, pelvic dystocia, recurrent abdominal pain, intrauterine growth deficit, and worsening of common gastrointestinal symptoms in pregnancy (vomiting, nausea, reflux) and recurrent urinary tract infection, however, data on pregnancy in these patients are scarce in the literature, which led to the description of this clinical case. Based on the above, the authors present the case of a pregnant woman carrying the Silver Russel Syndrome accompanied in a high-risk prenatal regimen.
WFNS, 25, with Silver Russel Syndrome, referred to the high-risk prenatal service after emergency care with complaints of abdominal pain. The diagnosis was made in childhood using larger and smaller criteria, as described in the medical literature [2]. The identification of corporal asymmetry, prominent forehead, triangular face, intrauterine and postnatal growth deficit was responsible for its diagnosis. At the moment, in the adult phase, corporal asymmetry, prominent forehead and triangular face are still identified with ectoscopy.
She started prenatal care at 29 weeks of gestation. Laboratory tests of the prenatal routine without any change. She was a secondary pregnancy (a previous cesarean section), hemodynamically stable, short stature (139 cm), initial weight of 37.2 kg. Initiated iron replacement, in the dosage of 60 mg/day of elemental iron, in the form of ferrous sulfate.
It evolved with elevated blood pressure levels in pregnancy, without associated proteinuria, being classified as gestational hypertension, with control through rest. Abdominal pain was constant throughout the pregnancy, with worsening in the third trimester, motivating several emergency services, but without uterine contractions or cervical changes (dilatation and erasure), not characterizing preterm labor. There was a good parameter of fetal growth evaluated clinically and by obstetric ultrasonography. It was decided to perform the interruption of pregnancy with 39 weeks by caesarean section, with extraction of the live fetus, with good evolution, without anatomical changes, being discharged after 48 hours of hospitalization. The child presented good growth pattern, having normal development for the current age.
Despite abnormalities in sexual development, which may be associated with Silver- Russell syndrome, such as precocity at menarche, acquisition of secondary sexual characteristics, and maturation of the vaginal mucosa, while there is a mismatch between bone and chronological ages, fertility is usually not compromised, mainly in the female sex. Thus, the patient presented spontaneous pregnancy [1-3].
The major problem of SSR is the body asymmetry and short stature that can determine obstetric complications for vaginal delivery. Cephalopelvic disproportion (CPD) is believed to occur due to short stature and narrow pelvis. Maternal height below 155 cm (61.02 in has been considered an obstetric risk factor for dystocia and evolution for cesarean section. A study carried out in Thailand, considering a cut of 145 cm, found that short stature was significantly associated with a higher rate of CPD (OR = 2.4; CI = 1.8-3.0), even controlling variables such as birth weight, parity and obstetric care [4]. However, other studies have not verified a higher frequency of PWD in low-height parturients, and some authors believe that maternal height should be associated with other anthropometric diameters, especially the maternal pelvis to predict CPD [5]. However, in this case, the cesarean section was chosen not only for the height of this patient (139 cm), but also for the asymmetry of the lower limbs, which could cause difficulty in limb abduction during the expulsive period (Figure 1).
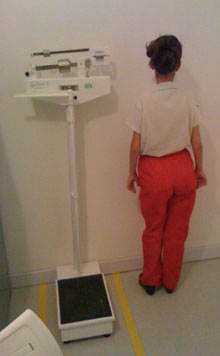 Figure 1: Body asymmetry and growth deficit: Low stature (139 cm) is associated with asymmetry of lower limbs. In this case, the right leg is shorter than the left. The triangular face and the prominence of the forehead.
View Figure 1
Figure 1: Body asymmetry and growth deficit: Low stature (139 cm) is associated with asymmetry of lower limbs. In this case, the right leg is shorter than the left. The triangular face and the prominence of the forehead.
View Figure 1
Despite reports of eating difficulties in SSR, the patient did not present any gastrointestinal changes, since the pregnancy itself increases symptoms such as nausea, vomiting and reflux, with adequate weight gain and uterine height with fetal growth compatible with the usual. Ultrasound examinations have not identified a fetus with restricted intrauterine growth or identifiable deformities. The weight of the newborn was also considered normal, so that patients with SSR may have normal children. Thus, these patients should receive obstetric care in specialized services, aiming the screening of fetal growth deficit, adequate assessment of the maternal pelvis for the decision on the best way of delivery. This way, it is suggested that the cases be individualized considering the variety of phenotypic manifestations that the syndrome presents. Caesarean section should be considered in patients with important body asymmetries associated with short stature.