Patent Blue Violet dye is commonly used for selective localization of the lymphatic system before sentinel lymph node biopsy. This procedure is routinely recommended for staging the axilla in early breast cancer. However, it has long been recognized that such dye is associated with anaphylaxis. Here, we present a case of an intraoperative grade 2 anaphylaxis which commenced 20 minutes following the subcutaneous periareolar injection of patent blue for sentinel lymph node detection during segmental mastectomy. The timing of the reaction, clinical signs, and results of skin testing confirm patent blue to be the triggering agent.
Anaphylaxis, Patent blue dye, Anesthesia, Lymph node biopsy
Sentinel lymph node detection and biopsy have become the standard of care for the most accurate staging of breast cancer. Patent Blue Violet (PBV) dye, and its derivative isosulfan blue, are often used for this procedure, in Europe and the USA, respectively. Methylene blue dye is less frequently used. Although rare, allergic reactions to PBV dye can occur unexpectedly, and with unpredictable severity. The objective of this paper is to present an uncommon case of intraoperative allergic reaction after subcutaneous periareolar injection of PBV dye, and to demonstrate that this event is not that simple and needs more extensive and dedicated evaluation.
Patient consent was obtained for publication of this case report.
A 40-year-old, 70 Kg, ASA physical status 1 female was admitted for elective excision of a left breast cancer with concomitant sentinel lymph node localization by patent blue dye. She reported no known drug allergies, no previous use of Patent Blue dye, and she had never experienced allergic contact dermatitis with cosmetics. Her vital signs were within the normal range, and her basic laboratory results were unremarkable.
General anesthesia was induced and maintained using propofol 200 mg, cis-atracurium 10 mg, remifentanil, midazolam 2 mg, ketamine 15 mg, sevoflurane (1.5-2%) and O2/Air (50/50%). Antibiprophylaxis was provided by 2 g of cefazoline intravenously (IV). To prevent postoperative nausea and vomiting, dexamethasone 4 mg, and ondansetron 4 mg IV were given.
After disinfecting the surgical field with povidone-iodine (Betadine®), 3 ml of 2.5% aqueous solution of patent blue V Guerbet diluted to 5 ml with normal saline was injected into the retroareolar area, and then the breast was massaged for 5 minutes.
Twenty minutes after PBV injection, she developed peripheral arterial desaturation (SPO2 = 94%), arterial hypotension (a decrease from 123/65 to 95/50 mmHg), tachycardia (from 80 to 110 beats/min), and diffuse severe blue urticaria all over her body and along the inferior mastectomy skin flap (Figure 1 and Figure 2). No bronchospasm was noted. At this time, our hypothesis was that patent blue dye may have caused the anaphylactic reaction. Sustained improvement was achieved with the administration of intravenous bolus of 10 µg of epinephrine, 200 mg of hydrocortisone, and aggressive fluid resuscitation with 500 ml of crystalloids (0.9% Saline's solution) and 500 ml of colloids (Voluven®) over a period of 20 minutes. She was extubated in the operating room at the end of the surgical procedure without evidence of angioedema, stridor, or respiratory compromise. The patient was observed for 48 hours on the ward, and was given hydrocortisone (100 mg ± 3/day), cetirizine (Allergica®), and famotidine. The subsequent course was uneventful. Delayed anaphylaxis was not observed, but skin and urine blue discoloration persisted. The patient was discharged home on postoperative Day 3.
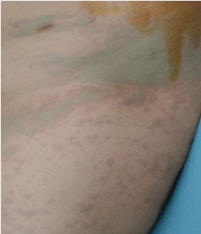 Figure 1: Bluish urticarial-like plaques on the abdomen and lower limbs.
View Figure 1
Figure 1: Bluish urticarial-like plaques on the abdomen and lower limbs.
View Figure 1
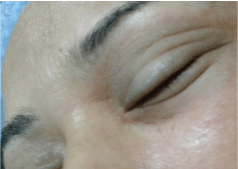 Figure 2: Blue swollen eyelids.
View Figure 2
Figure 2: Blue swollen eyelids.
View Figure 2
Blood-gas analysis revealed that partial oxygen pressure (PaO2) and arterial saturation (SaO2) were within the normal range (200 mmHg and 99%, respectively).
The serum mast-cell tryptase (MCT) levels, measured 2 hours after the clinical reaction and at baseline (48 hours after the event), were in the normal range (2.6 and 1.5 µg/L respectively; normal < 11 µg/L).
With the patient's consent, subsequent assessment by skin testing using standardized procedures was performed 6 weeks later. The skin-prick test (SPT) to PBV dye showed a 4 mm positive reaction (Figure 3), and negative response to all additional drugs received at the time of the procedure (Propofol, Remifentanil, Cis-atracurium, Ketamine, Midazolam, Cefazoline, Ondansetron). SPTS to latex, and methylene blue dye are also negative (Figure 4).
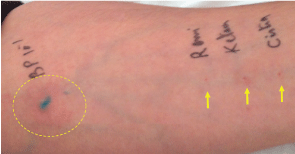 Figure 3: Positive skin prick test to Patent blue V.
View Figure 3
Figure 3: Positive skin prick test to Patent blue V.
View Figure 3
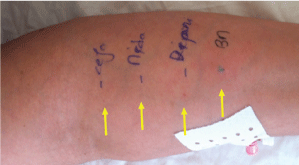 Figure 4: Negative SPT to methylene blue dye and additional drugs.
View Figure 4
Figure 4: Negative SPT to methylene blue dye and additional drugs.
View Figure 4
In this case, the clinical history is consistent with anaphylaxis. Indeed, skin prick tests are positive to PBV, and negative to all other drugs used, and to latex. On the balance of probabilities, PBV is the most likely causal agent for the anaphylactic reaction.
Sentinel lymph node biopsy (SLNB) is an established technique for early staging of the axilla in clinically node-negative patients with breast cancer. This procedure removes the need for systematic axillary lymph node dissection, and thus allowed to reduce perioperative and lifelong morbidity [1].
Several blue dyes, with or without isotope, are widely used for sentinel lymph node detection. Their accuracy for SLN localization is comparable [1]. Patent blue violet is the most frequently used blue dye in Europe, and isosulfan blue (an isomer of patent blue) in the USA. Methylene blue dye is less frequently used [1].
Historically, numerous dyes have been used to understand the mechanisms driving allergic responses in animal models for almost a century. They allow to monitor changes in vascular permeability that occur due to mast cell IgE cross-linking and histamine release. Evans Blue dye is currently the standard dye utilized for measuring allergic responses in the skin. It pools where edema collects, and so, help to quantify localized allergic responses, and to visualize hives [2].
During general anesthesia, the most frequently incriminated allergic substances are neuromuscular blocking agents, followed by antibiotics and dyes [3]. In most cases, clinical symptoms of hypersensitivity reactions occur immediately or within minutes of intravenous administration of treatments. When symptoms are delayed and occur during the surgical procedure, a reaction involving latex, a vital dye, an antiseptic or a volume expansion fluid should be suspected [3]. Hypersensitivity to PBV, which is administered subcutaneously or intradermally by the surgeon, has a late onset (10 to 45 min after the dye injection) [4,5]. In our case, the delay of 20 minutes before the onset of anaphylaxis is explained by the slow reabsorption from subcutaneous injection of PBV.
Outside medicine, vital dyes are used in cosmetics, textiles, and as a food colorant (E 131). Since these reactions can arise on the first medical exposure, it is thought that the widespread use of PBV potentially exposes the general population to the risk of allergic sensitization, leading to unpredictable hypersensitivity reactions [6].
Allergic reactions to blue dyes are not that simple, and needs more extensive and dedicated evaluation. To readily diagnose anaphylaxis can be particularly difficult under general anesthesia because hypotension is a common side effect of many drugs administered intraoperatively. On the other hand, the anesthetist is faced with the problem of polypharmacy, where several drugs need to be administered in quick succession. This can make subsequent identification of the causative allergen difficult [3]. For best patient outcome, however, treatment of anaphylaxis must be immediate and aggressive.
Allergies to PBV dye are normally associated with increased serum histamine, IgE, and tryptase levels. Hence histamine has a short elimination half-life (15-20 min), immediate sampling is recommended [7]. Serum tryptase has a peak plasma level within an hour and remains high for 6 hours. To compare the concentrations during an immediate reaction with baseline levels, a tryptase measurement must be performed after > 24 hours following a reaction or when the patient is referred for investigation [8]. Tryptase may not be increased in mild reactions, like in our case. Its absence does not preclude the diagnosis of IgE-mediated anaphylaxis [7,8].
Skin tests (Skin Prick Test (SPT) or, mainly, intradermal tests) should be performed as suggested by the clinical history, and at least 4 to 6 weeks after an anaphylactic reaction to avoid false negative results [8]. Because many different agents are used in the perioperative period, it is always important to investigate all drugs and substances to which the patient was exposed.
In our case, blue hives and urine discoloration occurred, and persisted for 72 hours. It has been observed that, after the intradermal or intraparenchymal injection, patent blue is taken up by the lymphatic vessels from draining area, binds to albumin, and two thirds are absorbed in the first hour while the totality in 24 h. It is excreted in the urine and bile, and the patient urine may turn blue for up to 24 hours [8].
One of the most common drawbacks seen with the use of patent blue is interference with wavelength reading used to measure the oxyhemoglobin. It leads to factitious transient desaturation in digital pulse oximeter, without changes in arterial blood gas analysis values [9]. Latency of desaturation observed in our patient, is due to the site of injection of patent blue (subcutaneous). Intravascular injection causes an immediate drop in oxygen saturation [9]. Anesthesiologist should be aware of this dye and its interference with pulse oximetry, and our case report proves that point.
Although anaphylaxis usually presents as an acute episode, mast cells can release mediators hours after the initial reaction causing, a biphasic or late phase reaction in up to 10%. Sub-sequent episode of hypotension related to these biphasic and protracted cases can occur between 6 and 8 hours after the initial event. Patients should be monitored during this period, even if hemodynamically stable [10].
The grade II reaction observed in our patient may be explained by the low volume of PBV used (3 ml of diluted PBV), and the early administration of intravenous steroids (4 mg of dexamethasone) used to prevent nausea and vomiting.
The amount of dye used for SLN biopsy is not standardized. In a prospective analysis, King, et al. found that the success rate of detection of the sentinel lymph node did not differ depending on the amount of dye used and observed a higher rate of allergic reaction with increased dye volumes [11].
To the best of our knowledge, there are no unified consensus/guidelines on premedication plans to prevent perioperative anaphylaxis to PBV. It was found that pre-operative antiallergic medication does not significantly decrease the incidence of overall anaphylactic reactions but markedly reduce the severity of adverse events [12]. Despite the lack of evidence regarding their preventative effects, pretreatment with empiric protocol "100 mg of hydrocortisone or, 4 mg of dexamethasone +50 mg of diphenhydramine (H1 anti-histamines) +20 mg of famodine (H2 blockers) intravenously before patent blue injection" continues to be routinely recommend by many providers [13].
Allergic reactions were consistently reported more frequently for patent blue V, compared to methylene blue [13]. Cross-reactivity between the two dyes has been reported [13]. In our case, SPT to methylene blue is negative, suggesting that the dye may represent a safer alternative to PBV dye in SLN biopsy if indicated again in our patient. However, methylene blue is not the most effective dye for SLN localization based on its chemical structure, and the safety profile of this agent is contested by some authors [14].
Sentinel lymph node detection and biopsy is a major advance in the treatment of early breast cancer. Although rare, physicians must remain constantly vigilant for the potential risk of anaphylactic shock to blue dyes used for this procedure. Appropriate and immediate recognition of such adverse events is critical to proper management. This risk must be explained to patients when seeking consent for surgery. A follow-up assessment is of utmost importance to confirm the trigger for anaphylaxis, prevent recurrences, and define alternatives in case of future procedures.
There is equal author's contribution. There are no direct or potential conflicts for any of the authors involved in this manuscript.