Osteoclast-like giant cells have been reported in variety of different tumor types including breast carcinoma, pancreatic carcinoma, ovary tumor, uterine leiomyosarcoma, hepatocellular carcinoma, renal cell carcinoma. To the best of our knowledge, there are only two previous case reports in the literature showing endometrial stromal sarcoma with osteoclast-like giant cells. Endometrial stromal sarcoma is a rare uterine malignant neoplasm and includes low grade and high grade types. Here, we report a case of high grade endometrial stromal sarcoma with osteoclast-like giant cells. A 54-year-old female presented with a recent history of postmenopausal bleeding, a subsequent computed tomography scan revealed a large uterine/pelvic mass. Histologic examination revealed a malignant spindle cell neoplasm with tumor necrosis and some areas with clusters of osteoclast-like giant cells interspersed in the tumor. The neoplastic spindle cells were positive for CD10 and cyclin D1, negative for desmin, caldesmon and SMA. The osteoclast-like giant cells were also diffusely positive for cyclin D1.
Endometrial stromal sarcoma, Osteoclast-like giant cells, Cyclin D1
Endometrial stromal sarcomas are rare uterine neoplasms arising in the uterine corpus. Currently, endometrial stromal sarcomas are further separated into low and high-grade subtypes. Low grade endometrial stromal sarcoma is distinguished with its low mitotic activity and its resemblance to typical endometrial stroma [1]. In contrast, high grade endometrial stromal sarcoma has pleomorphic cells with vesicular nuclei and prominent nucleoli [2]. Immunohistochemical staining is very helpful in distinguishing these tumors. Low grade endometrial stromal sarcoma will stain for CD10, ER, and PR [3]. The high-grade subtype is typically negative for these markers and curiously also displays positivity for cyclin D1 [2].
Osteoclast-like giant cells have been reported in an extremely wide variety of different tumor types including melanoma [4], breast carcinoma [4], pancreatic carcinoma [5], ovary [4], uterine leiomyosarcoma [6], hepatocellular carcinoma [4], urothelial carcinoma [7], renal cell carcinoma [4], osteosarcoma [8], and lung carcinoma [4]. While the significance and cause of this phenomenon is poorly understood, recent studies have shown that expression of chemotactic factors by the tumor may be necessary to attract these giant cells [6,8]. Here we report a case of high grade endometrial stromal sarcoma with osteoclast-like giant cells. To the best of our knowledge, only two previous case reports of endometrial stromal sarcomas with osteoclast-like giant cells are present in the literature [9,10].
Our report is of a 54-year-old female with a 1.5-month history of postmenopausal bleeding. The patient had been postmenopausal for 7 years (since 2010) but noted new vaginal bleeding. The patient also began experiencing severe pelvic and abdominal pain, as well as difficulty with urination. She went to an outside hospital and a CT scan revealed findings concerning for metastatic uterine cancer. In addition to a large 15 cm pelvic mass, the CT scan also revealed right hydronephrosis and bibasilar pulmonary lesions. The patient was subsequently taken to the operating room. Vaginal examination revealed the cervix to be completely replaced by mass. A bladder scope revealed the mass extended to the bladder but did not ulcerate through the mucosa. Biopsies of the mass were taken and sent to pathology, revealing a malignant spindle cell neoplasm.
A hysterectomy was performed a few days later. The uterus, cervix, and bilateral tubes and ovaries were received into surgical pathology. A large 11 cm mass lesion was identified located in lower uterine segment and the posterior uterine wall that extended through the serosal surface. The mass did not appear to involve the cervix, tubes, or ovaries. Sections of the tumor revealed sheets of atypical spindle cells arranged in short to medium fascicles. Areas of tumor necrosis were present with edema and hemorrhage. The spindle tumor cells had moderate eosinophilic to amphophilic cytoplasm, with indistinct cell borders (Figure 1A). The nuclei were mostly round to oval in shape. The tumor nuclei were vesicular with 1-2 prominent nucleoli. The tumor cells demonstrated frequent mitoses as many as 37/10 high power fields. Interestingly, there were some areas with clusters of large, osteoclast-like giant cells (Figure 1B) present inside the tumor (involving 10% of the total tumor). Immunohistochemical staining revealed the spindle tumor cells positive for CD10 (Figure 1C) and cyclin D1 (Figure 1D). Additional stains for AE1/AE3, Caldesmon, Desmin, SMA, CD34. CD117. BCL-2, beta-catenin, ER, and PR were negative. The osteoclast-like giant cells were positive for CD68 (Figure 1E), supporting a histiocytic origin. The giant cells were also positive for cyclin D1 (Figure 1F).
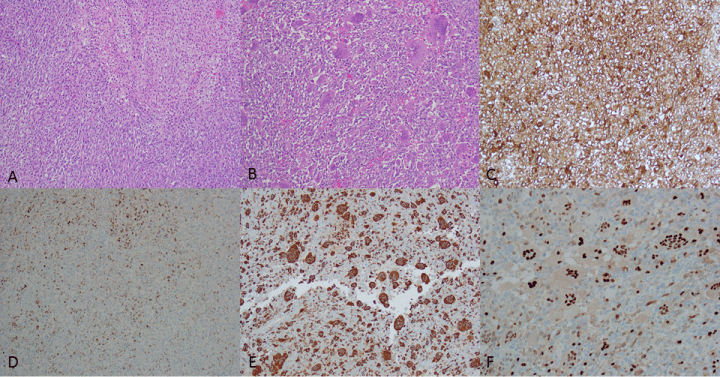 Figure 1: H&E section of the malignant spindle cells (Figure 1A, 100X) and area admixed with osteoclast-like giant cells (Figure 1B, 100X); The spindle tumor cells positive for CD10 (Figure 1C, 100X) and patchy positive for cyclin D1 (Figure 1D, 100X); the osteoclast-like giant cells positive for CD68 (Figure 1E, 100X) and cyclin D1 (Figure 1F, 100X). The positive and negative controls for immunohistochemistry were adequate. View Figure 1
Figure 1: H&E section of the malignant spindle cells (Figure 1A, 100X) and area admixed with osteoclast-like giant cells (Figure 1B, 100X); The spindle tumor cells positive for CD10 (Figure 1C, 100X) and patchy positive for cyclin D1 (Figure 1D, 100X); the osteoclast-like giant cells positive for CD68 (Figure 1E, 100X) and cyclin D1 (Figure 1F, 100X). The positive and negative controls for immunohistochemistry were adequate. View Figure 1
During pathology gross examination, the large mass was located at the lower uterine segment but did not involving the uterine cervix, which was different from the clinical impression of large uterine cervix mass. The cause of this discrepancy is more likely to be the large tumor mass located at the lower uterine segment made clinical impression of cervical mass. The clinical differential diagnosis includes large leiomyoma, leiomyosarcoma, endometrial stromal sarcoma and carcinosarcoma. The differential diagnosis of the histology includes leiomyosarcoma, high grade endometrial stromal sarcoma, carcinosarcoma with sarcoma overgrowth, and undifferentiated uterine carcinoma. The negative pankeratin AE1/AE3 rules out carcinosarcoma and undifferentiated uterine carcinoma. The positive CD10 and negative smooth muscle markers (Caldesmon, desmin and SMA) make the leiomyosarcoma unlikely and support the diagnosis of high grade endometrial stromal sarcoma.
Although endometrial stromal sarcoma is a rare tumor, a variety of different histological features have been described [11-13]. These features range from relatively common (sex-cord like pattern, fibromyxoid pattern) to rare (skeletal muscle differentiation, ossification, rhabdoid features) [9]. Only two previous case reports describe the presence of osteoclast-type giant cells in association with these tumors [9,10]. It appears that chemotactic factors expressed by the tumor itself may be responsible for attracting these giant cells. One such factor, receptor activator of nuclear factor kappa-β ligand (RANKL), has been shown to be highly expressed in another case of uterine sarcoma with osteoclast-like giant cells [6]. Additionally, the expression of cyclin D1 has been shown to be upregulated in osteoclast-like giant cells [14,15]. Cyclin D1 expression has also been shown to be associated the formation of giant cells in some studies, including multinucleation and increased chromosome content [15]. Owing to the extremely small sample size, it is currently unknown if this histologic variation has any clinical or treatment consequences. It is our hope that this article inspires future reporting of the rare variation, and that eventually enough data is collected to make effective treatment decisions for the affected patients. We also believe it is very useful to describe histologic variations to avoid inappropriate diagnosis, and perhaps shed more light on the tumor's biological makeup.
Endometrial stromal sarcoma with osteoclast-like giant cells is a rare histologic variant of endometrial stroma sarcoma, and this is the third reported cases in the literature. The significance of the osteoclast-like giant cell component is not clear, and the cyclin D1 expression in the osteoclast-like giant cells may contribute to the giant cell formation.