Adenomyosis is a rare cause of chronic pelvic pain or severe dysmenorrhea that presents in the adolescent population. Here we describe an 18-year-old nulliparous woman who presented with a history of severe and worsening dysmenorrhea with cramps and increased menstrual flow since the menarche occurred 4-years-ago. A magnetic resonance imaging (MRI) described a poorly defined junctional zone of the endometrium, suggestive of adenomyosis, associated with the discrete heterogeneity of the adjacent myometrium. The patient underwent a course of GnRH agonists for 6 months, followed by continuous combined oral contraceptives (COC) pills with pain resolution. In this population, fertility preservation is a goal and therefore initial therapy for focal adenomyosis involves hormonal suppression with COC.
Adenomyosis, Pelvic pain, Dysmenorrhea, Adolescent
Adenomyosis is a benign condition of the uterus defined by the presence of endometrial glands and stroma > 2.5 mm in depth in the myometrium and a variable degree of adjacent myometrial hyperplasia, causing globular and cystic enlargement of the myometrium, with some cysts filled with extravasated, hemolyzed red blood cells, and siderophages [1,2].
Cystic adenomyosis can be present in both an adult form, which is present in 5-7% of hysterectomy fibroid uteri and often associated with the diffuse subtype, and in a juvenile form seen in nulliparous women between 13 and 20 years of age, for which the true incidence is not known, since few cases have been reported. Although adenomyosis seems very rare before age 20, a cystic form has mainly been reported in young women [3,4].
A variant of adenomyosis that seems specific to young women is called myometrial cystic adenomyosis, in which young patients present with nonresponsive severe dysmenorrhea. Adenomyosis was commonly thought to be a condition confined to adulthood, with limited clinical cases in adolescents, but can be a cause of primary dysmenorrhea in this population. However, further research is needed in adolescent girls, particularly those whose pain is refractory to treatment with non-steroidal anti-inflammatories (NSAID) and/or combined oral contraceptives (COC) pills, to determine whether some cases of primary dysmenorrhea may actually be early stages of adenomyosis [5,6].
We report a case of primary dysmenorrhea in an adolescent with magnetic resonance imaging (MRI) revealing adenomyosis.
An 18-year-old nulliparous woman presented with a history of severe and worsening dysmenorrhea with cramps and irregular menstrual cycle with excessive bleeding since the menarche occurred 4-years-ago, these were insufficiently relieved by NSAID and COC. She reported having started using COC two-years-ago when her sex life began, and she never underwent surgery, had an abortion or suffer any trauma. Her family history is unremarkable.
Pelvic examination revealed a normal vagina, vulva and adnexae and a normal-sized anteverted uterus. Transvaginal ultrasound (TVUS) demonstrated a uterus of normal volume and irregular contours, homogeneous myometrium and endometrium and without change of thickness. Ovaries were enlarged at the expense of multiple follicles. A follow-up MRI obtained 1 month later described a poorly defined junctional zone of the endometrium, suggestive of myometrial cystic adenomyosis, associated with the discrete heterogeneity of the adjacent myometrium and, in addition, a small increase in the thickness of the posterior uterine wall (Figure 1).
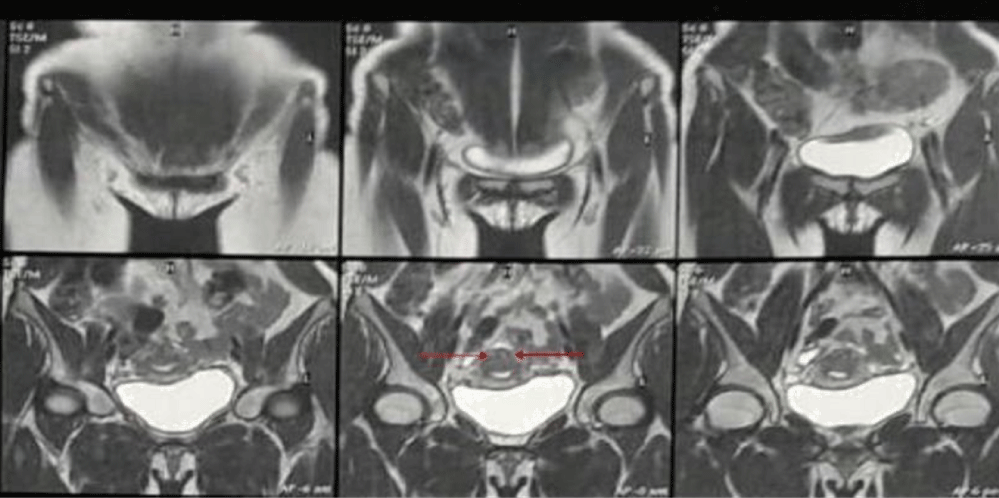 Figure 1: An asymmetric widening of the posterior junctional zone is shown in magnetic resonance imaging (MRI), with ill-defined border, presenting an elliptical shape and bright foci, with no mass effect on the endometrial cavity (arrows). View Figure 1
Figure 1: An asymmetric widening of the posterior junctional zone is shown in magnetic resonance imaging (MRI), with ill-defined border, presenting an elliptical shape and bright foci, with no mass effect on the endometrial cavity (arrows). View Figure 1
The patient underwent a course of GnRH agonists for 6 months, followed by continuous COCs with pain resolution.
This case demonstrates that adenomyosis is a rare but possible cause of dysmenorrhea and pelvic pain in adolescent patients, despite the disease being typically present in adult women in the third or fourth decade of life. Although endometriosis may be the most common cause of secondary dysmenorrhea in younger patients, adenomyosis should remain in the differential diagnosis [7].
Previous pathogenetic theories for adenomyosis have proposed that traumatization of the endometrial-myometrial interface, such as that caused by surgery or pregnancy may create a predisposition towards endometrial invasion of myometrium, and that local hyperestrogenism or dysperistalsis facilitates the process. However, evidence of adenomyosis early in reproductive life and in the absence of previous surgery or pregnancy suggests that invasion of endometrial tissue is not necessarily mediated mechanically; it may occur from endometrial-myometrial dysfunction [8]. Evidence shows that endometriosis and adenomyosis have in common an endometrial dysfunction involving both eutopic and heterotopic endometrium. Although anomalies are not identical, they share the common feature of leading to increased invasiveness. In both conditions, there is also a reaction of the inner myometrium that, although more pronounced in the case of adenomyosis, is nonetheless also present in endometriosis [6].
The symptoms of adenomyosis are variable and the proportion of women with adenomyosis who have abnormal uterine bleeding and/or painful symptoms, as was reported by the adolescent patient, is unclear. A consensus on the association between dysmenorrhea and adenomyosis is lacking, with some studies supporting this relationship, and others finding only a weak association [8].
Adenomyosis is a rare cause of chronic pelvic pain or severe dysmenorrhea in the adolescent population. For patients who have symptoms of dysmenorrhea or chronic pelvic pain refractory to NSAIDs or COC therapy, additional investigation with imaging may reveal this diagnosis as happened in this case. MRI is more indicated than TVUS, since it has shown potential superiority over TVUS in some situations, and because defined diagnostic criteria (Table 1) have made inter-observer variability less significant [9]. Although adenomyosis has traditionally been confirmed by histopathologic diagnosis from surgery, MRI can allow for accurate diagnosis of adenomyosis in most cases. Several studies have demonstrated sensitivity rates ranging from 70 to 88% and specificity as high as 91%. This is significantly better sensitivity and specificity of MRI compared with TVUS in the diagnosis of these abnormalities [9,10].
Table 1: Diagnostic criteria for adenomyosis in magnetic resonance imaging (MRI). View Table 1
Careful review of the literature reveals very few case reports, case series or small cohorts addressing adenomyosis or adenomyotic cysts presenting in the female adolescent [3,4,7,11,12]. A variety of imaging modalities were utilized in diagnosis. All cases presented with severe dysmenorrhea or pelvic pain, as reported by the patient in this case. In most cases, as in our patient and in the cases of two adolescents reported by Itam, et al. [7], the diagnosis was only made when patients did not respond to initial empirical treatment including the use of COC and NSAID.
Medical treatments for adenomyosis always follow the principles of the management of endometriosis, which are usually aimed at reducing the production of endogenous estrogen or inducing endometrial differentiation with progestins. Clinical evidence points to the clear and deleterious effect of uninterrupted ovulatory cycles on the development and persistence of adenomyosis. The objectives of medical treatment are the inhibition of ovulation, abolition of menstruation, and achievement of a stable steroid hormone milieu [2].
Both medical and surgical treatments offer opportunities for disease stabilization and regression. Initial therapy for focal adenomyosis involves hormonal suppression with COC, especially for the female adolescent in whom preserving fertility is paramount. Adolescents may represent a subset of patients with adenomyosis whose lesions are completely treatable with hormonal therapy [10].
For adenomyosis, the goal of therapy is important, and can include symptom relief and possibly increased fertility. The therapeutic goal of medical treatment is not lesion resorption: Lesions survive any drug, at any dose, for any period of use, and come back after treatment discontinuation. Therefore, treatment should be tailored to the specific symptom or the special request of the individual patient. The results from systematic literature reviews have consistently demonstrated that, if amenorrhea is obtained, there are no statistical differences between the various available drugs in terms of pain relief, but tolerability, side effects, and costs vary widely [2].
An example of drugs with higher costs and more troublesome side effects are GnRH agonists. They are very effective against adenomyosis related pain, and thereby also contribute to the occurrence of many successful pregnancies and deliveries, however their use is associated with frequent and intolerable hypoestrogenic side effects, including vasomotor syndrome, genital atrophy and mood instability, and the use of these drugs should be for a short period of time among adolescents who do not improve their symptoms with continuous use of COC, which is what happened in our case. GnRH agonists also have a negative impact on bone health and a possible negative influence on cardiovascular health [2].
Surgical management is necessary in cases where dysmenorrhea is medication resistant. Some authors argued in favor of the laparoscopic approach. Other surgical approaches have been proposed such as ablation after insertion of a radiofrequency needle under ultrasound guidance, the use of a single-incision with monopolar cautery or the use of robotic surgery. In the case of a focal lesion or adenomyotic cyst not involving the endometrial cavity, safe surgical resection is possible [4].
In conclusion, this case draws attention to a little known but not uncommon cause for both primary and secondary dysmenorrhea, which can affect young nulliparous women. MRI may be useful in establishing a diagnosis even when TVUS is normal. In this population, fertility preservation is the primary goal and, therefore initial therapy for focal adenomyosis involves hormonal suppression with COC. Further research is needed due to limited reports in the literature regarding management of adenomyosis in the adolescent.
The authors declare no potential conflicts of interest and no sources of support.
All authors equal contributed to the design and implementation of the research, to the analysis of the case and to the writing of the manuscript.