Ovarian tumors in adolescents are a medical challenge due to their rarity. The aim is to describe a case of adnexal disease in a girl with hot flushes after treatment. A 15-year-old girl presented a history of menstrual delay and progressive increase of abdominal volume. Initially, clinical suspicion was for pregnancy, but after abdominal magnetic resonance imaging, a solid-cystic abdominopelvic mass was revealed. She underwent laparotomy and pathologic evaluation revealed a bilateral ovarian dysgerminoma. Surgical menopause appeared one year after surgery and improved after hormone replacement. Ovarian cancer is rare in adolescence. Diagnosis, treatment and follow-up avoid further complications.
Adnexal diseases, Ovarian neoplasms, Premature ovarian failure
Ovarian tumors in the adolescent age group are a medical challenge due to their rarity and controversial management. The incidence of ovarian masses is estimated at 2.6 cases per 100,000 girls per year, and malignant ovarian tumors account for 0.9% of all childhood and adolescent malignancies [1,2].
Dysgerminoma is an ovarian tumor that is composed of primitive undifferentiated germ cells. It is the most common malignant tumor occurring in the ovary and these lesions are found most commonly in adolescents and young adults. Dysgerminoma is usually solid mass and grows rapidly; it is usually unilateral and tends to more frequently occur in the right ovary. Only 10-15% of cases have a bilateral involvement [3].
Advances in treating malignant diseases among adolescents have resulted in markedly improved survival rates. More than 70% of adolescents diagnosed with cancer can expect to be long-term survivors. However, with these advances, survivors now face the consequences of exposure to intensive multimodality therapies. Girls who are treated with chemotherapy, surgery, and/or radiation can potentially suffer the loss of the reproductive function. Premature menopause leads to the early and often unexpected loss of reproductive potential as well as the cessation of ovarian sex hormone production. Thus, adolescents who experience premature menopause are at increased risk of developing a variety of adverse health outcomes: Hot flushes, osteoporosis, accelerated atherosclerotic cardiovascular diseases and psychosexual dysfunction [4,5].
A 15-year-old girl presented with a history of amenorrhea, progressive increase of abdominal volume and pain in the lower abdomen beginning three months previously.
Menarche occurred at age 12 and since then she has had regular monthly menses and sexual activity began at age 14.
She sought a health facility for a suspected pregnancy and a serum level of human chorionic gonadotropin (βHCG) test was performed that was positive. Because the fetal heart sounds were not detected, she was referred to the emergency room, where during the physical examination a hardened abdominal mass with irregular contours occupying the whole abdomen was observed and was hospitalized for diagnostic clarification.
Abdomino-pelvic ultrasound examination revealed a solid abdominal mass, with somewhere cystic components, and Doppler revealed vascular masses with a volume of 3700 cc bilaterally. Abdominal magnetic resonance imaging (MRI) revealed a solid-cystic abdominopelvic mass, with probable origin in the left ovary, hypervascularity and causing mild bilateral hydronephrosis (Figure 1).
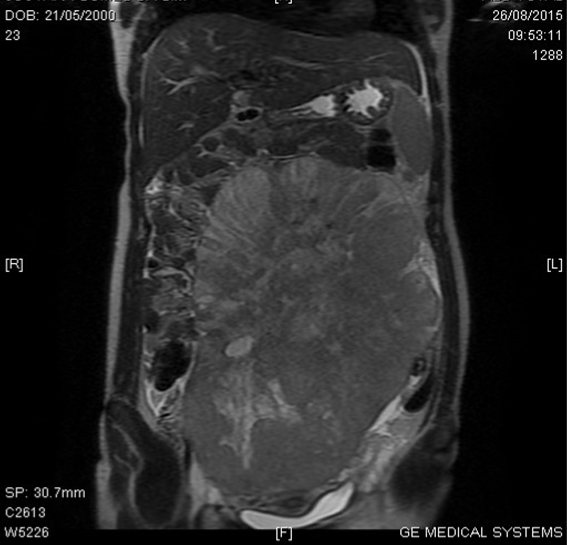 Figure 1: Pre-operative abdominal MRI scan picture, showing huge solid pelvi-abdominal mass. View Figure 1
Figure 1: Pre-operative abdominal MRI scan picture, showing huge solid pelvi-abdominal mass. View Figure 1
The imaging investigations pointed to suspicion of malignant ovarian tumor. Laboratory investigations were given in Table 1.
Table 1: Laboratory tests and tumor markers. View Table 1
Based on the clinical, imaging and elevated tumor markers findings, she was diagnosed with ovarian malignancy. She underwent exploratory laparotomy which revealed bilateral giant adnexal tumors (Figure 2). She underwent intraoperative evaluation with frozen/section and due to the diagnosis of dysgerminoma with peritoneal involvement, a total hysterectomy with bilateral oophorectomy, omentectomy, appendectomy, removal of peritoneal lesions, and para-aortic lymphadenectomy was done. She had good clinical evolution in the postoperative period and was discharged on the ninth postoperative day.
 Figure 2: Intraoperative picture showing both ovaries involved with a huge solid capsulated mass. View Figure 2
Figure 2: Intraoperative picture showing both ovaries involved with a huge solid capsulated mass. View Figure 2
The histopathological and immunohistochemical investigation of resected masses revealed bilateral dysgerminoma. The FIGO ovarian cancer staging was 3A.
Six months after surgery, she underwent adjuvant chemotherapy with bleomycin, etoposide, and cisplatin (BEP) for a period of three months.
After a year of surgical treatment, the girl sought gynecological care complaining of intense hot flushes, arthralgia, myalgia and vertigo. The evaluation by Blatt-Kupperman menopausal index presented a score of 25. She received a prescription for hormone replacement therapy (HRT) with transdermal estrogen and after 2 months of treatment underwent a reassessment with her score dropping to 11. Currently, she is being monitored in the climaterium outpatient clinic using HRT with significant improvement in her symptoms.
Malignant ovarian germ cell tumors (MOGCT) represent more than 50% of the cases of ovarian cancer in adolescence and more than 80% of the patients are aged 15 or less. Tumor markers are important for evaluating MOGCT for diagnosis and follow-up. They have been increasingly used for monitoring the clinical status of malignant germ cell tumors and among the most used are: Alpha-fetoprotein (AFP), βHCG, cancer antigen-125 (CA-125), lactate dehydrogenase (LDH) and carcinoembryonic antigen (CEA) [6]. Dysgerminomas, one of the types of MOGCT, have most commonly been associated with elevations in LDH and high serum hCG levels are present in 3% of cases. Moreover, elevations in AFP are even less common [6]. In our case, there were elevated levels of AFP, βHCG, LDH and CA-125.
The current standard management protocol for MOGCT is complete cytoreductive surgery followed by adjuvant chemotherapy, as in this case. However, just surgical treatment without adjuvant chemotherapy has recently been proposed for patients with FIGO stage 1 ovarian tumors [7,8]. In a study of 25 children and adolescents with a mean age of 12 years, Billmire, et al. [9] evaluated the surgery-only, watch-and-wait strategy and found that the overall oncologic outcomes were not impaired and 50% of the patients avoided having to take adjuvant chemotherapy.
The 5-year survival rate for childhood and adolescent patients after cancer treatment currently exceeds 80% because of the advances that have been made in cancer therapeutics. As a result of the increasing numbers of survivors, late health outcomes research has demonstrated that a significant proportion of survivors experience chronic health sequelae that result from complications of the disease or therapy. A prominent concern is the substantially elevated risk of ovarian dysfunction among female survivors who were treated with surgery and/or chemotherapy [10,11].
Evidently, bilateral oophorectomy results in premature ovarian insufficiency (POI) and counseling by a health professional is mandatory in view of the POI consequences, which can lead to symptoms that significantly affect the quality of life of adolescents, as seen in this case. HRT is indicated for the treatment of vasomotor and genitourinary symptoms in women with POI and to improve psychological, sexual and social effects of the premature surgical menopause among adolescents. It is also recommended to maintain bone health and prevent osteoporosis and may have a role in the primary prevention of cardiovascular disease [12,13].
Little data exists regarding the treatment regimens of adolescents with HRT. Treatment regimen proposed so far are empiric, and further studies are needed to establish: Optimal dosing in terms of safety and efficacy, long-term effect on bone, brain, and cardiovascular health, and the long-term risk of developing estrogen dependent cancers. Transdermal estrogen patch seems preferable because it doesn’t have the suppressive effect oral estrogens exhibit on both baseline and growth-hormone stimulated insulin-like growth factor-I (IGF-I) concentrations. Transdermal HRT was also reported to have a positive effect on serum lipid profiles, inflammatory markers, and blood pressure. Oral estrogen therapy increases renin substrate and the risk of hypertension [14]. In our case, clearly after the onset of HRT the adolescent had a marked improvement in the symptoms that made her seek professional help.
In adolescence, MOGCT are rare and can be confused with pregnancy as in this case. Early diagnosis and treatment based on the best evidence provide a high survival rate. Finally, adequate follow-up will allow for the diagnosis of sequelae of the disease or therapy, avoiding damaging consequences in the future of these adolescents.
The authors declare no potential conflicts of interest and no sources of support.
All authors equally contributed to the design and implementation of the research, to the analysis of the case and to the writing of the manuscript.