Cystic fibrosis (CF) is a multisystem disease that can have significant sinonasal manifestations. Viscous secretions are one of several factors in CF that result in chronic sinonasal pathology, such as sinusitis, polyposis, congestion, and obstructive crusting. Persistent discomfort and nasal manifestations of this disease significantly affect quality of life. Digital manipulation and removal of crusting by the patient in an attempt to alleviate the discomfort can have unforeseen damaging consequences. We present one such case and investigate other cases of septal damage secondary to digital trauma, as well as discuss the importance of sinonasal therapy in CF patients.
Septal perforation, Cystic fibrosis, Digital trauma, Rhinotillexomania, Nose picking
Cystic fibrosis (CF) is a systemic, inherited disease caused by mutations in the cystic fibrosis transmembrane conductance regulator gene that results in impaired anion transport, affecting the respiratory, exocrine, gastrointestinal, and reproductive tracts [1]. The impairment of ion transport results in impaired mucociliary clearance and characteristically viscous secretions, which acts as a nidus for inflammation, infection, and edema [2].
Involvement of the respiratory tract is a major cause of morbidity in this population, and upper airway involvement occurs in 90-100% of cases [3]. This disease can have profound effects on the nasal mucosa and paranasal sinuses [1,4]. Nasal symptoms in CF patients occur early, manifesting between 5-14 years of age, and represent a life-long problem in this population [5]. Patients with CF can develop thick nasal secretions contributing to chronic rhinosinusitis (CRS), nasal congestion, nasal polyposis, headaches, and hyposmia [6-8]. Sinonasal symptoms of CF are managed medically with topical agents and antibiotics, however surgery can be warranted due to the chronic and refractory nature of the symptoms, with 20-25% of CF patients undergoing sinus surgery in their lifetime [8].
Although sinus involvement is widespread in CF patients, one complication that, to our knowledge, has not been reported as a phenomenon is septal perforation from rhinotillexomania. Equally uncommon are reports of septal perforation in patients secondary to digital trauma (nose-picking). There have been a handful of reports of septal destruction resulting from habitual, aggressive digital trauma also known as rhinotillexomania (compulsive nose picking). These cases have been reported in the context of chronic nasal discomfort or psychiatric disease [9-11]. Septal perforation is traditionally associated with intranasal cocaine abuse, systemic rheumatologic disease, granulomatosis with polyangiitis, and glucocorticoid induced atrophy, among other causes [12-18]. Since this defect is commonly a manifestation of systemic disease, any patient presenting with idiopathic septal perforation merits thorough investigation into the etiology. We report a case of a 32-year-old woman with a history of CF presenting with facial pain and pressure whom was found to have obliteration of the nasal septum, extensive turbinate damage, lamina papyracea erosion, and partial ethmoidectomy secondary to digital trauma.
A 32-year-old woman with CF and a past medical history of seizures and depression presented to the rhinology clinic with facial pain and pressure. She was a former smoker who had been hospitalized three times in the last ten years for respiratory exacerbations of her chronic disease. Her CF was diagnosed at thirteen months of age by sweat chloride test (results of 102 and 108) and was confirmed by genetic testing (N1303K/F508del variant). She is managed at University Hospitals Pulmonary Cystic Fibrosis Clinic. Her lung function at presentation demonstrated a FVC of 3.01 L, a FEV1/FVC ratio of 59%, and an FEV1 of 51% of predicted value, consistent with severe disease. On initial presentation, she reported an extensive history of sinus discomfort, atopic disease, daily migraines, and recent fluctuations in her sense of taste and smell, as well as sleep disturbance, fatigue, throat clearing, itchy eyes, and epistaxis. Her only pulmonary symptom at that time was shortness of breath. The patient was using oral antihistamines, fluticasone spray, and routine saline irrigation to manage her symptoms, and had recently received a course of oral steroids and clarithromycin from an outside provider for acute sinusitis. Additionally, she was on tiotropium and albuterol aerosols, tobramycin nebulizer, a multivitamin, and enzyme replacement therapy including Pulmozyne and Pertzye. She denied nasal drainage, nasal airway obstruction, dysphonia, sneezing, or aspirin sensitivity.
Sinonasal endoscopy was performed and demonstrated a large septal perforation as well as the absence of the anterior aspect of the middle turbinate bilaterally without active polyposis or purulence. CT imaging showed sinuses consistent with left medial antrectomy, partial left ethmoidectomy, and bilateral middle turbinate resection, without evidence of polyposis, although this patient reported that she had never undergone sinus surgery. The septal perforation on the CT scan measured 21.6 mm in height and 27.4 mm in the anterior to posterior direction (Figure 1).
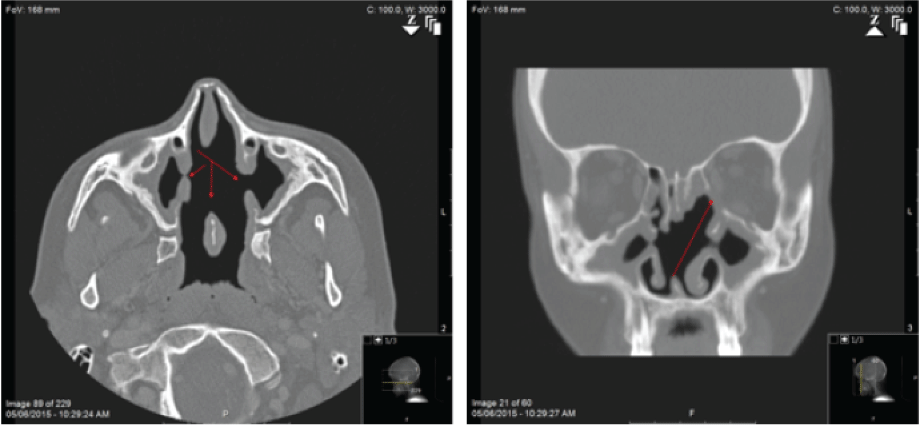 Figure 1: Computed tomography of septal perforation measuring 21.6 mm in the cranial to caudal direction and 27.4 mm in the anterior to posterior direction. View Figure 1
Figure 1: Computed tomography of septal perforation measuring 21.6 mm in the cranial to caudal direction and 27.4 mm in the anterior to posterior direction. View Figure 1
On further questioning, the patient stated that she used her fingers to chronically manipulate and pick her nose. She noted that after a period of time of digital manipulation, she was able to insert her finger on one side of her nose and manipulate the other side. She reported persistent irritation of her nose and manipulated it in order to obtain relief as well as to clear secretions and crusting. It was concluded that the changes seen on endoscopy and imaging were secondary to digital manipulation. Additionally, a diagnosis of CRS was made and the patient received a course of levofloxacin. The patient's condition did not improve and she later underwent surgical intervention with bilateral frontal sinusotomies, total ethmoidectomies, maxillary antorstomies with tissue removal, and sphenoidotomies with debridement of inflamed tissue and mucosa. The pathology report for the tissue obtained at the time of surgery showed evidence of chronic inflammation and did not show evidence of any rheumatologic disease process.
To our knowledge, there have been no documented reports of manual destruction of the nasal septum and turbinates in CF patients, or an increased prevalence of septal perforation in this population. Additionally, there are very few documented cases of extensive septal and turbinate destruction resulting from digital trauma, as was seen in this patient [9-11,19].
The degree of self-inflicted damage seen in this case reflects the lengths to which patients will go in order to relieve their discomfort and highlights a need for symptom management in patients with CF and nasal crusting. Conservative management with aerosolized nasal steroids, antihistamines, and saline irrigation has been regarded as the initial step in treating chronic sinonasal complaints in CF patients [20]. However, guidelines for dosing and interval of treatment have not been outlined, which may result in inappropriate and inefficacious therapies. The use of extended duration empiric antibiotic therapy, both topical and systemic, for these symptoms is particularly concerning, considering the high risk that CF patients have of colonization with multidrug resistant organisms [21].
Despite conservative therapy, up to 25% of CF patients will undergo endoscopic sinus surgery, and many require multiple returns to the operating room for recurrent symptoms [5,8,22]. Sinus surgery, although not curative, has been suggested to improve the quality of life in these patients by decreasing nasal obstruction and discharge while improving activity tolerance and sense of smell [20,23]. While cystic fibrosis is a serious disease, the last forty years has seen an increase in the life expectancy of this population [24-26]. With prolonged life, there has been an increase in prevalence and severity of chronic rhinosinusitis, and the prevalence of CRS in CF patients is up to four times higher than the general population [27,28]. This case may indicate that earlier discussions addressing the management of crusting and chronic nasal discomfort in CF patients are warranted to minimize possible self-inflicted nasal damage.
Additionally, while digital trauma is a rare cause of septal perforation, this case draws attention to the fact that it should be considered in the differential diagnosis in circumstances of septal damage with unclear etiology. Self-inflicted nasal damage has been reported as a manifestation of undiagnosed self-destructive behaviors. Our patient was never seen by psychiatry. Addressing underlying psychiatric conditions may be crucial in preventing this type of intranasal damage [9,29].
We present the case of a woman with a history of CF and CRS who was found to have obliterated portions of her nasal septum and middle turbinate and who caused significant damage to her paranasal sinuses and lamina papyracea by digital trauma. The severity of the self-inflicted damage in this case underscores the importance of sinus disease symptom management, as it demonstrates the lengths that patients will go to in trying to relieve the discomfort. This is especially important in the cystic fibrosis patient population, who experience refractory sinonasal symptoms from a young age. Further investigation in order to establish appropriate treatment guidelines for this particular patient population is warranted, keeping in mind cases such as this, which demonstrate the consequences of ineffective symptom management. In addition, in the broader population, it is important to keep rhinotillexomania on the differential when evaluating a patient with septal perforation of unknown etiology.
There is no conflict of interest.
None declared.