Supraglottic laryngectomy for laryngeal cancer aims to remove cancer of the larynx whilst preserving its functions of airway protection, breathing and voice production. A well-known long-term complication of this procedure is aspiration.
We present a case of a delayed epiglottis reconstruction with auricular free flap for surgical rehabilitation of dysphagia. Primarily the patient underwent supraglottic laryngectomy, bilateral neck dissection and radiotherapy. She had a permanent tracheostoma because of a complete paralysis of the right vocal cord and a residual minimal mobility of the left cord. Her main complaint was leakage of liquid from her tracheostomy whenever she was drinking something. The chondrocutaneous auricular free flap was harvested from the pinna and was based on the superficial temporal artery and accompanying vein. The vessels were anastomosed to the superior thyroid artery and vein via a submandibular neck incision.
The neo-epiglottis helped re-establishing a degree of protection of the glottis during deglutition of liquids reducing vocal cords irritation, thereby improving swallowing and voice quality. In conclusion this form of reconstruction should be taken in consideration when surgical rehabilitation of swallowing after supraglottic laryngectomy is indicated.
Supraglottic laryngectomy, Dysphagia, Epiglottis reconstruction, Microvascular free flap
Swallowing is the active propulsion of food and liquid starting from the oral cavity and ending in the stomach and requires a coordinated activity of nerves, muscles, the hyoid bone and the larynx [1]. The process can be divided in stages: oral, pharyngeal and oesophageal [1].
During the pharyngeal stage, the vocal cords adduct to seal the glottis and the arytenoid tilt forward to contact the epiglottis base.
When the hyo-laryngeal complex is pulled in anterior and superior direction against the base of the tongue, the epiglottis, acting like a shield, tilts backwards and covers completely the glottis [1]. The bolus descending from the oral cavity is deflected laterally on both sides in the paraglottic space to slide along the piriform fossae and through the upper oesophageal sphincter [2].
Supraglottic laryngectomy for laryngeal cancer aims to remove a malignancy originating within the larynx cranially to the vocal cords. The false cords, the epiglottis and the aryepiglottic folds can be removed; however the vocal cords are preserved. The second goal of this procedure is the preservation of the three functions of airway protection, breathing and phonation of the larynx. The surgical approach can be either through a neck incision or endoscopic, depending on the staging. A well-known complication is aspiration, due to removal of structures that are major players in protecting the tracheal inlet during deglutition, such as the false vocal cords and the epiglottis [3].
According to Logemann vocal cord adduction and laryngeal elevation were the 2 most common dysfunctions after supraglottic laryngectomy [4].
Aspiration affects as many as 39% of these patients according to Simonelli [5].
Dysphagia can have a huge impact on patients' life, causing undernutrition, dehydration, aspiration, chest infections [6] and affecting social interactions making it difficult to eat in public and reducing overall quality of life.
We present a case of epiglottis reconstruction for surgical rehabilitation of dysphagia after supraglottic laryngectomy and radiotherapy.
A 62-year-old woman presented complaining of leakage of liquid from her tracheostomy whenever she was drinking something. She had no dysphagia for solid food.
She had been already treated for a squamous cell carcinoma of the glottic and supraglottic area staged as pT2 pN2c M0 at another institution.
Five years previously she underwent horizontal supraglottic laryngectomy extended to the right arytenoid, together with bilateral functional neck dissection and tracheostomy followed by a cycle of adjuvant RT.
She was cured from her cancer, however suffered from dysphagia and dyspnoea and needed a short tracheostomy tube to keep her tracheostomy open because of a severe stenosis at the level of the vocal cords.
The patient underwent a full course of speech and language therapy to improve her swallowing and was able to swallow solid or semi-solid food and never needed a percutaneous gastrostomy tube.
Since the first operation, over the course of 5 years, she had 2 episodes of pneumonia ab ingestis. Her weight remained stable.
A videofluoroscopy, 3 years postoperatively, showed normal elevation of the complex hyoid-thyroid cartilage, followed by normal transit of the majority of the fluids along the oesophagus with concomitant silent aspiration. Most of the aspirated liquid was leaking through the tracheostomy (Figure 1), however a minimal inhalation of contrast medium was also evident in the right inferior lobe of the lung.
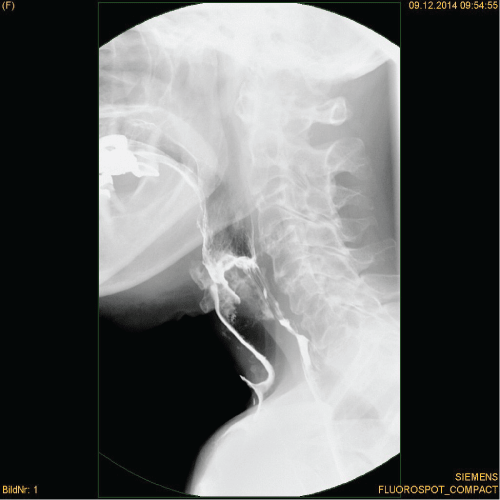 Figure 1: Videofluoroscopy: Aspiration and leakage of fluid through the tracheostomy.
View Figure 1
Figure 1: Videofluoroscopy: Aspiration and leakage of fluid through the tracheostomy.
View Figure 1
The patient had a whispered voice, however quality and volume were acceptable and she kept working as a teacher. She had to change shirts several times perday, as these would become completely wet and she was uncomfortable eating and drinking in the presence of others.
The preoperative evaluation included an assessment of the residual swallowing function by means of a videofluoroscopy and a Functional Endoscopic Evaluation of Swallowing (FEES). The latter confirmed the presence of aspiration and demonstrated a complete paralysis of the right vocal cord in a paramedian position and a residual minimal mobility of the left vocal cord with absent closure during coughing and phonation. The glottis opening was estimated to be approximately 3 mm in length and 1 mm in the transversal dimension during inspiration.
A Computed Tomography Angiography (CTA) and a CT with contrast medium ruled out tumours and lymph node metastasis and showed adequate vascularity for microvascular anastomosis.
Under general anaesthesia, after endotracheal intubation via the existing tracheostoma, a submandibular incision was performed along the old scaron the right hand side.
A platysma skin flap was raised and the upper border of the thyroid cartilage exposed. Following blunt dissection and under endoscopic control, the hypopharynx was opened at the level of the tongue base to allow for the passage of the flap pedicle.
Applying a nerve stimulator to the hypoglossal nerve, it was possible to pinpoint the best position for the transplant. The superior thyroid artery and vein were identified and trimmed on the right hand side of the neck (Figure 2).
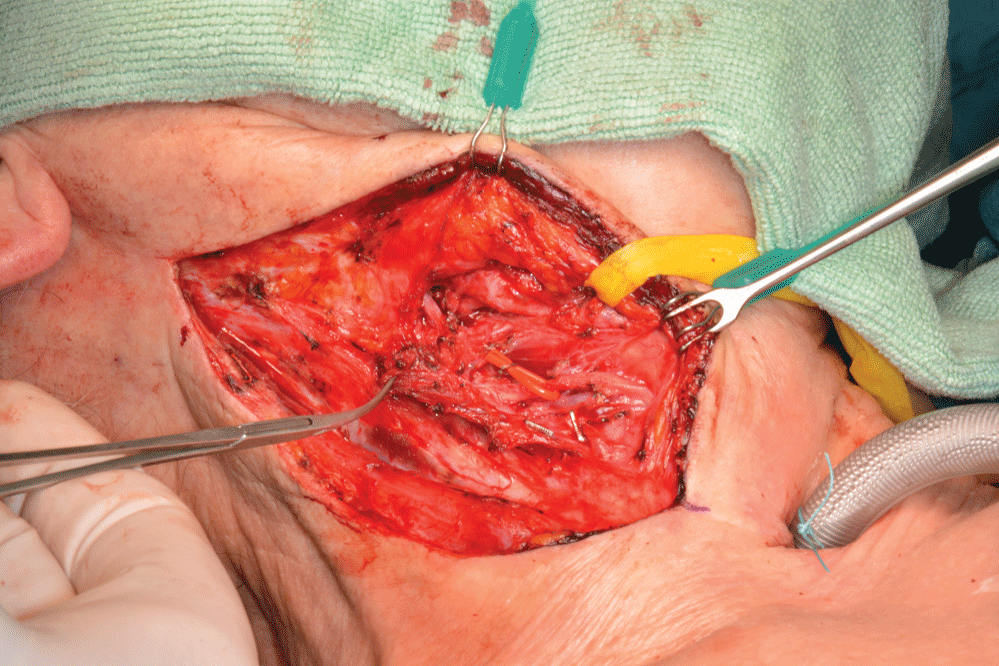 Figure 2: Submandibular incision with isolated neck vessels ready for the microvascular anastomosis. Right hand side.
View Figure 2
Figure 2: Submandibular incision with isolated neck vessels ready for the microvascular anastomosis. Right hand side.
View Figure 2
The flap harvest began after ultrasound identification of the superficial temporal artery on the right hand side. Access was gained using a preauricular incision with hockey stick extension in the temporal region. The Superficial Temporal Artery (STA) and venae comitantes were followed along their superior course. Two branches for the helix could be identified and the STA and accompanying veins were further dissected in cranial direction for a length of approximately 5 cm (Figure 3).
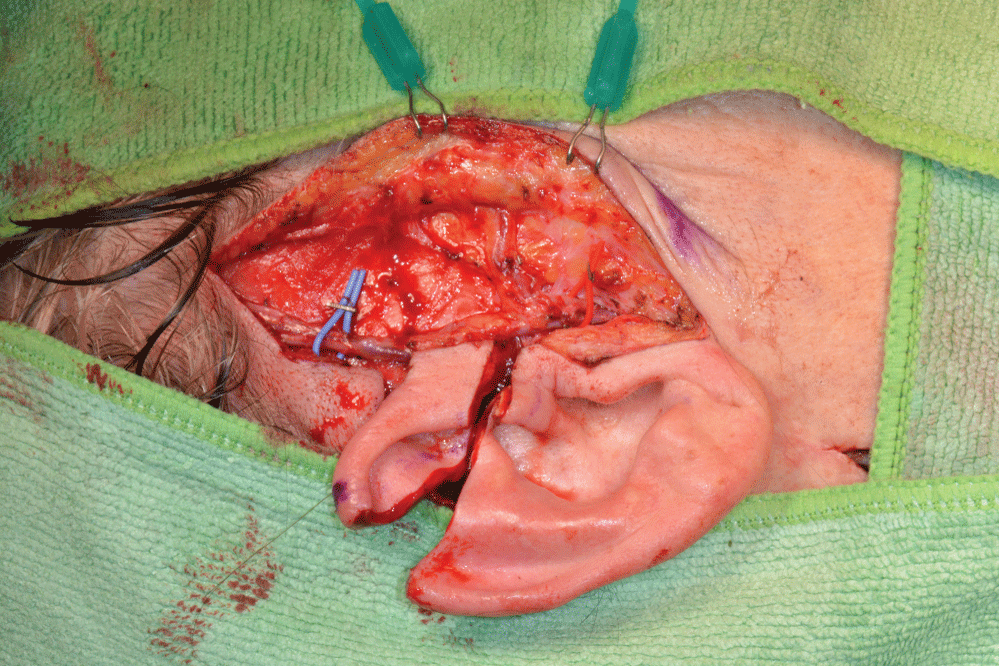 Figure 3: Preauricular incision, temporal vessels and flap design. Right hand side.
View Figure 3
Figure 3: Preauricular incision, temporal vessels and flap design. Right hand side.
View Figure 3
A triangular flap was raised from the superior aspect of the right pinna including the upper fourth of the helix and antihelix and part of the triangular fossa (Figure 4).
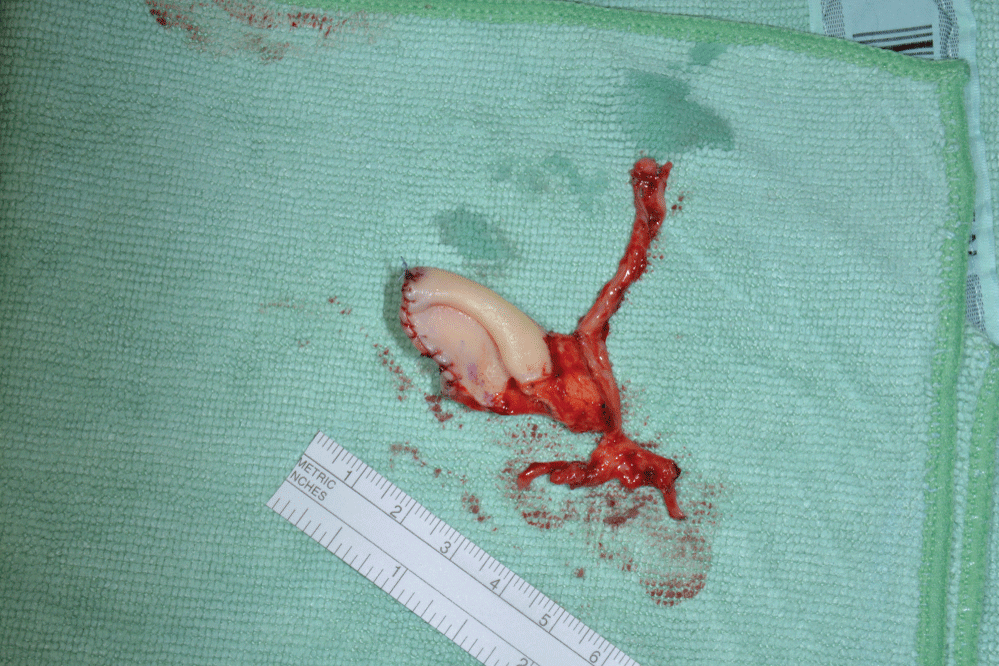 Figure 4: Chondrocutaneous auricular free flap with vascular pedicle.
View Figure 4
Figure 4: Chondrocutaneous auricular free flap with vascular pedicle.
View Figure 4
After clipping the vessels at both ends, the transplant was sutured to its recipient bed. The vascular pedicle was diverted through the hypopharyngeal window into the submandibular region on the right hand side and anastomosed with the superior thyroid artery and vein.
The flap was monitored with ultrasound and endoscopy (Figure 5) and the transplant was always vital, however, over the course of the first week, the patient developed a tracheitis with crusting. In view of these findings her tracheostomy tube was provided with a heat moisture exchanger (HME) filter.
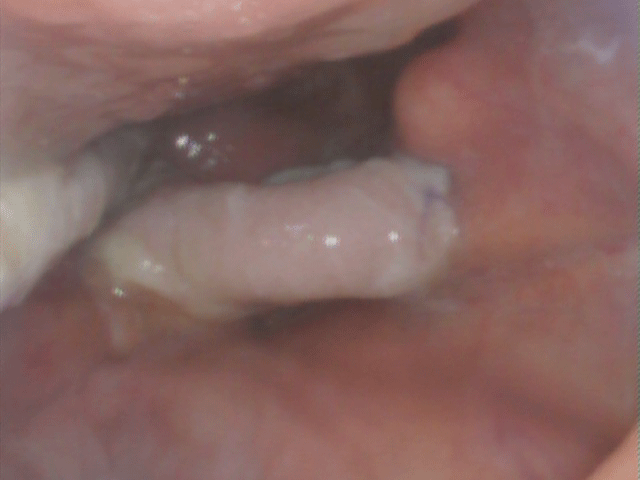 Figure 5: Endoscopic overview at day 3 postoperatively: Posterior pharyngeal wall at 12 o'clock, tongue base at 3 and 6 o'clock, nasogastric tube at 9 o'clock. The neo-epiglottis is the pale pink structure in the centre.
View Figure 5
Figure 5: Endoscopic overview at day 3 postoperatively: Posterior pharyngeal wall at 12 o'clock, tongue base at 3 and 6 o'clock, nasogastric tube at 9 o'clock. The neo-epiglottis is the pale pink structure in the centre.
View Figure 5
An inhalation therapy with Tyloxapol, a surfactant with mucolytic effect, was added to the existing regime based on humidified air inhalations, acetylcysteine and sultamicillin and the infection eventually healed. The NG tube was removed 14 days postoperatively and the patient could be discharged on day 27 in excellent general conditions.
Further endoscopic controls at 2, 3 and 6 months, showed a stable clinical picture with the neo-epiglottis slightly reduced in volume. 13 months postoperatively the transplant appeared as a mound covered by healthy mucosa (Figure 6).
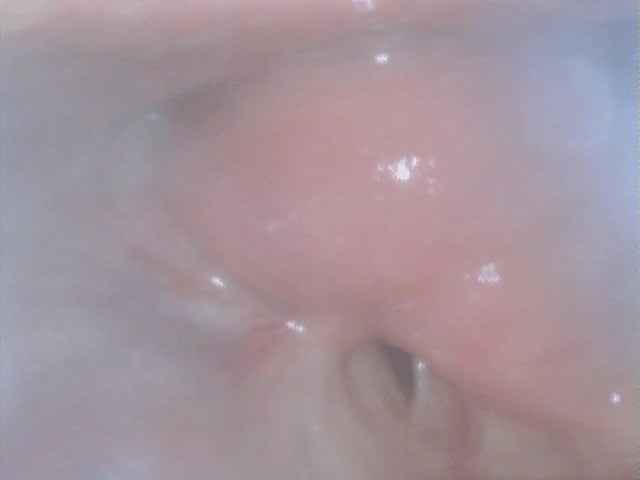 Figure 6: Endoscopic close-up view 13 months postoperatively: Tongue base at the very top from 9 to 1 o'clock. The neo-epiglottis appears as a red-pink mound in the centre and as a fold at 4 o'clock, partially covering the glottis (at 6 o'clock). A neo-vallecula is visible between the transplant and the tongue base.
View Figure 6
Figure 6: Endoscopic close-up view 13 months postoperatively: Tongue base at the very top from 9 to 1 o'clock. The neo-epiglottis appears as a red-pink mound in the centre and as a fold at 4 o'clock, partially covering the glottis (at 6 o'clock). A neo-vallecula is visible between the transplant and the tongue base.
View Figure 6
A video fluoroscopy showed retention of contrast medium of thick consistency above the neo-epiglottis and the patient is actually able to feel the presence of the bolus is in the neo-vallecula. Penetration and aspiration of contrast medium in liquid form were observed.
However, despite the latter findings, the patient can drink without any leakage from the tracheostomy in her daily life. She did not develop any episode of chest infection since the reconstruction (over 13 months post reconstruction). Furthermore the quality of her voice improved.
Aspiration of liquid and food is a well-known complication of supraglottic laryngectomy [7,8]. Swallowing rehabilitation with a speech and language therapist is necessary in the postoperative period [7].
From a surgical standpoint, local soft tissues pexies and flaps are possible if some remnants of epiglottis are still present after the resection [2]. Injection of fillers can be performed [9]. Epiglottis and tongue base have been reconstructed de novo with free radial forearm flap [3] and with chondrocutaneous auricular flap [10].
Recently an intralaryngeal prosthesis was successfully implanted into the larynx to stent a laryngeal stenosis and functionally replaced the epiglottis after supraglottic laryngectomy [6]. Our patient had already maximised her swallowing with speech and language therapy. A filler injection was not possible due to the fibrotic changes induced by multiple operations and radiotherapy.
A microvascular chondrocutaneous auricular free flap was selected as a reconstructive option in this case as it offers several advantages. The external ear has a cartilaginous framework lined by a thin epithelium like the epiglottis, therefore it is possible to replace like with like. The vessels at the donor site are readily available and easy to dissect, as they lie on a superficial plane.
The flap has its own vascular pedicle and can be transferred into a recipient bed even if it has been compromised by previous surgery and radiotherapy. The morbidity at the donor site is absolutely minimal and removing a small section of external ear doesn't cause any significant disfigurement (Figure 7). The defect can be camouflaged by wearing long hair, as it is often the case in women. Patients can still wear spectacles after the harvest.
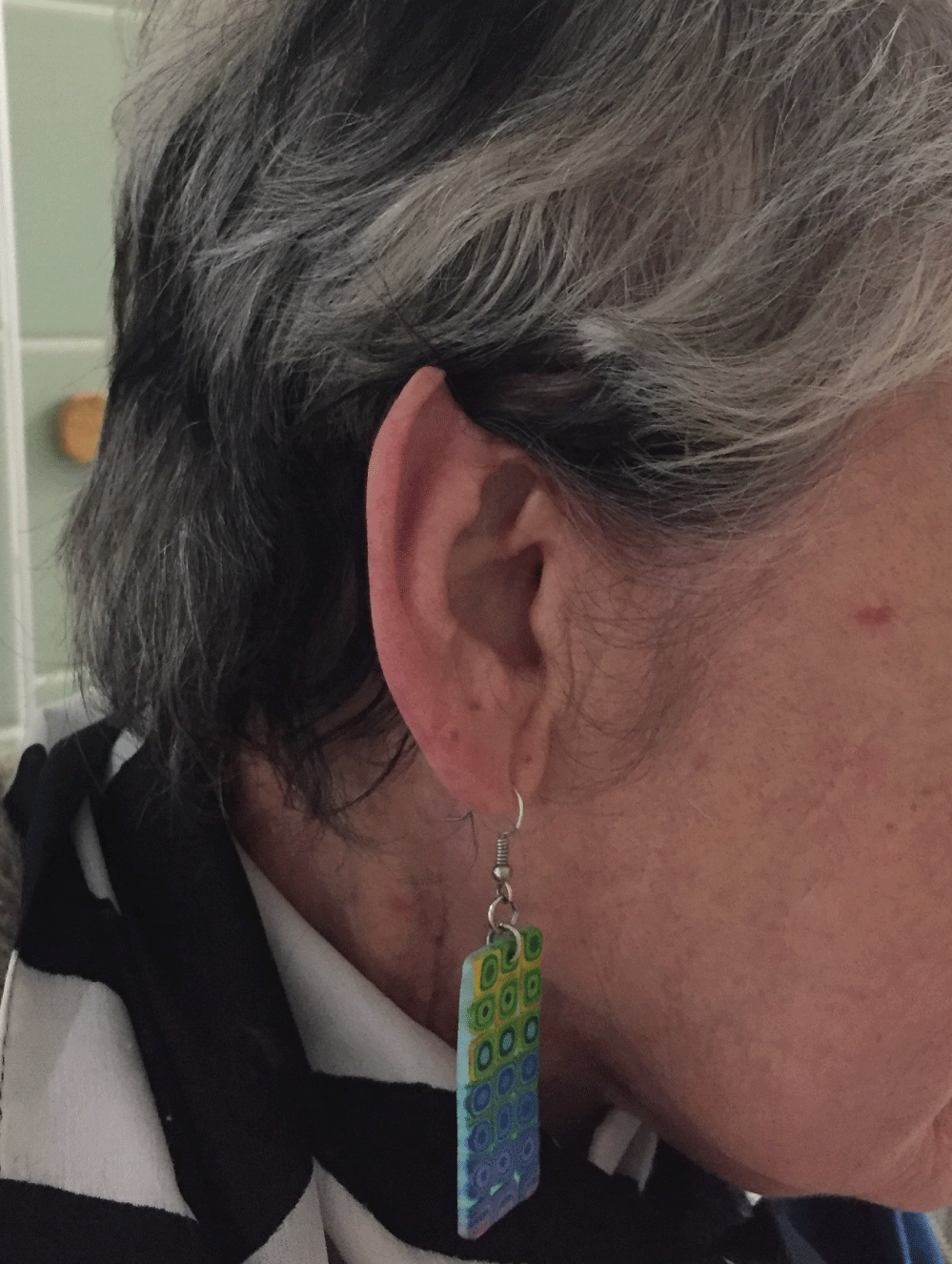 Figure 7: Donor site at 13 months postoperatively.
View Figure 7
Figure 7: Donor site at 13 months postoperatively.
View Figure 7
To our knowledge, this was the second time that an auricular free microvascular flap was used to reconstruct the epiglottis, after a case reported by Grajek, et al. [10]. Those Authors performed a supraglottic laryngectomy and a bilateral neck dissection followed by immediate reconstruction of the epiglottis. Our reconstruction was undertaken as a delayed procedure for treating an established case of dysphagia refractory to other more conservative measures. Supraglottic laryngectomy per se does not mandate a reconstruction in all cases and it should be undertaken only if swallowing rehabilitation and less invasive surgical options have failed or are not feasible. Our technique was minimally invasive, with a limited external neck incision. Thirteen months postoperatively we observed a degree of flap atrophy, similarly to the radial forearm transplants used by Hsiao, et al. [3].
Nevertheless, from a functional standpoint the functional gain was preserved. At videofluoroscopy the patient had to swallow contrast medium in alcoholic solution, which was extremely irritating for her mucosa, affected by permanent radiotherapy atrophy. Furthermore she had to swallow in a standing position with the head straight, whereas she normally drinks in a sitting position turning the head to the right to increase the glottic seal.
The improved quality of her voice is explained by the fact that the vocal cords are now better protected by the neo-epiglottis and therefore less exposed to repeated contact with liquids and are less oedematous.
In conclusion, a microvascular chondrocutaneous auricular free flap may be indicated in selected cases for the surgical rehabilitation of dysphagia after supraglottic laryngectomy when other options have failed.
No source of financial support or funding.
We have no conflicts of interest to declare.