Elder falls, Fall-prevention, Precision prevention, Precision lifestyle medicine
As the world population ages and older adults comprise a growing segment of the population, the public health community must formulate plans and work diligently to reduce health risks that compromise independence and quality of life for this age group. Falls are one such risk, as they often pose an immediate threat to safety and well-being. If an older person falls, there is a substantial chance of injury, and serious injuries, such as fractures or head trauma [1], are often life-threatening or life-changing.
In the United States, fall-related injuries are on the rise, resulting in over 800,000 hospitalizations annually [2]. Considering that the average cost of one episode of acute, fall-related injury care exceeds $30,000, [3] falls, and the injuries that they cause, pose an enormous, and ever-growing burden on our healthcare system and society.
Numerous randomized controlled trials have identified effective interventions for fall prevention [4]. Among these are interventions that older adults can implement themselves. And all can benefit from prevention. For example, strength and balance training lowers the risk of falling even among those who are not at high risk [4]. However, older adults are not aware of what works to prevent falls and do not take actions that will reduce their chances of falling [5]. For example, only about 3% of older adults in the United States report practicing balance exercise [6]. Low awareness of and minimal engagement in these proven strategies indicate a need to communicate more effectively to facilitate behavior change. We have previously described that clinical assessment and evidence-based management of modifiable fall risk factors is an effective means of reducing fall risk [7] (Figure 1). Here, we propose personalizing public health interventions and messaging to better promote self-driven fall prevention behaviors.
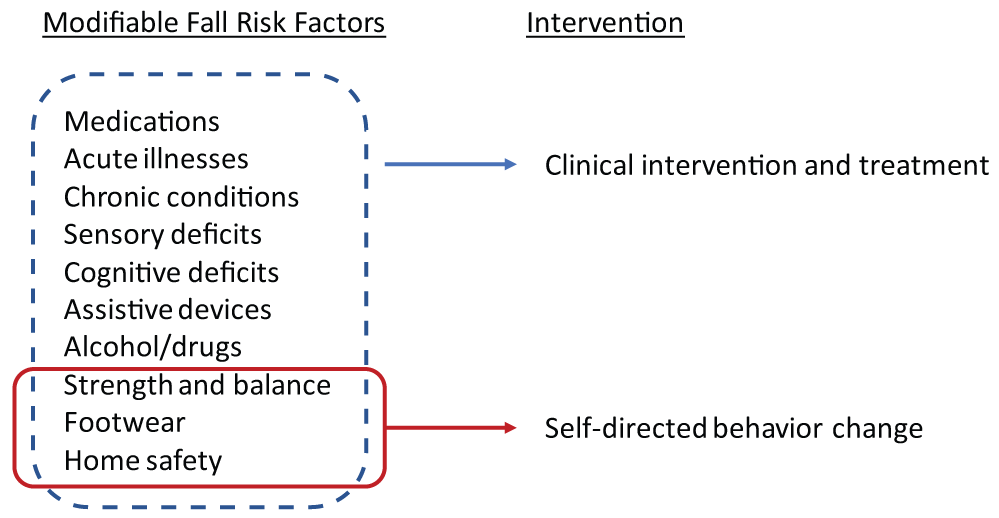 Figure 1: Of the known fall risk factors [6], some can be modified through self-directed behavior change, without clinical evaluation. We can promote these behavior changes through direct to consumer messaging, tailored to stage of change [17]. View Figure 1
Figure 1: Of the known fall risk factors [6], some can be modified through self-directed behavior change, without clinical evaluation. We can promote these behavior changes through direct to consumer messaging, tailored to stage of change [17]. View Figure 1
To date, public health communications regarding falls have largely been generic, "one-size-fits-all". See for example, "What YOU Can Do to Prevent Falls" published on the Centers for Disease Control and Prevention (CDC) website [8]. While very helpful as a point of departure, to be most effective, fall prevention must be personalized to the individual [9,10]. Indeed: Fall prevention is an ideal application of "precision lifestyle medicine [11]", in which a lifestyle intervention is tailored to features of an individual - for example, his/her biological and/or other personal characteristics. While the concept of precision (or personalized) medicine has been gaining increased attention (e.g., in the realm of cancer care), application of the concept of "precision" in the realm of health promotion and disease and injury prevention has been limited [11].
Herein then, focusing on prevention of falls and their associated consequences, we highlight three ways in which to personalize fall prevention: 1) Considering key personal characteristics, 2) According to readiness to make changes, and 3) Based on personal preferences and needs. We include a real-world case to illustrate (see sidebar).
As with other precision medicine and precision lifestyle interventions, personal characteristics should be factored in to help formulate recommendations for fall prevention. The severity of an individual's balance impairments should influence the type of exercise program that is recommended. For those who have mild impairments, a self-guided exercise program is appropriate; for those with higher risk, such as those who are frail [13], a supervised program would be advisable. For example, the Otago Exercise Program, which employs a supervised and individually-tailored design, has shown success especially among higher-risk groups such as those over age 80 and those who have fallen in the past year [14]. For those with memory difficulty that might impair recall of exercises or limit insight into safety risks, involving a family caregiver or concerned friend to cue the older adult and assist him/her in implementing the options he/she prefers is critical. For those overwhelmed by anxiety about falling during their daily routines, initial recommendations should directly address anxiety/fear - for example, through cognitive-behavioral interventions such as A Matter of Balance [15,16].
Some modifiable risk factors for falls, such as psychotropic medications, must be addressed by a healthcare provider [7]. However, others are under the direct control of the individual, including decisions about whether to wear supportive footwear, improve the safety of one's home, or add strength and balance exercises to one's fitness routine. Communication aimed at influencing these behaviors must consider the individual's current attitudes and beliefs. For example, we know that some older adults view fall prevention as not personally relevant [17]. To communicate more effectively, we can employ health behavior theory, such as the transtheoretical model of behavior change. This model describes five stages in behavioral change: Precontemplation, contemplation, preparation, action, and maintenance, each reflecting the level of the individual's readiness to change [18]. With regard to strength and balance exercise, for example, some older adults could be in preparation or action, looking for a group balance class in their neighborhood. Others will be firmly planted in the first stage, precontemplation, either having never seriously thought about starting strength and balance training, or remaining unconvinced that such exercise would help keep them from falling.
We can improve our fall prevention efforts by recognizing that not all older adults are ready to take action to reduce their fall risk. In a home hazard reduction trial, participants who made the home modifications suggested by an occupational therapist were more than twice as likely to believe that falls could be prevented by making the home safer, compared to those who neglected the recommendations [19]. Not surprisingly, belief in the efficacy of home hazard reduction was associated with adherence. The occupational therapist's action-based recommendations were well suited to individuals who were motivated to change and simply needed instructions about how to proceed. In contrast, individuals who did not believe in the efficacy of home safety modification did not follow through on recommended home modifications. Viewed through the lens of the transtheoretical model, these "precontemplators" remained unconvinced and required a different type of intervention, such as an educational program introducing the benefits of home hazard reduction.
Older adults seeking to prevent themselves from falling must ultimately make their own lifestyle choices. Fall prevention ideally should be a process of personal empowerment and self-driven change. In an analysis of semi-structured interviews with older women participating in a home-safety study, Clemson, et al. found that the notion of control was a key factor influencing home-safety decisions [20]. These women were more likely to have followed through on recommendations over which they felt ownership. These results suggest we should offer customizable plans which give the individual maximal control and ownership.
And choices abound [21]. For those ready to begin an exercise program for fall prevention, options range from group classes to self-guided routines that can be done at home [21]. Even among home options, individuals can either set aside dedicated time for strength- and balance-enhancing movements (e.g. the Otago Program [21]), or simply integrate these movements into daily life, such as intentionally squatting when putting laundry in drawers (e.g. Lifestyle approach to reducing Falls through Exercise, LiFE program) [21]. This range of options, representing different types and settings of activity, will accommodate individuals with different preferences and functional abilities. This abundance of evidence-based options can accommodate a wide range of preferences and allows for recommendations to be adapted as preferences and/or abilities change over time.
How can we achieve a more personalized approach to fall prevention and also achieve broad reach? Standardized materials can be written with the understanding that not everyone is ready to take action or that preferences for strength and balance training options will vary wildly from person to person. Still, it remains a near impossible task to create standardized materials that will resonate with every possible audience. For these reasons, we suggest a shift to tailored communication.
Technology-driven strategies to facilitate tailored communication hold promise. Computer algorithms allow us to make recommendations based on an individual's unique characteristics and preferences. Computer-driven tools have been developed that provide tailored advice to older adults with regard to nutrition, physical activity and weight loss [22]. To date, there have been few studies of the effectiveness of computer-based tailoring for fall prevention. As one notable exception, an online tool provided physical activity options that aligned an individual's self-rated comfort with physical balance and preference of exercise location [23]. People who utilized this tool found the advice to be relevant and expressed greater confidence in their ability to perform the suggested strength and balance activities as compared to people who received standardized, untailored materials. The ultimate effect of such tools, if broadened to provide advice about additional fall-prevention behaviors (e.g., footwear choices, home modifications), could be quite large. Computer tailoring offers a practical and economical way to proactively reach a large audience, while also recognizing individual preferences and needs.
Numerous controlled trials of fall-risk reduction interventions have given us the evidence to recommend a variety of preventive measures [4,24,25]. Now we must translate this body of evidence in a way that is relevant to and used by older adults in daily life, outside of trial circumstances. This needs to be accomplished not only in clinical interactions but also in the context of public health efforts to reduce elder falls. A personalized approach should increase adherence to proven fall-prevention strategies, foster lasting change, and ultimately reduce the burden of falls on both society and individuals.
A 66-year-old, community-dwelling woman with depression, obesity, and fibromyalgia-related chronic pain has fallen 3 times in the past year. She feels unsteady when walking and so for the past 3 months has been walking with a cane. Falls have become a significant source of anxiety for her, and she has stopped doing activities she enjoys, such as shopping at her local farmer's market and hiking on trails with her son. At home, she sometimes wears slip-on shoes and spends most of her free time watching television. She lives in a basement apartment which she admits is poorly lit. She would ultimately like to be free of the need for a cane and get back to doing things she enjoys. She wants to learn what she can do to prevent falls and is highly motivated to make any changes that would allow her to walk with better balance.
After completing her fall risk self-assessment on her mobile phone application that she downloaded for this purpose, the application integrated the information she inputted, assessed her key personal characteristics, stage of change for beginning a fall-prevention exercise routine, and her preferences for exercise location. She then received the following recommendations:
1. Sign up for A Matter of Balance workshop, offered in your neighborhood, to address your fear of falling.
2. Give away your slip-on shoes and wear your lace-up tennis shoes instead.
3. Talk with your apartment building manager about additional lighting in your unit.]
None.
Andrew Lawson received financial support by the Medical Student Training in Aging Research Program (NIH 2T35AG026736-11). Dr. Mensher has no conflicts of interest to report. Dr. Meischke has no conflicts of interest to report. Dr. Phelan received salary support from the Centers for Disease Control and Prevention to advise on development and dissemination of the Stopping Elderly Accidents, Deaths & Injuries (STEADI) tool kit.