Despite the increasing frequency of presentations for retained rectal foreign body, it remains a topic of intrigue, likely in part due to the taboo nature of the dilemma and also the ingenuity that is often required for successful extraction. Although the true incidence of retained rectal foreign body is unknown, there is data to suggest that the incidence is on the rise [1] and has been reported to be nearly one per month at a high volume center [2]. Previous studies have shown the problem to be much more prevalent in men [3]. Age at presentation has no boundaries but is more common in the 4th and 5th decades of life [4]. The most common foreign bodies are bottles and glasses, but offending objects may include almost anything; sex toys, light bulbs, aerosol canisters, wire, fish hooks, and many more [3,5]. Sexual gratification appears to be the most common reason for insertion although the details surrounding the event are often obscured by patient embarrassment [4]. Bedside extraction has a high success rate and is generally the preferred treatment when possible [2,6]. Some cases are not amenable to bedside extraction. We present a case of successful extraction of jagged broken glass from a patient's rectum without the need for ostomy or transabdominal surgery.
A 62-year-old man with no significant past medical history presented to the emergency department about one hour after insertion of a tall thin glass into his rectum. The patient attempted to remove the glass but the end of it broke off. With the onset of rectal pain and bleeding, he decided to go to the ER via EMS. The patient had normal vital signs on presentation. Digital rectal exam was not performed due to the presence of broken glass. External perianal exam was significant for blood at the anal verge. X-ray confirmed presence of the retained foreign body (Figure 1). The patient brought a matching glass, so that we could understand what the foreign body looked like (Figure 2). Due to the presence of rectal bleeding, we knew that there was high likelihood of rectal injury. The patient was brought to the operating room for anorectal exam under anesthesia with removal of the foreign body. He was placed in high lithotomy position in the candy cane stirrups. A Lone Star retractor was carefully placed to evert the anus. Fractured glass was visible in the anus pushing into the anal sphincter. The glass was thin and was pushing up against the wall of the anus/distal rectum circumferentially. A few pieces of glass broke off while attempting to place retractors around the foreign body. Ultimately the only retractor that we were able to successfully place between the glass and the rectum was a narrow malleable. Numerous malleable retractors were placed circumferentially around the foreign body to protect the anal canal from the sharp, jagged edge of the glass cup. We attempted to remove the glass with this technique; however the closed end of the glass was suctioned to the rectal wall proximally. We passed an Argyle suction catheter with a chimney valve past the glass into the rectal lumen and insufflated air above the glass which successfully released the suction. With this maneuver, we were able to shimmy the glass out using the circumferential malleable retractors. The glass measured 16 cm in length by 5 cm in width (Figure 3). There was 200 cc of blood in the rectum after the glass was removed. Transanal endoscopic microsurgery (TEMS) was performed to assess for rectal injury. A very patulous anus precluded the use of flexible sigmoidoscopy due to inadequate insufflation. TEMS revealed two 1 cm mucosal injuries in the distal third of the rectum which appeared superficial and required no intervention. There was a 2-3 centimeter left posterior quadrant anal sphincter injury involving the internal anal sphincter and a few fibers of the external anal sphincter. This was repaired with a running 2-0 Vicryl suture and the distal aspect was left open to allow for drainage. There was also an anal mucosal injury over a large hemorrhoid which was repaired with a Vicryl suture. Given that there was no frank full-thickness rectal injury, we elected not to perform a diverting stoma. Post-operatively, the patient did well. A CT scan of the pelvis was performed to evaluate for any glass fragments not previously identified during examination under anesthesia. This was negative for retained foreign body. The patient tolerated a diet and was discharged on post-operative day 0.
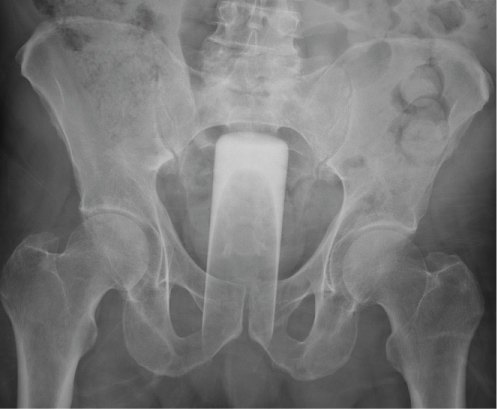 Figure 1: X-ray confirmed presence of the retained foreign body. View Figure 1
Figure 1: X-ray confirmed presence of the retained foreign body. View Figure 1
 Figure 2: Foreign body. View Figure 2
Figure 2: Foreign body. View Figure 2
 Figure 3: Glass Size. View Figure 3
Figure 3: Glass Size. View Figure 3
As long as patients have rectums, retained foreign bodies will continue to occur. Due to the lack of homogeneity in retained objects, each case may present a unique technical challenge. Several algorithms have been developed and all agree that peritonitis requires exploratory laparotomy [2,3,5,7]. If peritonitis or suspected perforation is not present, most authors recommend bedside trans-anal extraction when possible. However, one author at an institution with low incidence of rectal foreign body (2 patients per year), disputed this due to risk of advancing the object further into the colon and high failure rate of bedside transanal extraction in their series of ten patients [7]. Regardless of the setting (bedside or OR), transanal extraction is preferred over trans-abdominal for obvious reasons. A variety of methods have been employed when manual extraction fails. Tools that are used for other purposes (i.e. bone cutters, Kocher clamps, tenaculum, etc) may be useful to clutch and extract the foreign body [3,6]. There are also case reports of successful extraction using the aid of an obstetric vacuum device [8,9]. Other minimally invasive techniques have been employed with success, including endoscopic extraction and transanal minimally invasive surgery (TAMIS) [1,10,11]. Despite advances in technology, laparotomy and even colostomy is required in 8-13% and 2-6% of cases of retained foreign bodies, respectively [2,12]. Due to the risk of rectal injury, endoscopic evaluation is recommended after the foreign body is successfully removed [3].
Treatment of retained rectal foreign bodies can present unique situations for patients and surgeons. Safe and successful transanal extraction often requires a little bit of creativity. Use of the right retractors and elimination of negative pressure with proximal air insufflation allowed our patient to go home without an incision or a colostomy. Transanal endoscopic microsurgery is a safe and effective way to assess the rectal mucosa if flexible endoscopy is not possible.