Acute appendicitis is the most common surgical emergency worldwide, but the diagnosis continues to challenge clinicians. In the light of the constantly increasing demand for evidence-based treatment and avoiding unnecessary surgery, the traditional rates of negative appendectomies up to as high as 25% are no longer considered acceptable. Preoperative diagnostic imaging now plays a key role in the routine investigation of this patient-group, however there are controversies regarding the use of these examinations.
A retrospective analysis was carried out of all patients operated on at Levanger Hospital, Norway for suspected acute appendicitis during the period 2003 until 2014. We analyzed the preoperative work-up including radiological examinations and postoperative diagnosis for every patient.
A total of 1140 patients were operated on during this 12-year period. During 2003-2005, 39 of 282 patients (14%) underwent ultrasonography, CT scans or both. For the period 2012-2014 this number increased to 264 of 302 patients (87%). The proportion of Negative Appendectomies Rate (NAR) for the two periods were respectively 12% (33 of 282) vs. 6% (n = 19 of 302). In 2014, only 5 of 120 patients were operated on, based solely on clinical suspicion. A multivariable analysis of risk factors for NAR showed that when imaging concluded with direct signs of appendicitis, the Odds Ratio (OR) for NAR was 0.46 (CI 0.27 to 0.79) compared to no imaging. The corresponding OR for indirect signs of appendicitis on imaging was 3.53 (CI 1.38 to 9.04) and for inconclusive examination 3.87 (CI 2.11 to 9.10).
The use of preoperative diagnostic imaging prior to appendectomy increased from 14% to 87%. This was accompanied by a decrease in NAR by 50%. Direct signs of acute appendicitis on preoperative imaging seemed to be a good predictor for the diagnosis. Indirect signs or inconclusive imaging seemed to increase the risk for removing a normal appendix.
Acute appendicitis is the most common diagnosis requiring emergency surgery, and patients are frequently cared for by junior doctors. Historically, up to 25% negative appendectomies have been accepted [1]. However, this number is relatively high, exposing the patient to unnecessary postoperative complications, increased long-time risk, and contributing to increased hospital costs [2].
To help improve clinical diagnostic accuracy, various scoring systems have been proposed, such as Alvarado-score, de Dombal score, and RIPASA score [3,4]. Recent trials showed that an increased use of preoperative CT and Ultrasonography (US) greatly benefits the clinician in establishing a correct preoperative diagnosis, decreases the Negative Appendectomy Rate (NAR) by avoiding unnecessary surgery, and reduces the number of appendectomies [5-7].
These findings suggest a more liberal use of preoperative radiological examinations, and some guidelines recommend imaging studies routinely in the work-up of patients with suspected acute appendicitis [8] On the other hand, some studies conclude that neither CT nor US improve the diagnostic accuracy, but delay surgery [9,10] thus increasing length of hospital stay and cost [11]. The combination of clinical evaluation and radiological investigations may be the ideal work - up [12,13].
We observed a major increase in the use of preoperative radiological examinations over the last decade. In this study, we analyzed the association between changes in the use of preoperative imaging of patients with acute appendicitis, and its possible effect of reducing NAR.
The Strengthening and Reporting of Observational Studies in Epidemiology (STROBE) statement [13] was used in the analysis and to prepare the manuscript. The study was approved by the Regional committee for medical and health research ethics as an evaluation of clinical practice.
All patients operated at Levanger Hospital in North Trøndelag County, Norway, during 2003-2014 with NCMP-NCSP code JEA00 (open appendectomy), JEA01 (laparoscopic appendectomy) or JEA10 (appendectomy with drainage of abscess) or discharged with ICD - 10 codes K35.0 to K35.9 were identified from the electronic patient administrative system of the Levanger Hospital and included (n = 1179). This institution is the single primary hospital for a population of 90,000 inhabitants from 10 municipalities south in North Trøndelag County.
The patients are unselected and representative of this area. Patients undergoing appendectomy electively, or appendectomy done en passant, were excluded (n = 39). We did not include patients with other suspected causes of abdominal pain, nor patients undergoing US and CT, ending up with another diagnosis than appendicitis. The total number of patients included in this retrospective cohort was 1140 patients.
Data were collected from the records of the patients with regard to gender, age, date and time of onset of symptoms, admission, type of surgery and discharge. Data on diagnostic work-up included results of C-Reactive Protein (CRP), White Blood Count (WBC), temperature measurement, and preoperative US and CT. No patients had MRI. Further, peroperative evaluation of the appendix, surgical approach, histological evaluation of the appendix, and use of per-and postoperative antibiotic treatment were recorded.
In 818 patients (72%), the removed appendix was examined by a pathologist. All examined specimens were analyzed at the Department of Pathology, St. Olavs Hospital, Trondheim. Histology was the base of the final diagnosis, overruling the surgeons' peroperative evaluation. In the remaining number of patients (n = 322), the surgeons' peroperative evaluation of the appendix was taken as the diagnosis. During the first three-year period, the appendix was sent for examination by a pathologist, only if macroscopic pathology other than appendicitis was encountered. This routine changed during the study period, and currently all specimens are submitted, hence an increasing number of pathology reports exist for the last two periods: 2003 - 2005 n = 54 (19%), 2006 - 2008 n = 169 (65.5%), 2009 - 2011 n = 294 (98.7%) and 2012 - 2014 n = 301 (99.7%). During the two first periods, seven specimens were evaluated as false negative peroperatively, as the pathology report concluded appendicitis. For the two last periods 6 specimen were evaluated false negative peroperatively.
Non-perforated acute appendicitis was defined as presence of inflammation in the removed specimen, including phlegmonous appendicitis (i.e., transmural inflammation of the appendix wall without necrosis or perforation) and gangrenous appendicitis (i.e., inflamed appendix with necrosis of the appendiceal wall). The diagnosis of perforated appendicitis was based on either the presence of perforation described by the pathologist, or the clinical presence of a perforated appendix. The clinical diagnosis overruled the histological diagnosis, because it would dictate further treatment with antibiotics and prolonged hospital stay.
There was no routine applied for the description of the appendix specimen, hence a wide variability ranging from 'appendicitis' only, to more refined descriptions were found. For this reason, we categorized the histological findings as either normal or acute appendicitis. Based upon the surgeon's operation report we further classified the specific type of appendicitis as non-perforated (phlegmonous or gangrenous), or perforated appendicitis (with abscess formation or free peritonitis).
The radiologic department did not stick to defined diagnostic criteria for CT nor US throughout the study period. For this reason, we classified the conclusion this way: Not performed, direct signs of appendicitis, indirect signs of appendicitis, inconclusive examination (only used in US).
The cohort was divided into age subgroups. Age was treated as a categorical variable, for us to compare differences between age groups.
Continuous variables were found to be non-parametrically distributed, and central tendency was reported by median and range (minimum to maximum). The exact Cochran-Armitage test was used to test for trends in proportions. The associations between NAR as outcome variable and various explanatory variables were analyzed using a binary logistic regression model, and Odds Ratios (ORs) and 95% Confidence Intervals (CI) were reported. Likewise a logistic regression analysis was performed to study risk factors for finding a perforated appendix.
Two-sided p-values < 0.05 were considered significant. The analyses were performed using IBM SPSS Statistics 24 (SPSS Inc., Chicago, Illinois, USA) and StatXact 9 (Cytel Inc., Cambridge, Massachusetts, USA).
During the study period, 1140 patients (median age 26 years (1-91), 604 males (53%) were operated on for suspected acute appendicitis. Open operation was performed in 849 patients, laparoscopy in 278, and laparoscopy converted to open in 13. The overall proportion of NAR was 12%, with a significant difference between males (9.6%; 58 of 604) and females (14.6%; 78 of 536), p = 0.01. The proportion of perforated appendicitis was similar in both genders, 18.9% in males and 18.5% in females.
Figure 1 displays the various types of appendicitis for each year. NAR decreased successively since 2008. During the last three years, when the use of preoperative radiological examination reached 87%, NAR was 8.2% (n = 8) in 2012, 4.7% (n = 4) in 2013 and 5.8% (n = 7).
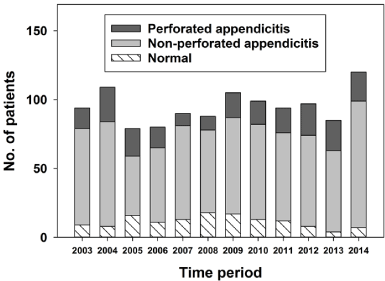 Figure 1: Type of acute appendicitis in relation to time period.
View Figure 1
Figure 1: Type of acute appendicitis in relation to time period.
View Figure 1
Figure 2 shows the number of different types of acute appendicitis in relation to age, while the percentage of type of acute appendicitis in relation to age is shown in Figure 3. The proportion of NAR was almost identical from one 10-year age-group to another. Perforations occurred most frequently in the youngest children and in the elderly patients. Appendectomy was performed most frequently in the age group 10-19 years, with 30.5% (n = 346) of all.
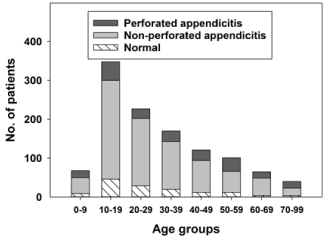 Figure 2: Type of acute appendicitis in relation to age.
View Figure 2
Figure 2: Type of acute appendicitis in relation to age.
View Figure 2
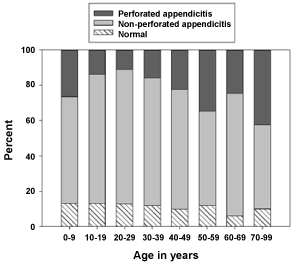 Figure 3: Percentage of type of acute appendicitis in relation to age.
View Figure 3
Figure 3: Percentage of type of acute appendicitis in relation to age.
View Figure 3
Table 1 shows how the use of preoperative radiological examinations (CT, US or both), NAR, and the perforation rate varied during the four 3-year periods. During the first period, 14% of the patients (n = 39) had either preoperative US, CT examination or both, during the last period this number increased to 87% (n = 264). The negative appendectomy rate decreased from 12% during the first 3 years to 6% during the last period. On the other hand, the perforation rate increased significantly from 13%, to 22% during the last three 3-year periods. This coincided with older patients in recent periods.
Table 1: Total number of appendectomies for suspected acute appendicitis in relation to time periods. View Table 1
Table 2 shows the results of preoperative US in relation to preoperative CT. Only 65 patients had both US and CT. When US was inconclusive, a CT was often performed, showing direct signs of appendicitis in a number of patients.
Table 2: Preoperative US examinations in relation to CT examinations performed 2003-2012. View Table 2
Table 3 shows the results of a multivariable logistic regression analysis of risk factors for removal of an uninflamed appendix in patients operated on for suspected acute appendicitis. Indirect signs of appendicitis or inconclusive examination were associated with a 4-fold increased frequency of removing a normal appendix.
Table 3: Multivariable analysis of risk factors for removal of an uninflamed appendix in patients who had appendectomy for suspected acute appendicitis. View Table 3
Figure 4 shows a Forest plot displaying results of the multivariable analysis of risk factors for removing a normal appendix. The corresponding ORs are shown in Table 3. Female gender, inconclusive preoperative imaging and indirect signs of appendicitis seemed to increase the risk of removing a normal appendix, whereas direct signs of appendicitis, increased WBC and CRP decreased the chance for negative appendectomy.
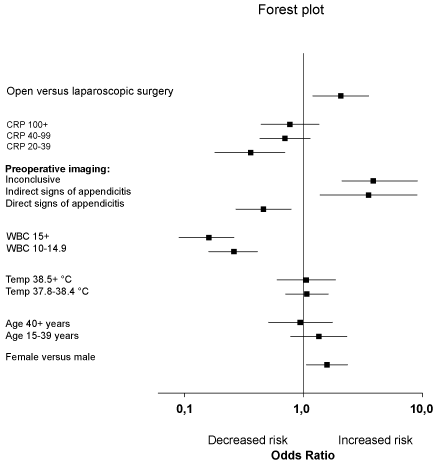 Figure 4: Forest plot of ORs after multivariable analysis of different risk factors for removal of a normal appendix, c.f Table 3.
View Figure 4
Figure 4: Forest plot of ORs after multivariable analysis of different risk factors for removal of a normal appendix, c.f Table 3.
View Figure 4
Table 4 shows findings of preoperative imaging in relation to WBC. In patients with a WBC < 10, a total of 27% (56/208) had a negative appendectomy. When preoperative imaging showed direct signs of appendicitis, this percentage was reduced to 14% (11/81). For WBC > 15 the corresponding percentages were 7% (31/437) vs. 5% (6/131).
Table 4: Preoperative imaging and white blood count in relation to NAR. View Table 4
The median time from admission to surgery was 5 (0.4-69) hours without preoperative radiological examinations, versus 12 (2.3-180) hours if US or CT had been done. A perforated appendicitis was not associated with the number of hours between admission and surgery (OR = 1.0, 95% CI 0.986 to 1.014).
The analysis revealed that the use of US, CT, or both modalities in the preoperative diagnosis of acute appendicitis during 2003 to 2014 had increased from 14% to 87%. Simultaneously, a decrease in NAR from 12% to 6% was observed. Female gender, a normal leukocyte count, indirect signs of appendicitis or inconclusive preoperative imaging was associated with NAR. Traditionally, a higher number of negative appendectomies have been accepted for women than for men. Seetahal, et al. reviewed 56,000 negative appendectomies, finding women accounting for over 70% of the negative appendectomies [14]. In the previously mentioned RIPASA score, female gender gives a lower risk score than male gender [2]. Our findings of association between female gender and NAR, coincides with previous reports.
Numerous reports have described the association between acute appendicitis and elevated WBC, with differing results [15-18]. In our material, an elevated WBC showed a decreased risk for removing a normal appendix. The results of WBC must be weighed against the clinical picture and findings from preoperative imaging.
The present study showed that imaging seemed to help the surgeon to a correct diagnosis when the radiologist reported direct sign of appendicitis. On the other hand, when imaging showed indirect signs of appendicitis, or was inconclusive, this seemed to be confusing, leading to a high percentage of NAR.
The increased use of preoperative imaging in our cohort seems comparable to the general development in western countries. In the United States, CT investigations were estimated to 3 million in the 1980s and 67 million in 2006 [19]. Radiological investigations are commonly used in the work-up of patients with acute abdominal pain, including suspected acute appendicitis. Some authors claim that routine imaging may reduce unnecessary surgery [5]. In the Netherlands Bakker, et al. [7] published guidelines for the work-up of suspected appendicitis to avoid unnecessary appendectomies, estimated to 2500 operations annually. They recommend radiological investigations prior to every appendectomy. This was found to be cost-effective by Boonstra, et al. [20], in an analysis of 466 patients before and after the implementation of these guidelines.
The use of preoperative US and CT has increased dramatically in our department, especially since 2009. The rate of negative appendectomies has fallen. This change has also been observed by others [4,5]. The incidence of appendectomies performed is relatively steady in our series, while some report a decrease in the number of appendectomies with increasing use of US and CT [4].
The increasing use of preoperative CT is controversial, and there is a fear of an increasing amount of radiation-induced malignancies due to ionizing radiation [19]. A recent report by Kim, et al. [21] concluded that low-dose abdominal CT was not inferior to standard-dose CT regarding NAR in young adults, with a lower median radiation dose - length product as compared to standard-dose CT (116 mGy*cm vs. 521 mGy*cm, respectively).
This aspect is more important the younger the patient's age, and with regard to patients in the reproductive age. If US is inconclusive, we may consider low-dose CT a possible radiological examination in the diagnosis of acute appendicitis [21,22]. With regard to pediatric patients, US is the first choice imaging technique. Wagenaar, et al. [23] showed a 30% reduction of preoperative CT investigations, after introducing a protocol where US was the primary investigation.
Faiz, et al. [24] found no deaths among 234,402 patients aged below 49-years, who underwent laparoscopic appendectomy in United Kingdom during 1996-2006, confirming this a procedure with extremely low mortality. With this in mind, and the additional advantages of shorter time to surgery and the possibility for intervention, diagnostic laparoscopy is an important alternative of the available armamentarium to assure optimal care of patients with suspected acute appendicitis.
The increased use of US and CT examinations was associated with some hours delay from admission to surgery. In the multivariable analysis, the time from admission to surgery was not associated with a higher risk of perforated appendicitis. Finding of an increased perforation rate during recent periods could be explained by an increased number of patients in the 40+ group, constituting 31.2% of the patients in the last three-year period, compared to 20.5% in the first three-year period. Guller, et al. [25] found higher perforation rates with increasing age in their material. The median time from admission to operation increased by nearly four hours in our material, coinciding with other reports [8, 9].
The current study includes all the patients operated on for acute appendicitis during a 12-year period at a single institution, serving an unselected population of 90,000 people. Records of all patients were available, and necessary data could be extracted with missing values for histology reports only. The hospital's catchment area has been unchanged throughout the study period, thus representing a stable population. We think that in this setting, an institutional review based on clearly defined and accessible data, was warranted to provide data that are otherwise difficult to obtain consistently over a long time-period with significant changes of the use of radiological examinations. No other changes in the work-up, such as interpretation of clinical signs or results from blood tests that may explain changes in treatment policy, were introduced during the study period.
The retrospective design implies several weaknesses. Histological reports were missing for a considerable number of patients, in particular for the first period (2003-2007). In those cases, we had to rely on the surgeons' evaluation. When we compared the surgeons' evaluations with those of the pathologists, only a small number of patients had been given a different diagnosis by the surgeons. We are aware of previous reports showing that as many as one third false negative diagnoses were made during diagnostic laparoscopy [26], and 9.2 - 35% normal appendices were removed, based on postoperative histological evaluation [27]. There has been no consensus regarding the pathologists' evaluation of the appendix and the grade of inflammation in the present study. Due to the retrospective design, we can only observe our findings as associations. They do not prove causality, wherefore they must be interpreted with caution.
The increased use of preoperative CT and US was associated with a decrease in the number of negative appendectomies. The observed increase of perforated appendicitis was attributed to more patients of older ages operated during the later periods. We think it is reasonable to use diagnostic imaging tools in the work-up for suspected appendicitis. However, the harmful effects of radiation must be kept in mind. When imaging showed direct signs of appendicitis, a negative appendectomy occurred very infrequently. On the other hand, when imaging showed indirect signs of appendicitis, or was inconclusive, negative appendectomy was often the case if the surgeon decided to operate.
The authors declare no conflict of interest.