A number of surgical procedures for treating chronic ankle instability have been described. Most of them are only to repair the anterior talofibular ligament (ATL) without considering the calcaneofibular ligament (CFT) injury and both chondral injuries of talus and tibia. We aimed to describe a modified procedure as alternative to already described surgical techniques that offer some advantages that we have observed.
In orthopedics, surgical procedures are categorized as anatomical and non-anatomical, and are performed through an open or arthroscopic approach, and literature reports a variable number of complications. In this case series report a minimally invasive modified anatomic technique is described. The procedure was done on 21 patients with diagnosis of chronic ankle instability, with a follow-up period up to two years after the surgery. Initially, an ankle arthroscopy was performed in all patients; in 70% synovectomy and chondral plasty was done before anatomic reconstruction of anterior talofibular ligament with cadaveric semi-tendinous tendon which was tunneled and fixed to the fibula with a titanium bottom, and distally, with one or two biodegradable screws into the talus and/or calcaneus due to an associated injury of CFT.
Patients had a mean age of 32 years (range, 23-60); 14 were male and seven female. Most of them used to practice some kind of sport activity. They had a preoperative and postoperative assessment according to the American Orthopedic Foot and Ankle Society (AOFAS; www.aofas.org) score and through their sport and daily activities reassuming time. A mean 25 points improvement in AOFAS scale was seen, and sport reassuming occurred in 90% of patients in a lesser time than with usual techniques. With our proposed technique, a rigid immobilization is not used allowing an immediate rehabilitation program and free walking by three weeks.
This modified technique is a treatment alternative for ankle chronic instability that has produced satisfactory outcomes through an anatomic, safety, and reproducible surgical reconstruction.
Ankle chronic instability, Repetitive sprain, Ligament plasty
Post-traumatic chronic lateral ankle instability is a frequent disorder and, according to literature, a precise prevalence is lacking [1]. It causes working inability, limitation in sport performance, and long-term arthrosis sequelae. Some authors, however, say that this entity occurs in 10-20% of all ankle sprains and predominates in young athletes [1-3].
Delay in diagnosis and treatment of this injury is usually caused because traditionally ankle sprains are treated superficially by sport trainers or primary care physicians, so patients see a specialist several months later for pain persistence, sport performance reduction, repetitive sprains, long-lasting inflammation, and instability feeling [4-7]. Health care professionals and patients usually consider these ankle injuries as minor problems, so conservative or even empiric measures for their management are chosen, with the subsequent delay in diagnosis and effective treatment [4-7].
Once the orthopedic surgeon diagnoses the condition, the dilemma arises concerning the surgical technique, the choices being the functional repair of the anterior talofibular ligament (ATL) and/or calcaneofibular ligament (CFT) when is also injured. There is a number of surgical techniques for ligament plasty, and range between those that repair first the ATL leaving untouched the CFT confirming that there is not a consensus on a specific procedure that may be considered as the gold standard for this type of injuries [7,8].
Surgical techniques may be categorized as anatomical and non-anatomical. Non-anatomical procedures, such as the one described by Evans and Watson-Jones in the 50s, and more recently the technique described by Chrisman Snook, suggest the use of the peroneal brevis tendon to replace the damaged ligament without modifying its distal insertion into the fifth metatarsal bone provoking so an additional compression and an unbalanced sub-astragalin joint. As a consequence, there is a great detraction about these procedures because they consist of an open and complex surgery requiring a long immobilization and rehabilitation period, with short- and long-term complications frequently occurring, mainly subtalar arthrosis and muscle unbalance leaving therefore a great number of athletes that are not capable to reassume their sport activities or not reaching their previous level of performance [8-13].
Examples of anatomical procedures are those such as the ones described by Bröstom, and Bröstom-Goul in the 80s. The first technique consists of direct repair of the torn ligament, and the second technique involves reinforcing the extensor retinaculum. Both techniques have their respective drawbacks including that they use an open approach, the CFT is not repaired, and in many patients insufficient ligament remains or damaged ligament are found preventing the desired plasty and consequently mandating prolonged rehabilitation periods, up to six months, with a high risk of recurrence of the injury [8,14-16].
On the other hand, most of authors agree that current arthroscopic repair procedures are complex surgeries performed through blind reconstructions, are very labile and they do not integrally solve the problem [7,8,17,18].
For all the reasons abovementioned we present a 100% anatomic and minimally invasive modified technique that we have been performing since 2013 consisting of an ankle arthroscopy followed by a 3 cm incision over the body of the ligament in order to safely perform the plasty of one or both injured ligaments.
This procedure does not require rigid immobilization for a long period of time in the postoperative period. A Walker type boot is used to allow immediate rehabilitation and assisted ambulation for two weeks, and by the third week, the boot is removed. This way, the number of complications is reduced (i.e., delay in recovery due to long-lasting immobilization, reduction in sport performance, pain and inflammation persistence based on AOFAS score), and working and sport reintegration time is faster than that required with the abovementioned surgical techniques.
We present our experience along with the results and the technique description as a further alternative for the great amount of existing surgical procedures to ankle ligament repair for this frequent pathology.
This is a case series report of 21 patients submitted to this modified technique between January 2013 and April 2016, with a follow-up of at least two years. Patient's mean age was 32-years-old (range 23-60 years-old). Fourteen (14) were male and seven women. Two were high-performance athletes; 15 used to practice some sports recreational activity, and the remaining four patients did not practice any sports.
The diagnosis of chronic ankle instability was done with the history of a severe ankle sprain and the treatment they received, considering if that therapy was insufficient or not. Treatment types varied from bandages and immobilization with splints, to orthosis and circular devices, and in most cases, they did not solved the problem timely; all these modalities were applied in emergency rooms. Two-view simple X-rays were taken in all cases mainly to rule out fractures. Due to symptom persistence, all patients finally saw an orthopedic surgeon specialist. In our group, the time since the first traumatic event ranged from six months to four years. The number of repetitive sprains while practicing minor sports activities or during daily life activities ranged from three to 12 ankle sprains before surgery.
In order to support the clinical diagnosis, the classification of the American Orthopedic Foot and Ankle Society (AOFAS) scale was applied, both preoperatively and postoperatively, along with ankle magnetic resonance images (MRIs; Figure 1) [19]. The same surgical team operated all 21 patients using the same technique. In every case the informed consent was obtained, and all the Mexican Health Laws were followed. The same specialist group performed the follow-up assessments following the AOFAS score until final discharge and sports reassuming, if it was the case.
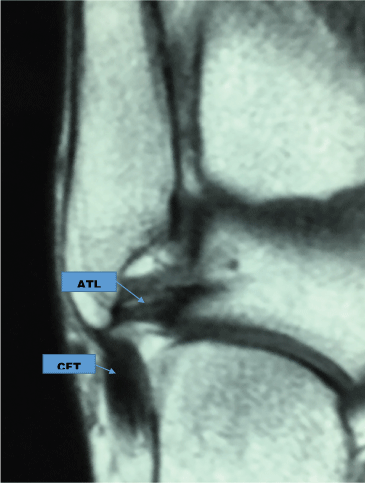 Figure 1: MRI showing both the calcaneofibular ligament (CFT) and the anterior talofibular ligament (ATL).
View Figure 1
Figure 1: MRI showing both the calcaneofibular ligament (CFT) and the anterior talofibular ligament (ATL).
View Figure 1
The modified technique we are presenting is based on the hypothesis that any tendon, whether cadaveric or belonging to the patient himself/herself has enough endurance to replace an injured ATL by absorbing the joint charges, something that has been shown for over 60 years after having performed replacement procedures of this tendon with a peroneal brevis tendon without documental evidence of tendon rupture [8,9]. Additionally, the semi-tendinous tendon has been routinely used for a cruciate ligament plasty in the knee, which is a more weight-demanded joint than the ankle joint; for this reason, we are certain that this modification of the original technique provides a high degree of safety and reliability.
The technique used consisted in an ankle arthroscopy through the usual ports, anteromedial and anterolateral, in all the patients to intentionally look for the presence of chronic synovitis and/or a chondral injury according to Outerbridge scale [20], whether in the talus or in the tibia, more specifically over the lateral corner of the joint. The premise was that an ankle chronic instability would necessarily produce this type of injuries, as it will be seen in the results we obtained [8,16,21-23]. In our group of patients and depending on the injury grade [20], a razor chondroplasty was performed, and in five patients microfractures were added.
Following the arthroscopy, the ischemia is placed, and a 3 cm curve skin incision is done, at the site where presumably the body of the ATL is located (Figure 2). Through this incision, the ATL and CFT status may be assessed for the surgical planning of the ligament repair, in one or two directions, by using a cadaveric allograft.
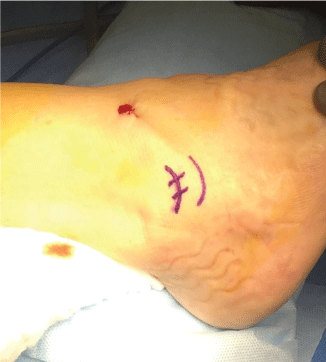 Figure 2: A 3 cm skin incision.
View Figure 2
Figure 2: A 3 cm skin incision.
View Figure 2
Allograft preparation: Simultaneously, a semi-tendinous free cadaveric allograft is prepared, with a maximal length of 12 cm and a minimal diameter of 0.5 cm, folded on itself and placed on the top buttonhole. A sturdy suture attached to a titanium bottom for fibular fixation and the remaining two free ends may be used together when there is only an ATL injury, or individually to repair both ligaments (Figure 3).
 Figure 3: Graft preparation.
View Figure 3
Figure 3: Graft preparation.
View Figure 3
The proximal fixation of the allograft is performed through a fibular tunnel done at the ATL insertion level by using a guide introduced under fluoroscopic guidance, distally to proximally, with a forward-backwards angle of 60 degrees and a minimal length of 3 cm. At this time it is necessary to separate the peroneal tendons so they are not injured with the guide point when emerging through the bone posterior cortical, preferably with a Homans separator or a narrow periosteum scrapper, located through a 0.5 cm incision. Once the guide point is located, a 4 mm cannulated drill is used to make a tunnel of at least 2 cm in length where the fibular part of the free tendon will be resting. The tunnel depth within the tendon is marked and introduced by pulling the free ends until the titanium bottom anchors in the posterior cortical of the fibula (Figure 4).
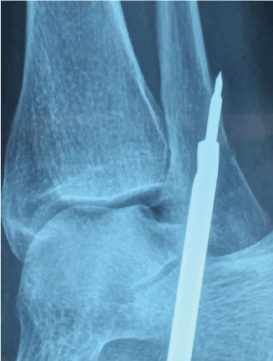 Figure 4: Proximal tunnel.
View Figure 4
Figure 4: Proximal tunnel.
View Figure 4
When only the ATL is injured, the distal fixation is performed with the ankle in neutral position over the anatomical insertion of the ligament by joining the two ends to fixate them within the tunnel made with a minimal depth of 2 cm over the talus (Figure 5). If an added lesion of the CFT is found, both graft ends are separated, and the other part of the tendon is fixed in the anatomic position of the ligament, over the calcaneus, also through a 2 cm length tunnel.
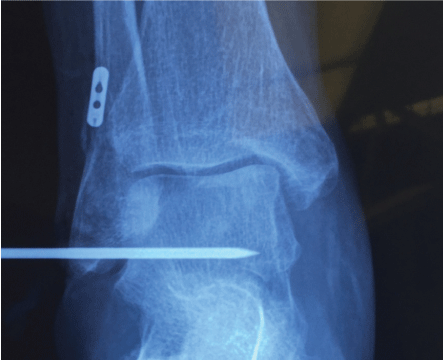 Figure 5: Distal tunnel over the astragalus.
View Figure 5
Figure 5: Distal tunnel over the astragalus.
View Figure 5
A tenodesis is performed with a biodegradable screw (Figure 6). If both ligaments are damaged, each end of the graft will be individually used to repair the ATL but also the CFT by using two screws. The ankle stability is checked verifying the new ligament tension, range of motion, and non-existence of an anterior drawer and the final closure is as usual. In every case we use platelet rich plasma taken from the own patient to bath the tendinous graft and, with the remaining of the plasma, to infiltrate the ankle joint.
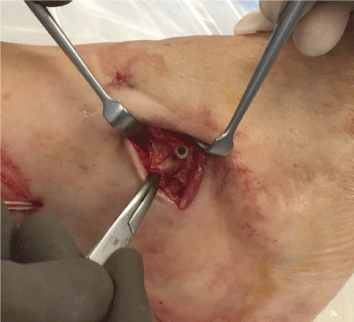 Figure 6: Distal fixation with a biodegradable screw.
View Figure 6
Figure 6: Distal fixation with a biodegradable screw.
View Figure 6
We use cryotherapy for two weeks, immobilizing the joint with a Walker boot and with the use of crutches for partial discharge during 15 days after the surgery, removing the boot at times to initiate the rehabilitation program starting since the first postoperative day. The orthosis device is definitively removed after three weeks of the surgery, and free walking is allowed by then.
Periodical assessments by counting the progress in the score on the AOFAS scale are performed, and depending each case reassuming sport activities progressively at six weeks after surgery are allowed.
A two-year periodic follow-up of patients was performed until completion of the time and the final discharge by seeing them at the office. The predominant injury was on the right ankle in 12 patients and on the left ankle in nine. The number of sprains ranged from 3 to 12 with a mean of 7, and the time of those sprains ranged from 6 months up to 4 years before the surgery decision was undertaken.
Before the surgery, 95% had pain mainly associated with sport activities and 80% noted permanent inflammation of the affected ankle. Recovery from new repetitive sprains took longer every time they occurred with the consequent withdrawal of sport activities and more work leaves due to the injuries.
On physical examination, inflammation was corroborated and an exquisite pain was elicited by pressing at the injured ATL level. The anterior drawer phenomenon was clinically seen in nine patients, and it was more notorious in those with an injury of both ligaments, ATL and CFT.
Dynamic X-rays in varus and valgus were not a reliable study to perform the surgery since it depends a lot on the lab where they were taken, the technique used, and on the person performing the maneuver so we used RMI instead as it is a more trustful image study. The ligament injury was clearly seen only in one patient. On the other hand, RMIs were inaccurate in 20% of the cases for a ligament injury, and in 61% for the chondral lesion. This way, we insist that clinical criteria are the most important to make the surgical decision, always recommending an ankle arthroscopy [8,23].
Preoperatively, mean AOFAS score was 64.6 points out of 100, and postoperatively all patients had a mean of 25 points (90.8) improvement with a notorious decrease in pain severity at the end of the assessment period as mentioned in AOFAS score. All patients (100%) reassumed their jobs by two months in average, and their sport activities by four months (Figure 7).
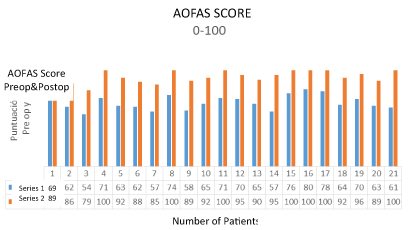 Figure 7: American Orthopedic Foot and Ankle Society (AOFAS) score obtained both preoperatively and postoperatively.
View Figure 7
Figure 7: American Orthopedic Foot and Ankle Society (AOFAS) score obtained both preoperatively and postoperatively.
View Figure 7
High-performance athletes (one marathon-runner and one triathlete) were able to reassume their sports activities although the triathlete had a 20-30% decrease in his sport performance but he performed his daily activities normally. Two other patients stop playing soccer in spite of they did not have any discomfort while playing. The remaining (15) patients reassumed all their activities completely.
During the arthroscopy a grade I-III chondral lesion (Outerbridge classification) was observed in 70% of the patients, with mild to severe synovitis in 100% of the patients. A partial synovectomy with razor chondral repair was performed, and in five patients this procedure was supplemented with microfractures [20].
Finally, we concluded that the results were excellent in 18 patients (86%), in two (9.5%) the results were good due to mild to moderate pain persistence at the site of the surgical incision, and in one patient (4%) the result was considered as regular since she was not able to reach 100% of her previous sport performance. All these was assessed according to AOFAS scale (www.aofas.org). Probably because it was a minimally invasive procedure, there were not infections nor wound dehiscence.
The only major complication that we observed was in a female marathon runner who was not able to reassume totally (100%) her sport activity by showing a 20-30% decrease in her performance even though she had not functional limitations or pain in other less demanding sports activities.
In the follow-up period, we did not find any radiology or clinical evidence of subtalar arthrosis. We think that this is a good modified technique with the advantage that it is an anatomically minimally invasive technique that has been used by many other authors that have used autologous or allogenic tendinous grafts [9,10].
A minimally invasive modified surgical technique using an autograft (it may be an allograft) to repair CFT and ATL injuries following an ankle arthroscopic procedure is presented. It is based on performing an ankle arthroscopy in all the cases since we observed the presence of chronic synovitis in all of our patients and 70% of chondral lesions, all of which were repaired during the procedure avoiding so future damage such as chronic pain and sports functional inability. All this has been pointed out previously in the world literature [1-7].
On the other hand, the technique uses a 3 cm minimally invasive incision, which is width enough to visualize both ligaments and to correctly apply the graft. Through the years, this graft has shown to be effective enough to replace a broken or damaged ligament, which is frequently hard to repair by direct methods [8-10].
Our results have been satisfactory and no drawbacks have been seen. It consists of an anatomical repair with no residual subtalar arthrosis and less time to resume full working and sports recovery compared to other techniques. All of this is because the immobilization time is less when using an anatomical technique through minimal invasion which translates in a less number of complications because enables a solid repair that allows an early rehabilitation and reintegration to a normal life style.
We should continue watching our patients in order to see their long-term evolution. Also, the surgery cost versus the recovery saving time, especially in high-performance athletes, is a main consideration. Even the procedure is costly and we are aware that cadaveric graft is not always available in many surgical centers worldwide, the technique might be taken as the gold standard in the future due to the obtained benefits, motivating us to recommend it as an alternate procedure instead many other techniques already described in the world literature to treat these, every time more frequent injuries.
JCR was involved in the conception, design, surgery, information collecting, analysis of the results, and writing of the manuscript. JCVM participated in the surgery of the patients, analysis of the results and review of the submitted manuscript.
There was no external funding for this study. The authors declare not having any conflict of interest.