Left ventricular mass regression after aortic valve replacement is largely incomplete and often most of patients do not achieve left ventricular mass normalization.
To evaluate the hypertrophy regression in patients with "appropriate" hypertrophy compared with those who developed an excess or "appropriate" hypertrophy in the setting of pure aortic stenosis.
A population of 40 patients operated for aortic stenosis was divided in two groups according to the pre-operative level of hypertrophy. Eighteen patients entered in the group of "appropriate" hypertrophy and 22 patients in the group of "appropriate" hypertrophy. Hemodynamic and echocardiographic parameters were collected pre-operatively, at discharge, 3, 6 and 12 months postoperatively.
Patients with "appropriate" hypertrophy experienced a greater and faster mass regression with -30 ± 11% compared with -15 ± 14% (p < 0.001) of the appropriate hypertrophy. Pre-operative left ventricular mass was the most powerful independent predictor of hypertrophy regression in both groups (p < 0.001), while secondary independent variables were linked to fluid dynamics of the prostheses (p = 0.02) in the group of "appropriate" hypertrophy and diabetes (p = 0.045) for "appropriate" hypertrophy.
Left ventricular mass regression and normalization is a complex phenomenon and is influenced by several factors. Patients with "appropriate" hypertrophy experienced the largest hypertrophy regression with a full recovery of ventricular function and size. In this group the ventricular mass has the propensity to regress regardless the residual valve gradient. On the contrary the fluid dynamics of the bioprostheses affected the hypertrophy regression in patients with "appropriate" hypertrophy.
LVM regression, AVR
Left ventricular (LV) hypertrophy is a form of adaptation to a chronic cardiac overload. In the setting of aortic stenosis (AS), LV hypertrophy develops to limit the increase of LV systolic wall stress. Aortic valve replacement (AVR), is expected to eliminate the LV burden, inducing regression of LV hypertrophy [1,2] and possibly LV mass normalization with an improvement of life expectancy and elimination of symptoms. Left ventricular mass normalization is the most difficult goal to achieve because of irreversible alterations often present in the myocardium [3-5] at time of operation, as well as the presence of associated patients and prosthesis factors [6-8].
In chronic LV pressure overload several growth factors are triggered [9] followed by an expansion of both myocytes and interstitial compartments [10] with the extent of LV mass that is virtually unrelated to the degree of AS [11]. Furthermore, other clinically recognizable patient-specific factors such hypertension, obesity and peripheral vascular disease, may influence the extent of pre-operative LV hypertrophy and its regression postoperatively [1-3,5-7].
Indeed, there are patients who develop a degree of hypertrophy, called "inappropriate hypertrophy", that excesses the level of LV afterload, calling into question the role of LV workload as the unique cause of hypertrophy [12,13].
The objective of this study was to evaluate LV mass regression, after AVR, in patients with "appropriate" LV hypertrophy compared with those who developed an excess or "appropriate" hypertrophy in the setting of pure aortic stenosis.
The study population comprised 40 patients enrolled in a prospective randomized trial who had been divided into 2 groups according to whether they were to receive a Trifecta (St-Jude Medical Inc. Minneapolis MN) or a Freestyle (Medtronic Inc. Minneapolis, MN) bioprosthesis [14]. The protocol comprised an echocardiographic study pre-operatively and at discharge, 3, 6, 12 months post-operatively. Other patients' population characteristics are reported elsewhere [14]. The patients were included if they met the following criteria: Pure or prevalent aortic stenosis, age > 70 years, native aortic annulus diameter ≤ 2.3 cm (measured on pre-operative echocardiograms), EF ≥ 50%, first-time operation, sinus or atrial rhythm and no concomitant cardiac procedure anticipated other than coronary artery bypass graft. The local Institutional Ethics Committee approved the study protocols.
Pre- and post-operative LV hypertrophy was defined by indexing the LV mass (LVM) using the patient's height in meters with the allometric power of 2.7 [15]. The cut-off values for hypertrophy were > 50 g/m2.7 in males and > 47 g/m2.7 in females. This method has proven to be more sensitive in diagnosing LV hypertrophy, than using the Body Surface Area (BSA), since it is not affected by the patient's weight. LV mass was calculated using the corrected ASE formula [16]: LVM = 0.8 [1.04(IVSd+LVEDD+PWd)3LVEDD3]-0.6, where IVSd is the end-diastolic interventricular septum thickness, LVEDD is the LV end-diastolic internal diameter and PWd is the LV end-diastolic posterior wall thickness. For each patient, the LV mass was predicted by the following formula: Predicted-LVM = (0.64*SW) + (-18.1*Sex) + (6.63*height2.7) + 55.13 where SW is stroke work (systolic BP × SV × 0.0144, expressed in g-meters), height is in meters and sex is coded as 1 = men; 2 = women [12,13]. Any patients with an LVM ≥ 28% [12,13] the predicted-LVM value were classified as having an "appropriate" hypertrophy. With this cut-off, the group of "appropriate" hypertrophy had 22 patients while the group of "appropriate" hypertrophy had 18 patients. Patients were considered to have hypertension when they were being treated for hypertension at the time of operation [15]. We also calculated the valvuloarterial impedance (Zva) as: (SAP + MG)/SVi, where SAP is the systolic arterial pressure, MG is the mean transvalvular pressure gradient and SVi is the stroke volume index. While the Systemic Arterial Compliance (SAC) was calculated as: SVi/PP, where SVi is stroke volume index and PP is brachial pulse pressure.
Pre- and postoperative echocardiographic studies were performed by 3 experienced echocardiographers, with an echocardiography machine iE33 (Philips Medical Systems, Eindhoven, Netherland) equipped with 2.5-3.5 MHz transducers. The peak and mean valve gradients were calculated using the modified Bernoulli equation with correction for subvalvular velocities. The Effective Orifice Area (EOA) of the prosthesis was calculated by using the continuity equation and indexed by BSA.
The data were statistically analysed using SyStat 13.0 software (USA). The continuous variables were expressed as mean ± SD. We verified the normal distribution by the Shapiro-Wilk's test and, when p < 0.1, the variable was log-transformed. Discrete variables were compared by the χ2-test with Fisher's Exact test when appropriate. For each group we performed a simple linear regression with LVM index (LVMi) regression as dependent variable. Those variables that yielded a moderate correlation with the Pearson's correlation coefficient > 0.3 were tested in a multiple linear regression analysis. Because of the limited numbers of subjects available for the analysis (a group with 18 patients and a group with 22 patients) we performed the multiple regression analysis with no more than 2 independent variables. As the independent variable with the strongest correlation with the LVMi regression was the pre-op LVMi, any other variable was tested to be independent from the pre-op LVMi only. P values < 0.05 were considered significant.
In the group of patients with "appropriate" hypertrophy there were only female, the BSA and BMI were lower compared with the "appropriate" hypertrophy group. Besides, there was a higher incidence of diabetes and a higher level of pBNP in the group with "appropriate" hypertrophy compared with the group with "appropriate" hypertrophy (Table 1). The 2 groups did not display any afterload differences, showing similar mean gradient, EOAi, SAC and Zva (Table 2). The group with "appropriate" hypertrophy showed some degree of LV dysfunction having lower EF, Cardiac Index, stroke volume index, higher e/e' as well as a dilated LV as resulted in the greater LVEDVi and LVESVi, compared with the "appropriate" hypertrophy group (Table 2). As expected, LV mass was higher in the group with "appropriate" hypertrophy 74 ± 16 g compared with the group with "appropriate" hypertrophy 52 ± 8 g (p < 0.001). Finally, the incidence of hypertrophy was 100% for the group with "appropriate" hypertrophy, while it was 69% (p = 0.008) for the group with "appropriate" hypertrophy.
Table 1: Patient's profile. View Table 1
Table 2: Echocardiographic Findings. View Table 2
The distribution of the two types of prostheses, in the two groups, was similar with the stentless valves present in 59% and 39% (p = 0.340) for "appropriate" and "appropriate" groups respectively.
One patient died at 3 months for gastric cancer. The post-operative fluid dynamics of the valves were similar between the two groups. The mean gradient was 7 ± 3 mmHg and 6 ± 3 mmHg (p = 0.253), while the EOAi was 1.1 ± 0.3 cm2/m2 and 1.1 ± 0.2 cm2/m2 (p = 0.948) for "appropriate" and "appropriate" hypertrophy respectively.
At 1-year, the pre-operative LV mass regressed significantly to 49 ± 9 g (-30 ± 11%) in the group with "appropriate" hypertrophy and to 44 ± 7 g (-15 ± 14%) for the group with "appropriate" hypertrophy. Residual hypertrophy was present in 61% and 33% (p = 0.08) of patients with "appropriate" and "appropriate" hypertrophy respectively. In both groups most of the LV mass regressed in the first 3 months, however, a faster rate of regression was observed in the group with "appropriate" hypertrophy (Figure 1). LV function improved substantially in the group with "appropriate" hypertrophy, with no longer statistical significance in the difference of the LV cavity size for both diastolic and systolic volumes. Indeed, the post-operative LVEDVi were 40 ± 6 ml/m2 and 41 ± 8 ml/m2 (p = 0.614) while LVESVi were 15 ± 3 ml/m2 and 14 ± 3 ml/m2 (p = 0.823) in the group with "appropriate" and "appropriate" hypertrophy respectively.
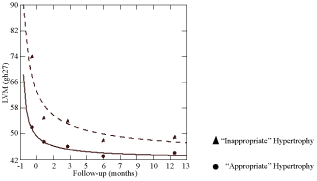 Figure 1: LVMi regression through the 1 post-operative year. View Figure 1
Figure 1: LVMi regression through the 1 post-operative year. View Figure 1
In Table 3 are reported the simple and multiple linear regression analysis conducted separately in the two groups. The results revealed that the pre-operative LVMi was the strongest independent variable with an R -0.82 (p < 0.0001) and -0.65 (p = 0.001) for "appropriate" and "appropriate" hypertrophy respectively. Two separate set of secondary independent variables were found at the simple linear regression analysis. For the group with "appropriate" hypertrophy only two variables, linked to the fluid dynamics of the bioprostheses, emerged as significant at the simple and multiple regression analysis. While for the "appropriate" hypertrophy a set of factors related to specific clinical condition arose. Nevertheless, at the multiple linear regression only diabetes emerged as independent to pre-operative LVMi.
Table 3: Echocardiographic Findings. View Table 3
Our study showed that 45% of the patients, at time of AVR, had developed an "appropriate" hypertrophy and these experienced twice as much LVMi regression, with -30% ± 14 compared with -15% ± 11 (p = 0.009) of the group with the "appropriate" hypertrophy. Interestingly, most of the LV mass regressed in the first 3 months post-operatively in both groups, but at a faster rate for the group with "appropriate" hypertrophy (Figure 1). Nevertheless, at 1-year, the patients with "appropriate" hypertrophy still exhibited a higher LVMi with 49 ± 8 g compared with 44 ± 7 g (p = 0.037) of the "appropriate" hypertrophy group.
Hemodynamic load is the stimulus that triggers a chain of biological events that leads to LV hypertrophy by widening the myocyte compartment with an increase in size and number of myocytes [9,10,17], as well as by increasing the interstitial compartment with fibrosis deposition [18-22]. Usually the myocytes/interstitial compartment ratio is 1 to 3 [3-5,10,21,22] but, when LV dysfunction develops, the interstitial compartment grows disproportionately [4,5,10,18,19].
Because up to 20% of patients with AS [23], in our study 15%, do not develop a pre-operative LV hypertrophy, the adaptive role of the LV hypertrophy has been questioned advancing the concept that hypertrophy is a maladaptive phenomenon [18]. The degree of AS is not the main responsible for the grade of LV hypertrophy [11,23] but is a part of a complex network of interaction among patient-specific factors [24-27]. That explains the variability in the extent of pre-operative LV mass from patient to patient who apparently have the same degree of AS. Indeed, our data confirmed this variability, with substantial differences in pre-operative LVMi between the 2 groups despite a similar aortic valve burden (Table 2).
Duration of the disease, prior to surgical correction, plays a significant role in generating irreversible structural alterations [28], as much as chronic pressure overload leads to a reduction in capillary density [29], myocytes loss [4,30] and fibrosis deposition [4,9,30]. As the disease progresses, with the transition from compensated to a decompensated state, the LV function decreases, and the chamber dilates causing further collagen deposition [30-32]. In our study, the group with "appropriate" hypertrophy showed some degree of LV dysfunction with reduced EF, cardiac index, larger LV diastolic and systolic volumes, higher pBNP and LV filling pressure, in the form of e/e' (Table 1 and Table 2). Thus, the condition of "appropriate" hypertrophy is present when a more advanced stage of disease has been reached with structural changes beyond the compensatory requirements. This is a significant issue, because pre-operative LV mass and indices of underlying irreversible myocardial alterations are correlated to a worse outcome [3,33].
Among the recognizable patient-specific factors inducing LV hypertrophy, gender is one of the most notable as well as hypertension, diabetes and BMI. In our study, gender and diabetes were unevenly distributed between the groups, while for the BMI there was a trend in being higher in the group with "appropriate" hypertrophy (Table 1). The gender issue was in line with other studies in which was demonstrated that male gender easily develops a higher LVM, fibrosis deposition and LV dysfunction than females [34-36].
Although AVR is usually followed by a substantial LV mass regression [1,2,7], most patients do not normalize their LV mass [2,3,8]. Our current study confirmed that numerous patients did not achieve LV mass normalization. Indeed, the percentage of residual hypertrophy, was 61% and 33% (p = 0.08) for the "appropriate" and "appropriate" hypertrophy group respectively (Table 2). We confirmed that the extent of the pre-operative LV mass was the main factor predicting post-operative LV mass regression in both groups, while secondary factors differed according to the groups. Left ventricular mass regression is a process involving both interstitial and myocytes compartments [19,22] and the value of LV mass [3,19], at 1-year post-operatively, is correlated to the extent of pre-operative myocardial fibrosis, myocytes diameter and nuclear volumes [3,4]. The latter, are all signs of a rather irreversible condition present inside the myocardium at time of operation. Persistence of LV hypertrophy after AVR has multiple causes and may be due to a combination of patient-specific factors (such hypertension, Zva, diabetes, gender, obesity and other biological factors), fluid dynamics of the prosthesis and irreversible alterations in the myocardium. Hypertension is one of the most frequent factor that may be responsible for the persistence of LV hypertrophy [6] along with the high stiffness of the vascular system, resulting in a high arterial impedance or Zva [37]. These two conditions hamper LV mass regression both pre-operatively, with the deposition of irreversible fibrosis [11,20,23], and post-operatively if the hypertension is not adequately treated or a high LV impedance persists [6,36]. Apparently, this was not the case in our study, because both hypertension incidence and the level of the Zva and arterial compliance were similar in the two groups. Gender is known to influence LV remodeling in AS, since a higher mass, fibrosis deposition and possibly structurally irreversible alteration are more likely findings in males than in females [37]. In addition, angiotensin-renin system may modulate the degree of LV hypertrophy differently in male and in female patients [25]. The univariate analysis in the group with "appropriate" LV hypertrophy provided a distinct set of variables correlated with LVMi regression, which were compared with the group of patients with "appropriate" hypertrophy. However, only the pre-operative LVMi and diabetes predicted the extent of LV mass regression.
The role of patient-prosthesis mismatch in patients' outcome has been debated for years. An incomplete relief of the LVOT obstruction may sustain residual hypertrophy [2] as it has already been shown. For this very reason, in the past, the unsatisfactory performance of stented valves had prompted to adopt stentless bioprostheses to attain low valve gradients, although, in this regard, mixed results have been reported. More recently, a new generation of stented valves has become available with improved fluid dynamics [14].
In the group with "appropriate" hypertrophy the effect of the fluid dynamics of the bioprostheses on LV mass regression was apparent. The mean gradient and the EOAi were independent from the pre-operative LVMi with the mean gradient that accounted for 12% of the total variance. On the contrary, the fluid dynamic characteristics of the bioprostheses appeared not to play any role in the group with "appropriate" hypertrophy, in which only the diabetes emerged as an independent factor. In this group of patients, a key role on the hypertrophy development was probably played by other hypertrophic stimuli more than simply the level of LVOT obstruction. Thus, once the valve obstruction was removed, the high propensity to regress of the hypertrophy due to the excess of the LV mass, might have concealed any effect of the bioprostheses fluid dynamics.
For this study we did not analyze the effect of the type of prosthesis (stentless vs. stented) on LV mass regression for two main reasons. Firstly, our previous studies showed that, in term of fluid dynamic, both at rest and under stress, and the leaflets kinematics the two valves were equal [12,38,39]. Secondly, the distribution of the stentless valves was 59% and 39% (p = 0.340) for "appropriate" and "appropriate" groups respectively.
LVM regression and normalization are a complex phenomenon and are influenced by several factors. Patients with an excess of hypertrophy experienced the largest hypertrophy regression with a full recovery in LV function and size. In this group the LV mass had the propensity to regress regardless the residual valve gradient. On the contrary, the fluid dynamics of the bioprostheses affected the hypertrophy regression in patients with "appropriate" LV hypertrophy.
This study was conducted on a group of selected patients because one of the entry criterion for randomization was an EF of at least 50%. Thus, the assumption made might be valid only for those patients with normal or with mild LV disfunction. No data regarding post-operative arterial pressure value and hypertensive therapy, in patients with hypertensive history, were available. Although LV hypertrophy regression largely occurs within the first two postoperative years, we can't exclude that part of the LV mass could continue to decrease for several years at a slower rate.
None.
-Giordano Tasca: Design, data analysis and interpretation, drafting article, statistics.
-Francesco Trinca: Data collection, statistics and critical revision of the paper.
-Beatrice Riva: Data collection, data analysis and approval.
-Douglas Skouse: Data collection, data analysis and approval.
-Elisabetta Lobiati: Data collection, data analysis and approval.
-Caterina Chiara De Carlini: Data collection, data analysis and approval.
-Amando Gamba: Design and approval.