QT interval correction for heart rate (QTc) is essential for clinical usage. A new QTc formula has been developed based on a data agnostic mathematical approach in a large population ECG data base. The formula requires testing on a within individual basis under conditions of intervention to increase heart rate. The objective of this study was to examine the stability and reliability the new QTc formulae within individuals when Heart Rate (HR) is increased by dobutamine.
HR and QT interval were measured in fifteen individuals who received intravenous dobutamine in a sequential protocol at 5, 10, 20, 30 and 40 micrograms/kg/min.
Dobutamine produced a significant (p < 0.0001) increase in heart rate and a significant (p < 0.0001) reduction in QT. The new QTc formula showed relative stability with little change across the dobutamine dosages. Using a linear regression to evaluate the HR-QT interval, showed a significant (p < 0.0001) negative slope for the relationship. In contrast, the slope of the QTc-heart rate relationship for the new QTc formula did not differ from zero.
The new QT correction formula is relatively independent of the effect of increasing heart rate and should be useful QTc formula especially in conditions of increased heart rate.
QT interval, QT heart rate correction formula, Dobutamine
Assessment of the QT interval on the ECG has attracted considerable attention as a marker for potential drug-induced cardiac toxicity or drug-induced sudden cardiac death [1-3], electrolyte abnormalities [4], as well as the identification of individuals with genetic mutations that carry a high risk of sudden death [5]. A new QT-heart rate correction formula (QTc) has been developed based on ECGs from about 13,600 individuals in the NHANES US population study [6]. This QTc was shown to be was superior to other formulae [6,7]. The value of this approach, however, has not been tested in the same individual under different conditions of heart rate stress.
A critical aspect of the evaluation of the QT interval is its adjustment for heart rate because of the recognized inverse relationship between QT interval and heart rate. Studies that established QTc formulae including the most recent one, utilized data on different individuals who have different heart rates. While there is considerable power in the large numbers of individuals from population based studies, they do not address between individual variability.
Specifically these studies are not able to take into consideration variables that produce different resting heart rates that might in turn influence the QT interval. The importance of the individual responses to test the robustness of the QT-heart rate correction formulae is well recognized [8]. The new QT-heart rate adjustment formula has not been subject to protocol driven changes in heart rate to determine whether QTc is stable when heart rate is increased. The objective of this study was to examine the new QT correction formula for its ability to remain stable in the same individual across a range of heart rates.
The patient population were individuals who received dobutamine for a MIBI study and whose baseline ECG showed sinus rhythm, no interventricular conduction delay (or bundle branch block) or significant ST-T changes. The study was approved by the Institution's Research Ethics Committee.
Twelve-lead ECGs, recorded at a paper speed of 25 mm/s, were acquired in the supine position. Heart rate and QT measurements were made at specific time points during each stage of the dobutamine protocol. The first ECG was in the drug free, baseline condition, within 1 min before the beginning of dobutamine administration. The second ECG was at 2 min and 50 seconds after the first dose of dobutamine was started. Every subsequent ECG was taken 3 min after the increase in dobutamine concentration. The last ECG reported was 50 seconds after the fifth dose, or 15 min and 50 sec after initial infusion. The dobutamine protocol consisted of intravenous infusion of dobutamine. Dobutamine was started at 5 micrograms/kg/min and increased at 3 min intervals to 10, 20, 30 and 40 micrograms/kg/min. In a few individual, the dose of dobutamine was stopped after 30 micrograms/kg/min when a marked tachycardia occurred.
The heart rate and QT interval were measured manually from the ECG. For each RR interval, a caliper was used to measure the distance from one peak of the QRS complex to the next peak. Each recorded RR value was the mean of two consecutive RR intervals. The distances measured were in 0.25 mm increments. The average of two measurements was used in all analysis. For each QT interval, a caliper was used to measure the distance from the start of the QRS complex to the end of the T wave. The end of the T wave was defined as the intersection of a horizontal line representing the baseline of the ECG to the tangent of the downward curve of the T wave at its steepest point. The ECG baseline is typically defined at the level of the PR interval. If the PR interval was very short and could not be easily used or absent, the beginning of the QRS complex was used. Each pair of corresponding RR and QT interval was taken from the same complex. The distances measured were in 0.25 cm increments, with an uncertainty of ± 0.25 cm. As two readings were taken from each lead, the average of two was used in all analysis, The QT interval was almost always measured from lead II. Rarely, excessive baseline artifact (noise) in lead II, required QT measurement from leads I or III.
The basis for the formulation of the new QTc has been presented in detail [6]. Briefly, a spline correction function, modeled using a cubic regression spline with four knots and an adjustment for gender was fit to the QT and heart rate ECG data from 13,600 individuals in the US National Health and Nutrition Examination Survey (NHANES) II and III studies, conducted by the Center for Disease Control (CDC) of the US [6]. Considering the person's age, the spline QT correction, was developed. With each observation weighted by the respective NHANES sampling weight with spline parameters selected as those that minimized the least squares estimate fit of the QT-heart rate relationship [6]. The ECG exclusion criteria were abnormalities that made calculation of the QT interval difficult such as right or left bundle branch block, myocardial infarction left ventricular hypertrophy or rhythm not being sinus [6].
Several approaches were used. In the first approach, all data from the ECG prior to and at the end of each dose of dobutamine were used. After completion of dobutamine infusion, QTc was compared. In the second approach, the slope of the relationship, between QTc and the different dobutamine dose was assessed. A linear least squares regression model was used to calculate the slope of QTc vs. heart rate relationship (GraphPad Prism). The data are presented as mean ± 1SD. Statistical testing used repeated measures ANOVA to test variables across the different dobutamine doses. The relationship between QT and heart rate used regression analysis. Comparisons of the mean data for two different groups used the nonparametric Wilcoxon signed rank test.
Dobutamine was associated with a significant (p < 0.0001) increase in heart rate that increased from 74.3 + 11.6 bpm (mean ± SD) at baseline to 76.7 + 13.3, 88.0 + 16.3, 104.0 + 20.7, 113.2 + 21.0 and 120.6 + 13.8 bpm at respectively 5, 10, 20, 30 and 40 micrograms/kg/min of intravenous dobutamine (Figure 1). The magnitude of the change in heart rate was apparent (inset) and was significant (p < 0.001) as it increased by 48.6 + 12.0 bpm from baseline to the highest dobutamine dose. There was a significant (p < 0.0001) reduction in QT interval with increasing dobutamine doses (Figure 2). The magnitude of the change in QT interval was apparent (inset) as the QT interval decreased significantly (p = 0.008) by 85.3 + 36.2 msec from baseline to the highest dobutamine dose.
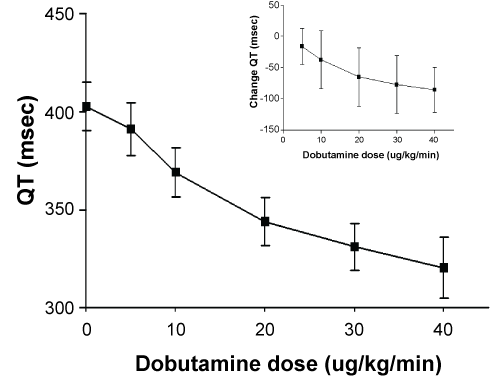 Figure 1: Shows the mean heart rate (± SD) at the end of each dobutamine dose administration. The inset shows the change in heart rate from baseline to each of dobutamine doses. The sample size was the same at each dose (n + 15) except for the highest dose (N = 10). The same sample size was present in the following two figures.
View Figure 1
Figure 1: Shows the mean heart rate (± SD) at the end of each dobutamine dose administration. The inset shows the change in heart rate from baseline to each of dobutamine doses. The sample size was the same at each dose (n + 15) except for the highest dose (N = 10). The same sample size was present in the following two figures.
View Figure 1
 Figure 2: Shows the mean QT interval (+ SD) at the end of each dobutamine dose administration. The inset shows the change in QT interval from baseline to each of dobutamine doses. View Figure 2
Figure 2: Shows the mean QT interval (+ SD) at the end of each dobutamine dose administration. The inset shows the change in QT interval from baseline to each of dobutamine doses. View Figure 2
The new QTc was not significantly different at the different dobutamine dosages and there was no significant change in QTc across the different dobutamine doses (Figure 3).
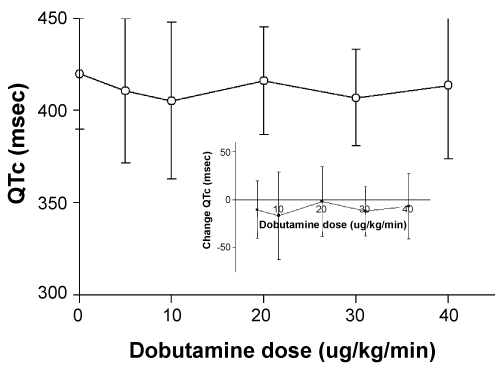 Figure 3: Shows the corrected QT interval (mean + SD) at the end of each dobutamine dose administration. The inset shows the change in corrected QT interval (mean + SD) at the end of each dobutamine dose administration. View Figure 3
Figure 3: Shows the corrected QT interval (mean + SD) at the end of each dobutamine dose administration. The inset shows the change in corrected QT interval (mean + SD) at the end of each dobutamine dose administration. View Figure 3
The heart rate QT relationship was explored in two ways. First the QT interval at the mean heart rate for each stage of the dobutamine dosages was examined (Figure 4). There was a significant negative correlation between the two factors as the QT interval reduction was associated with increasing heart rates. In contrast, there was no such relationship for the new QTc formula.
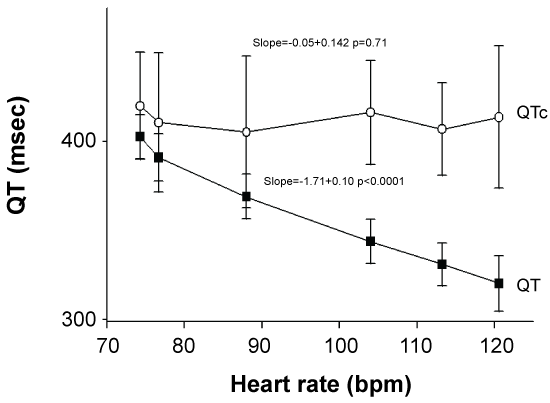 Figure 4: Shows the QT interval at the mean heart rate for each stage of the dobutamine dosages for uncorrected QT (solid squares) and QTc (open circles).
View Figure 4
Figure 4: Shows the QT interval at the mean heart rate for each stage of the dobutamine dosages for uncorrected QT (solid squares) and QTc (open circles).
View Figure 4
Because the relationship of QT to heart rate can vary between individuals [8], this relationship was examined for each individual. This is exemplified in one case in which the QT interval at each heart rate is displayed. The significant negative correlation between QT and heart rate was eliminated by the new correction formula (Figure 5). QT interval at each heart rate for each individual was examined (Figure 6). Because the goal of an adjustment formula is to produce QTc values that are not correlated with heart rate i.e. the slope of QTc/RR regression being zero, the linear slope for each individual was calculated. The mean value for the QTc was close to zero i.e. -0.20 + 0.58 msec/bpm and was significantly (p < 0.001) less that the uncorrected QT which had a slope of -1.89 + 0.56 msec/bpm.
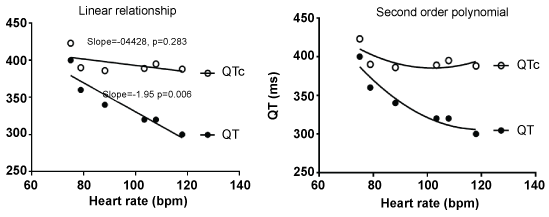 Figure 5: Shows a case with the QT interval for heat heart rate for uncorrected QT (solid squares) and QTc (open circle). The linear slope for each relationship (QT-Heart rate) is shown along with the significance level indicating whether the slope of the relationship is different from zero i.e. no relationship between QT interval and heart rate.
View Figure 5
Figure 5: Shows a case with the QT interval for heat heart rate for uncorrected QT (solid squares) and QTc (open circle). The linear slope for each relationship (QT-Heart rate) is shown along with the significance level indicating whether the slope of the relationship is different from zero i.e. no relationship between QT interval and heart rate.
View Figure 5
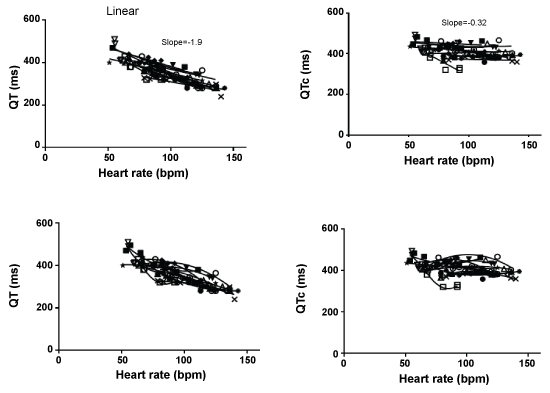 Figure 6: Shows the QT interval at each heart rate for each individual and each line represents the relationship for each individual with the QT interval (left panel) and corrected QT interval (right panel). The linear slope QT-Heart rate is shown for all the individuals and represents the mean + SD from each individual.
View Figure 6
Figure 6: Shows the QT interval at each heart rate for each individual and each line represents the relationship for each individual with the QT interval (left panel) and corrected QT interval (right panel). The linear slope QT-Heart rate is shown for all the individuals and represents the mean + SD from each individual.
View Figure 6
This is the first study to test the newer QT correction formula in the setting of intra-individual changes in heart rate. The increase in heart rate was induced by catecholamines. The new formula was found to be relatively independent of heart rate. These data suggest that this QT correction formula should of considerable value in identifying drug toxicity and electrolyte imbalance in patients with increases in heart rate [1,2,4,5]. QT heart rate adjustment formulae, including the one used herein, were been developed after examination of the QT intervals in different persons with different heart rates. This kind of analysis includes between person variability of QT assessment in addition to considerations of QT-heart rate relationship. Thus there is concern about the extent to which between individual variability influences the validity of a QTc formula i.e. persons with faster heart rates may have different myocardial characteristics that are determinants of QT duration, compared to persons with slower heart rates [8]. Instead the present study evaluated the change in heart rate in the same individual and examined its impact on the QT interval.
Two kinds of data analysis were used-an assessment of group data at each dobutamine dose and an assessment of the change in QT with change in heart rate for each individual. Using the first approach there were little differences in the QTc with increases in heart rate. Because an individual data approach has been proposed as the optimal one to adjust for changes in QTc [8], the slope of the QTc-heart rate relationship was evaluated in each individual as heart rate was increased. The inverse correlation between QT interval and heart rate was obliterated by the new QTc formula.
Heart rate was increased by administration of dobutamine. This study elucidates the differences of opinion on the effects of dobutamine on QTc in the very few studies that have previously commented on this question [9-11]. The present study showed no significant effect of dobutamine on QT interval once the QT interval has been corrected for the effect of heart rate. Dobutamine-induced stress cardiomyopathy was reported to be associated with prolonged QTc but the kind of correction formula was not specified [12]. This data also has specific relevance to the assessment of the QT interval in situations of catecholamine administration or excess. Catecholamine administration has been proposed as a diagnostic tool to unmask concealed long QT Syndrome [13]. Hyper adrenergic states are present in a number of clinical conditions and those associated with psychiatric conditions or in critically ill patients where the measurement of QT interval is an important consideration for assessment of drug toxicity or electrolyte abnormalities [2,4,14].
There are several limitations of this study that warrant further discussion. First, the sample size was relatively small. Dobutamine is a relatively infrequently used method to induce myocardial stress for imaging so that such cases are infrequent. Second, the effects of dobutamine entails considerations of its kinetics in the circulation (pharmacokinetics) and binding to relevant cardiac receptors which are manifested as immediate responses as well as a mono-exponential response to a new steady-state value [11,15]. Third, evaluation of a new QT correction formulae confront the challenge of the absence of a true (gold) standard against which a new formula can be judged. Fourth, there was no correction for QT/RR hysteresis i.e. the QT interval duration is not only dependent on the simultaneously measured RR intervals but also on the prior RR intervals. How quickly the QT interval adapts to heart rate changes and how long is the 'memory' of previous RR intervals stored in the myocardium is difficult to ascertain with the dobutamine infusion protocol which involves a stepwise increase in dobutamine concentration in order to ensure significant increases in heart rate. Auto-regression equations have been developed to minimize hysteresis but they require prolonged recordings at steady state [16]. In the absence of such prolonged observation periods, investigators have suggested using the heart rate correction formula at a fixed time interval [16] such was used in the protocol in this study. The QT interval in the present study was measured after 3 min of dobutamine infusion at each dosage.
The newer QT-heart rate correction formula provides a very good adjustment for increases in heart rate. Clinical practice should consider switching to the newer formula especially in conditions of faster heart rates.
None.