Human herpes virus infection induces lifelong latent infection that most likely reactivates when the immune system deteriorates. It usually presents with localized, painful vesicular rash in one or contiguous dermatomal distributions. Although, more serious manifestations like aseptic meningitis, acute retinal necrosis, herpes zoster ophthalmicus and Ramsay Hunt syndrome especially in the immunocompromised. We report a case of 2-dermatomal cutaneous herpes zoster in an adult in the tropic with vitamin D deficiency.
Herpes zoster, Immunocompetent, Tropic, Vitamin D
Herpes zoster, well known as shingles is caused by the reactivation of dormant Varicella-Zoster virus which travels from dorsal root ganglion through the sensory nerves down to the dermatomal skin for the manifestation of its characteristic vesicular rashes [1]. There is often a prodrome of headache, malaise, followed by paresthesia, pain, itching and rashes along the dermatomal distribution on the thorax or face [2]. Varicella-Zoster virus is human double stranded DNA virus with manifestation of primary infection as chicken pox or varicella which present clinically as disseminated painful vesicular rashes typically in the childhood [1].
Varicella zoster virus-specific cell mediated immunity is required to halt this viral reactivation and this immunity is strong in the younger ages [2]. This explains the relatively low incidence of shingles in the lower age groups. The cell mediated immunity decreases with aging, and this correlates with increased incidence of herpes zoster in the elderly [4]. Those patients with T-cell deficiency like HIV patients, bone marrow transplant recipients can present with severe forms of herpes zoster [1]. Humoral immunity does not play a role in the protection against the reactivation of herpes zoster virus as antibodies levels are relatively preserved throughout all age groups [3].
The deficiency of vitamin D has been implicated in the pathogenesis and complications of herpes zoster [5,6]. However, it is concluded that good exposure of sunlight at the tropics gives adequate vitamin D [7].
Therefore, we present a report of herpes zoster in a middle aged immunocompetent man with vitamin D deficiency at the tropic.
A 42-year-old male banker presented to the anesthesia pain clinic with one day history of gradual onset of severe burning constant pain at the right anterior chest wall below the right nipple. There was no known relieving factor but it was aggravated by mobility. There was associated malaise but no history of insect bite, trauma, fever, nausea or vomiting. There was a history of recent 2-month vacation spent in United States during winter. Patient has taken Tylenol but there was minimal relief. Past medical was remarkable for chickenpox infection during childhood, no varicella vaccination. Family history was not contributory. On a level of 0-10 scale of assessment, patient rated his pain as 10. Physical examination revealed an increased in blood pressure (142/94 mmHg) and heart rate (102/min). His weight was 70 kg and height 174 cm. There was no peripheral lymphadenopathy, organomegaly or muscle wasting.
There was diffuse tenderness at the right antero-lateral dermatomal level of T5-T6, no erythema. A provisional diagnosis of shingle (prodrome pain), to rule out tietze disease was made. Chest X-ray was ordered while blood samples were collected for blood work. Patient was given intravenous 75 mg pethidine and 30 mg ketorolac. He was observed for 8 hours and allowed to go home on oral 75 mg tramadol 6 hourly when his pain scale was 3.
The patient presented with the following day with multiple erythematous vesicular itchy rashes at the same dermatomal level of T5 and T6 (Figure 1). The results of the blood work and Chest X-ray were normal except cholecalciferol which was 11 ng/ml. Patient was the started on oral 800 mg acyclovir 5 times daily for 1 week, 1000 IU cholecalciferol daily for 1 month, 10 mg loratadine 8 hourly for 5 days and to continue tramadol for extra 5 days. He was subsequently counseled to be exposed to the sunlight at least 30 minutes daily. Follow up visit a week later showed the herpes zoster blisters and discomfort have resolved with no residual neuralgia, although there was still skin dyspigmentation.
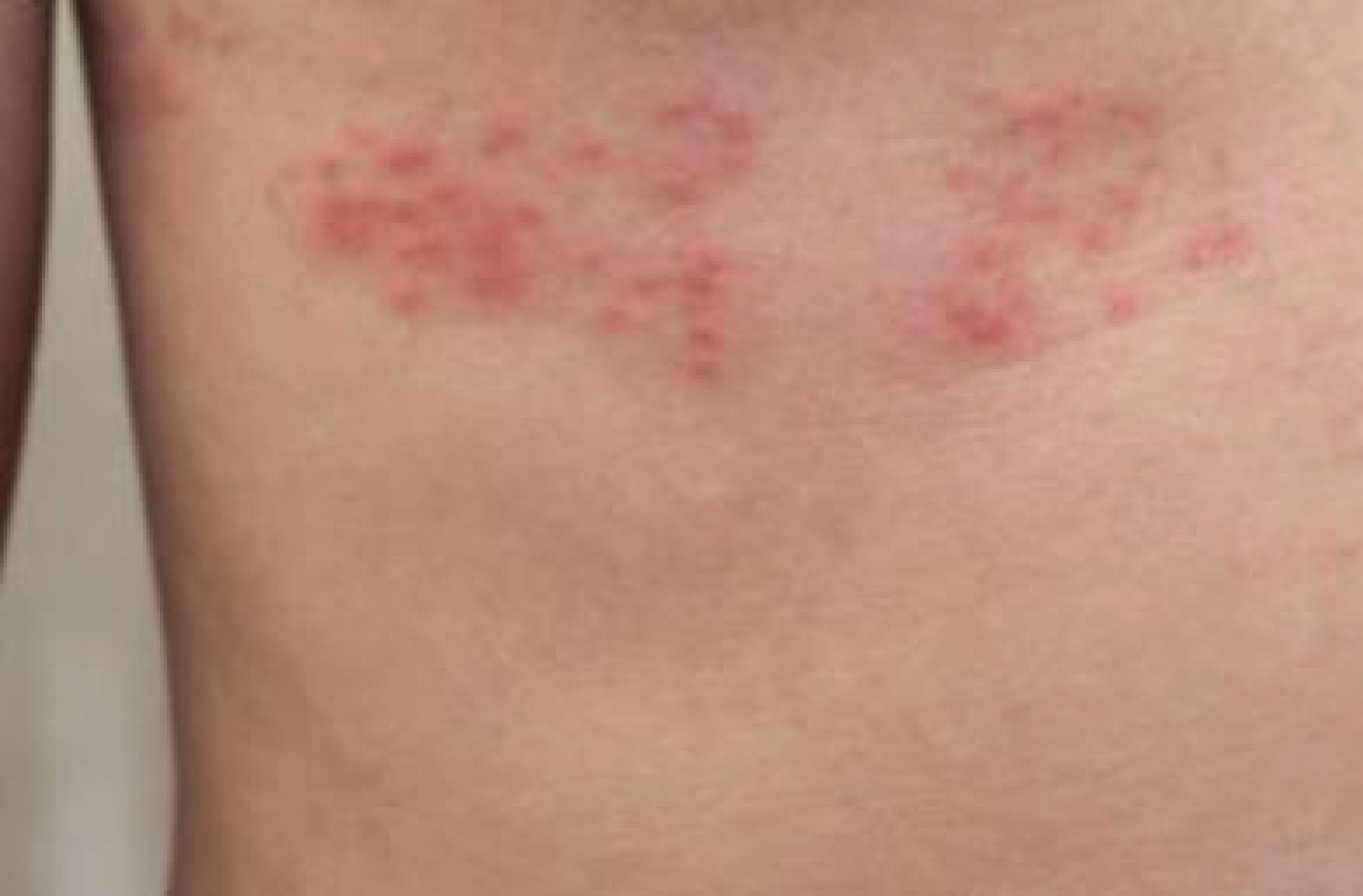 Figure 1: Erythematous rashes at the antero-lateral T5 and T6 dermatomes. View Figure 1
Figure 1: Erythematous rashes at the antero-lateral T5 and T6 dermatomes. View Figure 1
The onset of herpes zoster is often heralded by pain and paresthesia within the dermatome(s) by 48 to 72 hours which is followed by areas of erythema. Subsequently, discrete vesicles appear in the distribution of the dermatome that correspond to the infected dorsal root ganglion but does not cross the midline [8]. The diagnosis of herpes zoster is clinically done with clinical appearances and characteristic symptomatology. The most common risk factor for herpes zoster is a decrease in immunity. In such immunocompromised individuals, the herpes zoster lesion may involve multiple dermatomes or wide disseminations in up to 10% of the individuals but rare in immunocompetent individuals [8,9]. Advancing age is another risk factor for herpes zoster especially in the immunocompetent individuals [10-12].
Our patient was a middle aged man, immunocompetent based on history, physical examination findings (no fever, weight loss, lymphadenopathy, organomegaly), laboratory results (normal complete blood count, random plasma glucose, negative HIV screen) and good response to oral acyclovir. He was not on any immunosuppressive medication and did not have any obvious malignancy. However, there was a deficiency of vitamin D noted on the laboratory test. There is increasing evidence of association of vitamin D with reactivation of herpes zoster as shown by Chao, et al. in their study [6]. In another study [5], vitamin D was shown to be closely linked to the clinical courses of herpes zoster, from pathogenesis to complications. There is a possibility of alteration of immunity by the decreased level of vitamin D as a study [12] has shown. The earlier in vivo demonstration of vitamin D deficiency suppressing cell mediated immunity by Yang, et al. [13] might offer exact explanation for the reactivation of herpes zoster in our patient.
Of particular interest is that the patient lives in a tropical country with abundant sunlight. Sunlight is a good source of vitamin D [7]. It might be possible that our patient had reduced exposure to sunlight as the history revealed 2-month vacation in the United States during winter and he was on no vitamin supplement medication. The reduced sun exposure tilts the balance to increased risk for vitamin D deficiency [14]. It is also reported that people with a naturally darker skin require three to five limes longer exposure to sunlight to make adequate amount of vitamin D [15].
Herpes zoster reactivation is rare in immunocompetent individuals but can occur in people with vitamin D deficiency. This case serves as a reminder to the primary care physicians to encourage the patients to maintain their optimum vitamin D level by adequate sunlight exposure and oral vitamin supplementation.
Nil.
Nil.