The construction of a coaxial circle breathing circuit encloses the inspiratory limb within the expiratory limb to preserve heat, humidity, anesthetic gas, and oxygen. However, the construction also makes kinks or breaks in the enclosed inspiratory limb difficult to detect. With kinking or disconnection of the central inspiratory limb, the patient may rebreathe expiratory gases, leading to a significant increase in dead space and concomitant respiratory acidosis. We describe a clinical case in which a disconnection in the inner inspiratory limb of a King (King Circuits, Noblesville, IN) coaxial breathing circuit resulted in severe respiratory acidosis 4 hours after induction during a craniotomy for tumor resection. Similar cases have been reported in the literature [1-3], but this one differs in the timing of the rebreathing and respiratory acidosis. Therefore, anesthetic providers who are aware that coaxial circuit failures associated with the inspiratory limb can occur at any time during surgery will be in a position to identify the problem early, thereby limiting the degree of respiratory acidosis that develops and reducing the risk of associated complications.
Coaxial circuit failure, Respiratory acidosis, Hypercapnia
The circle breathing circuit is the most widely used breathing circuit in the United States. In a circle system, removal of carbon dioxide (CO2) with a CO2 absorbent allows rebreathing and conservation of exhaled oxygen, anesthetic gases, humidity, and respiratory heat. The circle system consists of a fresh gas inflow source, inspiratory and expiratory unidirectional valves, inspiratory and expiratory corrugated tubing, a Y connector, an overflow valve (also called a pop-off or adjustable pressure-limiting valve), and a reservoir bag. Circle breathing circuits facilitate the use of low-flow systems, and their low resistance makes them appropriate for both pediatric and adult patients.
A coaxial system (King Circuits, Noblesville, IN) is a circle breathing circuit that encloses the inspiratory limb within the expiratory limb. This design decreases the circuit's bulkiness and better conserves the heat and humidity of the inspired gases. However, kinks or breaks in the enclosed inspiratory limb may be difficult to detect. When there is kinking or disconnection of the central inspiratory limb of the breathing circuit, the patient may rebreathe expiratory gases, leading to a significant increase in dead space and concomitant respiratory acidosis. This respiratory acidosis often becomes severe because neither an increase in minute ventilation nor fresh gas flow will correct it. The resulting hypercarbia and decrease in blood pH can lead to cardiac arrhythmias [1], hypoxemia [2], and increased cerebral blood flow, which may cause an increase in intracranial pressure in a patient with an intact cranium. Therefore, prompt recognition and correction remains critical to prevent possible patient injury. We describe a clinical case in which a disconnection in the inner inspiratory limb of a King coaxial breathing circuit resulted in severe respiratory acidosis during a craniotomy for tumor resection.
A male in his 50s with recurrent oligoastrocytoma was scheduled for a bifrontal craniotomy for tumor resection in the Brainsuite (BrainLab, Feldkirchen, Germany), an intraoperative magnetic resonance imaging (MRI) suite. The patient's surgical history included a previous uneventful left frontal craniotomy for tumor resection and an inguinal hernia repair. The patient's preoperative baseline vital signs were: blood pressure, 143/89; heart rate, 82 beats per minute (bpm); respiratory rate, 18 breaths per minute; and oxygen saturation, 96% on room air. The baseline physical exam revealed a healthy-appearing male in no acute distress who was neurologically intact grossly; the patient had clear breath sounds bilaterally and heart tones that were regular in rate and rhythm. The patient had a normal airway exam with a Mallampati class 3 score.
In the anteroom of the Brainsuite, the patient underwent a smooth intravenous induction with fentanyl, lidocaine, propofol, and cisatracurium. The providers intubated the patient with an 8.0 single-lumen cuffed endotracheal tube and confirmed proper placement with measurement of positive end-tidal CO2 (ETCO2) and auscultation of equal breath sounds bilaterally. The patient was mechanically ventilated using the Dräger Fabius® MRI anesthesia machine (Draeger Medical Inc, Telford, PA) set to volume control mode with minute ventilation of 9.8 L and FiO2 of 0.6, achieving an ETCO2 in the mid-20s. Anesthesia maintenance consisted of sevoflurane and continuous infusions of remifentanil, propofol, and cisatracurium.
The surgeons placed the patient's head in 4-point pins, and he was subsequently transported into the operating room of the suite. After completion of a preoperative MRI scan, the patient was prepped and draped in the standard manner. The surgical incision was made and the surgery proceeded uneventfully for the first 3 hours. At that time, the providers moved the patient into the MRI scanner for an intraoperative MRI.
During the move, the CO2 water trap cassette that attaches to the MRI-compatible monitor was inadvertently dislodged from its holder. After replacing the CO2 water trap cassette, the providers observed an abnormal capnogram depicting an ETCO2 waveform with a continuous expiratory wave lacking an inspiratory break; the ETCO2 and fractional inspiratory CO2 values were nearly equal. To rule out failure of the CO2 water trap and capnography sampling line, the providers replaced those components, but the patient's abnormal capnogram persisted. The providers also checked the circuit, which consisted of multiple extensions to allow for adequate distance between the ventilator and the patient when positioned in the bore of the magnet, for visible defects but found no compromise. While utilizing manual ventilation, the providers confirmed that the patient was receiving adequate ventilation by observing bilateral chest rise and auscultating equal breath sounds bilaterally.
In addition to the abnormal capnogram, the providers observed progressive increases in the ETCO2 reading, from 24 to 50 mmHg, and heart rate, from 70 to 90 bpm. However, the patient's blood pressure, oxygen saturation, and temperature remained stable. The soda lime CO2 absorbent was checked, but there was no evidence of saturation or retained heat, as the container was not warm to the touch. Although the patient had previously undergone general anesthesia twice without adverse events, the elevated ETCO2 readings raised concerns for a hypermetabolic syndrome, so the emergency cart was made available and an arterial blood gas was drawn. The providers discontinued the inhalational agent and converted the patient to total intravenous anesthesia with continuation of the propofol, remifentanil, and cisatracurium infusions. The patient was also placed on 100% oxygen and fresh gas flows were increased from 2 to 10 L/minute.
To allow for closer inspection of each circuit component, the neuro-anesthesiologists detached the entire circuit from the patient and ventilated the patient with a bag valve mask. To assess the integrity of the inner tube, the providers applied lateral force to the circuit, flexing each extension at its base to make any defect more visible. Two breaks in the central inspiratory limb of the distal extensions were found. Both extensions were replaced, after which the patient's capnogram normalized. The ETCO2 reading also began to trend downward, quickly normalizing to baseline values in the mid-20 s.
The blood gas results drawn before the defective coaxial circuits were identified revealed severe respiratory acidosis, with: pH 7.16; PaCO2 79 mmHg; PaO2 386 mmHg; HCO3 28 mmol/L; lactate 0.3 mmol/L; base excess -2 mmol/L; Na+ 140 mEq/L; and K+ 4.2 mEq/L. At the time the blood gas results were obtained, the ETCO2 was 81 mmHg. By the providers' estimate, the time from first appearance of the abnormal capnogram to discovery of the faulty circuit extensions was 15 minutes.
The remainder of the surgery proceeded uneventfully and the patient was extubated in the operating room. He recovered in the postoperative anesthesia care unit with subsequent admission to the neurosurgical care unit. After a routine postoperative course, the patient was discharged home on postoperative day 2 in good condition. He did not suffer any apparent short or long-term effects from his intraoperative episode of hypercapnia and severe respiratory acidosis.
Hypercapnia is increased arterial CO2 tension that results in respiratory acidosis. During general anesthesia, the presence of hypercapnia presents as hypercarbia, or elevated ETCO2. Causes of intraoperative hypercapnia include reduced minute ventilation, increased CO2 production, or decreased elimination. Reduced minute ventilation may be due to either hypoventilation or increased alveolar dead space (and consequent decrease in alveolar ventilation) [4]. Because this patient was mechanically ventilated with adequate tidal volume and respiratory rate, which were both unchanged for over 3 hours of surgery, the providers ruled out hypoventilation as a cause for the elevated CO2. Decreased alveolar ventilation can occur in the setting of mechanical ventilation if there is too much positive pressure exerted resulting in compression of the pulmonary vasculature. Furthermore, both active bronchospasm or intrinsic lung disease can also increase alveolar dead space and arterial CO2 tension. However, the patient had normal peak airway pressures and did not have evidence of wheezing on physical exam nor a history of pulmonary disease. Based on these findings, decreased alveolar ventilation was ruled out as a cause for the elevated CO2.
Increase CO2 production can result when a patient is in a hypermetabolic state. Intraoperatively, hypermetabolic conditions include malignant hyperthermia (MH) and sepsis. Signs of MH include an elevated ETCO2 that does not improve with increasing ventilation, generalized muscle rigidity, hyperkalemia, tachycardia, myoglobinuria, and hyperthermia. Laboratory findings include the presence of metabolic acidosis and elevated creatine kinase. Although precautionary measures were taken to treat presumptive MH, the absence of generalized muscle rigidity, metabolic acidosis, hyperkalemia, and hyperthermia helped to rule MH out as a cause for the elevated CO2. Although sepsis can mimic MH in its presentation with associated signs of fever, tachycardia, metabolic acidosis, and elevated creatine kinase, its diagnosis usually relies on identification of an infectious source and associated hypotension, both of which were not present in this patient [5,6].
In the setting of mechanical ventilation, technical problems that either compromise ventilation or CO2 elimination should be considered as potential causes of elevated CO2. Impaired ventilation may result from either bronchial obstruction or mainstem intubation. However, normal peak airway pressures and the presence of bilateral breath sounds on physical exam helped to rule out impaired ventilation as a cause for this patient's hypercapnia. Other technical problems may arise from ventilator-associated failures that impair CO2 elimination. These equipment failures, which include a faulty expiratory valve, exhausted CO2 absorbent, or a defective breathing circuit, can cause rebreathing of expired gas and consequent hypercapnia. To distinguish between a faulty expiratory valve and exhausted CO2 absorbent, the providers increased the fresh gas flow by three-fold and noted that it had no affect on the ETCO2. Increased fresh gas flow will help normalize ETCO2 in the setting of an exhausted CO2 absorbent but does not affect hypercarbia resulting from a faulty expiratory valve [7]; therefore, the providers were able to exclude the CO2 absorbent as a cause for the rebreathing. Although not done in this case, the next step would have been to replace the valve components and/or change the ventilator if the providers suspected the expiratory valve was the problem.
Ultimately, what the providers found was a disconnection in the central inner tube of the coaxial breathing circuit that resulted in rebreathing of expired gases and severe respiratory acidosis. The lateral force or stretching of the coaxial tube when the patient was moved into the MRI scanner for the intraoperative scan likely caused the tube to disconnect. The disconnection was difficult to detect because of its location within the inner coaxial tube and subtle appearance. In fact, the disconnection only became obvious when the providers actively applied lateral force to the circuit, bending it at its base in order to expose the defect (Figure 1). Consequently, the displacement of the inspiratory limb compromised the integrity of the circle system and its ability to remove expired CO2.
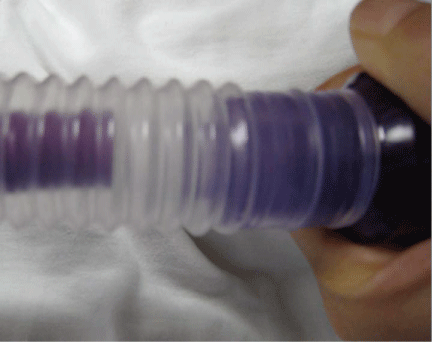 Figure 1: Actual defective co-axial circuit extension discovered intraoperatively. The disconnection in the central inspiratory limb is more visible with stretching and flexion of the circuit.
View Figure 1
Figure 1: Actual defective co-axial circuit extension discovered intraoperatively. The disconnection in the central inspiratory limb is more visible with stretching and flexion of the circuit.
View Figure 1
Similar cases have been reported in the literature [1-3], but this one differs in the timing of the rebreathing and respiratory acidosis. In previous reports, the hypercarbia and acidosis developed within 90 minutes or less after surgical incision, when movement of the anesthesia machine after induction and intubation caused a misassembled circuit and/or extension set to malfunction [1-3]. However, in the current case, the providers assume that the circuit and extension sets were initially intact, since positioning of the patient after intubation and movement of the patient from the induction room to the operating room did not compromise the patient's ventilation.
To determine a possible explanation for the 4 hour delay in the appearance of the circuit defect, the providers assessed several new King circuits and found that nearly all of the inspiratory limbs of these circuits could be disconnected by applying lateral force. We speculate that exposure of the circuit to the heat and humidity of rebreathed gases during routine ventilation may have compromised the mastic holding the central inner tube intact. As a result, less force was needed to displace the central inner coaxial tube in this case. Thus, in this scenario, movement of the patient into the MRI scanner may have created enough lateral force to cause the circuit to become compromised.
Because the circuit was intact at the start of the surgery, it would have been difficult to prevent the subsequent disconnection of the central inner tube. However, anesthesia providers who are aware of the possibility of coaxial circuit failures associated with the inspiratory limb will be in a position to identify the problem early, thereby limiting the degree of respiratory acidosis that develops and reducing the risk of associated complications. However, other potential causes of rebreathing of CO2 to consider include malfunctioning valves, depleted CO2 absorbent, and excessive gas channeling through the absorbent. We recommend visually inspecting the circuit as part of the routine machine and equipment check during anesthetic preparation and in the event of any derangement of physiologic parameters intraoperatively. In compliance with FDA requirements, the providers contacted the manufacturer and recommend that other providers do the same when they detect problems with circuits or extensions.
Of note, informed consent for this case report was not obtained from the patient due to the fact that he was deceased at the time the manuscript was prepared and submitted. However, no patient identifiers have been included.