Telemedicine, Heart failure, Geriatrics
Chronic diseases, e.g. chronic heart failure (CHF), diabetes mellitus (DM), and chronic obstructive pulmonary diseases (COPD), remain serious diseases in terms of their functional or survival prognosis, and morbidity and mortality are high [1]. This applies particularly well to CHF, in which the mortality rate of patients with stage III-IV disease according to the NYHA classification is at least currently around 30% at 5 years in more recent studies. The cost of these chronic diseases has rocketed, and is estimated at several billion dollars in developed countries. What's more, these patients are often elderly and have one or more chronic diseases. Thus, their management is a challenge for healthcare professionals. Their needs eat up large amounts of medical resources, just as a shortage in the time careers can provide is beginning to be felt, with medical deserts and a lack of access to healthcare professionals, e.g. Family Doctor and Nurse, among other problems.
Patients with these chronic diseases, e.g. CHF or COPD, frequently present for emergency hospitalization and rehospitalization, which impairs the quality of their life. Some of these hospitalizations could be avoided if patients took greater responsibility for their disease and were followed up better. This last point has been particularly well documented in CHF and DM. Telemedicine may be of aid in this setting. Indeed it may even optimize the management of such chronic diseases, particularly by preventing emergency and repeat hospitalizations [2]. From the perspectives of the health care system, the management of these chronic diseases is also very expensive with an economic cost and a cost in time of health professionals, especially in doctor's time. It may also make it possible to structure integrated care pathways. In this setting, Nurses can play a major role in monitoring patients, particularly in case of telemonitoring. Above all, they can also play a key role in coordinating the care pathways of their patients with chronic diseases. This is the case in France, where telemedicine and therapeutic education led to the delegation of medical tasks to nurses.
Since the beginning of the 2000's, numerous telemedicine projects have been conceived and developed in the area of chronic diseases, especially in CHF [2]. Practically all of them have investigated telemonitoring (or tele management, as it is also known). The results of those telemedicine projects differed from study to study and were fairly inconclusive regarding any potential clinical benefit in terms of, for instance, rehospitalization or a decrease in morbidity and mortality. Nevertheless, several reviews and meta-analyses seem to have shown an undeniable utility for telemedicine. Moreover, all these projects have demonstrated an economically beneficial. Depending on the study, the savings were calculated to be between $5,000 and more than $50,000/year/patient depending on the stage of HF and the setting of the study [2]. It is worth bearing in mind that those projects, particularly the earlier ones, more closely resembled telephone follow-up with care providers with a Nurse traveling to the patient's home. Hence in our opinion those studies represent the first generation of telemedicine projects: "telemedicine 1.0" [3].
Over the last 4 to 5 years, a second generation of projects has emerged in the chronic diseases area, e.g. in the CHF or DM area, particularly in developed countries, e.g. in France [3]. These projects are known as "telemedicine 2.0", because they utilize the new Information and Communication Technology (ICT) and the web. Most of these projects rely on the usual connected tools for monitoring chronic diseases, as such as blood pressure meters, weighing scales, and pulse oximeters in CHF, or glucometers in DM., which relay the information collected via Bluetooth, 3G or 4G and incorporate tools for interaction between the patient and healthcare professionals, particularly the patient's Nurse, like telephone support centers, tablets, and websites [3,4]. Some of them also provide tools for motivation and education, and occasionally, questionnaires about symptoms, such as dyspnea, palpitation and edema as experienced by the patient. The leaders of the industrial world, e.g. Air Liquide, Philipps, Sanofi, Abbott, are beginning to take an interest in this subject. It should be noted that all these projects give Nurses a significant role.
We have developed in Strasbourg such of "telemedicine 2.0" project, centered on the patient's Nurse and Family Doctor. The E-care has been developed to optimize the home-monitoring of CHF patients. It detects situations in which there is a risk of cardiac decompensation and rehospitalization, and it does this via a telemonitoring 2.0 platform [5,6]. The E-care platform generates indicators of a worsening of the patient's health status. These "warning alerts" are generated for any HF decompensation that may lead to hospitalization if not treated. Between February 2014 and April 2015, 175 patients (mean age: 72 years; mean Charlson index: 4.1) were included in an experimentation of the E-care platform. During this period, the E-care platform was used on a daily basis by patients, the patient's Nurse and the family Doctor, according to a defined protocol of use specific to each patient. During the study, the E-care system generates 700 alerts in 68 patients. Retrospective analysis of the "warning alerts" showed that the E-care platform automatically detected any worsening of the cardiac function with sensitivity, specificity, and positive and negative predictive values of respectively, 100%, 72%, 90% and 100% [7]. Both the patient's Nurse and Family Doctor, and all the patients, even the frailest, used the E-care system without difficulty until the end of the study. In the present experience, "warning alerts" have preceded cardiac decompensation for up to 5 days. In this experiment, Nurses had a key role (Figure 1). They received the alerts. They treated them according to a pre-defined protocol and called if necessary the family Doctor.
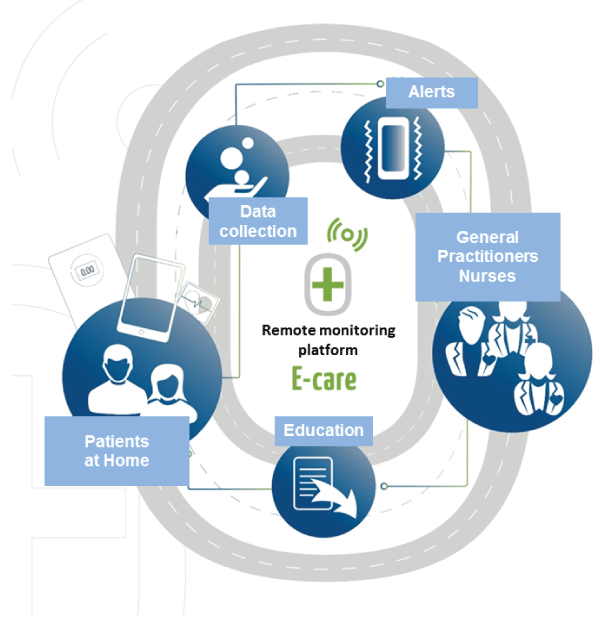 Figure 1: Key role for the patient's Nurse and the family Doctor. In detail, the role of nurses was planned from the start of the E-care project. The latter was supervised as provided by Article 51 of the French Social Security Financing Act, as part of a delegation of tasks. In this setting, their first mission was to make sure that the patient took the constants correctly and respected the protocol. For the non-autonomous patients, they realized themselves taking constant. They received the alerts and had to treat them according to a protocol well-defined by the care team and personalized according to the patient status. They had to warn the doctors in charge of the patient in case of situations at risk of cardiac decompensation. They also had the mission to continuously achieve a hygienic and dietary education of the patient and to insist on the respect of the observance by the latter. View Figure 1
Figure 1: Key role for the patient's Nurse and the family Doctor. In detail, the role of nurses was planned from the start of the E-care project. The latter was supervised as provided by Article 51 of the French Social Security Financing Act, as part of a delegation of tasks. In this setting, their first mission was to make sure that the patient took the constants correctly and respected the protocol. For the non-autonomous patients, they realized themselves taking constant. They received the alerts and had to treat them according to a protocol well-defined by the care team and personalized according to the patient status. They had to warn the doctors in charge of the patient in case of situations at risk of cardiac decompensation. They also had the mission to continuously achieve a hygienic and dietary education of the patient and to insist on the respect of the observance by the latter. View Figure 1
In detail, the role of nurses was major in the E-care project, as in other recent telemedicine projects. In the aforementioned project, this role was planned from the start of the E-care project (Figure 1). The latter was supervised as provided by Article 51 of the French Social Security Financing Act ("article 51 de la Loi de Financement de la Sécurité Sociale française"), as part of a delegation of tasks ("délégation de tâches") [2]. In this setting, their first mission was to make sure that the patient took the constants correctly and respected the protocol. For the non-autonomous patients, they realized themselves taking constant. They received the alerts and had to treat them according to a protocol well-defined by the care team and personalized according to the patient status. They had to warn the doctors in charge of the patient in case of situations at risk of cardiac decompensation. They also had the mission to continuously achieve a hygienic and dietary education of the patient and to insist on the respect of the observance by the latter. As a result, their functions were upgraded.
As demonstrated by the E-care project, the "telemedicine 2.0" projects are perfectly compatible with the care pathways being developed in chronic diseases by the developed countries health authorities. What's more, all these findings should be analyzed with regard to the benefit of these telemedicine solutions. This experience may lead us to witness the birth of the medicine of tomorrow! In the field of chronic diseases, given the epidemiology and expected shortage of time careers can provide, what we need is better follow-up and better education, improved prevention and anticipation, but, above all, better selection of the patients whose use of the healthcare system will be indispensable [2,8]. In this setting, telemedicine represents an opportunity to upgrade the function of the Nurses!
The authors state that they have no conflicts of interest to declare except Mr. M. Hajjam, who is the science director of the company PREDIMED Technology.
E-care was funded by the first call for tenders of the 2014 "Investment in the Future" initiative in France. PRADO INCADO is funded by the regional health agency of the north-east of France.