Myocardial Bridging (MB) is a congenital anomaly in which a segment of a coronary artery takes a "tunneled" intramuscular course under a "bridge" of overlying myocardium. The first reference of MB in coronary arteries, the association with angina and anatomically as referred by Reyman in 1737. Considered a "benign" finding since the myocardial bridge causes coronary artery narrowing during systole therefore myocardial bridges should not compromise blood supply to the musculature during diastole. The Left Anterior Descending coronary (LAD) is the most frequently affected vessel (70% in an autopsy series) and in some cases hearts contain more than one bridge, affecting the same vessel or different coronaries.
MB also has been associated with angina, myocardial infarction, arrhythmia, depressed left ventricular function, left bundle branch block, myocardial stunning, apical ballooning syndrome, early death after cardiac transplantation, and sudden death. The MB is a clinical condition with several possible manifestations, and its clinical relevance is debated.
The classification used for decision making proposal for Schwarz based on Clinical-Angiographic Data and Long-Term Follow-Up, with angiographic finding and relationship with symptoms only in MB over the LAD. The new technologies as intravascular ultrasound and valuation in Fractional flow reserve or Cardiac Computed Tomography Angiography (CCTA) they allow to visualize the coronary anatomy with more precision and better visualization of MB not only in LAD besides that study in another arteries (branch arteries), not only in LAD and correlate the symptoms with these findings.
Congenital coronary anomalies detected by CCTA compared to invasive coronary angiography are evidenced in studies. A new terminology and assessment to studies are necessary according to current technologies. The assessment and implications of MB not only in the main arteries (LAD), but also in the branches of the coronary arteries.
Myocardial bridging, Tunneled artery, Coronary angiography, Ultrasound, Cardiac computed tomography angiography
The first reference of MB was Reymann, H, the anatomically description Published in the Dissertationem inauguralem De Vasis Cordis Propriis, written in Latin, described anatomically the presence of MB in a description and their relationship with angina in 1937. When noted this anatomy in human heart. Described was a congenital variant of a coronary artery in which a portion of an epicardial coronary artery (most frequently the middle segment of the LAD takes an intramuscular course [1]. The relation of MB in coronary arteries and presence of angina was described by Black S in 1796 [2]. An in-depth analysis of autopsy samples was presented by Geiringer E, et al. in 1951 [3]. In 1960 Porstmann W publish "The mural coronary" described abnormal finding of MB in the angiographic study [4]. In 1961, Polacek was the first to use the term "myocardial bridge" when described these formations calling them as MB, referred occur in 85.7% of all hearts; the occurrence is more frequent in the region of the left coronary artery in a study of 70 patients [5] (Figure 1).
The MB in a study of is a clinical condition with several possible manifestations, and its clinical relevance is debated. Kramer J described in 1974 the clinical significance of isolated coronary MB such has benign and frequent condition involving the left anterior descending artery in asymptomatic patients without angina and presence of MB in angiographic study [6].
In a study of coronary angiograms of 64 heart transplant patients were reviewed by Wymore P to determine the incidence of myocardial bridges. Only in 33% of these patients, myocardial bridges were detected, almost exclusively across the mid portion of the left anterior descending coronary artery. This is an evidence for the poor angiography for the diagnostic of MB except in the LAD [7].
The MB is a clinical condition with several possible manifestations. Also has been associated with angina, [8] myocardial infarction, [9] arrhythmia, [10] depressed left ventricular function, left bundle branch block, [11] myocardial stunning, [12], apical ballooning syndrome, [13] early death after cardiac transplantation, and sudden death [14].
In a meta-analysis in MB were included 2519 articles and analyzed 21 articles of these. The presence of MB led to a significantly increased risk for Major Adverse Coronary Events (MACE) - OR = 1.53(1.01-2.30), p < 0.001 and myocardial ischemia [15].
MB represent an anomaly of coronary artery flow in which the branches flowing subepicardial descend into the myocardium more shallow or deeper, and after a shorter or longer intramyocardial flow, it reappears in the subepicardial tissue. Bundles of myocardial fibers, which in the form of small bridges, pass over the corresponding part of the coronary artery ("tunnel" segment), are marked as the MB [16]. Myocardial bridges are most commonly localized in the middle segment of the LAD, in other reports the anatomical variant of ramus intermedius artery presents MB [6,11]. Diagonal and marginal branches may be involved in 18% and 40% of cases [17]. Also has reported the presence of multiple myocardial bridges and left ventricular dysfunction and left bundle branch block, in a patient with angina and positive stress test [11] (Figure 2).
These are distinguished between two types of bridging: Superficial bridges (75% of cases) crossing the artery perpendicularly or at an acute angle toward the apex, and muscle bundles arising from the right ventricular apical trabeculae (25% of cases) that cross the LAD transversely, obliquely, or helically before terminating in the interventricular septum [18] Figure 3.
Only 15% of coronary blood flow occurs during systole, and because myocardial bridging is a systolic finding in angiography. Obviously, this allows only to recognize the muscle bridges in the main coronary arteries. In coronary angiograms MB are to be detected indirectly, based on the systolic reduction of lumen. The tachycardia may worsen ischemia because of a decrease in diastolic filling time and in coronary flow reserve [19]. MB have been described as superficial or deep on the basis of: a) They range from 0.3 to 28 mm in depth, b) Anatomically they consist of either superficial myocardial fibers that traverse over the LAD or deep fibers that encircle the LAD [5,7], and c) Bridges > 5 mm deep are less amenable to surgical myotomy. The hemodynamic impact of myocardial bridging depends on the thickness and length of the bridge, the orientation of the bridge relative to myocardial fibers, and the presence of loose connective or adipose tissue around the bridged segment [18,20].
Coronary artery spasm, first described by Prinzmetal, is not an uncommon and has been recognized as an important cause of chest pain in patients with normal or non- significant obstructive coronary artery and the association of this with MB was also reported [21]. Physiologic evaluation of myocardial bridging performed with dobutamine and evaluated the Fractional flow reserve, evidenced such as dobutamine increased the morphologic and functional severity of MB [22].
The same relationship between alterations in the immunohistochemical expression of three vasoactive agents endothelial Nitric Oxide Synthase (eNOS), endothelin-1 (ET-1), and Angiotensin-Converting Enzyme (ACE) and the occurrence human atherosclerosis was investigated in relation to the MB of the Left Anterior Descending coronary artery (LAD), an anatomical site that experiences increased shear stress [23]. This is a phenomenon relationship with development of in atherosclerotic lesions in MB, but it's as associated too with endothelial dysfunction in patients with angina and non-obstructive coronary artery disease. Patients with MB and endothelial dysfunction had lower WSS in the proximal LAD and greater wall shear stress in the mid-LAD. The presence of MB significantly contributes to low wall shear stress and endothelial dysfunction relationship. It recognized the relation in alteration in vasoactive agent and wall shear stress in endothelial dysfunction and development of atherosclerotic lesions by abnormal function in the endothelium of coronary vessel and promotes the vasospasm artery and presence of angina without atherosclerotic lesions [24].
The segment proximal to the bridge in LAD frequently shows atherosclerotic plaque formation, although the tunneled segment is typically spared [16]. Because low shear stress may contribute to atherosclerotic plaque formation proximal to the bridge, whereas high shear stress may have a protective role within the tunneled segment [25]. Plaque formation is related to the factors described, but additionally to the atherogenic risk factors of the patient. The presence of MB is a proatherogenic process but is related to the patient's age and coronary risk factors. This is evidential by Schwarz E performed a study in patients with chest pain, angiographic MB of the left anterior descending artery without obstructive coronary artery disease. Patients were evaluated for clinical symptoms, objective signs of ischemia by stress test, intracoronary Doppler flow measurement and coronary flow reserve. Coronary flow reserve was significantly higher proximally (2.9 ± 0.9) compared with segments distal to the MB (2.0 ± 0.6, p < 0.01). MB classification for symptomatic patients with MB: Type A: Incidental finding on angiography, no objective signs of ischemia; Type B: Objective signs of ischemia, and Type C: With or without objective signs of ischemia and altered intracoronary hemodynamics (by QCA/CFR/intracoronary Doppler). Types B and C responded well to β-blockers or calcium channel antagonists. Patients with type C refractory to medical therapy were treated with stenting of the MB [26].
The historic gold standard for diagnosing myocardial bridges is Coronary Angiography (CA) with the typical milking effect and a step down-step up phenomenon induced by systolic compression of the tunneled segment [27]. In coronary angiograms MB are to be detected indirectly, based on the systolic reduction of lumen and the milking effect may be missed. The limited frequency of myocardial bridging observed angiographically (0.5% to 16%) is in contrast with that of autopsy studies, which have reported a frequency of 40-80% [27,28]. The new imaging techniques such as Intracoronary Ultrasonography (IVUS) allow an accurate assessment of vascular anatomy. With Doppler studies, the coronary flow reserve measured proximal to the myocardial bridge was normal or slightly reduced and that distal to the bridge was impaired. With the low rate of diagnosis referred by angiography the IVUS, it's an excellent method for studying MB, but not for routine diagnosis of these [29]. When intracoronary Doppler imaging was used, a characteristic early diastolic fingertip phenomenon was observed, but studies performed are only in MB of the LAD. With intravascular ultrasonography, it can be demonstrated that vessel compression within the myocardial bridge is not solely a systolic event but persists throughout a large portion of diastole, can MB proximal and distal pressure measurements [30].
MB can also be visualized with the use of novel noninvasive imaging techniques such as Electron Beam Tomography (EBT) and Cardiac Computed Tomography Angiography (CCTA) (Figure 4 and Figure 5).
The CCTA has as a non-invasive alternative for evaluation of coronary anatomy with a lower referral threshold than coronary angiography. Ghadri J, et al. performed a study with the analysis in morphological features of coronary anomalies can be evaluated more precisely by CCTA than by CA, which might lead to a higher identification of congenital coronary anomalies in CCTA compared to CA. The prevalence of coronary anomalies was 7.9% in CCTA group and 2.1% in CA (p < 0.01). The most commonly coronary anomaly detected by CCTA was myocardial bridging 42.8% and with CA 21.2% (p < 0.01). The authors concluded that the prevalence of coronary anomalies is substantially higher with CCTA than CA even after exclusion of patients with myocardial bridging which is more frequently found with CCTA [31]. The CCTA has seen substantial technical advances over the last decade, particularly regarding spatial resolution and an impressive reduction in radiation dose exposure [32]. The CCTA is considered the primary imaging modality to detect and characterize the anatomy of a Coronary Artery Anomalies (CAA). It has a higher rate of detection of CAA than invasive coronary angiography and other noninvasive imaging modalities, because three-dimensional visualization of the entire coronary tree allows accurate depiction of the origin, course and ending of the coronary vessels [33]. Whenever knowledge of the anatomy of the cardiac vessels is crucial, CCTA represents a highly valuable noninvasive modality because of its capability to visualize the coronary arteries accurately and three-dimensionally, yielding a higher detection rate over invasive coronary angiography Figure 6 and Figure 7. Because of its noninvasive nature, relatively low cost and low radiation exposure, a further increase of the utilization of CCTA may be expected, which may consequently be paralleled by an increasing absolute number of incidentally detected CAA [31]. If necessary, the prospective studies for the evaluation of incidental findings and prognosis.
Medical treatment of MB is described and includes β-blockers with decrease the tachycardia and increase diastolic time, with a decrease in contractility and compression of the coronary arteries [19]. Calcium channel blockers and stents [34]. The frequency of in-stent restenosis requiring target vessel revascularization was 36% and high inflation pressures may be required for optimal stent implantation, with a higher risk of coronary perforation [35]. Nitrates generally should be avoided because they increase the angiographic degree of systolic narrowing and can lead to worsening of the symptoms [36]. The invasive treatment such as minimally invasive Coronary Artery Bypass Grafting (CABG), [37] and surgical myotomy [38]. Surgical treatment with dissection of the overlying myocardium should be limited to patients with symptoms that persist despite medical treatment. Good clinical results have been reported in a small series of patients, although serious complications such as right ventricular perforation and left ventricular aneurysm are possible [39]. In the 2018 the Guideline for the Management of Adults with Congenital Heart Disease, published by Stout K, et al. in the section of Coronary Anomalies and Anomalous Coronary Artery Evaluation, relate to the Clinical Importance of anomalous aortic origin of the coronary artery and Risk of SCD [40]. Referred intramural course of coronary artery into context of this coronary anomaly, but don't have any mention a recommendation about the presence of study in presence of MB.
Additional large multicenter clinical databases are required to evaluate the long-term efficacy of different treatments.
Myocardial bridging is generally considered to be a benign condition, it has been proposed as a cause of angina-like chest pain, coronary spasm, myocardial ischemia, acute coronary syndromes, left ventricular dysfunction, stunning, left bundle branch block and arrhythmias, and even sudden cardiac death. Myocardial bridging must be considered especially in patients at low risk for coronary atherosclerosis but with angina, like chest pain or established myocardial ischemia. The best image for the study MB is the CCTA, they use in patient with symptoms or conditions associated with MB are useful. If necessary, a registry for the incidental finding of MB in the CCTA and long term follow up. Medical therapy with beta-blockers and calcium channel blockers remain the mainstay of treatment. For select patient's refractory to intensified medical therapy, surgical intervention, or less preferably PCI with DES, can be considered. This is not a Coronary Anomaly? This is an unforgotten entity in several recommendations. Larger registries and randomized clinical trials are warranted to shed light on optimal strategies for patients with myocardial bridging.
None.
The author declares that they have no conflict of interests.
None.
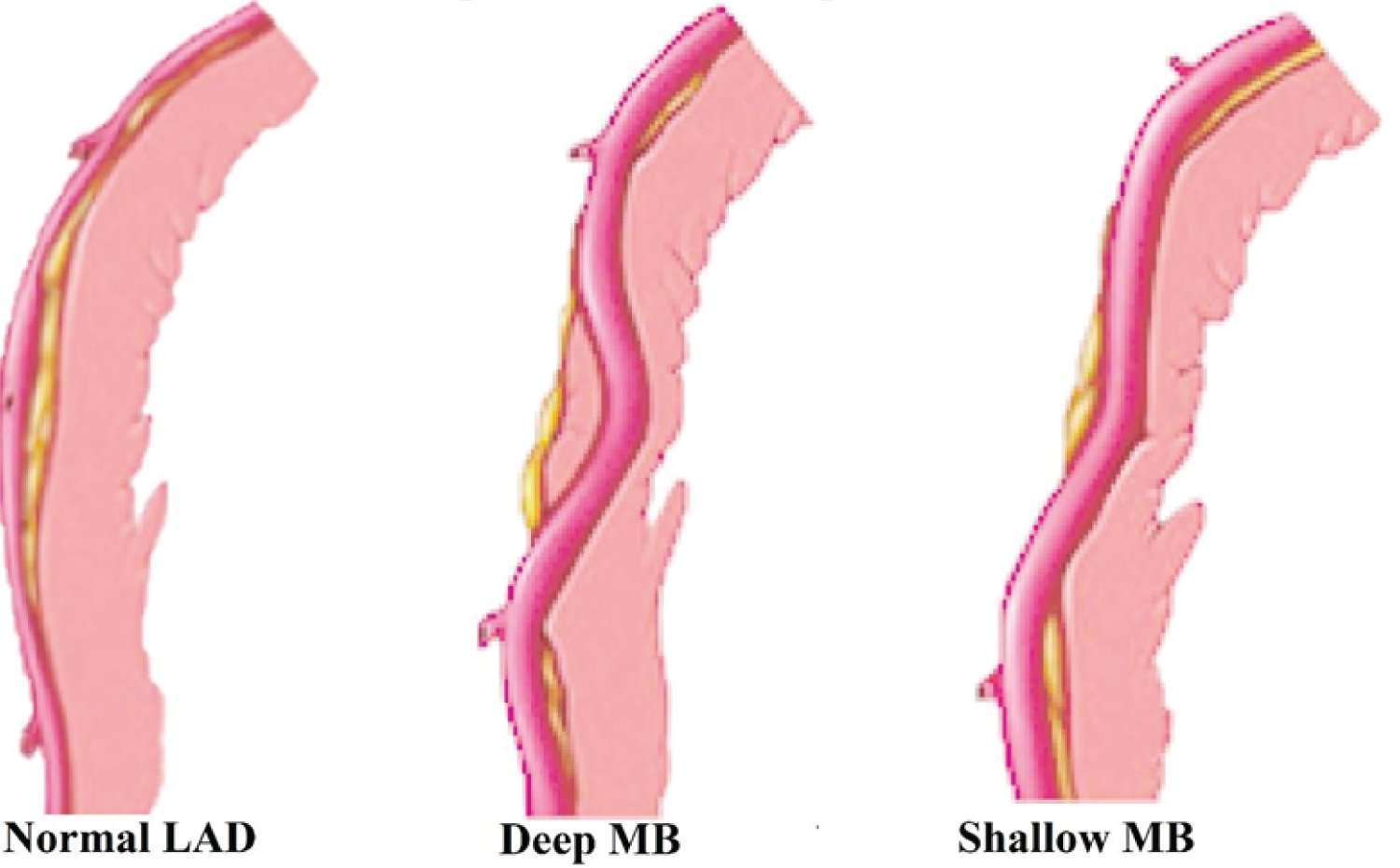
Figure 1: Illustration depicting normal coronary artery anatomy in LAD, deep MB and shallow MB in LAD.
LAD: Left Anterior Descendent Artery; MB: Myocardial Bridge.
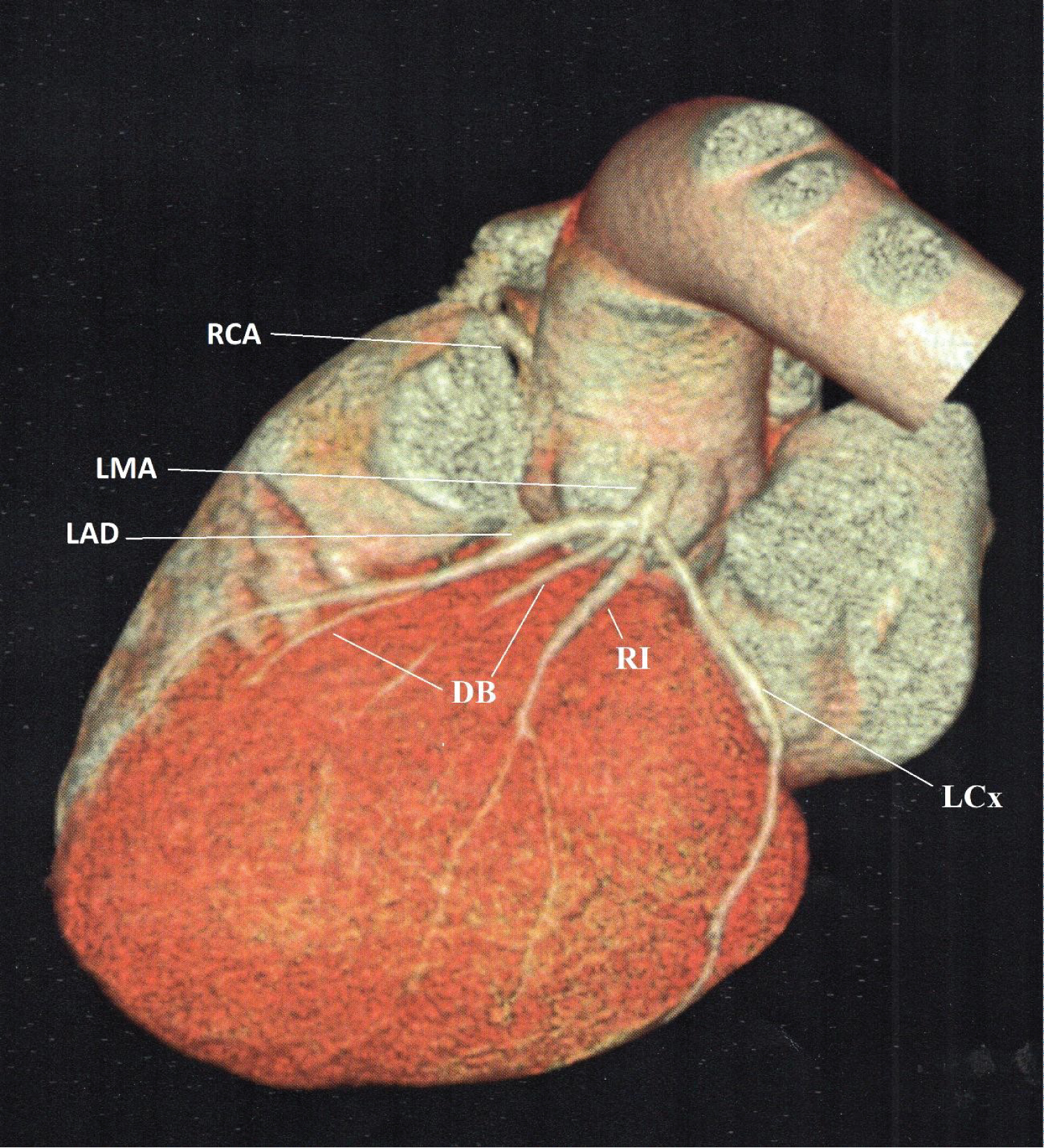
Figure 2: Cardiac computed tomography angiography. LMA, without lesions; LAD artery, without atherosclerotic lesions, with a deep intramyocardial course up to 16.6 mm (MB); Fist DB, with intramyocardial course (MB); LCx, first diagonal without lesions with intramyocardial course in distal third (MB). RI, of moderate size with two rams intramyocardial course (MB) in middle third. RCA, dominant without lesions.
LMA: Indicates Left Main Coronary Artery; LAD: Left Anterior Descending; DB: Diagonal Branch; LCx, left circumflex; RI: Ramus Intermedius; RCA: Right Coronary Artery. MB: Myocardial Bridge.
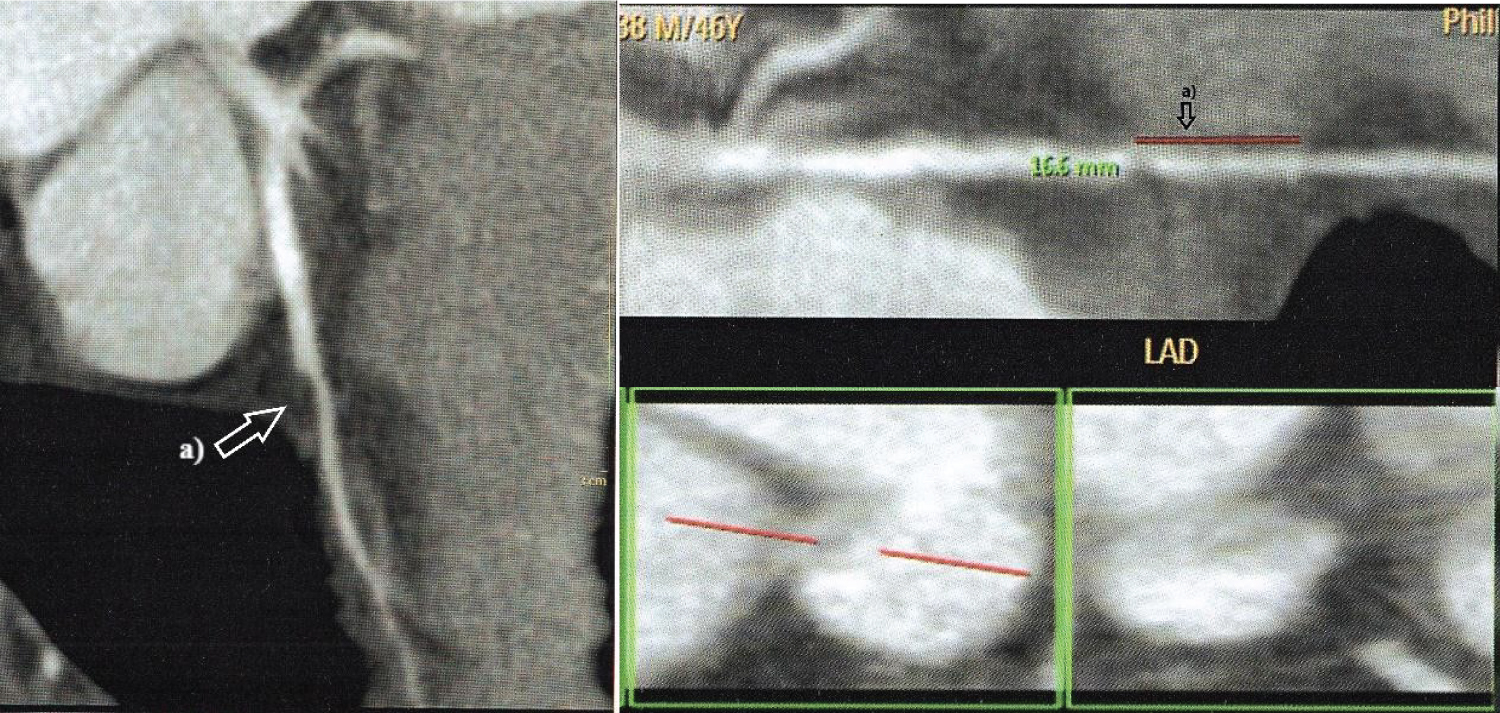
Figure 3: Additional analysis of the LAD MB in Figure 2 with CTTA. a) Cross-sectional view of intramyocardial course in LAD and View of an intramyocardial course in LAD (16.6 mm); Longitudinal view of intramyocardial course in LAD.
LAD: Left anterior descending; MB: Myocardial bridge; CCTA: Cardiac computed tomography angiography.
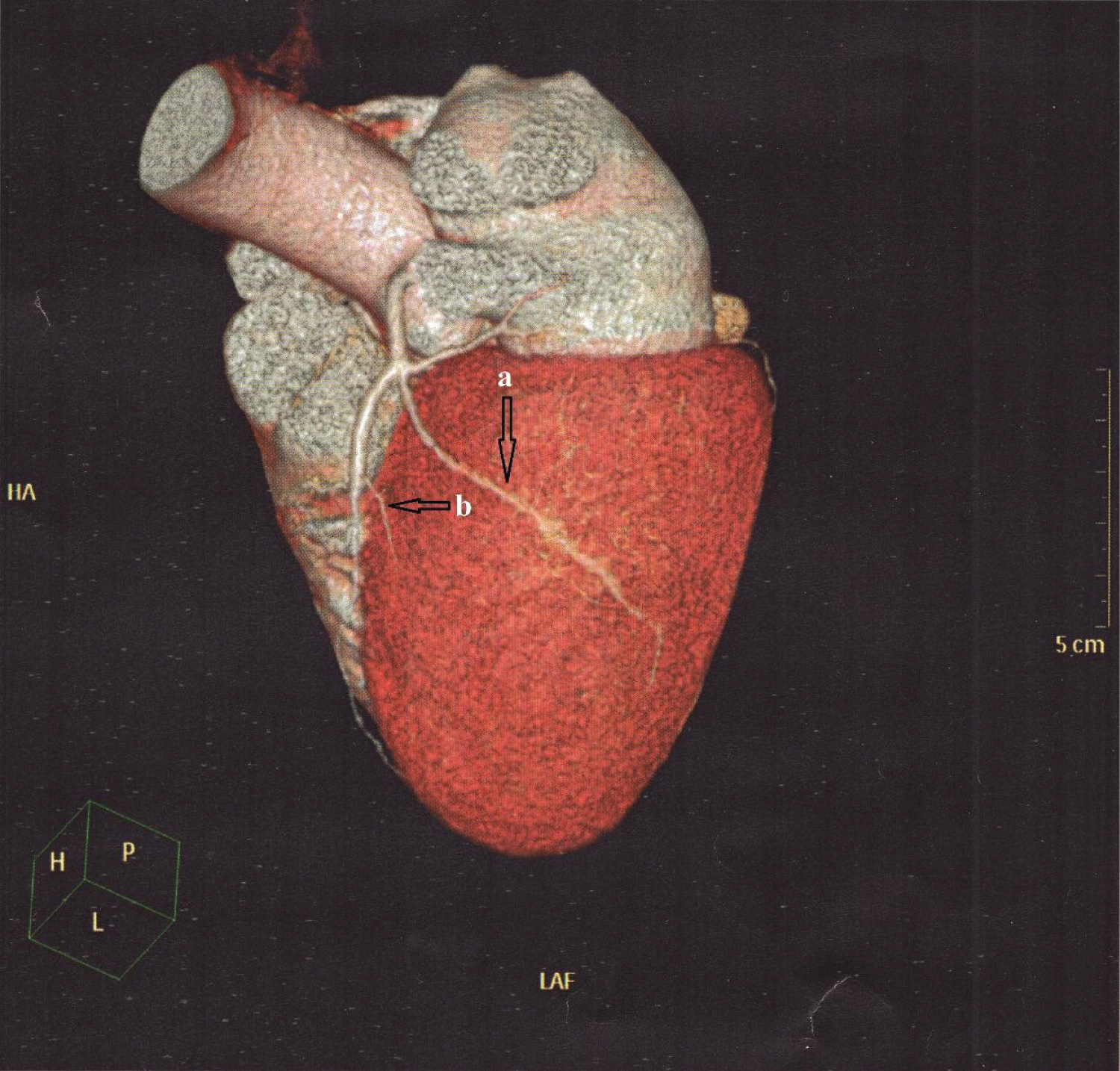
Figure 4: Cardiac multislice angiotomography. Coronary artery calcium score was 0. Left anterior descending artery without atherosclerotic lesions. (A) Showed in Ramus intermedius artery of moderate size with a deep intramyocardial course (MB); (B) The first diagonal artery without atherosclerotic lesions with intramyocardial course in distal third (MB). Circumflex artery, without lesions Right coronary artery dominant without lesions.
MB: Myocardial Bridge.
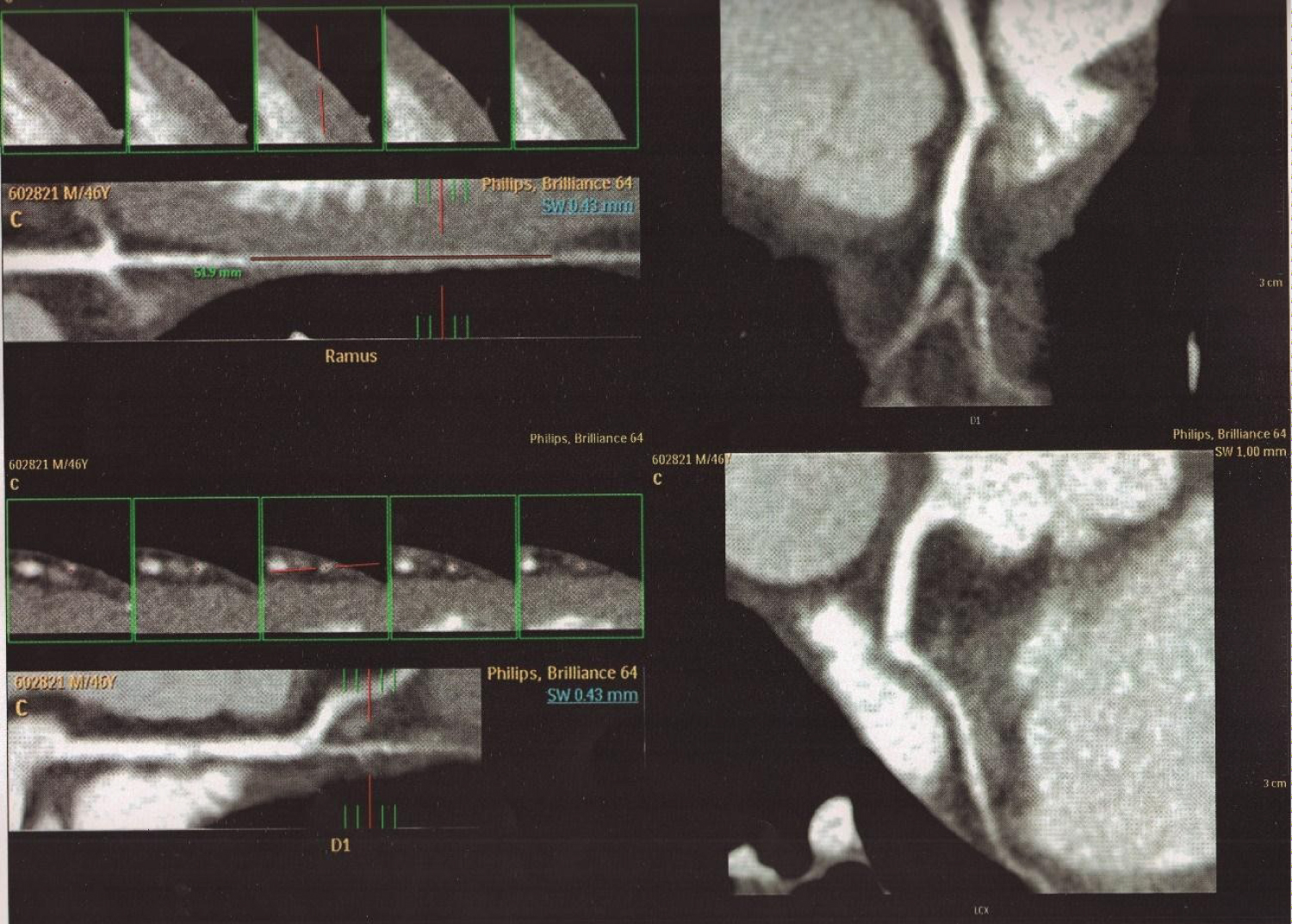
Figure 5: Additional analysis of the myocardial bridge in the ramus intermedius artery and first diagonal artery showed in Figure 4 with CTTA. Cross-sectional view in an extended intramyocardial course (MB) in RI artery (51.9 mm); and in the first diagonal artery.
CCTA: Cardiac Computed Tomography Angiography; MB: Myocardial Bridge; RI: Ramus Intermedius
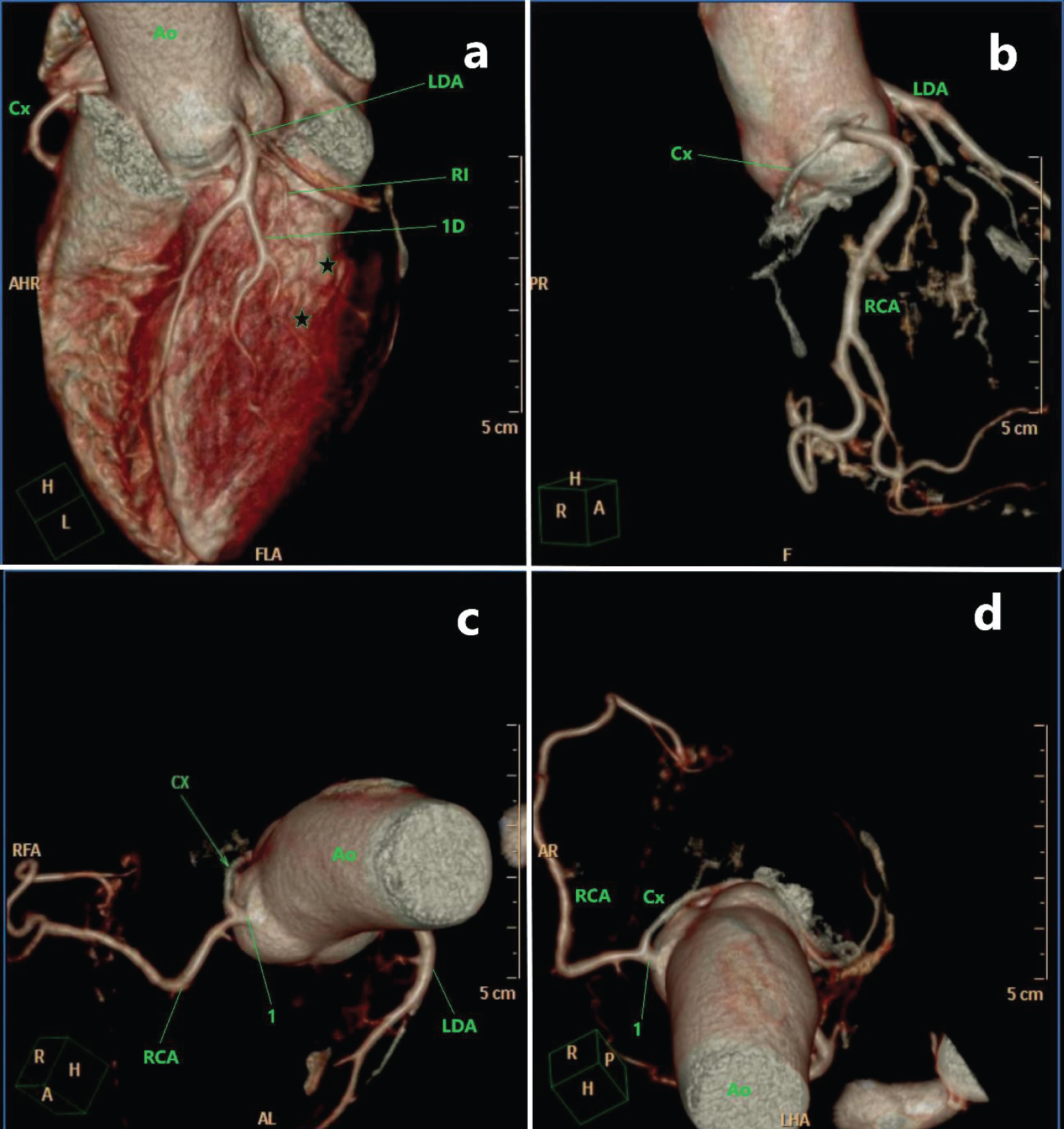
Figure 6: Coronary computed tomography angiography. Calcium score was 0. Showed presence of ectopic left circumflex coronary artery. The presence of Myocardial Bridges (MB) in ramus intermedius artery, and MB in the first diagonal branch artery (asterisk). The presence of ectopic left circumflex coronary artery (Cx in green) arising from the proximal part of the right coronary artery (RCA) and single Right Coronary Ostium (RCO).
MB: Myocardial Bridge
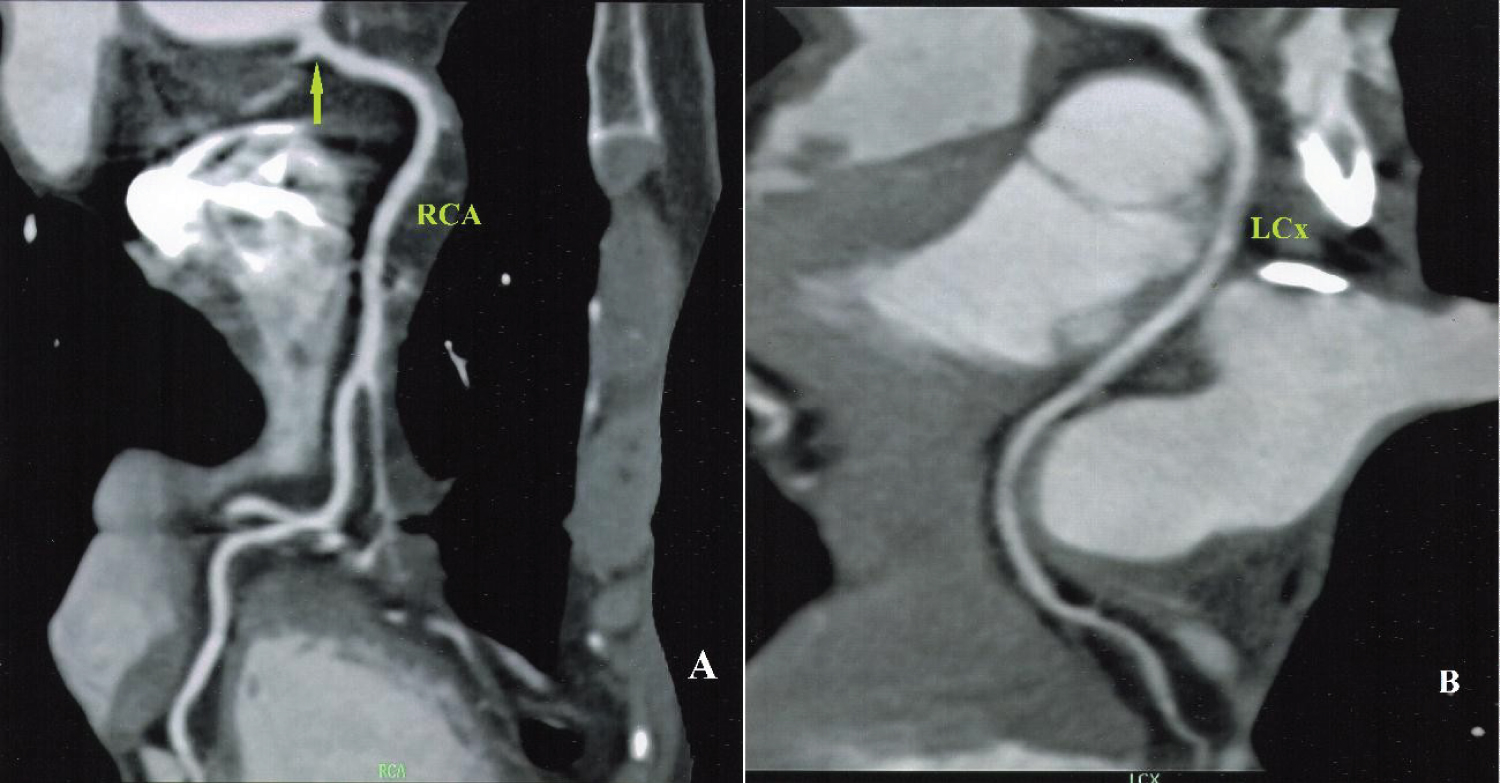
Figure 7: Analysis of the ectopic Cx showed in the Figure 6 with CTTA. (A) Longitudinal view shows the course of anomalous aortic origin of a Cx arising from the inappropriate sinus (right coronary sinus) (green arrow); (B) Longitudinal view shows the course of Cx goes backward and to the left, circling the aorta from behind, then passing between the posterior aortic wall and the anterior right atrial wall.
LCx: Left Circumflex artery; RCA: Right Coronary Artery; Cx: Circumflex Artery; CCTA: Coronary Computed Tomography Angiography