A previously healthy, 5-year-old boy was visiting the USA from Europe one week ago. He presented to our hospital with 18 hours history of high-grade fever, rash, vomiting, and progressive lethargy. On physical exam, he was obtunded, febrile, tachycardic, tachypneic, hypotensive and with a nonblanchable purpuric rash on the face and extremities. A possibility of Meningococcemia considered. Fluid resuscitation, broad-spectrum antibiotic therapy started after obtaining blood cultures. Vasopressor therapy with norepinephrine initiated and child transferred to pediatric intensive care unit. Over the next 1-2 hours, his purpuric rash became generalized (Figure 1), and his shock worsened. Vasopressor therapy escalated, and fluid resuscitation continued with crystalloids and blood products. He was endotracheally intubated and kept on mechanical ventilator. His laboratory workup revealed leukopenia, thrombocytopenia and abnormal coagulation parameters. Despite aggressive treatment, he progressed to cardiac arrest and the child died within 4 hours of admission. His postmortem cerebrospinal fluid (CSF) gram stain revealed intracellular gram-negative diplococci in neutrophils (Figure 2 with arrows). His blood culture and CSF culture grew Neisseria meningitides.
Neisseria meningitides, also known as Meningococcus, is a potentially life-threatening cause of fulminant sepsis (meningococcemia) [1]. Patients present with high-grade fever, petechial or purpuric rash and rapid progression to purpura fulminans and hypotension [1]. Purpura fulminans characterized by diffuse purpuric rash due to dermal vascular thrombosis because of endothelial dysfunction and coagulation cascade activation [2]. Presence of purpura fulminans is one of the poor prognostic factors [2]. Aggressive fluid resuscitation and early administration of antibiotic with intravenous ceftriaxone is vital for the successful outcome [1].
None.
None.
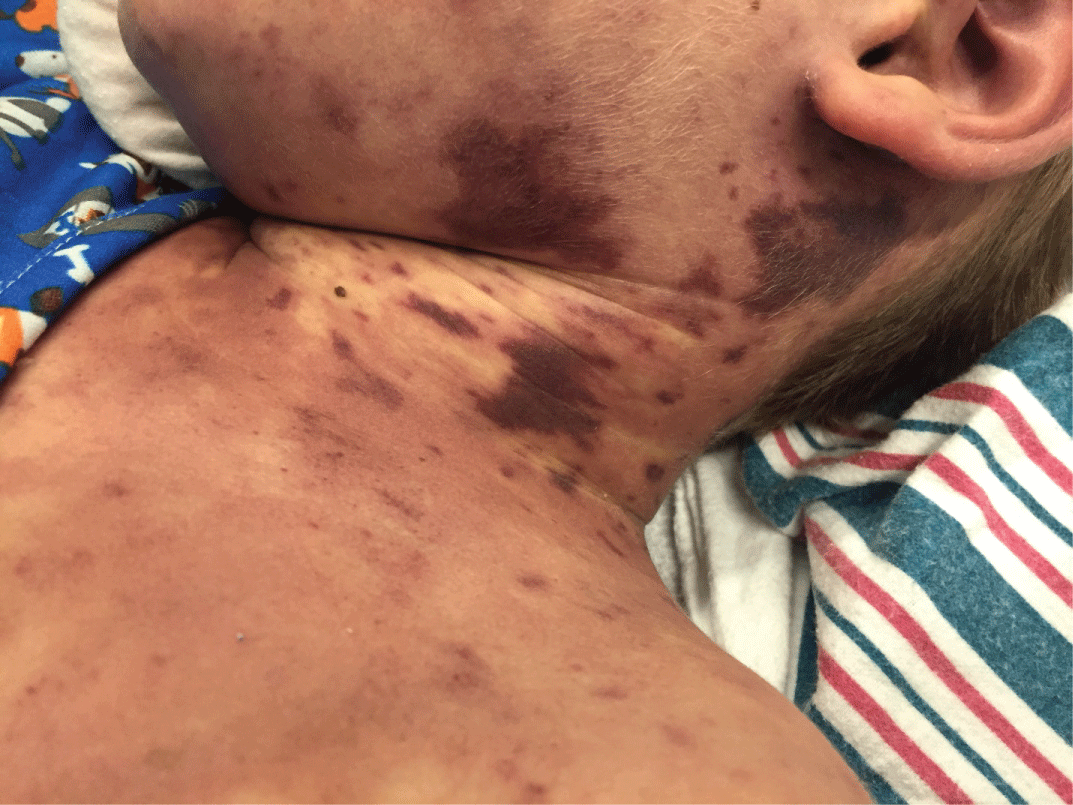
Figure 1: Diffuse erythematous skin with multiple purpuric lesions- Purpura fulminans.
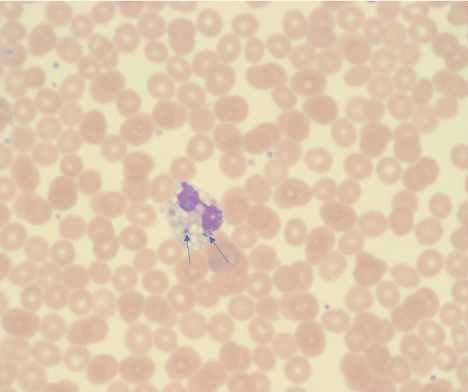
Figure 2: Cerebrospinal fluid gram stained smear showing neutrophil with intracellular gram-negative diplococci (indicated with arrows).