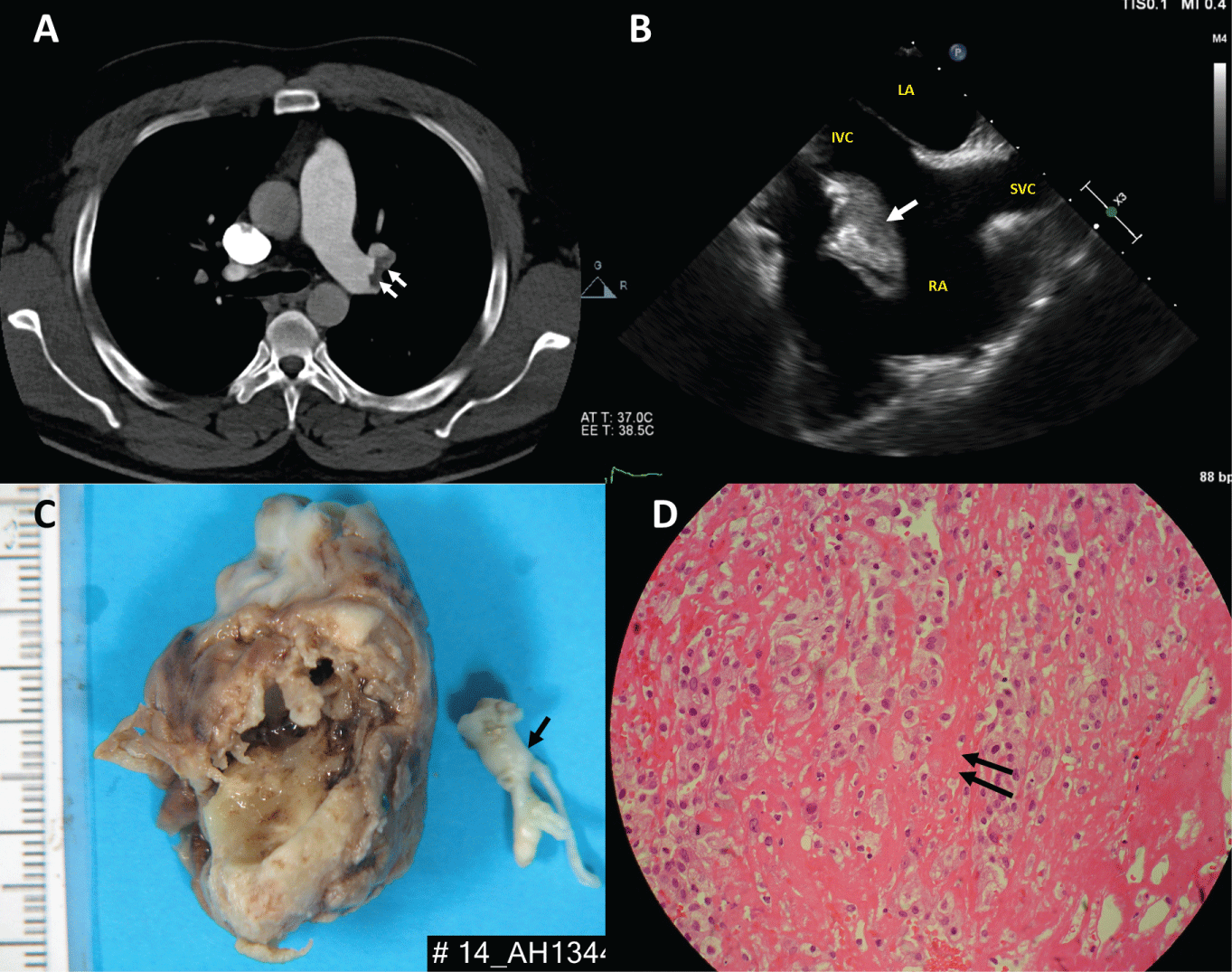
30-year-old man normally fit and healthy presented with collapse and palpitation. He was tachycardic with a heart rate of 120 beats/min and hypoxic with oxygen saturation of 85% on arrival. CT pulmonary angiography confirmed extensive bilateral segmental and sub segmental pulmonary emboli with evidence of right heart strain (Panel A). Laboratory data revealed an elevated international normalized ratio (INR) of 1.4, prolonged partial thrombo plastin time (aPTT) of 49 seconds and a low fibrinogen level of 1.0g/L. Blood cultures were unremarkable. CT abdomen and pelvis showed no evidence of malignancy.
3 months prior to this presentation he had a similar coagulopathy with elevated INR of 2.0, a prolonged aPTT of 73 seconds and a low fibrinogen level of < 0.3g/L which resolved following administration of fresh frozen plasma and cryoprecipitate. Lupus anticoagulant screen and antinuclear antibodies were normal.
Heparin was administered in view of his coagulopathy. Again, his coagulopathy resolved the following day. Trans oesophageal echocardiography confirmed a large right atrial mass measuring 3.9cm x 1.8cm with a stalk attached near the inferior vena cava (IVC) (Panel B, Online video). There was no obstruction to the tricuspid valve. An urgent operation was performed in view of the risk of further pulmonary embolism. On opening the right atrium a large tumour was found (Panel C) It was attached by a stalk to the eustachian valve and was very close to the IVC cannula. There were no other clots or tumour seen in the right atrium or ventricle. The tricuspid valve appeared normal. No myxo matous tumour was identified on H&E stained sections but only abundant partially organised blood clot with degenerate stroma (Panel D). The patient had an uncomplicated recovery and was discharged home on warfarin 6 days after the surgery. Post-surgery echocardiography confirmed no residual mass in the right atrium and he had no further coagulopathy.