Leiomyomas or fibroids are the most common benign tumor of uterus and it often increases in size during pregnancy. Its incidence in pregnancy is approximately 1.5-2% and is associated with increased risk of complication during pregnancy including abortions, preterm labor, red degeneration, malpresentations, increased cesarean section rates, postpartum hemorrhage. We hereby, discuss a case of large multi-lobed uterine fibroid complicating the second trimester of pregnancy. Our patient presented with a large leiomyoma of approximately 28 × 30 cm size at 28 weeks of gestation with acute red degeneration of fibroid with intra-capsular and intra-peritoneal bleed. Life saving subtotal hysterectomy was done and around 1.5-2 liters of blood was drained out from the abdominal cavity. The total weight of uterus with fibroid was around 15 kg and benign leiomyoma was confirmed on histopathological examination.
Fibroids are one of the most common benign smooth muscle tumors of the uterus [1,2], with an overall incidence of 40-60% in 35-years-old female and 70-80% by age 50 years [3]. They have both smooth muscle and fibroblast components, with significant amount of fibrous extracellular matrix, which all are responsible for the pathogenetic process [1]. The exact etiology of uterine fibroids is still unclear with many theories of its origin [3]. Various factors like genetic predisposition, steroid hormones, environmental factors, etc. play an important role in the fibrotic processes and angiogenesis, ultimately leading to formation and growth of uterine fibroids [4]. Hence, the origin of leiomyomas can be multifactorial [5]. Furthermore, the fibroids are enormously heterogeneous in their pathophysiology, location, size and their clinical presentation [1]. During antenatal period the diagnosis of fibroids becomes further challenging as the ultrasound's ability to detect fibroids in pregnancy is very low (1.4%-2.7%), mainly due to its decreased efficiency to differentiate between fibroids and normal thickening of the myometrium. Hence, the reported prevalence of leiomyomas during pregnancy is underestimated and under-reported. Also, the exact association between uterine leiomyomas and poor pregnancy outcome is still not known [3]. Various studies have revealed that 60-70% of fibroids in antenatal women show no change in volume. Around 22-32% show increase in volume, especially in first trimester, with very minimal change in volume in second and third trimesters [6].
Most fibroids usually remain asymptomatic in antenatal period, but in some patients, it may present with acute abdominal pain which is most common complication of fibroid during pregnancy and is due to red degeneration or torsion or impaction of pedunculated fibroid [3]. Degeneration of fibroids is a common process and it usually occurs when the fibroids grows enormously in size, resulting in decreased blood, oxygen and nutrient supply. After hyaline degeneration, red degeneration is commonly seen during pregnancy [7]. It is hemorrhagic infarction of uterine leiomyoma, and complicates around 8% of tumors during pregnancy, though the prevalence is only 3% of all uterine leiomyomas [7,8]. Red degeneration is commonly seen in women with big fibroids of size more than 5 cm and usually occurs in late second or early third trimester of pregnancy. The pain mainly occurs due to vessel kinking leading to tissue hypoxia, ischemia and necrosis with release of huge amounts of prostaglandins [3]. Here we present a rare case of second trimester pregnancy with huge fibroid with red degeneration with massive intracapsular and intraperitoneal bleed in a patient with situs inversus and dextrocardia.
A 34-years-old primigravida patient came to the Obstetrics and Gynecology Out Patient Department of a rural tertiary care center of Northern India with chief complaints of amenorrhea since, seven months, abdominal distension with pain in abdomen since, one month and breathlessness since ten to fifteen days. She was receiving her previous antenatal checkup at some private hospital where her first trimester ultrasound (USG) revealed a fetus of 12 weeks with a large uterine mass of 12 cm. Her repeat USG for the complaints of pain in abdomen in second trimester revealed uterus of 21 weeks gestation with a rapidly enlarging uterine mass of 20 cm, highly vascular, so a suspicion of Gestational trophoblastic neoplasia was made. She was advised Magnetic Resonance Imaging (MRI) followed by USG guided Fine Needle Aspiration Cytology (FNAC) of the mass which revealed typical whorled pattern suggestive of fibroid uterus. She was advised admission at that time, but patient refused admission. She then reported to our Institute with abdominal pain and increased breathlessness since 10-15 days which was increasing in severity and intensity. Patient was admitted under high risk unit. On general examination patient appeared sick, tachyonic anemic (pallor2+) with blood pressure 110/70 mmHg, pulse rate was 120/min. Patient was febrile with 101 degree Fahrenheit temperature. Her Cardiovascular and Respiratory system examination revealed dextrocardia and decreased air entry on left side of chest. On per abdominal examination, abdomen was tense, tender to touch and distended up to xiphisternum. Uterus and fetal parts could not be appreciated. Fetal heart sound could not be heard with stethoscope. A repeat USG abdomen and chest was advised which showed a huge fibroid of 28 × 30 cm with intracapsular bleed of around half to one liter. There was single live intrauterine fetus of 27 weeks gestation. In addition to this the patient had situs inversus with dextrocardia. So, the provisional diagnosis of Primigravida with 27 weeks gestation with huge fibroid uterus with red degeneration with intra capsular bleed with situs inversus and dextrocardia was made. Patient was put on intravenous antibiotics along with antipyretics and analgesics. All the investigations including complete blood count, Liver function fest, Renal function test, were sent and were within normal limits with hemoglobin 9.2 g/dl and total leukocyte count of 16,000/cumm. Blood was sent for cross matching. Patient and her relatives were counseled about the high risk to the patient and the fetus. On second day the patient started deteriorating with blood pressure falling to less than 100/60 mmHg, tachycardia (pulse rate more than 140 beats per minute), pallor increased and the abdomen became very tense and tender to touch, so the decision to do urgent exploratory laparotomy was made, explaining all high risk to the relatives along with the consent to do the hysterectomy if needed. Intraoperative findings included hemo-peritoneum (1-1.5 litre) with uterus of 28 weeks size with large multilobed fibroid seen arising from the anterior surface of uterus with larger lobe measuring 28 × 30 cm and the other lobe was degenerated with intracapsular bleed of around 2-3 litres and size 15 × 20 cm (Figure 1). Both the lobes were receiving rich vascular supply from the retroperitoneum, mesentery of the gut with dense adhesions. All the adhesions and supply were carefully clamped and cut to free the fibroid. An attempt to save the uterus was made, but due to the deteriorating maternal condition (on operative table BP 60/40 mmHg, PR 140/min) first hysterotomy was done to remove the fetus and save the uterus, but since the patient continued to bleed profusely so the decision to do hysterectomy was made and subtotal hysterectomy was done as life saving procedure (Figure 2). Bilateral abdominal drain was left in situ and abdomen closed after achieving complete hemostasis. Intraoperative six transfusions were given including three units Packed Red blood cells (PRBC) and three units of Fresh Frozen Plasma (FFP). In Immediate postoperative period patient was given two units of PRBC, two units platelets and four units FFP. Patient started recovering and was extubated on second day of surgery. Since the post-operative hemoglobin was less (5.5 g/dl), three more units of whole blood were transfused. Her histopathological report revealed bilobed fibroid uterus with hemorrhagic infarction and cystic degeneration (Figure 3).
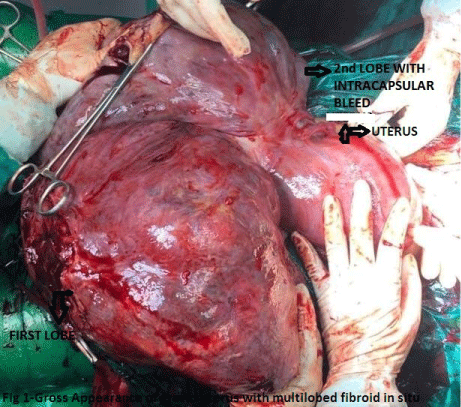 Figure 1: Gross appearance of gravid uterus with multilobed fibroid in situ.
View Figure 1
Figure 1: Gross appearance of gravid uterus with multilobed fibroid in situ.
View Figure 1
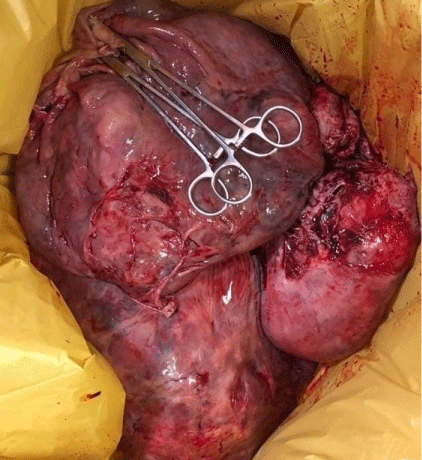 Figure 2: Uterus with multi-lobed fibroid after removal.
View Figure 2
Figure 2: Uterus with multi-lobed fibroid after removal.
View Figure 2
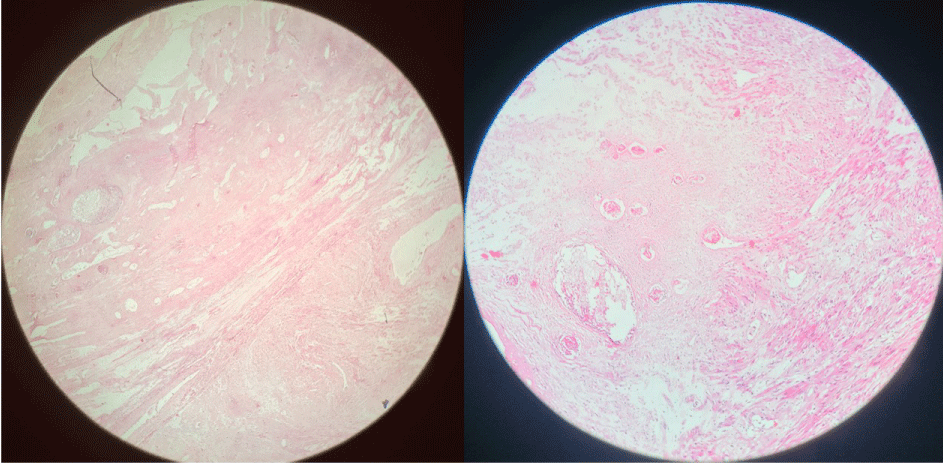 Figure 3: Microscopic appearances showing bundles of smooth muscle fibers with areas of red degeneration.
View Figure 3
Figure 3: Microscopic appearances showing bundles of smooth muscle fibers with areas of red degeneration.
View Figure 3
Her stitches were removed on post-operative day nine and ten alternatively. So, after a total of 17 transfusions the patient recovered from blood loss and was discharged on postoperative day 11 under satisfactory condition and was advised to come for regular follow up.
Uterine Leiomyoma are one of the most common benign tumours evidenced in pregnancy with a reported incidence of 0.1 to 10.7% of all pregnancies and the incidence further increases with the advancing age of mother [9]. They rarely show any change in size during pregnancy but can increase in size and volume in first trimester and very rarely in second and third trimester [6] but unlike in this case the fibroid was rapidly growing in second trimester both in size and volume [6]. The exact pathogenesis of these smooth muscle tumours is not clear, but the two main ovarian steroidal hormones; oestradiol and progesterone play a significant role in its growth. The growth promoting effects of these hormones is mainly through local production of specific growth factors which causes augmentation of mitotic rate [10]. Another theory that explains the pathogenesis is response to injury, especially during menstrual cycle in which ischemic damage leads to release of various vasoconstrictive substances, which causes smooth muscle cells of the myometrium to react and synthesis extracellular fibrous matrix [11]. Furthermore, after vascular injury there is over expression of basic fibroblast growth factors in leiomyomas, resulting in their growth [12,13]. Fibroids during pregnancy may become complicated due to degenerations resulting in abdominal pain which may present as mild or acute abdomen [14]. They can cause complications in ante-, intra- and postpartum periods of pregnancy which include spontaneous abortions, preterm labour, premature rupture of membranes, abruption placenta, placenta previa/accrete, labour dystocia, red degeneration, malpresentation, intrauterine growth restriction, feto-pelvic disproportion, retention of placenta, postpartum haemorrhage, etc [15-17]. Around 10%-40% of all prepartum complications during pregnancy with fibroid are due to the presence of fibroid itself [18].
Patients with uterine fibroid during pregnancy usually present with severe abdominal pain. In our case also the patient presented with acute abdominal pain with distention. A variety of factors such as epigenetic or genetic mechanism, disorganization of extracellular matrix, growth factors have shown interaction with pathogenesis of growing fibroid [15]. As far as management is considered, conservative with anti-inflammatory therapy is considered as gold standard, and the surgery is generally avoided during pregnancy because of the risks of hysterectomy secondary to severe haemorrhage, pregnancy injury, and pregnancy loss [3]. The main conditions that induce inevitably the surgical procedure are the torsion of pedunculated fibroids or rare cases of necrosis with resultant inflammatory peritoneal reaction, and if symptoms persist for more than 72 hours of drug therapy. Therefore, the diagnosis needs a particular attention for the appropriate management choice [3,15].
Surgical removal of fibroids in pregnancy can be performed by laparotomy or laparoscopy technique taking into account the volume and location of nodules. Another treatment modality namely uterine artery embolization (bilateral) has been performed by interventional radiologists to control postpartum haemorrhage and alternative procedure for treating large symptomatic fibroids in women who are not pregnant and not desirous of future fertility [3].
A similar case report was published by Yordanov, et al. which reported that a 34-year-old woman, primipara at 14 weeks presented with the complaints of acute abdominal pain, on ultrasound it was found that she had a twisted sub serous pedunculated myoma with diameter of 20 cm. An urgent median laparotomy with myomectomy was performed without any complications. On the 38th week of pregnancy the patient delivered a healthy, 3400 g, full-term baby by caesarean section [15].
Another case was reported by Panchal, et al. in 2012 where a 35-year-old, booked multipara with previous caesarean with pre-eclampsia with fibroid uterus on regular treatment, was taken up at term for elective caesarean section and delivered a live baby boy with good APGAR score [16]. Intraoperatively the capsule of fibroid got opened during uterine incision leading to uncontrolled bleeding so total obstetric hysterectomy was done as a lifesaving procedure [19]. In our case the patient presented acutely with breathlessness and acute abdomen in her late second trimester, so we failed to save her pregnancy and uterus, but we managed to save her life with massive blood transfusions. Hence, pregnancy with fibroid is considered as high-risk condition with increased maternal and neonatal complications. In future we can think of doing uterine artery embolization immediately after extraction of baby to control bleeding and to avoid the need for hysterectomy.