This is a case study of women with Invasive Cervical Cancer (ICC) and her course of treatment, showing the critical need for prevention through aggressive screening and vaccination programs. Even though cost of treatment was a barrier, she completed her radiation therapy and felt better. Then she experienced an aggressive recurrence associated with bilateral lungs metastasis thereafter and the only option was to refer her for palliative chemotherapy. This report highlights the difficulty faced by patients in getting radiation treatment in Low and Middle-Income Countries (LMIC) like Cameroon. It also supports the view that cervical cancer prevention via vaccination and with routine screening is crucial in addressing the growing burden of cervical cancer in LMICs especially given the cost of access to treatment and dearth of radiation treatment infrastructure.
Invasive cervical cancer, Cervical cancer screening, Cost, Radiation treatment and Palliative chemotherapy
Invasive Cervical Cancer (ICC) has been reported as the second leading cause of cancer morbidity and mortality among women in Cameroon by the International Agency for Research on Cancer (IARC) GLOBOCAN 2012 (17.5 deaths per 100,000 per year and 30.0 cases per 100,000 per year versus 17.6 deaths per 100,000 and 35.3 cases per 100,000 for breast cancer) [1], but this may be an underestimation due to the lack of specific country-level data on cervical cancer screening and the absence of a national cancer registry [2-4]. Two studies (sample size 540 and 4,813) report Visual Inspection with Acetic Acid (VIA) positive rates for Cameroon women of 12.9 and 21.7 respectively [5,6].
The Cameroon Baptist Convention Health Services (CBCHS), a faith-based organization with a network of 81 health facilities in 6 of Cameroon's 10 regions [7], has a nurse-led Women's Health Program (WHP) that has used Digital Cervicography (DC) to screen over 56,000 women for cervical cancer since 2007. With DC, WHP providers use digital cameras and Samsung Galaxy S4 Cell Phones to project highly magnified (up to 30×) real-time images of the cervix onto a commercial 13-inch Television (TV) screen that can be seen by both the woman and the provider [8]. TVs give a much clearer image than projecting onto a computer screen, are inexpensive, and require fewer connecting devices [8]. The cervicographs taken are linked to each woman's medical record in the WHP database. Cervical abnormalities visible on the TV are used to describe the findings to each woman screened, thus empowering her to participate in treatment decisions. This appears to be important in reducing or preventing risk for treatment refusal. Cervicographs are archived for follow-up comparison, staff training, consultation, and quality improvement. WHP nurses offer same-day cryotherapy, cold coagulation, punch biopsy, referral for Loop Electrosurgical Excision Procedure (LEEP), or other indicated interventions [8].
WHP runs the largest cervical cancer prevention program in Cameroon [9]. Between 2007 and 2014, the program screened 44,979 women for cervical cancer using the VIA-DC technique and the overall positive rate was 9.0% [9]. From 2007 through 2013, the prevalence of ICC in WHP was 613 per 100,000 women screened. This is higher than the prevalence of 80.7 per 100,000 reported by GLOBOCAN 2012 for Cameroon [1]. The reason could be attributed to selection bias because a good number of women with symptoms suspicious of ICC self-referred themselves for screening. The majority of these ICC cases (61.1%) were in women over age 50 [9].
BT, 51-years-old G5P4014 housewife was first seen in early December 2011 at Etoug-Ebe Baptist Hospital Yaoundé (EBHY) with a history of persistent watery vaginal discharge and postcoital bleeding of 2 months duration. Upon speculum examination, BT was found with a broad exophylic cauliflower-like lesion with contact bleeding. An exocervical punch biopsy was done at 12 and 3 o'clock positions of the cervix. Blood loss was approximately 20 cc and homeostasis was achieved by pressure and application of Monsel's solution. The specimen was sent to histopathology at the Yaoundé Gynaeco-Obstetric and Pediatric Hospital (YGOPH), a large referral hospital in Cameroon's capital. Three weeks later the histology report confirmed an invasive squamous cell cervical cancer. The cancer was staged at IIB with left parametrial extension. The staging was done by rectovaginal examination alone. BT was referred for radiation treatment at the Douala General Hospital at the economic capital of Cameroon. This is the lone functional radiation oncology center in Cameroon.
It was quite a hardship for this impoverished family to raise enough money for radiation treatment in addition to a six-weeks stay in Douala; which is one of the most expensive cities in Cameroon. Even though the cost of radiation treatment has been subsidized in Cameroon by the government, it is still very expensive for even an average Cameroonian family creating a barrier to treatment. To complete a course of radiotherapy plus concurrent chemotherapy, she had to spend 270,000 Frs ($540) excluding transport fare, lodging and feeding for herself and her caregiver.
It took 4 months for her to raise enough funds to afford the treatment. Being the women's leader in her local church, the church made a series of free-will offerings to support her treatment. She started her radiotherapy with concurrent chemotherapy at the Douala General Hospital in April 2012 which cost her 270,000 Frs ($540) including 180,000 Frs ($360) for radiotherapy and 90,000 Frs ($180) for concurrent chemotherapy. The treatment appeared quite successful and she felt much better thereafter. The offensive vaginal discharge and other symptoms ceased and life returned to normal for her again.
She returned to EBHY in November 2012 for follow up. Upon speculum examination, her cervix appeared clean and healthy. Both VIA and Visual Inspection with Lugol's Iodine (VILI) were negative.
In April 2014, BT returned to the clinic at EBHY with a history of one episode of postcoital bleeding. Speculum exam revealed a small ectropion. Both VIA and VILI on DC were negative and she was reassured.
In July 2014, she returned to the clinic again complaining of persistent postcoital bleeding. Speculum exam showed a moderate to severe bleeding ectropion. VIA on DC was uncertain with an ill-defined acetowhitening at the lower lip of the cervix. An exocervical punch biopsy was done at the 6, 12, 9, and 1 o'clock of the ectropion. The specimen was sent again to the YGOPH for histopathology and revealed ICC. The patient was referred back to the radiation oncology unit at Douala General Hospital for proper management. At the hospital in Douala, it was realized that she had been given an appointment for brachytherapy for May 2012 which she had never attended. She intimated that she was never informed of the appointment even though it was written in her consultation card. She saw it but did not understand it.
The patient then received the brachytherapy in December 2014, which cost 160,000 Frs ($320). The treatment was so tedious that she described the experience as "gone into hell and came out". For 5 days and 5 nights (120 hours), she was put in a room alone in lithotomic position on a gynecological coach. She was not permitted to move. That is, she was not supposed to get up, turn to the left nor right, move her hands or legs, nor any part of her body. During this period, she did not eat food but was able to drink some fluids with assistance. She had to spend most of the time alone in the room with no one to neither talk to nor encourage her. It was more than a nightmare for her as she went through this procedure. She felt better after the treatment, with symptoms subsiding and she thought it was finally cured.
In December 2015, only a year later, she felt abdominal heaviness and discomfort. She did a pelvic ultrasonography which revealed a hydrometra of 95 cc. She returned to Douala to show the ultrasound report to her Radiation Oncologist, who aspirated the hydrometra and she felt better again.
In February 2016, she returned to the clinic at EBHY again with history of profuse malodorous vaginal discharge. On speculum examination, the cervix was found with fungations and necrosis and with profuse dark-brown malodorous discharge. A report was made and sent to the radiation oncology unit of Douala General Hospital for advice. The advice was that all that could be done now is palliative chemotherapy.
While she was preparing funds to commence the palliative chemotherapy, she returned to clinic at EBHY in July 2016 to complain of severe persistent non-productive cough. She was asked to do a chest X-ray which she did and the report showed bilateral lung metastasis. She therefore had to start her palliative chemotherapy urgently at the Yaoundé General Hospital. She was placed on Azantac 50 mg, Atarax 25 mg, Solupred 20 mg, Plitican 50 mg injection, Zophren 8 mg, Taxol 150 mg and Carboplatinne 450 mg. Each session of palliative chemotherapy cost 150,000 Frs ($300) to be taken 3 weeks apart. The total length of treatment was to be determined by her response to the treatment.
BT and her family became so discouraged that despite all the treatments, expenses and sacrifice they have made, the disease has continued to progress (Figure 1).
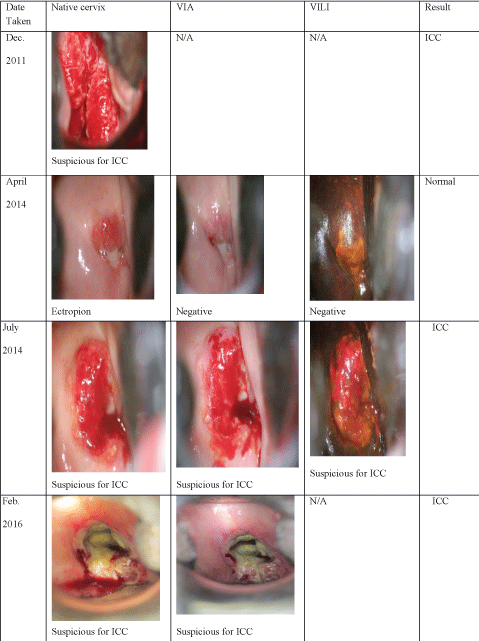 Figure 1: Table of cervical photos of the woman. (N/A: Not Available). N.B: The photos of November 2012 in which she was perfectly negative for VIA and VILI are not available. View Figure 1
Figure 1: Table of cervical photos of the woman. (N/A: Not Available). N.B: The photos of November 2012 in which she was perfectly negative for VIA and VILI are not available. View Figure 1
In this case, the disease has advanced despite all available treatment options creating distress, financial difficulties and apprehension in the family. This situation could have probably been prevented if this woman had had cervical cancer screening some five to ten years prior to 2011. It is often said that prevention is better than cure because it is cheaper, easier and less invasive to prevent a disease than to attempt curing it. Among all cancers, cancer of the cervix is one of those cancers that can be prevented almost 100% [10]. It is therefore heart-breaking to see a woman suffering and dying from a disease which is highly preventable. Even though vaccines are now available against the disease, screening and treatment of precancerous lesions remains the pillar of cervical cancer prevention in developing countries. WHO recommends screening to begin at age of 30 [8] but the Cameroon National Committee for the fight against cancer recommends beginning at age 25. Screening a woman just once between 30 and 49 years reduces substantially her risk of developing the disease [10,11].
Could this patient have done better with a different treatment option? The only other option could have been concomitant radiation and radical hysterectomy. In a randomized study of radical hysterectomy versus radiation for the treatment of stage 1b to 2a cervical cancer, Landoni and colleagues followed up 469 women between September 1986 and December 1991. They found that 5-year overall and disease-free survival were identical in the surgery and radiation groups (83% and 74%, respectively, for both groups). Eighty-six women developed recurrent disease: 42 (25%) in the surgery group and 44 (26%) in the radiation group. They also discovered that 48 (28%) surgery-group patients had severe morbidity compared with 19 (12%) radiation-group patients (p = 0.0004) [12]. They noted that the combination of surgery and radiation had the worst morbidity, especially urological complications. Based on this report, we cannot say for sure that this patient could have done better if she had a different treatment option. WHO pointed out that 5 years survival for stage 1b to 2a cancer is 85% to 75% and 65% for stage 2b [13]. It is disheartening for a woman to spend huge family resources and goes through all the ordeals of treatment just for a less than 5-year survival or symptom free period. This woman was symptom free only for two years and then became symptomatic in increasing severity.
According to WHO (2014) factors influencing cervical cancer prognosis or five-year survival rates for women after completing the best treatment are 1) The clinical stage of the disease when first diagnosed; 2) Access to treatment; 3) Involvement of the lymph nodes (presence of cancer); 4) Presence of other chronic or acute diseases/conditions; 5) General health and nutritional status, including presence of anemia; 5) Degree of immunosuppression (e.g. HIV status) [8]. Except that BT had a little delay to commencement of her treatment, none of these factors were present in her. Therefore, one would have expected her to experience a longer disease-free period.
One other thing we noted in this case is ill-defined acetowhitening after radiotherapy. When the woman first reported postcoital bleeding, probably the cancer was already re-established but it took the form of an ectropion. It was only months later that an ill-defined AWE could be visible on a small portion of the cervix. We did not find any study that has reported characteristics of AWE postradiation treatment. It is recommended that studies be done to evaluate the performance of acetic acid (VIA) on postradiation patients. This will inform providers as to whether or not VIA is reliable in following up with these patients.
The woman did not receive her brachytherapy on schedule. She had this treatment two and a half years later. Maybe the treatment outcome would have been better if she received this procedure earlier. Even though it was written on her consultation card, she did not understand the meaning. The hospital staff probably assumed that she was going to read and understand the appointment. Such assumptions need to be avoided with proper discharge education. It is always advisable for the health care providers to explain the patient's appointments after writing it in their consultation cards. This also highlights the need for increased tracking and follow-up of patients following treatment. The use of mobile health technologies could be beneficial in this regard building on our work with using mobile phones to take pictures for cervical cancer diagnosis/screening.
In Cameroon, people are less likely to seek medical care in the absence of symptoms. This creates a barrier for follow up as patients have the tendency to return to their care providers only after symptoms have resurfaced or become unbearable.
Finally, cost is a major barrier to treatment in Cameroon. This woman and her family and church actually tried to raise money for her treatment. In WHP, many women have been diagnosed with ICC in rural areas who were not able to afford transport fare to Douala let alone the cost of treatment and lodging in the expensive Douala city. Such women had to suffer in pain in their homes while awaiting the worst. In some cases, their family members even abandon them because of the strong odor secondary to the disease. Unlike in developed countries where health insurance systems are well established, in Cameroon patients are expected to pay for their care upfront before receiving treatment. This is also a major setback for the country's health system. It is interesting that the church can play a role in supporting the treatment of their member with chronic disease. It may be good to evaluate the role of different religious groups in assisting their members to access treatment.
Cervical cancer remains a major threat to women's lives, especially in developing countries. Prevention is the best way to tackle the disease since treatment is too expensive and tedious. Even with effective treatment, 5-year free survival appears low. Fortunately, the disease is one of the most preventable cancers worldwide and with vaccination and routine screening; cancer of the cervix can become eradicated in the ensuing decades with strong government policies on primary and secondary prevention. This will need a collaborative effort of the women, health care providers, families and the community at large.
Many thanks to Dr. Teri Aronowitz of the College of Nursing and Health Sciences, University of Massachusetts Boston and Drs. Thomas and Edith Welty of the Cameroon Baptist Convention Health Services who provided editorial contributions to the paper.
The authors declared no potential conflict of interest with regards to authorship and/or publication of this article.