We would like to describe a case of a patient with Paget's disease of bone (PDB) and rheumatoid arthritis (RA) treated with tocilizumab.
PDB is a progressive monostotic or polyostotic metabolic disease characterized by a focal abnormal bone remodeling, with an increased bone resorption and an excessive, disorganized new bone formation [1]. It affects both men and woman, with a slight predominance in men [1], and rarely occurs before middle age; its prevalence increases steadily with age. PDB is the second most frequent metabolic bone disorder after osteoporosis, affecting up to 3% of adults over 55 years of age with a prevalence of 2.5% in England [2]. PDB is often asymptomatic, but patients can present with pain, deformity, or fracture in the affected bone. The etiology of the disease remains controversial, but genetic as well as environmental factors are deemed to be involved [3]. Rheumatoid arthritis has been associated with the disease in 1% of cases [4], but there are not many recent studies or case reports focused on the therapeutic options. The role of IL-6 in PDB pathogenesis has been analyzed in a recent review [5]. Tocilizumab (TCZ) has been approved in many countries for the treatment of moderate to severe RA in non-responding to one or more disease-modifying antirheumatic drugs (DMARDs) patients [6]. Diagnosis of PDB can be easily made with plain radiology of least on skeletal site [3]. Radiological features include initial osteolytic changes followed by sclerotic changes, bone enlargement, and cortical thickening. Measurement of serum total alkaline phosphatase is still the most frequently used and most useful biochemical marker for clinical management of PDB [3].
Paget's disease, Rheumatoid arthritis, Tocilizumab
A 65-year-old Caucasian woman presented to our Outpatients Clinic in July 2003 with a history of increasing leg weakness over the previous year, causing several falls, and intermittent low back pain. The patient described her pain as deep, well defined, persisting at rest, exacerbated both at night and by weight overload. She also complained of episodic paresthesias in the right sciatic nerve distribution, and back pain. She denied fever, night sweats, or weight loss.
After rheumatologic assessment, radiographs were taken, showing changes consistent with Paget's disease: Cortical thickening, enlargement, mixed areas of lucency and sclerosis, coarse trabecular markings and typical lytic and sclerotic changes.
Serum alkaline phosphatase was 1.9 times as high as the upper normal limit while a radionuclide bone scan revealed a markedly increased uptake in the pagetic hip and femur head.
She started a standard treatment with a bisphosphonate. We decided to use alendronate, 5 mg/day. Because the patient preferred the oral administration. Her symptoms improved and serum alkaline phosphatase levels declined to 0.8 equivalents. After two years of continued treatment, the patient achieved PBD remission.
In May 2004, the patient presented with pain and swelling of the hands, wrists and knees. She was anti-CCP positive and typical bone erosions were present on plain radiographs of wrists and hands. Rheumatoid arthritis was diagnosed. She was started on methotrexate (MTX), up to 20 mg/week, and obtained remission after six months. Two years later, the patient suffered from a RA flare, and leflunomide 20 mg/day was begun in place of MTX.
In December 2016, the patient returned to our outpatient clinic after a prolonged remission period. She complained of pain involving the right hip and both wrists and hands. Her DAS28 (ESR) score was 4.89.
Plain radiographs demonstrated progressive pagetic changes of hip and femur head including increased density and cortical and trabecular thickening. A bone scintigraphy showed hot spots in her pelvic bone. A MRI of the hip and femur head showed significant narrowing of the joint, resulting from pagetic changes (Figure 1).
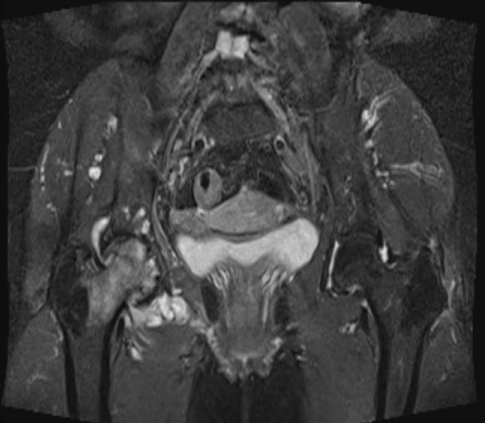 Figure 1: A MRI of the hip and femur head showed significant narrowing of the joint, resulting from pagetic changes. View Figure 1
Figure 1: A MRI of the hip and femur head showed significant narrowing of the joint, resulting from pagetic changes. View Figure 1
The serum alkaline phosphatase level was again 1.9 times as high as the upper limit of the normal range. After the screening tests for HBV/HCV/HIV infection and chest X-rays, we decided to start tocilizumab 162 mg/wk and to continue leflunomide.
Three months later, she did not have pain anymore, DAS28 was 3.4, and serum ALP was normal.
The ideal therapeutic option for PBD should eliminate bone pain, normalize serum total alkaline phosphatase, induce prolonged remission, heal radiographic osteolytic lesions, restore normal lamellar bone, and prevent recurrence and complications. Comparative trials have been published evaluating the relative efficacy of bisphosphonates in the treatment of PDB. These trials typically use extent of suppression of serum total alkaline phosphatase and duration of remission as evidence of superior treatment [7]. Based on recent pathophysiological findings, emerging strategies and therapies are being investigated, including pulse treatment with zoledronic acid [8], use of denosumab, a fully human monoclonal antibody specific for RANK ligands [9], and administration of tocilizumab, an interleukin-6 receptor inhibitor [10]. IL-6 was found to be over expressed in pagetic osteoblasts, and may be involved in both stimulation of osteoclast proliferation and inhibition of osteoblast growth. To date, tocilizumab has indication for treatment of RA only. In a recent study it has been demonstrated that Tocilizumab has a protective effect in an animal model of diabetic nephropathy [11]. Although IL-6 plays a role in causing joint damage in RA through a possible indirect effect on osteoclastogenesis and bone resorption, no clinical trials have been initiated to date in metabolic bone disorders associated with high levels of IL-6.
In this case report, we have shown that administration of low-dose alendronate (5 mg/day), tocilizumab 162 mg/week, and leflunomide (20 mg/day) resulted in effective control of both PBD and RA as early as after three months of therapy. Eighteen months later, the patient displayed low disease activity for RA and no signs and/or symptoms of PDB. To the best of our knowledge, this is the first report of successfully combined therapies for treatment of both PBD and RA. Other studies are required to eventually confirm this therapeutic protocol.
Written informed consent was obtained from our patient for publication of this case report and any accompanying images.