The Bahrain screening program depends primarly on the use of chest x-ray and PPD, while not using both symptom inquiry and Xpert MTB/RIF (XP). The essential keys are to teach and train all physicians in the detection of early symptoms with x-ray findings of active, inactive and diagnose latent pulmonary tuberculosis.
TB screening programme, Confirmatory test of TB, Radiological finding of TB, Sensitivity and specificity of TB screening tests
Setting a nationally standardized TB screening program is essential in the early detection of active pulmonary TB in Bahrain and training all Primary Care Physicians (PCPs) is vital for early detection of active TB cases [1].
TB screening is the process of system identification for apparently healthy people with suspected active TB by using tests, examinations, or other procedures which should be applied to risky groups [2,3].
The best method for TB screening is both symptom inquiry and chest radiograph (CXR), which depends on resource availability, cost and the expected yield [4,5].
The conventional three screening tests of TB are symptoms inquiry questionnaire by asking about the existence of prolonged productive cough, haemoptysis, night fever, night sweating, weight loss, and pleuritic chest pain, besides chest x-ray (CXR) and PPD screening test. The sensitivity of symptoms inquiry and CXR is better than other methods, and it has mirrors for any CXR abnormality' in symptomatic persons [4,6].
The common two confirmatory tests of active TB are sputum-smear microscopy (SSM) and Xpert MTB/RIF (XP). Nonetheless, most clinician's judgment to reach a diagnosis of active TB is from symptoms inquiry questionnaire and chest radiography findings. Any patients who do not respond after a short course of broad-spectrum antibiotics should be re-assessed for hidden TB [7].
The sensitivity and specificity of symptoms inquiry screening questionnaire are 77%, 66% respectively, while it is better in PPD 89%, 80% respectively; though it is higher in CXR reaches to 86%, 89% respectively [8].
Whereas, the sensitivity and specificity of the two confirmatory tests are 61%, 98% in SSM, respectively; though it is higher in XP reaches to 90%, 99% respectively [9]. The sensitivity and specificity analysis depend on many factors; such as the presence of HIV status, the age of the patient, the disease severity, background epidemiology, sputum processing and staining techniques, and diagnostic quality [7,9,10].
There is no ideal universal algorithm exist in primary care; nonetheless, the solution could be a screening test followed by one confirmatory test; or one screening test followed by two sequential confirmatory tests; or two parallel screening test followed by one confirmatory test; or two subsequent screening test followed by one confirmatory test [11].
Active primary pulmonary tuberculosis is a disease of infancy, or young adult when they are not exposed to the Mycobacterium TB bacilli. It may manifest as pneumonic consolidation (homogenous dense opacity or patchy opacification mostly in middle and lower lobes with or without hilar lymphadenopathy called Ghon complex. Other radiological features of active primary TB are either miliary opacities or pleural effusion or pulmonary oedema (Kerely B line) (Figure 1-6) [12,13].
 Figure 1: Chest x-ray showing dense homogenous opacity in right, middle and lower lobe of primary pulmonary TB. View Figure 1
Figure 1: Chest x-ray showing dense homogenous opacity in right, middle and lower lobe of primary pulmonary TB. View Figure 1
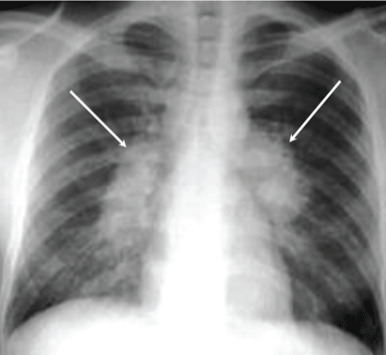 Figure 2: Chest x-ray showing bilateral hilar adenopathy of primary pulmonary TB. View Figure 2
Figure 2: Chest x-ray showing bilateral hilar adenopathy of primary pulmonary TB. View Figure 2
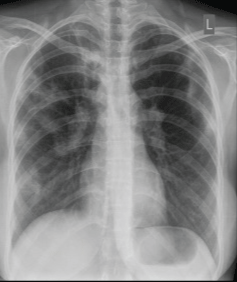 Figure 3: Chest x-ray showing patchy opacification on the upper right and mid-zone lung with fibrotic shadows, both hilar lymphadenopathies. View Figure 3
Figure 3: Chest x-ray showing patchy opacification on the upper right and mid-zone lung with fibrotic shadows, both hilar lymphadenopathies. View Figure 3
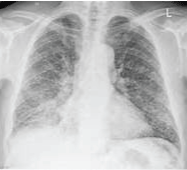 Figure 4: Chest x-ray showing bilateral diffuse miliary opacities of primary pulmonary TB. View Figure 4
Figure 4: Chest x-ray showing bilateral diffuse miliary opacities of primary pulmonary TB. View Figure 4
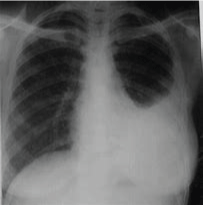 Figure 5: Chest x-ray showing dense opacity pleural effusion in the lower left lung of primary pulmonary TB. View Figure 5
Figure 5: Chest x-ray showing dense opacity pleural effusion in the lower left lung of primary pulmonary TB. View Figure 5
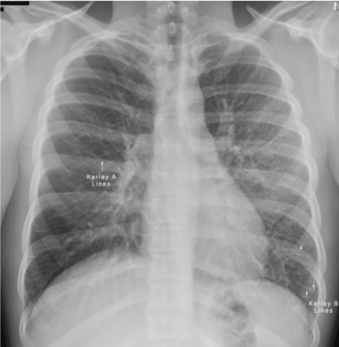 Figure 6: Chest x-ray showing Kerely B line due to interstitial oedema (in children only) of primary pulmonary TB. View Figure 6
Figure 6: Chest x-ray showing Kerely B line due to interstitial oedema (in children only) of primary pulmonary TB. View Figure 6
However, the chest x-ray finding of inactive TB are many such as fibrosis, persistent calcification (Ghon's focus), and a tuberculoma (persistent mass like opacities) [12,13].
The Ghon's focus is a small granulomatous TB lesion presents either in the superior part of the lower lobe or, the inferior part of the upper lobe, while the Ghon's complex is same Ghon's focus plus hilar lymph node adenopathy (Figure 7-9) [12,13].
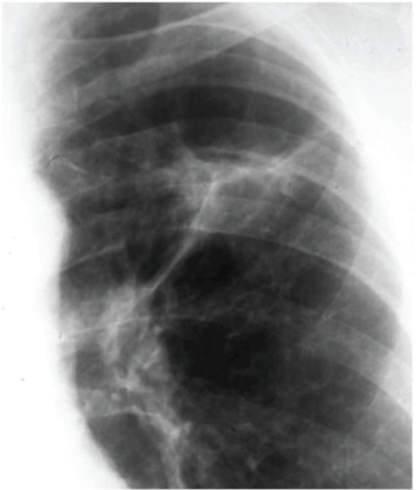 Figure 7: Chest x-ray showing Ghon's complex of active TB. View Figure 7
Figure 7: Chest x-ray showing Ghon's complex of active TB. View Figure 7
 Figure 8: Chest x-ray showing a Ghon's focus as persistent of the calcifying scar. View Figure 8
Figure 8: Chest x-ray showing a Ghon's focus as persistent of the calcifying scar. View Figure 8
 Figure 9: Chest x-ray showing smooth tuberculoma as persistent mass like opacities. View Figure 9
Figure 9: Chest x-ray showing smooth tuberculoma as persistent mass like opacities. View Figure 9
On the other hand, active post-primary pulmonary tuberculosis (TB reactivation or secondary TB) been a disease of the adult when the patient had previously exposed to Mycobacterium TB bacilli within the last two years when patient's immunity is deteriorating. X-ray findings of post-primary TB either an ill-defined patchy consolidation with a cavitary lesion or fibroproliferative disease with coarse reticulonodular densities usually involving the posterior segments of the upper lobe, or the superior segment of the lower lobe spread to endobronchial given "tree-in-bud" appearance [13-15]. The nodular lesion with poorly defined margins and with round density within the lung parenchyma also called hazy tuberculoma (Figure 10-14) [15].
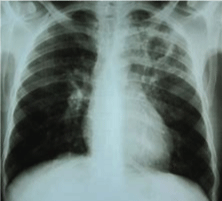 Figure 10: Chest x-ray showing cavitary lesion on the upper left lung post-primary pulmonary TB. View Figure 10
Figure 10: Chest x-ray showing cavitary lesion on the upper left lung post-primary pulmonary TB. View Figure 10
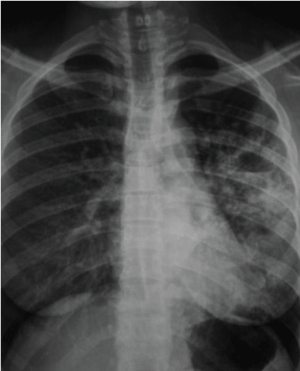 Figure 11: Chest x-ray showing cavitary lesion and air-fluid level on the lower left and middle lobe of right lung post-primary pulmonary TB. View Figure 11
Figure 11: Chest x-ray showing cavitary lesion and air-fluid level on the lower left and middle lobe of right lung post-primary pulmonary TB. View Figure 11
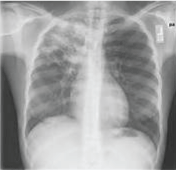 Figure 12: Chest x-ray showing fibroproliferative lesion on the upper right lung of post-primary pulmonary TB. View Figure 12
Figure 12: Chest x-ray showing fibroproliferative lesion on the upper right lung of post-primary pulmonary TB. View Figure 12
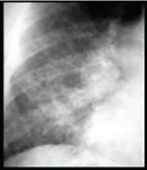 Figure 13: Chest x-ray showing coarse reticulonodular densities on the lower right lung of post-primary pulmonary TB. View Figure 13
Figure 13: Chest x-ray showing coarse reticulonodular densities on the lower right lung of post-primary pulmonary TB. View Figure 13
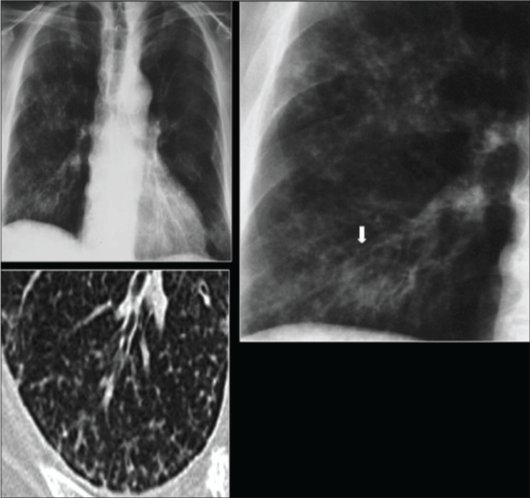 Figure 14: Chest x-ray showing coarse reticulonodular densities on the lower right lung of post-primary pulmonary TB. View Figure 14
Figure 14: Chest x-ray showing coarse reticulonodular densities on the lower right lung of post-primary pulmonary TB. View Figure 14
The end sequels of secondary TB are either fibrocalcific scar, fibronodular scar with lobar collapse, traction bronchiectasis mucoid impactions, pleural thickening, and pleural calcification (Figure 15-21) [15].
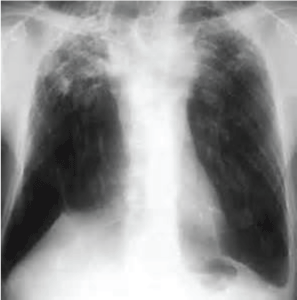 Figure 15: Chest x-ray showing fibrocalcific scar as airspace opacification or haziness between or surrounding these densities. View Figure 15
Figure 15: Chest x-ray showing fibrocalcific scar as airspace opacification or haziness between or surrounding these densities. View Figure 15
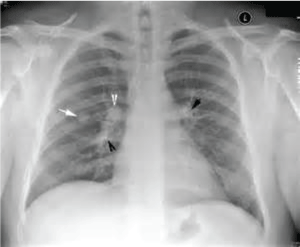 Figure 16: Chest x-ray showing discrete round nodule(s) with round edges without calcification. View Figure 16
Figure 16: Chest x-ray showing discrete round nodule(s) with round edges without calcification. View Figure 16
 Figure 17: Chest x-ray showing distinct fibrotic scar with volume loss or retraction with an upward deviation of the fissure or hilum on the corresponding side with asymmetry of the volumes of the two thoracic cavities. View Figure 17
Figure 17: Chest x-ray showing distinct fibrotic scar with volume loss or retraction with an upward deviation of the fissure or hilum on the corresponding side with asymmetry of the volumes of the two thoracic cavities. View Figure 17
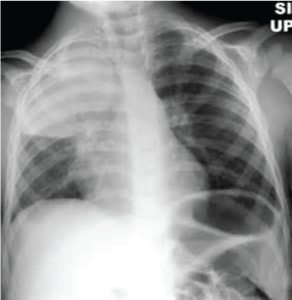 Figure 18: Discrete nodule(s) with volume loss or retraction-One or more nodular densities with distinct borders and no surrounding airspace opacification with a reduction in the space occupied by the upper lobe. Nodules are round or have rounded edges. View Figure 18
Figure 18: Discrete nodule(s) with volume loss or retraction-One or more nodular densities with distinct borders and no surrounding airspace opacification with a reduction in the space occupied by the upper lobe. Nodules are round or have rounded edges. View Figure 18
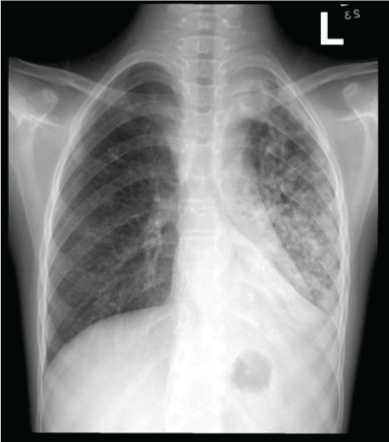 Figure 19: Chest x-ray showing volume loss, and lobar collapse. View Figure 19
Figure 19: Chest x-ray showing volume loss, and lobar collapse. View Figure 19
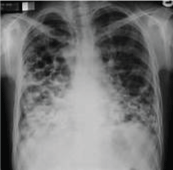 Figure 20: Chest x-ray showing course bronchiectasis densities on the bilateral lung of post-primary pulmonary TB. View Figure 20
Figure 20: Chest x-ray showing course bronchiectasis densities on the bilateral lung of post-primary pulmonary TB. View Figure 20
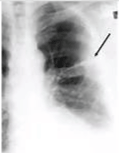 Figure 21: Chest x-ray showing pleural thickening of post-primary TB. View Figure 21
Figure 21: Chest x-ray showing pleural thickening of post-primary TB. View Figure 21
In general, the physician should have a high index of suspicion of active TB lesion and should differentiate it from inactive TB lesion (Table 1) [16,17].
Table 1: Radiological lesion of active and inactive pulmonary TB. View Table 1
Latent TB infection is an asymptomatic individual with a routine chest x-ray, and a negative sputum smear has a positive skin test (PPD/TST) (Table 2) or blood IGRA test result indicate previous TB infection [16,17].
Table 2: Classification of the positive tuberculin skin test (PPD) reaction [18]. View Table 2
The physician should know the causes of false-positive PPD reactions (e.g., Infection with non-tuberculosis mycobacteria, prior BCG vaccination, incorrect method of the administration, wrong interpretation of reaction, an incorrect bottle of antigen used). Likewise, the physician should detect causes of false-negative PPD reactions (e.g., low immunity, recent or ancient TB infection, early infancy ≤ six months, current live-virus vaccination or disease, incorrect method of PPD administration, and incorrect interpretation of reaction) [16,17].
PPD is contraindicated only for people who had a previous severe reaction (e.g., acute necrosis, blistering, anaphylactic shock, or ulcerations) to an earlier TST [18].
Treatment of latent TB infection is a once-weekly regimen of mixed rifapentine plus isoniazid for three months instead of 9 months INH treatment [19].
The minor X-ray findings that not suggestive of TB disease require no follow-up evaluation (e.g., Pleural thickening, diaphragmatic tenting, blunting of costophrenic angle, solitary calcified nodules or granuloma, minor musculoskeletal findings, and minor cardiac findings) [20-26].
Setting nationally standardized TB screening program is essential for early detection of active pulmonary TB. The best methods for TB screening are parallel to both the symptom inquiry and the chest radiography (CXR). Physicians should be trained for early diagnosis of active TB; they should differentiate between active and inactive radiological signs. The physician should provide diagnosis of latent TB infection and give the proper management. TB algorithm should be simplified and updated regularly
None.
None.
None.