A previously independent 80-year-old male had a significant single bright-red rectal bleed three day following a total hip replacement.
A patient review revealed a history of recent occasional PR bleeding typically manifesting as spotting on toilet paper often accompanied by constipation. He had known diverticular disease, haemorrhoids and a previous gastric ulcer. He was also on rivaroxaban for atrial fibrillation and had a 30 pack years history of smoking cigarettes. He had never had a colonoscopy.
A rectal examination was conducted which revealed a small mass at the anal verge which was diagnosed originally as a thrombosed external haemorrhoid and once the patent had stabilised after two units of blood he was discharged with a plan for outpatient colonoscopy within 3 months.
One month later the patient presented to the emergency department with enlarged groin lymph nodes and ongoing PR bleeding. Concerning features were then later elicited including unintentional weight loss, altered bowel habit and lethargy. On examination there were multiple firm left inguinal lymph nodes and a dark coloured anal mass. An examination under anesthetic was performed revealing a large firm melanocytic anal mass extending into the rectum. A biopsy was performed, and histopathology revealed malignant melanoma (Figure 1).
 Figure 1: Pigmented nodular melanoma with high-powered view showing eccentric irregular hyperchromatic nuclei with heavily pigmented melanocytes. View Figure 1
Figure 1: Pigmented nodular melanoma with high-powered view showing eccentric irregular hyperchromatic nuclei with heavily pigmented melanocytes. View Figure 1
A staging CT was conducted soon thereafter and showed a small lung nodule, multiple liver and spleen lesions (Figure 2) and significant lymphadenopathy (largest inguinal node measured up to 7 cm). The anorectal mass was also visible and measured 48 mm × 36 mm × 85 mm which was not visible in a CT conducted two months prior (Figure 3).
 Figure 2: Soft tissue density mass evident in posterior part of perineum. View Figure 2
Figure 2: Soft tissue density mass evident in posterior part of perineum. View Figure 2
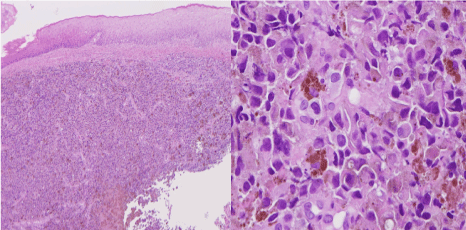 Figure 3: Ill-defined hypodense lesions consistent with metastatic deposits. View Figure 3
Figure 3: Ill-defined hypodense lesions consistent with metastatic deposits. View Figure 3
The patient was admitted under the care of medical oncology for treatment however it was soon concluded that curative treatment was not possible due to advanced disease progression and recent marked functional decline. He however underwent symptomatic radiotherapy to the primary lesion to reduce bleeding. Once symptom control was otherwise satisfactorily achieved the patient was discharged to a nursing home and was managed by community palliative care for two months until he passed away.
This case highlights the difficulties in identifying rectal cancer when a hemorrhoid diagnosis already exists. Prevalence of haemorrhoids has been estimated at about 40% [1] while primary anorectal melanoma accounts for approximately 0.4% of all malignant melanomas [2]. The local signs and symptoms of anorectal melanoma display a convincing masquerade and include bleeding, anal mass, anal pain, tenesmus, and changes in bowel habit which are frequently shared with symptomatic hemorrhoids [3]. The systemic effects of malignancy, namely weight loss and fatigue are typically only seen after metastasis and beyond cure [4]. On examination of such lesions, pigmentation is a cardinal feature of melanoma however prolapsed, thrombosed or necrosed haemorrhoids may show similar colour changes. Furthermore, clinical suspicion may be further hindered because up to 87% of these lesions are amelanotic [5].
Histological tissue diagnosis is the single established method of differentiation. However, if melanoma is not suspected, standard haemorrhoidectomy or polypectomy may not provide enough tissue to determine the extent of the lesion and reoperation may be required. It can therefore be suggested that even in the case of minor clinical suspicion, a biopsy should be taken first to confirm or exclude a diagnosis of anorectal melanoma [6]. Like in our patient, early nodal metastases are common and warrants a thorough diagnostic work-up including systemic imaging and endoscopic evaluation [4].
Following histopathological diagnosis and staging, surgical excision is the preferred treatment with or without the use of combined chemotherapy/immunotherapy and radiotherapy depending on the local and nodal infiltration as well as the presence of metastatic disease. The two widely used surgical interventions are abdominoperineal resection (APR), which reduces the risk of recurrence to a minimum however necessitates colostomy, or wide local excision, which results in greater functional preservation however a higher risk of disease progression [7].
There is a significant and proven role of radiation (both curative and palliative) in anorectal cancers however the effects of which are typically measured through far more common cancers such as squamous, basaloid, or cloacogenic carcinomas [8]. In these cases, radiation therapy alone can offer up to a 5-year survival rate of greater than 70% [9]. However, when combined with chemotherapy (such as with Fluroacil and mitomycin-C) a lower dose of radiation can be administered leading to fewer side-effects such as local tissue damage and irritation [10].
This case illustrates the importance of considering anorectal malignancy, including melanoma, as a differential diagnosis even in benign sounding PR bleeding. A thorough examination and high index of suspicion is required as a delayed diagnosis can have significant consequences for the patient.