Objective: Acute appendicitis is a prevalent surgical emergency that requires prompt diagnosis and intervention. Ultrasound is frequently utilized as a first-line diagnostic tool due to its accessibility and non-invasive nature. However, its diagnostic accuracy can vary due to several influencing factors. Histopathological examination remains the gold standard for confirming appendicitis. This study evaluates the compatibility between ultrasound findings and histopathological results in diagnosing acute appendicitis.
Methods: A prospective cross-sectional study was conducted across three hospitals in Iraq Al-Turki Hospital, Al-Jumhori Hospital, and Al-Sadr Hospital from November 29, 2024, to February 3, 2025. A total of 158 patients clinically suspected of having acute appendicitis underwent abdominal ultrasound followed by surgical appendectomy. Histopathological examination of the removed appendix served as the reference standard. Statistical analysis was conducted to calculate sensitivity,
Results: Out of 158 patients, 110 had positive ultrasound findings. The diagnostic performance of ultrasound revealed a sensitivity of 100%, specificity of 70%, positive predictive value of 82.4%, negative predictive value of 100%, and an overall diagnostic accuracy of 87.5%. There were no false negatives, indicating that ultrasound was highly effective in ruling out appendicitis when negative.
Conclusions: Ultrasound proved to be a highly sensitive and effective diagnostic tool for detecting acute appendicitis, particularly valuable in ruling out the condition. Despite variability due to operator and patient-related factors, its strong correlation with histopathological results supports its role as a frontline diagnostic modality, especially in emergency and resource-limited settings.
Acute appendicitis, Ultrasound
The appendix is a thin, hollow tube located in the lower right portion of the abdomen. It is anatomically connected to the cecum, which is the initial part of the large intestine. Typically, it lies at a location known as McBurney’s point, which is situated between the navel and the upper part of the right hip bone. The appendix generally measures between 7 to 10 centimeters in length, although its size can vary. Its average diameter is about 6 millimeters. The distal end of the appendix is closed, giving it a worm-like appearance, which is reflected in its name [1].
Appendix is lined internally with a mucosal layer and contains lymphoid tissue, which plays a role in the immune system, particularly during childhood. Its walls are composed of the same histological layers as the rest of the gastrointestinal tract: mucosa, submucosa, muscularis, and serosa [2]. Although the appendix is not considered an essential organ in adults, its potential immune function in earlier stages of life continues to be recognized [3]. One of the most common and urgent medical conditions involving the appendix is acute appendicitis. This condition, characterized by acute inflammation of the appendix, is a leading cause of severe abdominal pain that often necessitates emergency surgical intervention [4]. If not promptly treated, appendicitis can result in the perforation of the appendix and the spread of infection into the abdominal cavity, leading to peritonitis and posing a significant risk to the patient’s life [5-8].
Clinically, appendicitis typically presents with a constellation of symptoms, including sharp pain localized in the lower right side of the abdomen, nausea, vomiting, anorexia, and fever. Surgical removal of the appendix (appendectomy) remains the most effective and common treatment to prevent serious complications. Treatment options include:
• Open surgery, where a single incision is made in the lower abdomen to remove the appendix [9].
• Laparoscopic surgery, a more advanced technique that uses small incisions and specialized instruments, offering a faster recovery and reduced risk of infection [10]. In select early-stage cases, antibiotic therapy may be considered; however, this approach does not always negate the need for surgical intervention [11].
• The diagnosis of appendicitis involves a combination of clinical evaluation and diagnostic tests [12].
• Clinical examination to assess pain location and abdominal tenderness.
• Laboratory tests, particularly blood tests that may reveal elevated white blood cell counts suggestive of inflammation.
• Urine tests, which help rule out urinary tract conditions that may mimic appendicitis. While Imaging studies, most notably [13-16].
• Ultrasound - a non-invasive, rapid, and accessible imaging method.
• CT scan - offering greater accuracy in identifying signs of inflammation Among these, ultrasound and histopathological examination are key tools in the diagnosis and confirmation of appendicitis. Ultrasound imaging allows clinicians to detect signs of inflammation or fluid collection around the appendix quickly and safely. In contrast, histopathological analysis, conducted post-surgically, is considered the gold standard for confirming the presence and severity of appendicitis through microscopic examination of the removed tissue [17].
The importance of this study lies in evaluating the extent of compatibility between ultrasound findings an histopathological results. If ultrasound imaging can reliably predict the presence and severity of appendicitis as confirmed by histopathology, it may serve as a dependable diagnostic tool. This can enhance early diagnosis, reduce the rate of unnecessary surgeries, and optimize treatment planning.
Therefore, understanding this correlation is essential. It contributes to improving the accuracy and reliability of non-invasive diagnostic techniques, ultimately supporting clinical decision-making and patient outcomes. Ultrasound is commonly used as a first-line imaging modality due to its accessibility, safety, and cost-effectiveness. However, ultrasound findings can be limited by various factors, including the patient's body habitus, the skill of the operator, and the position of the appendix within the abdomen. These limitations contribute to significant variability in diagnostic accuracy, leading to discrepancies between sonographic assessments and the actual pathological state of the appendix [18,19].
Given that histopathological examination of the removed appendix is considered the gold standard for definitive diagnosis, it becomes essential to assess how reliably ultrasound correlates with histopathological findings. There is a clear need for diagnostic tools that are not only accurate and early but also non-invasive and practical in emergency settings [20]. Therefore, investigating the extent of compatibility between ultrasound and histopathology in cases of appendicitis is crucial for improving diagnostic confidence, reducing unnecessary surgeries, and enhancing patient outcomes [20-22].
The primary aim of this study is to evaluate the extent of compatibility between ultrasound findings and histopathological results in the diagnosis of acute appendicitis. By comparing the imaging-based diagnosis obtained through ultrasound with the definitive histopathological diagnosis after surgical removal of the appendix, the study seeks to determine the diagnostic accuracy and reliability of ultrasound as a non-invasive, rapid, and accessible diagnostic tool. This evaluation aims to contribute to improved clinical decision-making, reduce the incidence of unnecessary surgeries, and support the use of ultrasound as a dependable method for early detection and diagnosis of appendicitis, especially in emergency settings.
This study is a prospective, observational, cross-sectional study conducted to evaluate the diagnostic accuracy of abdominal ultrasound (US) in detecting acute appendicitis by comparing ultrasound findings with histopathological examination (HPE), which serves as the gold standard. The research was conducted across three prominent hospitals in Iraq: Al-Turki Hospital and Al-Jumhori Hospital located in the city of Al-Hilla, and Al-Sadr Hospital in the city of Najaf. These hospitals were selected for their advanced diagnostic and surgical capabilities, as well as their high patient throughput related to abdominal emergencies.
The study was carried out over a period of approximately ten weeks, specifically from 29 November 2024, to 3 February 2025. During this time, all patients who were clinically suspected of having acute appendicitis and who met the inclusion criteria were enrolled in the study.
A total of 158 patients were included in the study. All participants presented to the emergency departments of the aforementioned hospitals with signs and symptoms suggestive of acute appendicitis, such as right lower quadrant abdominal pain, fever, nausea or vomiting, anorexia, and elevated white blood cell (WBC) count. Upon presentation, each patient was assessed clinically and underwent an abdominal ultrasound examination performed by experienced radiologists using standardized scanning protocols. The ultrasound results were recorded as either positive (indicating signs consistent with appendicitis such as a noncompressible tubular structure > 6 mm in diameter, presence of peri appendiceal fluid, etc.) or negative (no signs of appendicitis).
Following clinical and radiological evaluation, patients underwent surgical appendectomy. The excised appendix was then sent for histopathological analysis, which confirmed or ruled out the diagnosis of appendicitis based on microscopic examination. A structured data collection form was used for each patient to document:
1) Demographic data: age and gender.
2) Clinical symptoms: presence of pain, fever (categorized as none, 37.5°C, or 38°C), vomiting, and anorexia.
3) Laboratory results: WBC count (normal or elevated).
4) Ultrasound findings.
5) Histopathological results.
All data were cross-verified with patient records for accuracy and consistency.
Patients age below 18 and above 60, patients with no medical disease (past medical history negative).
The collected data were entered into Microsoft Excel and analyzed statistically to determine the diagnostic value of ultrasou 4. False Negatives (FN) [23]: Cases where ultrasound was negative but histopathology confirmed appendicitis. Based on these values, the following were computed:
• Sensitivity = TP / (TP + FN)
• Specificity = TN / (TN + FP)
• Positive Predictive Value (PPV) = TP / (TP + FP)
• Negative Predictive Value (NPV) = TN / (TN + FN)
• Accuracy = (TP + TN) / Total number of cases
Furthermore, a matching analysis was performed to compare the consistency between ultrasound and histopathological findings. Cases were classified as: 1) Positive matching: both US and HPE results were positive, and 2) Negative matching: both results were negative. The diagnostic performance was then summarized in contingency tables and visualized using bar charts and pie charts to enhance clarity.
The study was conducted in compliance with ethical standards. Permission to access patient data and perform diagnostic evaluations was obtained from the respective hospitals. All patient data were anonymized to maintain confidentiality. If required by the institutional review boards, verbal or written consent was obtained prior to inclusion.
This chapter presents a comprehensive statistical analysis of the data collected from patients suspected of having appendicitis. The objective is to evaluate the extent of compatibility between ultrasound findings and histopathological outcomes and to assess the diagnostic accuracy of ultrasound in clinical settings. The study analyzed a total of 158 participants in (Table 1), with a fairly even distribution of age groups. Among the participants, 78 individuals (49.4%) were aged above 30, while 80 individuals (50.6%) were under the age of 30. Regarding gender distribution, a majority of the participants were male, with 100 males (63.3%), and the remaining 58 (36.7%) were female. The study also examined the presence and severity of fever, which was observed in varying degrees among the participants. Specifically, 50 individuals (31.6%) did not experience any fever, while 58 participants (36.7%) had a mild fever of 37.5°C, and 56 participants (34.7%) experienced a higher fever of 38°C. Pain, a common symptom in the study group, was reported by a significant majority of 152 participants (96.2%), while a small number, just 6 participants (3.8%), reported no pain. Vomiting was also a frequent symptom, with 110 participants (69.6%) experiencing it, while 48 participants (30.4%) did not. Anorexia, another symptom commonly associated with illness, was present in 102 participants (64.6%), and 56 participants (35.4%) did not report this symptom.
Table 1: Descriptive statistics. View Table 1
The study further examined white blood cell (WBC) counts as an indicator of potential infection or inflammation. Of the participants, 70 (44.3%) had a normal WBC count, while 88 participants (55.7%) showed an increased WBC count, indicating a possible underlying infection or inflammatory response. In terms of diagnostic imaging, ultrasound was used to evaluate the participants, and 110 cases (69.6%) had positive ultrasound findings, suggesting an abnormality or condition consistent with the clinical diagnosis. In contrast, 48 participants (30.4%) had negative ultrasound results, indicating that no significant abnormality was observed. These findings highlight the variability in clinical presentation and diagnostic outcomes among the study participants.
The study also assessed the correlation between ultrasound findings and histopathology results (Table 2 and Figure 1). Among the 34 participants with positive ultrasound results, 28 had a positive histopathology result, while 6 had a negative histopathology result. For those with negative ultrasound findings (14 participants), all 14 had negative histopathology results, and none showed a positive histopathology result. In total, 28 participants had both positive ultrasound and positive histopathology findings, while 20 participants had negative histopathology results, regardless of the ultrasound outcome.
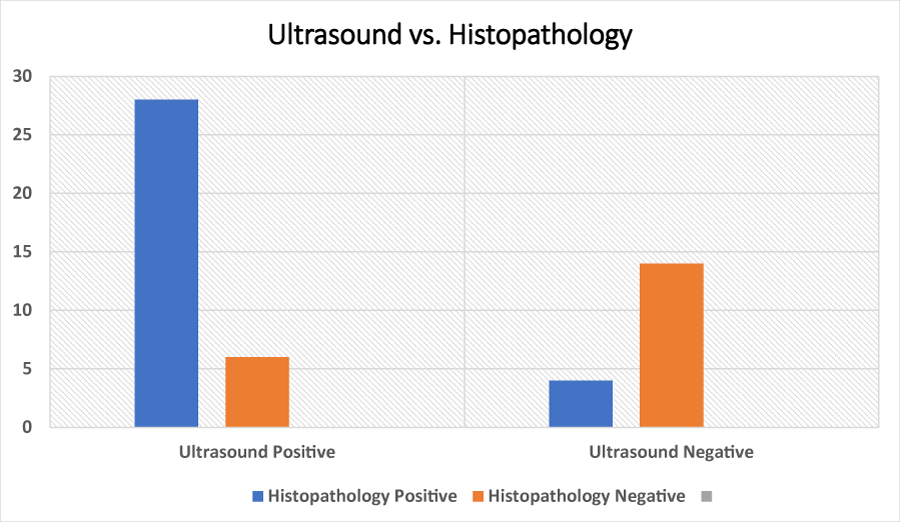 Figure 1: Ultrasound Vs. Histopathology Results.
View Figure 1
Figure 1: Ultrasound Vs. Histopathology Results.
View Figure 1
Table 2: Ultrasound Vs. Histopathology results. View Table 2
The diagnostic evaluation of ultrasound compared to histopathology revealed strong performance metrics (Table 3). There were 28 true positives, 6 false positives, 14 true negatives, and no false negatives. The sensitivity was 100%, indicating that all actual positive cases were correctly identified. Specificity was 70%, reflecting that 70% of true negative cases were correctly recognized. The positive predictive value (PPV) was 82.4%, meaning that over 82% of the ultrasound-positive results were truly positive. The negative predictive value (NPV) was 100%, showing that all ultrasound-negative results corresponded to true negatives. Overall diagnostic accuracy reached 87.5%, demonstrating the reliability of ultrasound as a diagnostic tool in this context.
Table 3: Diagnostic performance of ultrasound. View Table 3
The matching results in (Table 4 and Figure 2), showed a total of 110 positive matching cases and 48 negative matching cases. This indicates that the diagnostic tool or method used successfully identified 110 cases where the test result matched the reference standard as positive, and 48 cases where it matched as negative, reflecting a consistent performance in both positive and negative classifications.
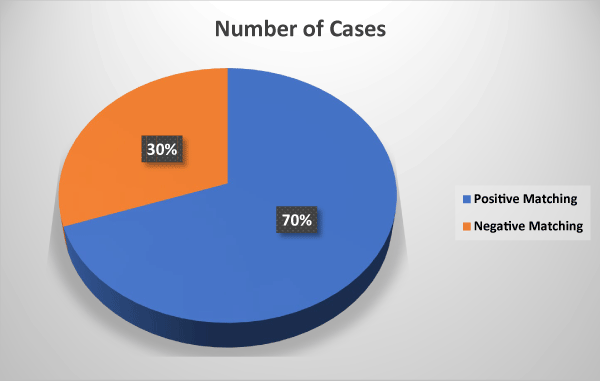 Figure 2: Diagnostic Performance of Ultrasound.
View Figure 2
Figure 2: Diagnostic Performance of Ultrasound.
View Figure 2
Table 4: Diagnostic Performance of Ultrasound. View Table 4
In the current study, ultrasound demonstrated a sensitivity of 100%, specificity of 70%, positive predictive value of 82.4%, negative predictive value of 100%, and an overall diagnostic accuracy of 87.5% in diagnosing acute appendicitis. These findings point to the strength of ultrasound as a highly sensitive tool, particularly effective in ruling out appendicitis when results are negative.
Compared to this study, Fu, et al., (2021) reported lower sensitivity and specificity, 77.2% and 60% respectively [24], in a meta-analysis that likely reflected broader inclusion criteria and a range of operator experience across settings. Similarly, Pather, et al., (2023) showed that ultrasound sensitivity in adults could vary widely between 39% and 96.4%, depending largely on whether the appendix was directly visualized, aligning with our findings where full visualization may have contributed to the high sensitivity [25].
In a retrospective assessment by Zhang, et al., (2024), diagnostic accuracy differed with disease stage: 68.75% in simple appendicitis, 73.22% in suppurative, and 81.81% in gangrenous cases [26]. These values fall below the overall accuracy we observed, likely due to the more detailed stratification in their methodology. Al- wageeh, et al., (2023) demonstrated that combining the Alvarado score with ultrasound yielded remarkably improved results-sensitivity of 98.5%, specificity of 82.9%, and accuracy of 94.7% [27]. This supports the notion that clinical scoring systems enhance diagnostic precision, which was not utilized in our study and may explain our lower specificity.
Kakar, et al., (2023) found that supplementing ultrasound with laboratory inflammatory markers such as leukocyte count, neutrophil percentage, and C-reactive protein led to almost perfect diagnostic values (99% sensitivity and 98% specificity) [28], a result that further highlights the benefit of integrating imaging with laboratory evidence-another strategy absents from our methodology. In another study, Lee, et al., (2023) emphasized that an appendiceal diameter ≥ 6.5 mm increased diagnostic accuracy to 92%, while our study did not quantify this measurement, which may have introduced variability in how positive findings were interpreted [29].
A broader view was offered by Ahmed, et al., (2022), who reported pooled values of 82.1% sensitivity and 85.9% specificity for ultrasound in appendicitis diagnosis, values close to our results in general accuracy, though again with better specificity [30]. This trend was echoed in standardized diagnostic studies like that of Morales, et al., (2020), who found sensitivity at 78% and specificity at 83%, emphasizing the utility of following structured reporting guidelines to enhance clarity and reproducibility-practices that were not formally applied in our protocol [31].
Supporting evidence from Alqarni, et al., (2019) found ultrasound to correctly diagnose 86% of appendicitis cases, though their 14% false-negative rate contrasts sharply with the zero false negatives in our study, possibly due to differences in operator training or equipment [32]. Conversely, Mansour, et al., (2019) reported notably lower performance in children, with sensitivity of 58% and specificity of 68%, which reflects the difficulties often encountered in pediatric imaging and reinforces the strength of our outcomes in an adult cohort [33].
Operator experience was thoroughly analyzed by Hassan, et al., (2023), who demonstrated significantly improved results when scans were performed by experienced radiologists a likely contributor to our excellent sensitivity [34]. Additionally, Youssef, et al., (2023) emphasized that obesity reduced ultrasound accuracy a factor we did not control for but which might explain our modest rate of false positives [35]. The role of evolving techniques was explored by Nakamura, et al., (2025), who applied contrast-enhanced ultrasound and reported improved diagnostic reliability. While we relied solely on conventional grayscale ultrasound, such techniques may prove beneficial in future research [36].
Finally, the relevance of point-of-care ultrasound (POCUS) in emergency settings was explored by Rivera, et al., (2023), who demonstrated that emergency physicians trained in ultrasound achieved 90% sensitivity and 85% specificity. This finding suggests that, with adequate training, even non-specialist operators can obtain reliable results-possibly mirroring the practical skill level of the operators involved in our study [37-40].
This study aimed to assess the compatibility between ultrasound findings and histopathological results in diagnosing acute appendicitis. The findings highlight that while ultrasound remains a widely accessible, non-invasive, and rapid diagnostic tool, its accuracy can be influenced by factors such as operator expertise and patient characteristics. Nonetheless, when used effectively, ultrasound can offer valuable preliminary insights that guide clinical decision-making. Histopathological examination, as the gold standard, confirms the final diagnosis and serves as a benchmark to evaluate the reliability of imaging modalities. The correlation observed between ultrasound and histopathological outcomes in this study supports the use of ultrasound as a frontline diagnostic method, especially in resource-limited or emergency settings. Ultimately, strengthening the diagnostic accuracy of ultrasound through improved protocols, training, and technology can significantly reduce unnecessary surgical interventions, enhance early detection, and improve overall patient outcomes in cases of suspected appendicitis.
I. Prioritize continuous training for radiologists and sonographers to enhance ultrasound diagnostic skills. Use standardized ultrasound protocols to reduce diagnostic variability.
II. Combine ultrasound with clinical and laboratory findings for accurate diagnosis; use CT when necessary.
III. Upgrade ultrasound equipment to improve image quality and diagnostic accuracy.
IV. Ensure routine histopathological examination of all removed appendices for confirmation and further insights.
V. Conduct larger-scale research to support findings and explore technological improvements.
VI. Educate patients about the diagnostic process to support informed decision- making.
The authors declare no conflict of interest.