Solid-cystic hidradenoma is an uncommon benign adnexal tumor arising from eccrine sweat glands which is also known as poroid hidradenoma. They are typically located in the head and neck area. In this report, a 76-year-old female patient presented with a painful and rapidly enlarging mass on the plantar forefoot. Surgical excision resulted in complete resolution of symptoms, with no recurrence observed at the two-year follow-up. Hidradenoma needs to be considered in the differential diagnosis of skin lesions located in atypical areas, as well as the importance of early surgical intervention for positive outcomes. This report includes the diagnostic evaluation as well as clinical and histological features of this tumor.
Hidradenoma, Sweat gland, Plantar forefoot mass, Adnexal tumor, Poroid
A clinically and Microscopically unique benign sweat gland tumor, solid-cystic hidradenoma of the skin initially developed as a single, cohesive idea in 1968 by Winkelmann and Wolff on adnexal tumors [1,2]. It was recently proposed that hidradenoma be divided into two groups: those with apocrine differentiation and those with eccrine differentiation, also referred to as poroid hidradenoma [3]. According to electron microscopy, these solid cystic lesions are originated in the eccrine sweat duct.
Over the years, this tumor has been referred to in the literature by various names, such as eccrine acrospiroma, clear cell myoepithelioma, and clear cell hidradenoma [4]. Kersting and Heiwig claim that a unique large-cell sweat gland tumor known as a solid and cystic hidradenoma might not have clear cells, and is comparable to a clear-cell myoepithelioma [5]. This kind of tumor most frequently occurs in the head and neck; it is uncommon to find it in the extremities. Radiation may be one of the exogenous risk factors, but none have been directly connected to this tumor [6].
One percent of primary cutaneous tumors are represented by hidradenoma. These tumors are most likely to develop in women between the ages of twenty and fifty [7]. The neoplasm manifests as a solitary, noncharacteristic dermal nodule located anywhere on the body, usually with a diameter ranging from 0.5 to 2 cm and without any prominent characteristics to establish a clinical diagnosis [8]. Skin changes are not common, but instances of red, blue, and purple discoloration, translucence, and ulceration accompanied by bleeding and viscous fluid discharge have been documented. The majority of cases do not present symptoms; however, certain lesions may develop tenderness when pressure is applied [9]. A study of nodular hidradenoma ultrasonography provides strong evidence of diagnosis when there is a presence of inner septa, “snow falling or fluid-level” sign in the cystic region [10].
Neoplasms involving the foot and ankle are rare, typically affecting soft tissue and being benign. However, hidradenoma can be malignant and metastasize to lymph nodes, bone, and lungs, with a high recurrence rate and mortality [11]. The identification of hidradenocarcinoma relies mainly on histopathological and immunohistochemical evidence. Surgical excision is largely curative, resulting in very low recurrence rates and an excellent prognosis for benign lesions [12].
We present a rare case of a painful, palpable solid-cystic hidradenoma located on the plantar side of the foot-an extremely uncommon site-mimicking malignancy or infection and necessitating extensive imaging and diagnostic workup for accurate diagnosis.
A 76-year-old woman presented initially in the clinic complaining of a mildly painful, growing mass for three to four weeks at the level of the first and second distal metatarsals on the right plantar forefoot. The patient's medical history was unremarkable. She denied previous skin lesions, congenital deformity, or any prior diagnosis of neoplastic disease. There was no relation of trauma or injury to the affected area. Clinical examination revealed a moderately sized, mobile mass in subcutaneous tissue with no soft tissue involvement below the first metatarsophalangeal joint. On palpation, the lesion was painful, and the skin had a normal appearance. The mass did not pulsate or illuminate. The patient related that the lesion had been enlarging progressively for three to four weeks. The overlying skin was normal in texture and color and had no breaks or ulceration. There appears to be no vascular abnormality present. There was no surrounding erythema or edema and no lymphadenopathy.
A three-view radiographic examination of the right foot was essentially unremarkable (Figure 1). It showed no evidence of intralesional mineralization, osseous erosion, or remodeling of the metatarsal bones. Afterwards, a magnetic resonance imaging (MRI) of the right foot was conducted revealing a subcutaneous lesion between the distal 1 st and 2 nd metatarsal (Figure 2).
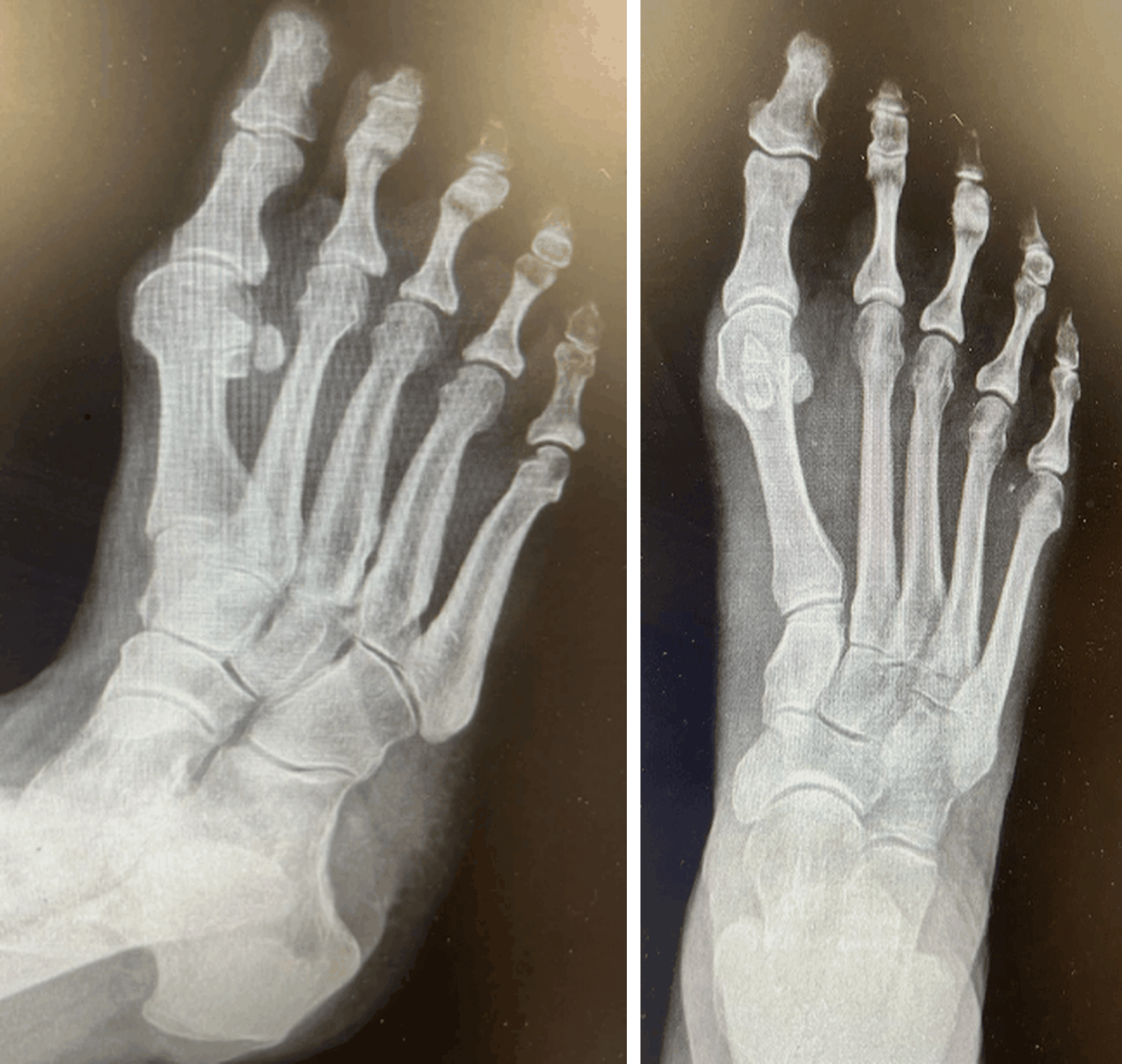 Figure 1: Anteroposterior view of right foot X-ray.
View Figure 1
Figure 1: Anteroposterior view of right foot X-ray.
View Figure 1
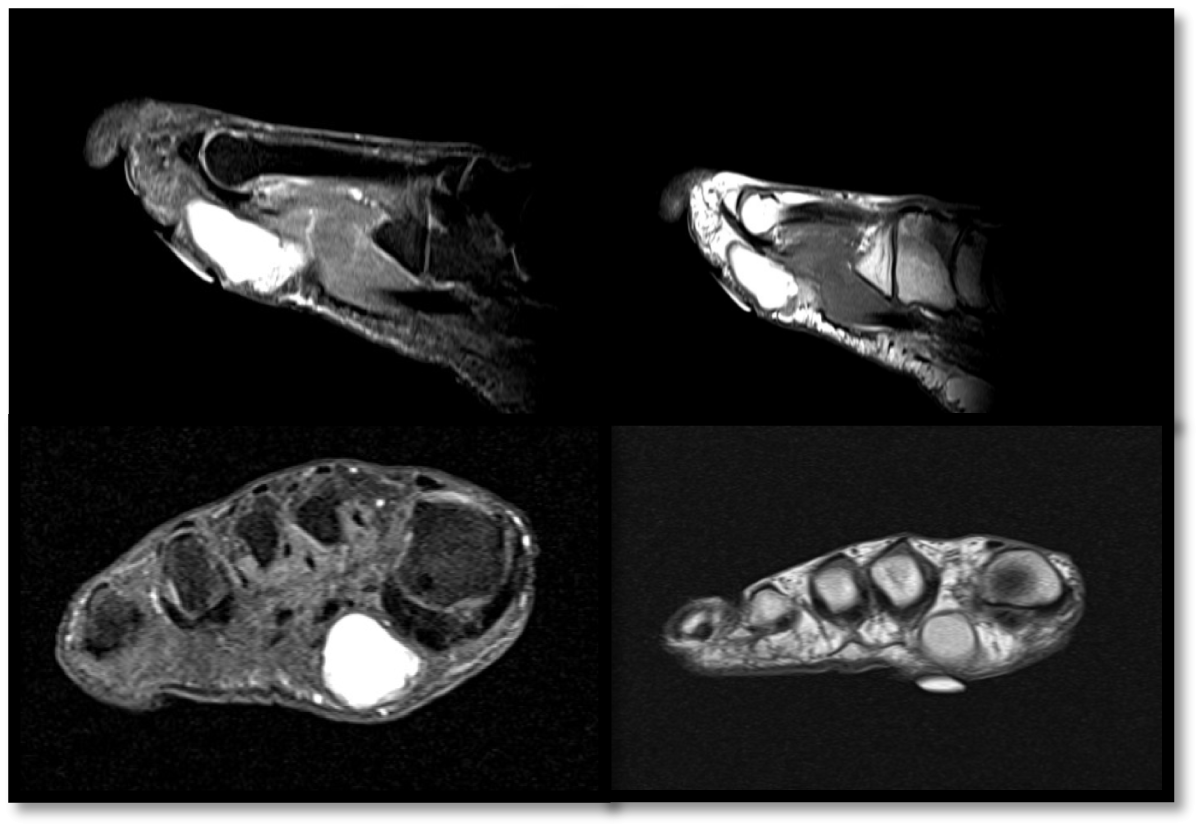 Figure 2: The magnetic resonance images exhibited a demarcated subcutaneous lesion measuring 3.5 × 2.6 × 1.6 cm located in the plantar forefoot at the distal first and second metatarsals, along the plantar aponeurosis. The lesion exhibited a heterogeneous hyperintensity on post-contrast sequences and somewhat hyperintensity on T1. The superficial aspect of the lesion seen 0.3 cm deep the skin surface and is seen abutting the superficial fascia of the lateral head flexor hallucis brevis and flexor digitorum brevis muscles. A cyst-like structure of greater size was observed, likely containing proteinaceous or hemorrhagic material.
View Figure 2
Figure 2: The magnetic resonance images exhibited a demarcated subcutaneous lesion measuring 3.5 × 2.6 × 1.6 cm located in the plantar forefoot at the distal first and second metatarsals, along the plantar aponeurosis. The lesion exhibited a heterogeneous hyperintensity on post-contrast sequences and somewhat hyperintensity on T1. The superficial aspect of the lesion seen 0.3 cm deep the skin surface and is seen abutting the superficial fascia of the lateral head flexor hallucis brevis and flexor digitorum brevis muscles. A cyst-like structure of greater size was observed, likely containing proteinaceous or hemorrhagic material.
View Figure 2
Considering the intractable nature of the plantar forefoot mass and the unresolved issue of malignancy, conservative and surgical intervention options were discussed. The patient opted for surgical excision. The patient was brought to the operating room and placed in a supine position. Following monitored anesthetic care, a local infiltration of 20 mL of 0.25% Marcaine plain was performed in local block fashion. A 2-inch incision was made over the plantar first metatarsal head using a meticulous blunt and sharp dissection retracting all bleeders encountered and neurovascular bundles.
Dissection was carried down to the level of the soft tissue mass. The mass was removed from the plantar foot without complications and the cultures were obtained. Gross examination of the mass revealed dimensions measuring 3.5 × 2.6 × 1.6 cm (Figure 3). It was dark and fluid-filled with brown fluid that had an odor to it. The wound was flushed and closed in layers without complications. A mass was sent for pathological examination as well as culture.
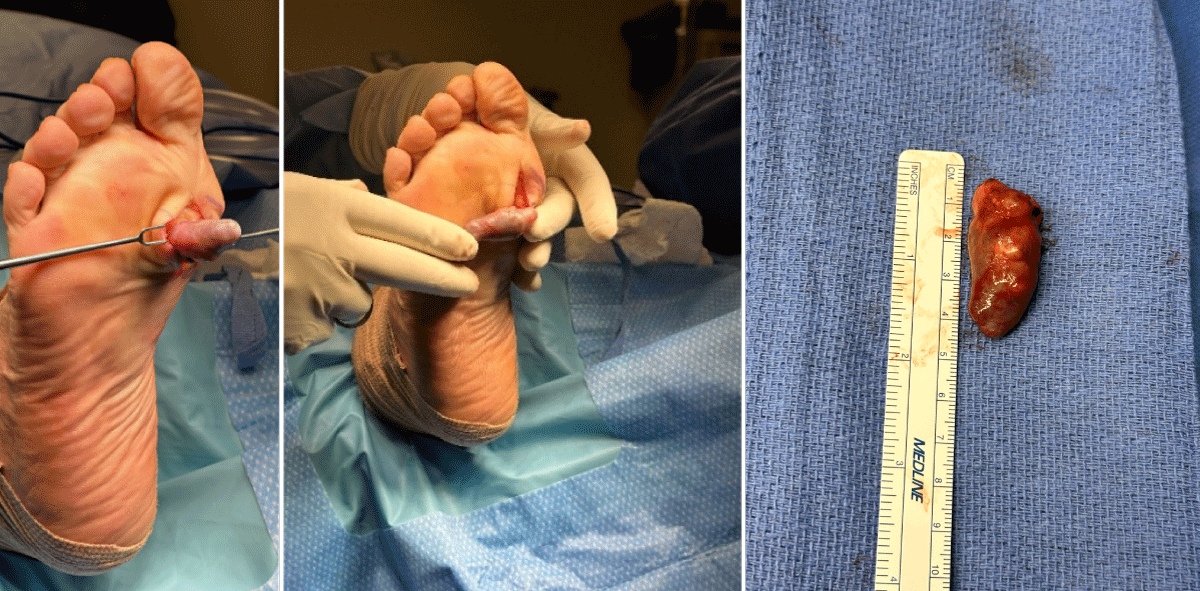 Figure 3: Right foot mass on plantar surface.
View Figure 3
Figure 3: Right foot mass on plantar surface.
View Figure 3
A Gram’s stain for bacterial and fungal cultures returned negative results. Sectioning revealed a collapsed, smooth-walled unilocular cyst, containing golden-brown, soft, friable debris. Histologically, the lesion had mixed cystic, solid, and mucinous/clear cell areas. The lesion was well indicated and lacked significant cytologic atypia, mitotic activity, and necrosis. The S100 and pankeratin exhibit positive staining which suggests that this lesion is not melanoma (Figure 4).
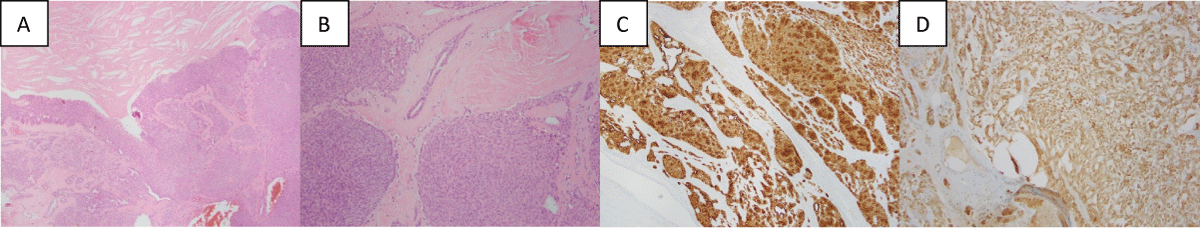 Figure 4: Histological and immunological images from excised hidradenoma: (A) Photomicrograph of hematoxylin-eosin (x4) showing an area of a proliferation of epithelial cells arranged in both solid nests and mucinous/clear cell areas which are a classic feature of hidradenoma; (B) Photomicrograph of hematoxylin-eosin (x10) further depicting the solid cellular nodules containing the thick, eosinophilic fibrous septa and hyalinized stroma; (C) Photomicrograph of S100 demonstrating areas of diffuse cytoplasmic brown positivity within the cells which is suggesting a significant portion of adnexal epithelial cells. Photomicrograph of Pankeratin displaying widespread brown staining which is a marker for epithelial cells.
View Figure 4
Figure 4: Histological and immunological images from excised hidradenoma: (A) Photomicrograph of hematoxylin-eosin (x4) showing an area of a proliferation of epithelial cells arranged in both solid nests and mucinous/clear cell areas which are a classic feature of hidradenoma; (B) Photomicrograph of hematoxylin-eosin (x10) further depicting the solid cellular nodules containing the thick, eosinophilic fibrous septa and hyalinized stroma; (C) Photomicrograph of S100 demonstrating areas of diffuse cytoplasmic brown positivity within the cells which is suggesting a significant portion of adnexal epithelial cells. Photomicrograph of Pankeratin displaying widespread brown staining which is a marker for epithelial cells.
View Figure 4
Postoperatively, the patient ambulated in the surgical shoe as tolerated for two weeks following transition to regular protective shoe gears. Sutures were removed at week two. Serial plain radiographs were taken at each follow up visit with no new abnormalities. At first-week follow-up, the patient was pain free with no complications (Figure 5). Patient was satisfied with the result and was able to return to normal activities.
 Figure 5: At 5-month follow-up, the surgical incision site was completely healed.
View Figure 5
Figure 5: At 5-month follow-up, the surgical incision site was completely healed.
View Figure 5
Solid-cystic hidradenoma is a benign skin tumor originating from eccrine sweat glands that usually appear asymptomatic, grows slowly, is solitary, and does not ulcerate [2]. They are mostly benign, with a low chance of malignancy. It affects all ages, most commonly females in the fourth to eighth decades of life [13]. Until now, we have only a few cases reported of solid cystic hidradenoma present at an unusual location of the dorsal foot as a mildly painful, nodular lesion. We present a similar case with acute and aggressive presentation in an elderly patient, raising more suspicion and diagnostic uncertainty.
These lesions most commonly appear as a single, fixed, firm nodule or plaque that is not painful. However, they can be multilobular, ulcerated, and fissured with cystic spaces, as observed in the current patient. Additionally, they can have discoloration as well. Unlike such a non-tender presentation of nodular hidradenoma on scalp reported by Shruthi Madhavi Govindarajulu [14], our patient presented with painful, progressively enlarging mass on plantar forefoot mimicking any malignancy.
MRI is useful in diagnosis due to higher contrast resolution for soft tissue lesions. On MRI, these tumors present as superficial lesions comprising both solid and cystic masses, distinguished by fluid levels in the cystic components and enhancement of the solid components. The cystic components show a range of MRI signal intensities, which is thought to result from differing quantities of cholesterol, hemorrhage, and sweat gland secretions present in the fluid [15]. Although histological examination is mostly used for the confirmation of malignancy. In our case, histologically the lesion had mixed cystic, solid, and mucinous/clear cell areas and lacked significant cytologic atypia, mitotic activity, and necrosis, ruling out malignancy.
It can originate from any cutaneous site, but the most common sites are the head and anterior surface of the trunk, with very rare cases in the extremities [16]. Only a few cases of foot hidradenoma have been reported yet, and all of them have been histologically confirmed [2,15,17].
In our case, the mass was progressively enlarging within three to four weeks and causing the patient some discomfort. As a result, we chose to perform a surgical excision to alleviate the patient's symptoms and establish a definitive diagnosis. Recurrences are usually uncommon, however, a routine follow-up is recommended as they are possible. The patient was pain free at the first week of postoperatively visit. At two years of continued follow up, no recurrence was observed, and all her symptoms had resolved.
Hidradenocarcinomas (HACs) typically develop de novo from eccrine and apocrine sweat glands, but they can also arise from the malignant transformation of a benign Hidradenoma (HA). Moreover, the recurrence rate of HA is lower than that of HAC. Consequently, eliminating HAs before malignant transformation can lead to a more favorable prognosis, underscoring the significance of early diagnosis and surgical intervention [18]. Jaime Sanchez Saz, et al. reported a case of a 27-year-old woman diagnosed with a hidradenocarcinoma over a previously excised hidradenoma in the right foot [6].
Solid-cystic hidradenoma remains a challenge to diagnose clinically without histological confirmation. We reported a case of solid cystic hidradenoma located in an atypical area on the plantar foot, exhibiting as a painful enlarging mass. The incidence of hidradenoma is higher in female than male. This type of benign tumor needs to be considered in the differential diagnosis for any dermal mass in the lower extremity, and it should be histologically confirmed. Early excision of hidradenoma prior to malignant transformation can lead to a more favorable prognosis, underlining the significance of early diagnosis and surgical intervention. The author’s approach is to surgically excise the lesion, followed by histological examination and careful clinical monitoring for recurrences over the next three to six months [4].