Penile cancer is a rare tumor; squamous cell carcinoma is the most common histologic type. This cancer is associated with poor prognosis. We report the case of a 56-year-old man, with a penile squamous cell carcinoma present for 06 years.
Penile cancer, Squamous cell carcinoma, Prognosis
Penile tumors are the rarest tumors of the male urogenital tract (1%). Squamous cell carcinoma is the most common histological type. Squamous cell carcinoma of the penis is most often presents between 50 and 70-years-old. Early diagnosis is imperative to avoid lymphatic spread that is associated with poor prognosis. We report the case of a 56-year-old man with squamous cell carcinoma of the penis present for 6 years.
A 56-year-old man presented with a lesion of the penis evolving for 06 years. There were no recent changes to the lesion. The patient denied any history of sexually transmitted infections. The patient was without a family history and in good general condition.
Physical examination showed ulcerated burgeoning lesion involving the glans penis (Figure 1) without inguinal lymphadenopathy or urinary signs. An Incisional biopsy was obtained and showed an epithelial tumor proliferation, arranged in masses and made of polyhedral cells, an abundant and eosinophilic cytoplasm, with a hyperchromatic ovoid nucleus. The diagnosis of a moderately differentiated, Infiltrating and non-keratinizing squamous cell carcinoma was retained (Figure 2A and Figure 2B).
The decision was made to refer the patient to urology department for evaluation and surgical decision.
Penile cancer is a rare tumor [1]. Their pathogenesis is not fully known; squamous cell carcinoma can evolve from penile intraepithelial neoplasia or develop de novo [2]. Squamous cell carcinoma of the penis has been associated with high-risk HPV infections [3]. Phimosis has been found in 25-60% of penile cancer patients, it is associated with an increased incidence of infection as well as dysplastic changes [4]. Other risk factors associated with the development of squamous cell carcinoma include smoking, HIV infection, poor genital hygiene, anterior penile lesions, chronic balanitis, lichen sclerosis and atrophicus and psoralen, and ultraviolet radiation [3]. The clinical presentation is variable, it may present as a small zone of induration and erythema or a large ulcerous and infiltrative lesion [3]. The prognosis is good for a localized disease; the most important prognostic factor is the extent of lymph node metastases, the prognosis with additional lymph node metastases is poor [6].
Penile cancer can cause high morbidity, a multidisciplinary management including dermatology, urology, medical oncology, radiation oncology, and psychiatry may be required.
The authors do not declare any conflicts of interest for this work.
All authors were actively involved in the development of this work.
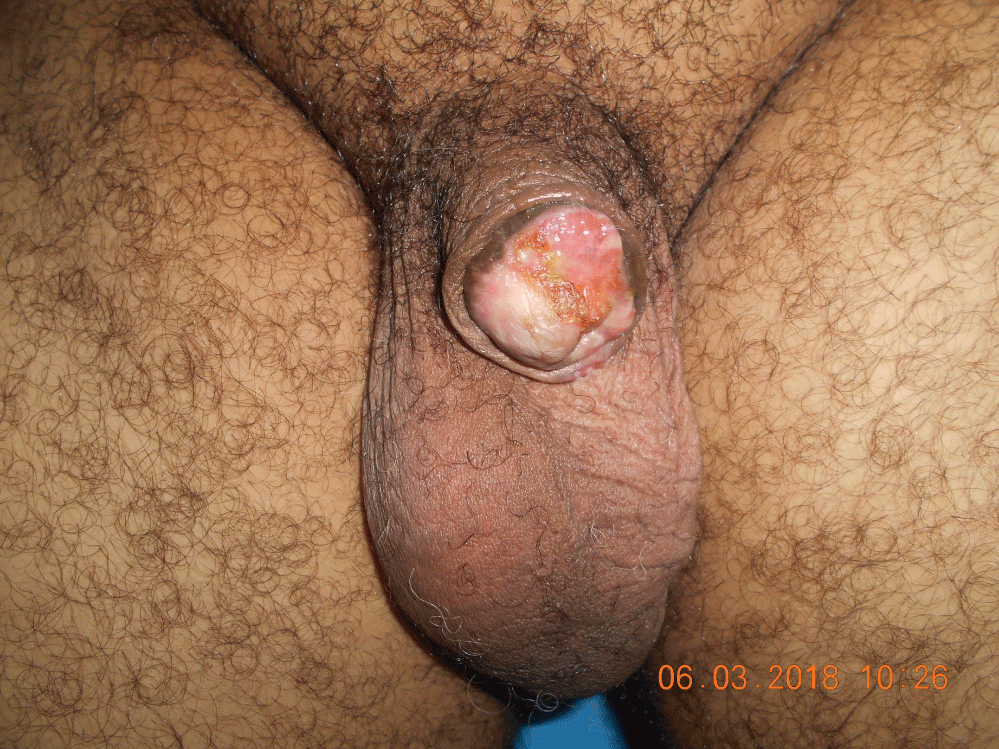
Figure 1: Erythematous and ulcerated lesion on the penis.
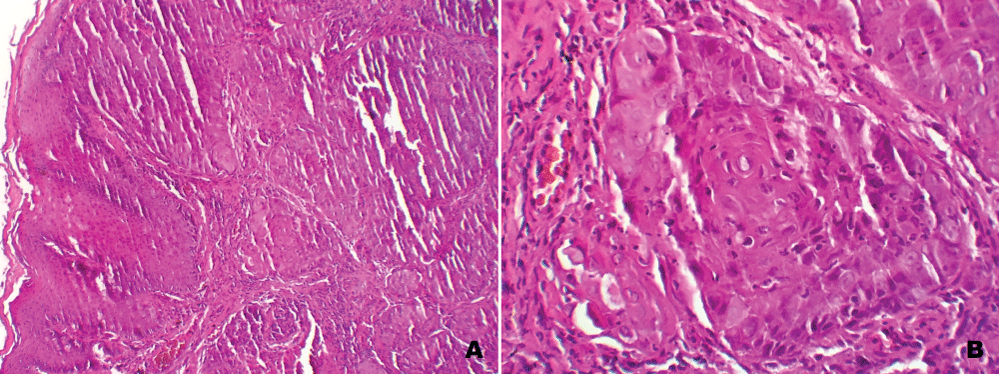
Figure 2: Infiltrating squamous cell carcinoma, moderately differentiated. A) Hematoxylin & eosin ×20; B) Hematoxylin & eosin ×40.