Black henna contact eczema is common and continues to increase. Paraphenyldiamine (PPD) in addition to its systemic toxicity not only exposes to a selective allergy to (PPD) but also to several of these derivatives and metabolites with cross reactions. We present a case of this irreflected practice.
Henna is very anciently used naturally by man for its dyeing characteristics for aesthetic and sometimes therapeutic purposes. Nowadays, and with the trend of tattoos, it is mixed with various chemicals to obtain a fast, durable and darker coloration, including para-phenyldiamine (PPD), a frequent source of local toxicity, including contact eczema and sensitization, and sometimes systemic. Our goal is to raise awareness, through this clinical case, the health authorities at first and the general public in a second time.
A young teenager of 16 years, without notable pathological antecedents including not known allergic to natural henna. Enjoyed a stay in the other city of Marrakech to make two tattoos at the two front arms (a scorpion and a dragon) with black henna. A week later, the young person consulted for erythemato-squamous lesions, very itchy at tattoo sites. The lesions were superinfected and the clinical examination for systemic involvement was without particularities (Figure 1). The diagnosis of contact dermatitis to black henna mixed with para-phenyldiamine (PPD) was discussed and withheld. The patient was initially treated with local antibiotic treatment with protected amoxicillin and fucidic acid for one week (Figure 2) and then with dermocorticoids and emollients for one month, with a favourable evolution.
Transient tattoos with black henna are currently very popular and may be a hidden source of awareness of (PPD) or one of its close derivatives in 2-7% of the population [1] and [2]. They contain up to 16% (PPD) compared to the allowed limit of 3% in hair dyes [2], this high content saturates the acetylation pathway, the direct consequence of which is the increase in the amount of metabolites (PPD) in the skin and activation of dendritic cells and lymphocytes of sensitized individuals. This allergy will persist throughout life with daily consequences and a possibility of cross-reactions to products containing (PPD) or one of its derivatives, which explains that the person become allergic to avoid contact with many products, with a considerable impact on its quality of life. The dermatological manifestations of contact dermatitis with PPD are of variable severity, similarly, cases of psoriasis on tattoo sites have been reported [3], noting finally, the relative gravity in patients with a deficit glucose-6-phosphate dehydrogenase (G6PD) [4].
The ever-increasing number of awareness cases (PPD) and the serious consequences for the quality of life of the patient justify the urgent need for public awareness and regulation of its use.
The authors do not declare any conflict of interest for this work.
All authors were actively involved in the development of this work the authors do not declare any conflict of interest for this work.
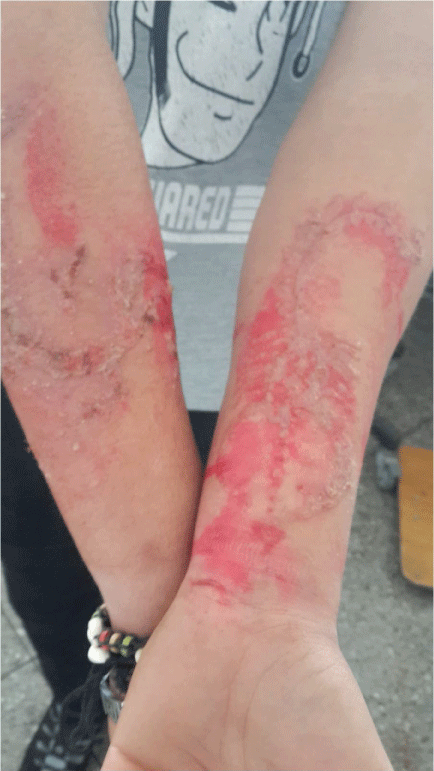
Figure 1: Lesions superinfected on admission.
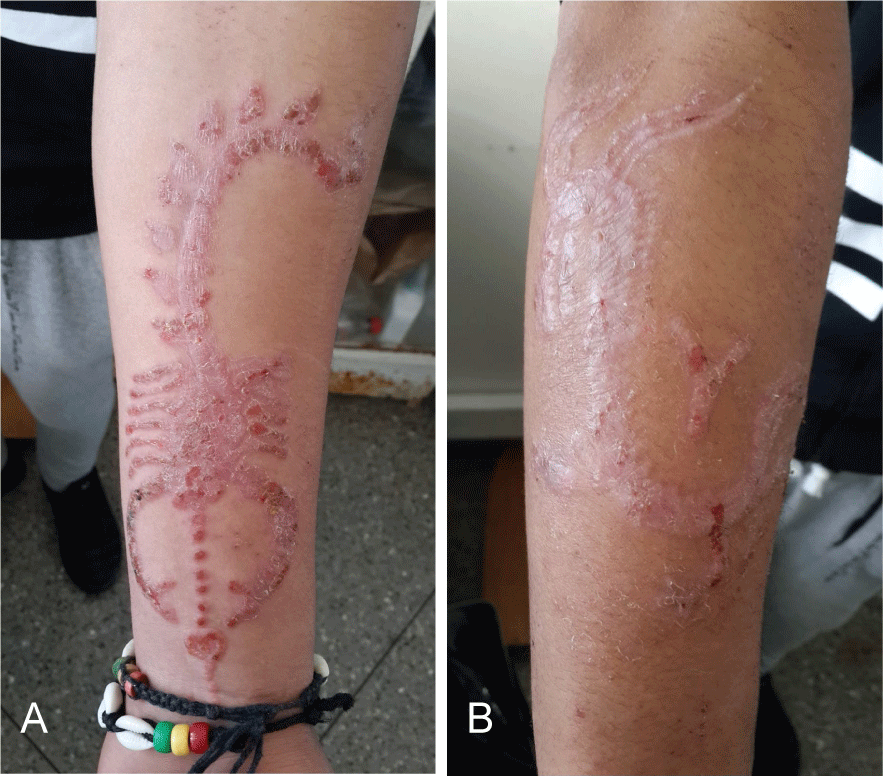
Figure 2: a,b) Clean lesions after 1 week of antibiotic treatment.