Infiltrating squamous cell carcinoma (SCC) of the penis is a rare tumor of easy diagnosis. The poor prognosis of this cancer justifies a rigorous oncological management which is often mutilating and badly accepted in our context. We present a case in an elderly man.
A 74-year-old man, with no notable pathological history, especially without condyloma or toxic exposure. Consulted for an ulcerated tumor of the ventrolateral side of the penis, of 5 centimeters in diameter, evolving for eight months, resistant to symptomatic treatments, bleeding on contact with an early scrotal infiltration and without inguinal lymphadenopathy or urinary signs (Figure 1). The cutaneous biopsy showed an epithelial tumor proliferation, arranged in masses and in casings made of polyhedral cells possessing a cellular framework, a cytoplasm of average abundance, basophilic and provided with a hyperchromatic ovoid nucleus and of variable size, the Mitotic figures are numerous, the stroma reaction is of fibroinflammatory type (Figure 2). The diagnosis of a moderately differentiated infiltrative and non-keratinizing epidermal carcinoma was retained. The locoregional and general extension assessment was reassuring and the patient was referred to an urology departement for additional care.
Penile cancer is rare and 95% of the cases histologically correspond to squamous cell carcinoma (SCC) [1]. Infection with oncogenic types of Human Papilloma Virus (HPV) and lichen sclerosus seem to be the main risk factors for this neoplasm [2,3]. The ignorance of practitioners, the conservative nature of the population, the taboos and the difficulties of access to care leaves even these tumors at advanced stages. Cancer of the penis can cause high morbidity because of both the disease itself and the treatment, which includes partial or total amputation of the organ [4].
Early diagnosis reduces this rate and allows for less aggressive treatment, contributing to these men's better quality of life. Training physicians for early detection of this type of cancer and instructing the lay population will certainly improve this scenario.
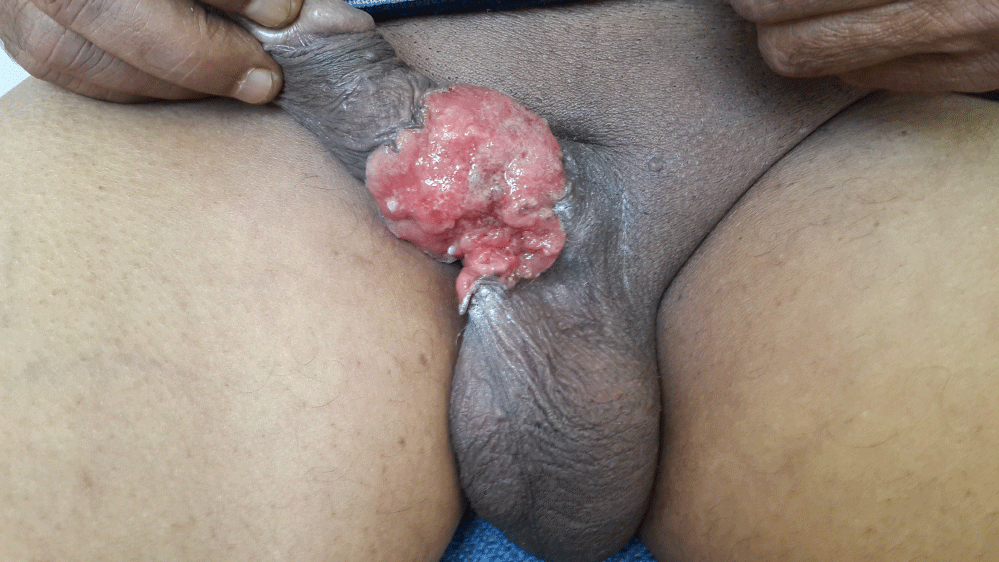
Figure 1: Ulcerated tumor of the penis.
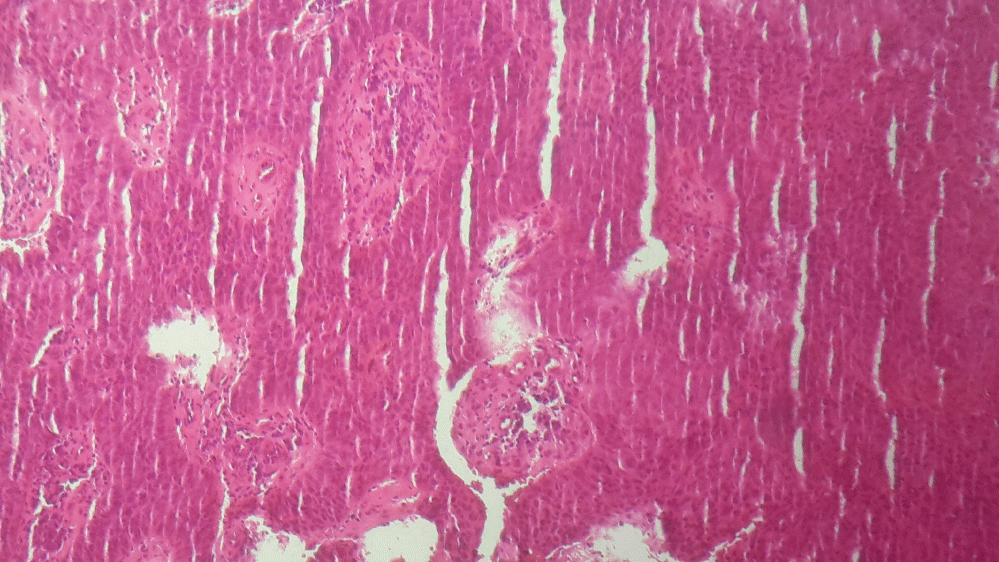
Figure 2: Infiltration of the dermis by carcinomatous proliferation.