Secondary amyloidosis (AA) is a real complication of chronic inflammatory diseases, including chronic inflammatory rheumatism. It is associated with a reserved prognosis justifying the use of all available therapies for the control of inflammation, the sole guarantor of a more favorable evolution. However, it rarely complicates the inflammatory dermatosis including psoriasis and remains far from the minds of young practitioners, hence the interest of recalling, through this clinical case, to watch in time this morbid complication sometimes in silence.
Psoriasis, Rheumatism, Amyloidosis, Biotherapy
Secondary amyloidosis (AA) is a real complication of chronic inflammatory diseases, including chronic inflammatory rheumatism. It is associated with a reserved prognosis justifying the use of all available therapies for the control of inflammation, the sole guarantor of a more favorable evolution. However, it rarely or rarely complicates inflammatory dermatoses including psoriasis and remains far from the mind of the dermatologist, hence the interest to recall, through this clinical case, to watch in time this morbid complication sometimes in silence.
A 45-year-old woman with a history of right breast neoplasia treated 4 years ago and a psoriasis vulgaris that has been evolving for 30 years by relapses and remissions with subsequent onset of arthralgia and deformities of the hands and feet (Figure 1a, Figure 1b and Figure 1c) has consulted for edema of the lower limbs evolving for a month in a context of deterioration of the general condition.
The biological assessment showed a mild leukocytosis, a moderate inflammatory syndrome, a hypoproteinemia at 51 g/l, a hypoalbuminemia at 22 g/l and a proteinuria of 24 hours at 3.27 g/24 h, the renal function was normal, the blood pressure was stable at 120/75 mmHg, cytobacteriological examination of the urine was sterile without hematuria, liver and cardiac outcomes were normal, diagnosis of a pure adult nephrotic syndrome was retained and renal biopsy puncture has been reported to have shown extravascular amyloid deposits in Congo Red (Figure 2).
The clinic and hand radiographs were in favor of psoriatic arthritis (Figure 1c and Figure 1d). The diagnosis of renal amyloidosis secondary to psoriatic arthritis was retained. The patient was put under a nephroprotective treatment, emollients, and topical corticosteroids and addressed in rheumatology consultation for biotherapy (anti-TNF). The evolution was favorable with a decline of 6 months.
The first description of the combination of amyloidosis and psoriatic arthritis was described by Moise, et al. in 1965 and since about thirty observations have been reported [1,2]. The clinical manifestations are related to the renal, digestive and cardiac localizations [3,4].
Although cutaneous involvement during systemic amyloidosis is rare but possible, distinction with primary cutaneous amyloidosis may occur, however, histology remains essential next to the clinic since amyloid deposits are usually present in amyloid cutaneous amyloidosis. Confined to the upper part of the dermis, in secondary systemic amyloidosis the amyloid deposit can be found in deeper areas of the reticular dermis [2].
Immunosuppressive treatments that provide haematological complications, leukaemias and sterility are currently being deterred by biotherapy, including anti-TNF [5]. The prognosis depends on affected organs, associated defects and the response to anti-inflammatory treatments [1,3-5].
Amyloidosis is a frequent complication of chronic inflammatory conditions. In dermatology, certainly rare, but it must be kept in mind especially young patricians. The goal of management is to control inflammation and biotherapies find their place in this indication for their effectiveness and especially their safety.
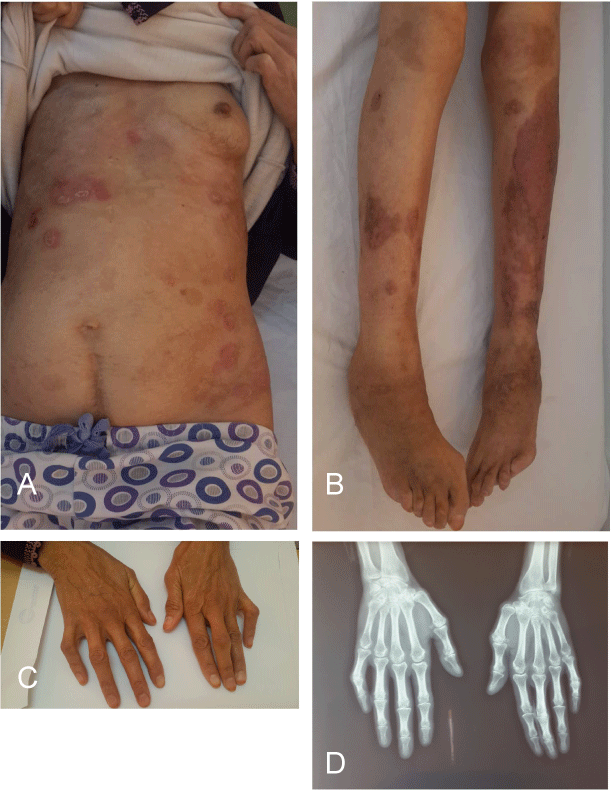
Figure 1(a,b,c,d): Psoriasis lesions with deforming polyarthritis of the hands and feet.
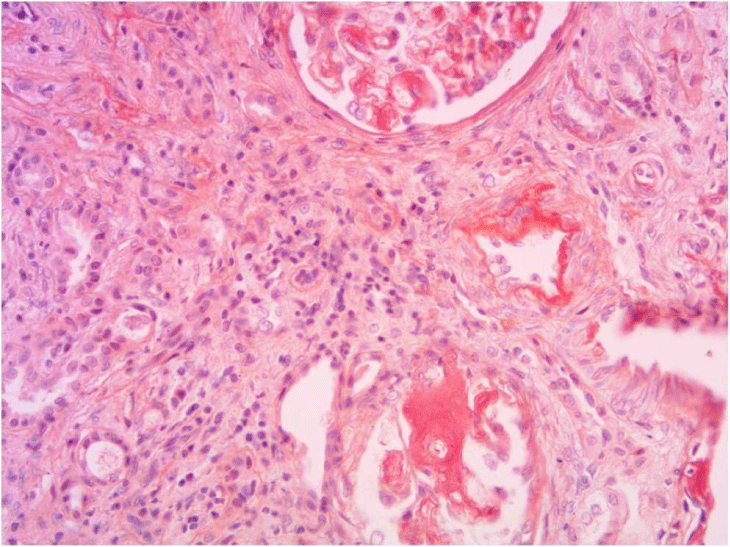
Figure 2: Renal biopsy puncture (Red Congo staining): Extravascular amyloid deposits.