The pseudoxanthoma elasticum (PXE) is a metabolic genetic disorder affecting connective tissue characterized by calcification and fragmentation of elastic fibers, which essentially affects the skin, the eyes and the cardiovascular system. We presented a typical example of a pseudoelastic xanthoma in a patient followed in ophthalmology and cardiology and it was the dermatological lesions that had helped to correct the diagnosis.
Pseudoxanthoma elasticum, Skin, Eyes, Cardiovascular system
The pseudoxanthoma elasticum (PXE), formerly known as Grönblad-Strandberg disease or generalized elastorrexia, is a metabolic genetic disorder affecting connective tissue characterized by calcification and fragmentation of elastic fibers, which essentially affects the skin, the eyes and the cardiovascular system.
A 50-year-old patient, married with three healthy children, followed by ophthalmology for a progressive reduction of visual acuity and in cardiology for precordialgia. Consulted for yellowish papular lesions and a pseudosclerous, retractile and thickened appearance of the skin of the upper half of the body evolving for 20 years (Figure 1a, Figure 1b and Figure 1c). Cutaneous biopsy showed fragmentation of elastic fibers, variously truncal fibers with loss of their branches, which favors elastopathy. Ophthalmologic examination showed a decrease in bilateral and deeper visual acuity on the left with a normal eye fundus and Optical Coherence Tomography (OCT) demonstrating subretinal choroidal involvement (choroidal neovessels) (Figure 2a and Figure 2b). The cardiovascular examination revealed a blood pressure of 150/90 mmHg with a normal ECG holter and echo heart. The diagnosis of pseudoelastic xanthoma with cutaneous, ophthalmological and cardiovascular involvement was retained.
PXE is a genetic disease of autosomal recessive inheritance due to mutations in the ABCC6 gene, located on the short arm of chromosome 16 (16p13.1), and encoding a transmembrane protein that binds ATP. Its prevalence is estimated at 1/25,000 to 1/100,000 births with female predominance, with no clear explanation to date [1-3]. Clinically, there is an important heterogeneity of the disease: Dermatological lesions appear during the second decade and progress in number and severity during adolescence. The rash is made up of yellow papules that can merge into a dermal infiltrate of the neck, folds of the elbows, popliteal hollows and umbilicus, accompanied by an excess of skin in the folds of the groin and armpits [1-3]. Ophthalmological involvement combines retinal pigmentation, drusens, angioid streaks, and neovessels. Macular decompensation around 50 is the most common complication of PXE [1,4]. Cardiovascular involvement leads to cramping and weakness of the lower and/or upper limbs due to early arteriosclerosis of medium sized arteries whose walls are calcified. Transient ischemic attacks and angina pectoris are rare. Gastric haemorrhage complicates 5% of cases, especially during adolescence. A consensus conference proposed major and minor criteria for the diagnosis of PXE. Most pathological manifestations are irreversible, but prophylactic measures can prevent or minimize certain manifestations of the disease, including cardiovascular disease. Excess skin can be removed by plastic surgery when unsightly [1-4].
PXE requires consultation with a geneticist and a multidisciplinary approach to the management of cutaneous lesions, ophthalmological complications, gastrointestinal or cardiovascular complications.
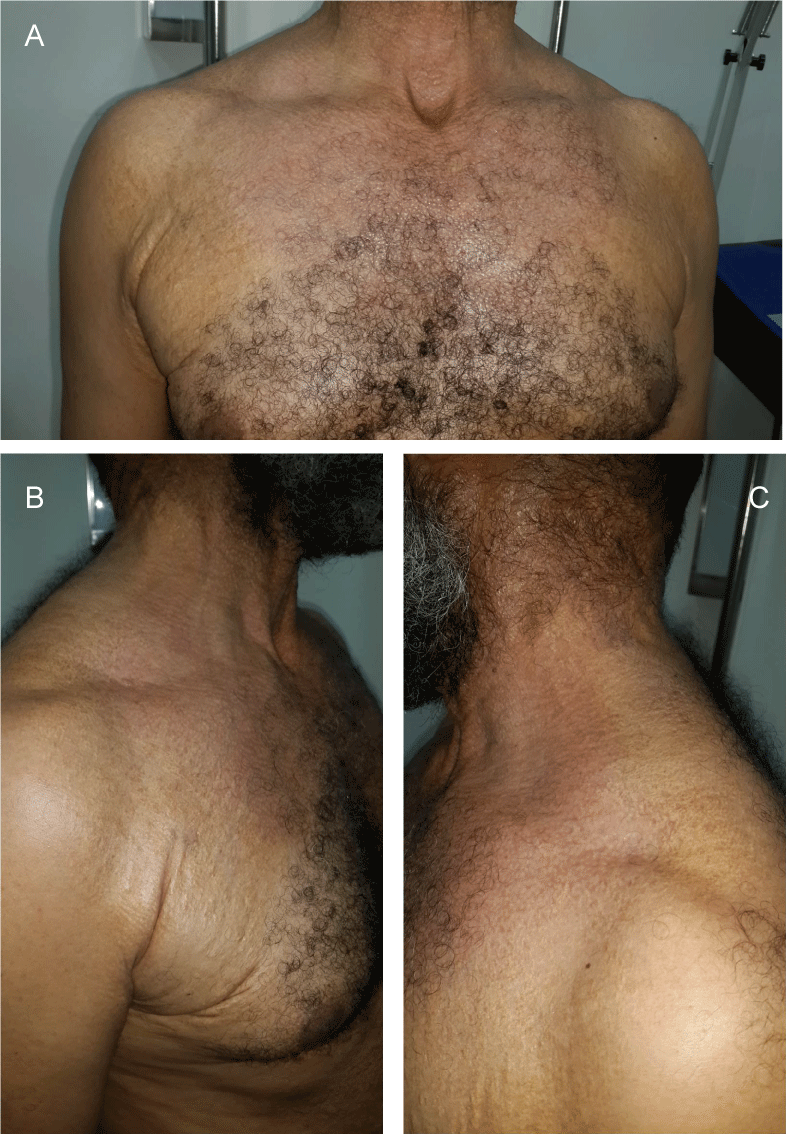
Figure 1(a,b,c): Yellowish papules on the anterior and posterior trunk predominant at the level of the folds with a retractile, thickened and pseudosclerotic aspect of the skin, the inhomogeneous color of the papules at the level of the trunk gives an appearance of poikiloderma.
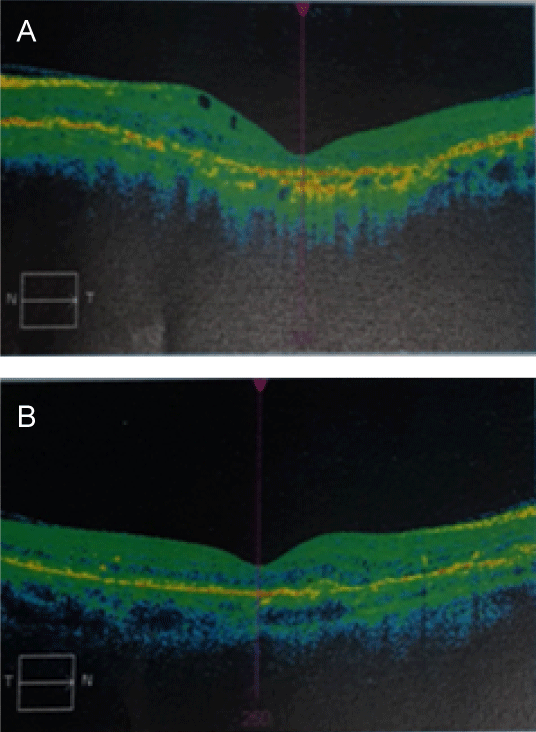
Figure 2(a,b): Optical Coherence Tomography (OCT) showing subretinal choroidal involvement (neo-choroidal vessels).