Parry-Romberg Syndrome (PRS) is an uncommon disorder characterized by a slowly and acquired progressive atrophy involving skin, soft tissue, cartilage, and bony structures. Accompanying atrophies of the other parts of the body are rarely reported. We report an extremely unusual case with PRS associated with contralateral lower extremity atrophy.
Parry romberg syndrome, Facial haematrophy, Extra-cephalic involvement, Lower limb, Scleroderma
Accompanying atrophies of the other parts of the body in the SPR are rarely reported [1]. We report an extremely unusual case with PRS associated with contralateral lower extremity atrophy, complicated by dorso-lumbar scoliosis and inequality of the 2 lower limbs.
A 12-year-old girl, with no significant antecedent, the youngest of a sibling group of three children, whose parents had no consanguineous relationship, consulted for a deformity of the chin progressively evolving for 2 years. The clinical examination revealed a straight hemiatrophy of the chin and the mandibular region without cutaneous in duration and without dental repercussions (Figure 1). It also had a homolateral temporal cicatricial alopecia, a 4 mm achromic macule in the right preauricular (Figure 2), and multiple supple and foldable hyperpigmented plaques on the neck, trunk, flanks and folds. The rest of the somatic examination revealed no abnormalities, other than a discreet scoliotic attitude of the lumbar spine (Figure 3). Antinuclear autoantibodies were positive at 1/80. The serology of borreliosis was negative. The cutaneous biopsy of the achromic macula was in favor of vitiligo. The scan of the facial mass demonstrated a discreet atrophy of the soft straight jaw parts without osseous involvement. The spinal teleradiography was in favor of dorso-lumbar scoliosis by inequality of the 2 lower limbs, with a 14 mm shortening of the left lower limb without apparent bone lesions.
Electroencephalogram, ultrasound of supra-aortic trunks, and cerebral MRI were normal. A systemic treatment with corticosteroids of 0.5 mg/kg/day and Methotrexate at 12.5 mg/week was initiated. The progression was satisfactory, with the end of the progression of atrophy, within a follow-up of 18 months. A facial lipostructure for morphological restoration is expected after stopping growth.
Parry-Romberg Syndrome (PRS), also known as progressive facial hemiatrophy, is a rare, sporadic condition frequently seen in women [2]. It appears towards the first or second decade, to gradually evolve for years (2-10 years) before stabilizing [2,3]. Clinically, it is characterized by progressive hemifacial atrophy, skin involvement, adipose tissue, muscles and sometimes adjacent bone tissue, where usually involving dermatomes of one or more branches of the fifth cranial nerve (V) [1], with a higher frequency of reaching the left side [2]. However, other sites have also been documented, including the neck, shoulders, chest, and lower limbs [4]. Our patient had a right hemifacial lesion (V3 territory) with an extension of the atrophy towards the contralateral lower limb, which was rarely previously described in the literature [1,5,6]. Treatment of SPR can be difficult. The main objective is to stop the progression of atrophy. Once the disease is stabilized, other aesthetic therapies can be used to repair tissue damage and decrease facial asymmetry [2,3]. The etiology of the SPR is still poorly understood and controversial. Some authors believe that this syndrome is a form of scleroderma, while others think it is a different entity [1]. However, many theories of the pathogenic mechanism explaining amyotrophy have been raised: genetic predisposition, trauma, infectious disorders especially in Borrelia burgdorferi, sympathetic dysfunction, vascular abnormalities and immunological disorder theory [3]. The latter is strongly referred to in our case, in front of the association of the SPR to the vitiligo, the presence of anti-nuclear antibodies, and the clinical improvement under immunosuppressors.
PRS may manifest many different clinical findings, but lower extremity involvement is extremely rare. Our case is unique in 2 aspects: The first is the isolated contralateral lower extremity involvement together with hemifacial atrophy (without affecting any part of the body) and the second is the remarkable shortness in the length of the effected extremity.
The authors don't declare any conflicts of interest.
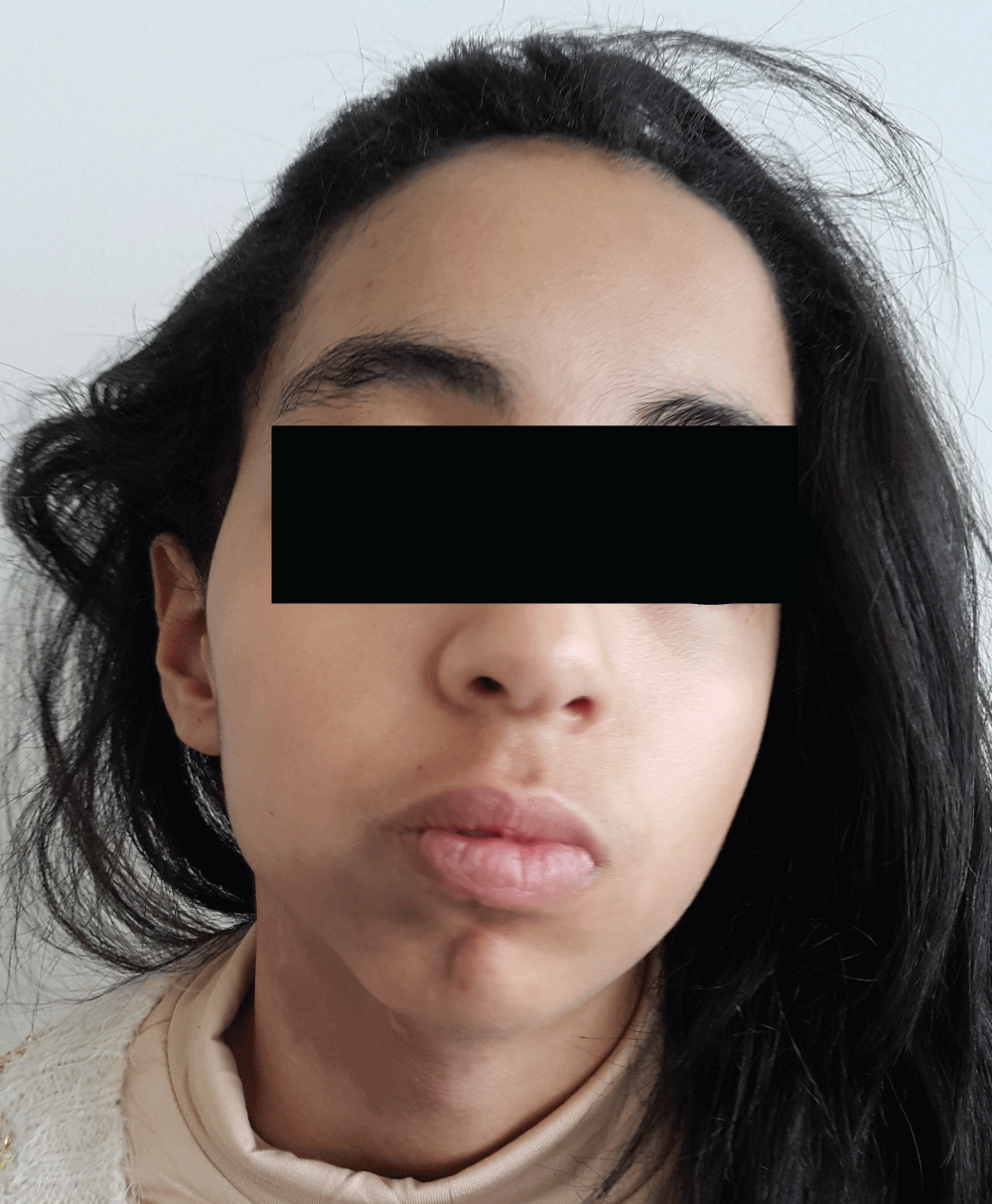
Figure 1: Right hemifacial atrophy (interesting the territory of mandibular branches of the fifth cranial nerve).
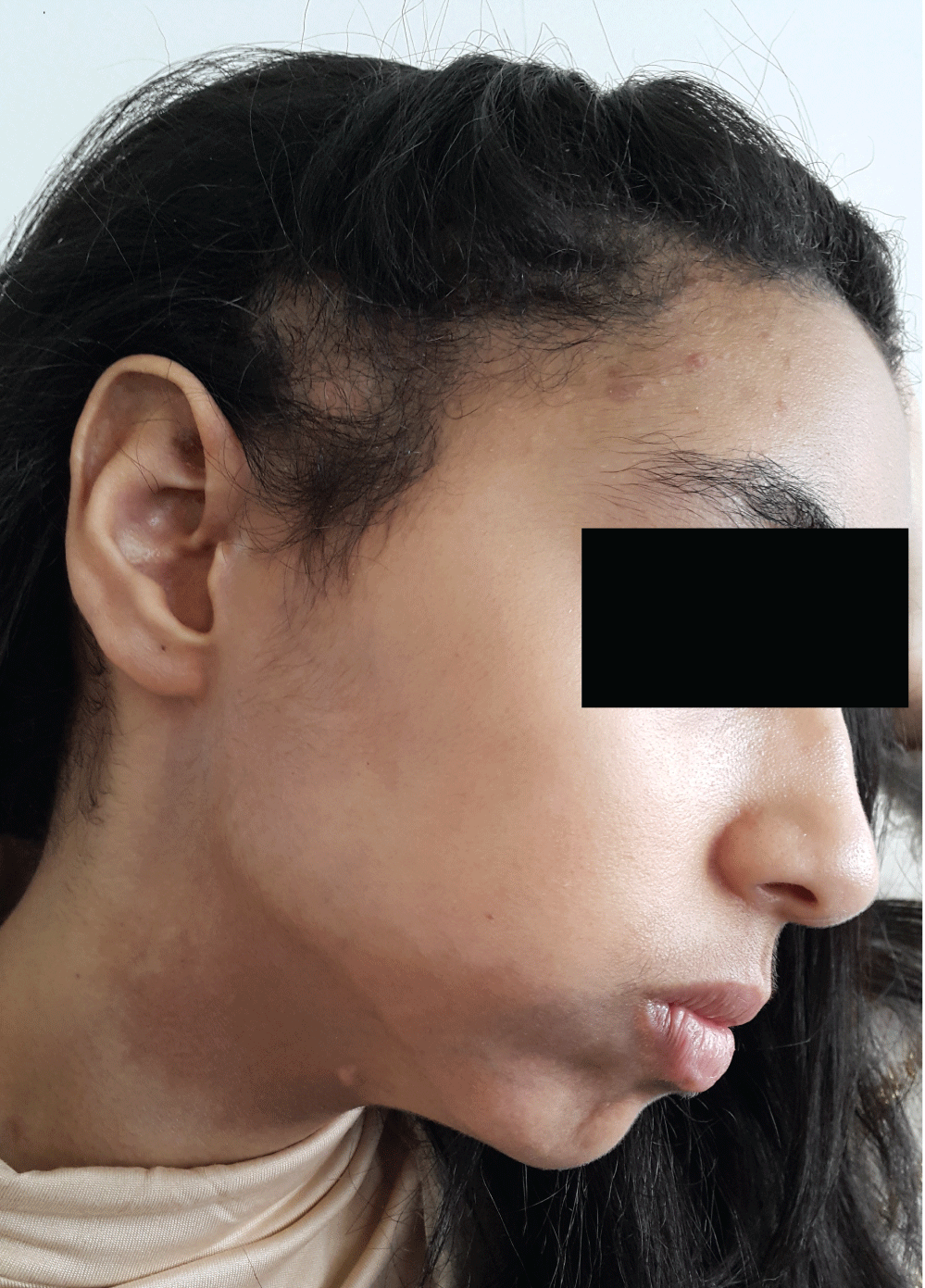
Figure 2: Right temporal scar alopecia, with a 4 mm achromic macula on the right preauricular region.
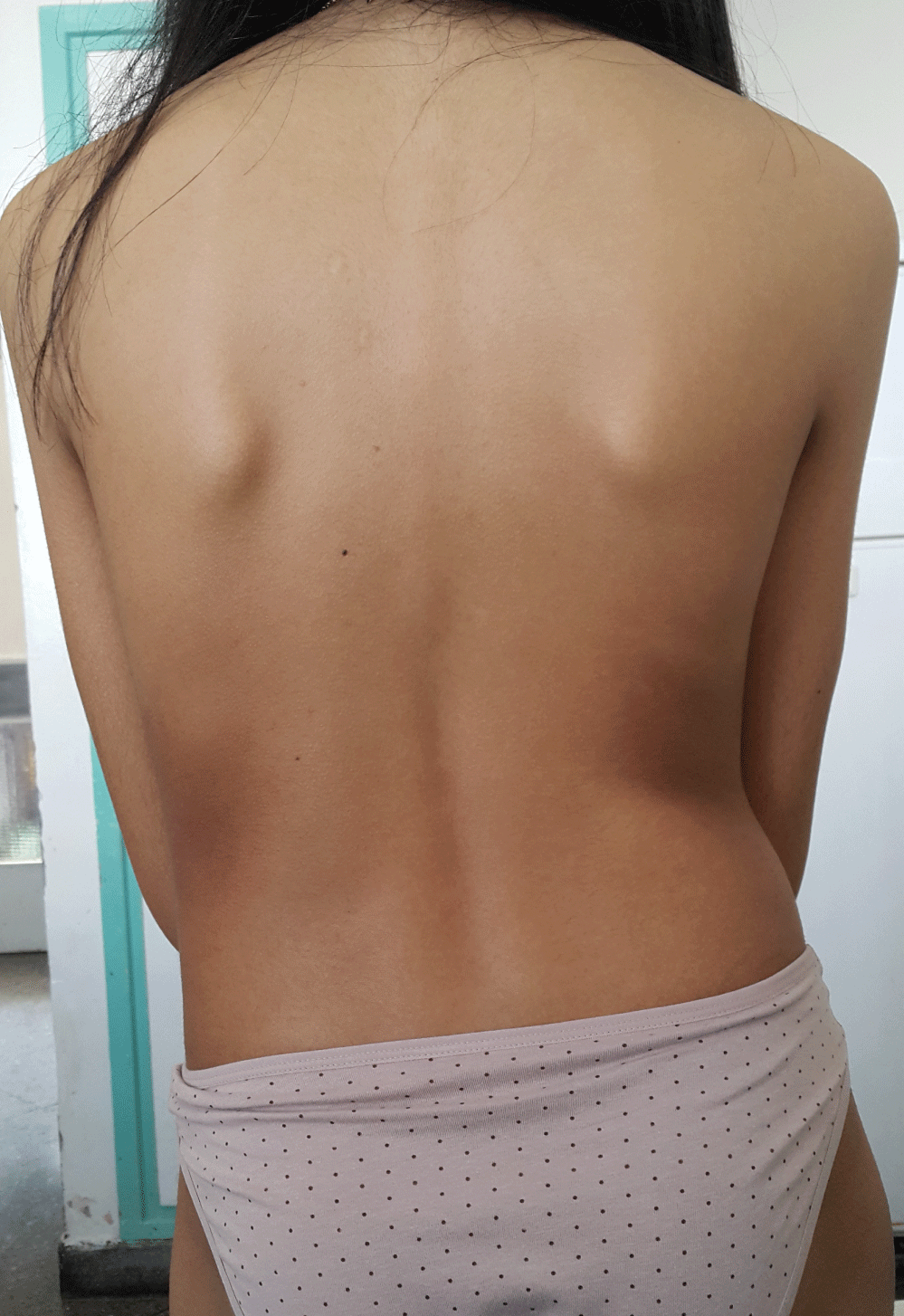
Figure 3: Scholastic attitude of the lumbar spine.