Calcific Uremic Arteriolopathy (CUA) or Calciphylaxis, is a severe morbid and life-threatening condition 1. Ischemic subcutaneous necrosis with vulnerable skin ulcerations are some of the characteristics of this rare but global spread disease.
Despite the diagnosis of CUA is clinical, histological confirmation remains the gold standard for definitive diagnosis. Biopsies describe small arteries and arteriolar medial calcification, intimal hyperplasia, inflammation with endovascular fibrosis and microthrombi [1].
Although the process of vascular calcification was thought to be a passive deposition of calcium-phosphate crystals, the present knowledge suggests cellular activity with differentiation of vascular smooth muscle cells (VSMCs) into chondrocyte as well as osteoblast-like cellular phenotypes and deficiencies in calcification inhibitors [2].
Known as vascular calcification important inhibitors there are: Fetuin A/α2-Heremans Schmid glycoprotein (AHSG), produced by the liver but acting as a systemic inhibitor of hydoxyapatite synthesis; the Matrix Gla Protein (MGP) which binds to insoluble calcium salts preventing hydroxyapatite crystals growth and, by blocking osteo-inductive properties of bone morphogenic protein-2, inhibits VSMCs from differentiating into osteoblast-like phenotypes. Finally the Growth Arrest Specific gene 6 (Gas 6) which has a protective role against vascular injury [3].
MGP and Gas 6 are both vitamin-K dependents proteins, so vitamin K antagonists’ intake, such as warfarin, may compromise these calcification inhibitors activation. Vitamin K2, one of the two types of vitamin K, is the most important for the peripheral gamma-carboxylation of MGP and Gas-6 [4].
Supporting warfarin as a precipitating factor for CUA development we report a case of a 65-year-old male gender patient with End-stage Renal Disease under hemodialysis for 6 years and a one-year mechanic aortic valve, taking warfarin, presenting typical skin lesions (Figure 1) and marked vascular calcifications (Figure 2). CUA was admitted as a probable diagnosis. Besides the positive anamnesis, biopsy was performed for confirmation. Treatment was established with relatively good outcome.
At two and half years of follow-¬up, the patient is alive. Although, he presents with recurrent arterial stenoses (Figure 3) which can be interpreted due to the process above described.
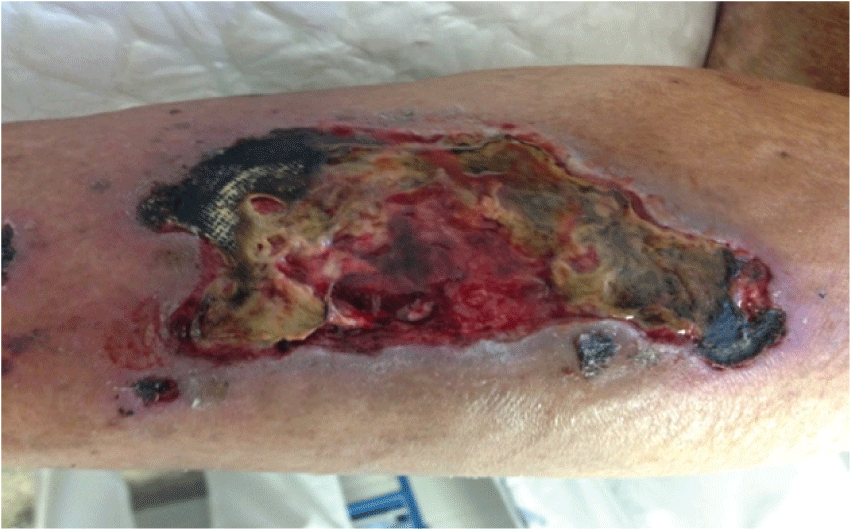
Figure 1: Right leg.
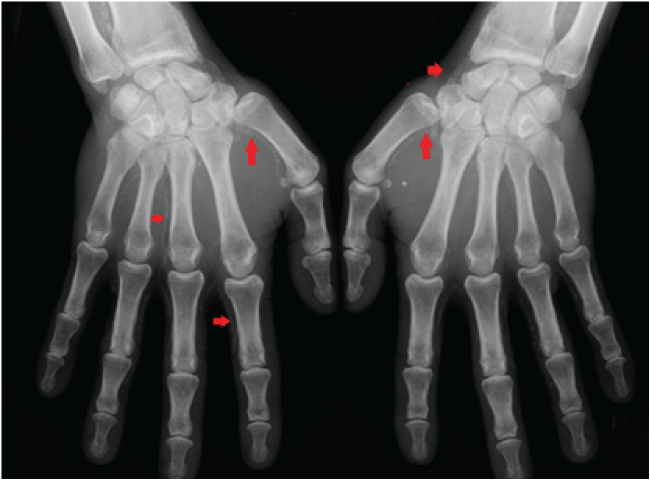
Figure 2: Hands with vascular calcifications.
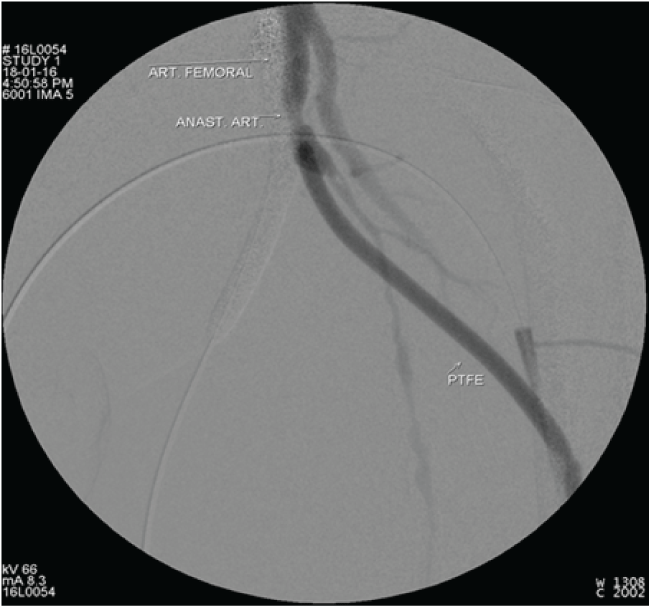
Figure 3: Arterial stenosis.