A 53-year-old man admitted to our emergency service with symptoms of intermittent vomiting and headache for a week. In the hospital the patient swiftly deteriorated to coma. Computed Tomography (CT) and Magnetic Resonance Imaging (MRI) of the brain were performed. CT imaging showed a large intra-axial cystic tumour with solid component in the right frontal lobe with diffuse perilesional vasogenic edema. MRI scan showed a large frontal cystic mass with mass effect upon the right ventricle and leftward midline shift approximately 12 mm. In contrast MRI imaging, heterogeneous enhancement in the solid component of tumour was noted. He underwent biopsy of the lesion and verified the diagnosis of Primitive Neuroectodermal Tumor (PNET) (Figure 1).
PNET is malignant, embryoblastic small cell neoplasm of childhood thought to results from primitive and undifferentiated neuroepithelial cells. PNET is extremely rare in adults. PNET may appears any location. The supratentorial PNET is most commonly in the temporo-parietal region. On MRI imaging typically occurs a large, lobulated, sharp-demarcated mass with heterogeneous signal T1 and T2 weighted images. It may have cystic, hemorrhagic and calcific component. The differential diagnozis of supratentorial PNET should involve glioblastoma multiforme, anaplastic oligodendroglioma, gangliocytoma and metastasis (Figure 2) [1-4]
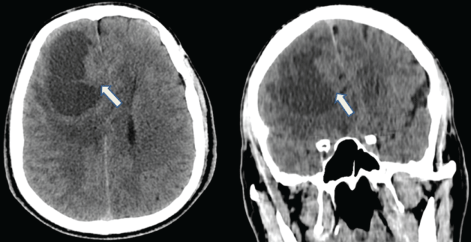
Figure 1: Computed Tomography (CT) scans: Axial and koronal non-enhanced CT images showing a large, well demarcated cystic mass with a solid component (arrow) in the right frontal lobe.
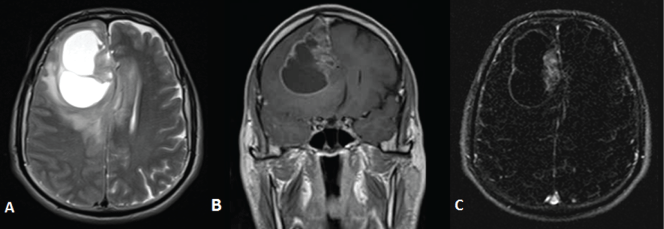
Figure 2: Magnetic Resonance Image (MRI):
A) Axial non-contrast T2 weighted images showing a large heterogeneous cystic mass with
severe perilesional edema and compressing the ipsilateral lateral ventricle;
B) Coronal post-contrast T1 weighted;
C) Axial subtraction images showing enhancement of solid component.