Digestive tract heamorrhage, Blind pouch syndrome, CT, Treatment
A 60-year-man was admitted to our hospital with the complaints of intermittent hematemasis for 6 months. The patients underwent side-to-side enteroanastomosis because of intestinal tuberculosis 30 years prior. Except for the iron deficiency anemia and decreases of the hemoglobin values down to 78 g/L, all the other laboratory values were within the normal range. Further investigation of the anemia included repeated colonoscopies and gastroscopies which didn't disclose a possible source of bleeding. Abdominal CT scan demonstrated multiple oval stones within regional blind end of small intestine and retained fluid was also noted in the sacculation (Figure 1, Figure 2 and Figure 3). Operation revealed an inflammed, oedematous, mesenteric sacculation in the blind end of intestinal afferent limb, which was located approximately 90 cm from the ileocecal valve. The involved segmental resection was completed with end-to-end stapled anastomosis. Surgery confirmed to be blind pouch syndrome and cut surface of the resected specimen showed mucosal ulcer and multiple stones in the lumen (Figure 4). The patient recovered well without any complications on the follow-up of one year.
The development of a blind pouch is related to the type of enteric anastomosis, commonly encountered in the previous surgical procedure with side-to-side anastomosis. According to Cannon and Murphy, this method of anastomosis may interfere with normal peristalsis as a result of interruption of the circular muscle fibers. Propulsion of the normal peristaltic contractions is discrupted, and the two opposed loops do not act properly to propel food in an antegrade fashion. Therefore, food may accumulate in the blind end of the intestine, gradually causing dilatation and eventual blind pouch formation. The incidence of blind pouch could not be elicited from a literature search. The blind pouch syndrome does not occur after end-to-end anastomosis. Presenting symptoms may include abdominal pain, anemia, weight loss, diarrhea or intermittent constipation, and gastrointestinal bleeding. There can be a delay in the onset of symptoms, as manifested in our patient. Multiple enteroliths and mucosal ulcer within the blind pouch simultaneously is rarely reported. Once the blind pouch syndrome is defined, segmental intestinal resection and end-to-end anastomosis, as was done in our patient, will lead to favorable outcomes. Although saccular dilatation containing calcification may be mimicked by other entities within the small bowel, the pertinent surgical history and the radiographic features allow blind pouch syndrome to be differentiated from other entities, such as Mechel's diverticulum, ileal dysgenesis, or acquired diverticulum.
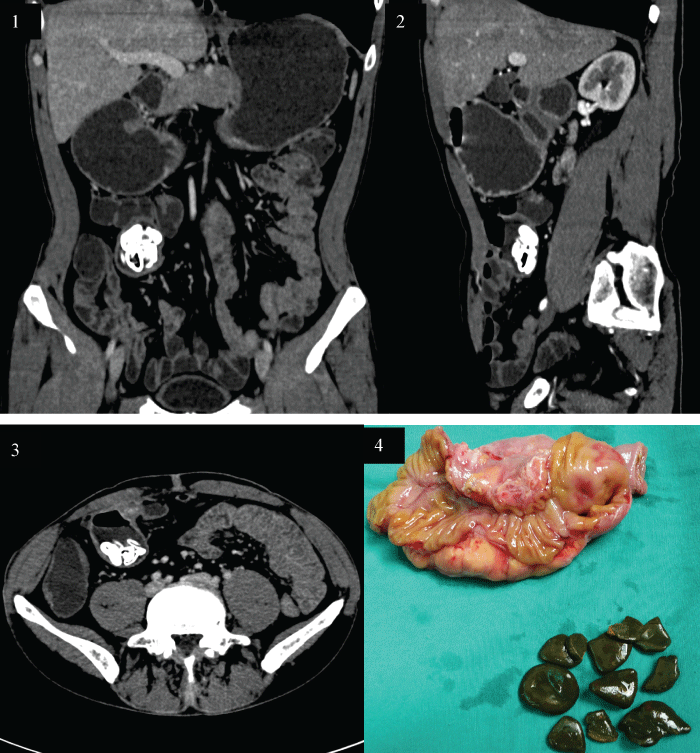
Figure 1: