Cerebral palsy; Hip dislocation; Hip stress; Reimers index; Wiberg angle; Hip biomechanics; Resultant hip force
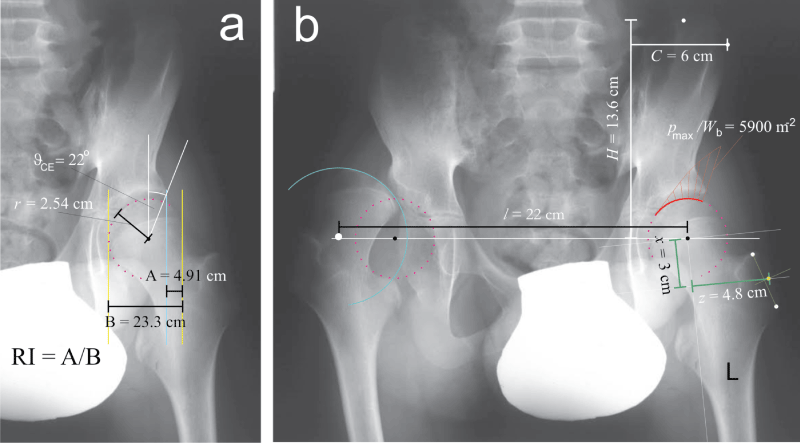
Hip dislocation is a relatively common complication in cerebral palsy [1]. Surgical intervention in the early ph ase is the preferred choice of treatment which however requires following the migration of femoral head with respect to acetabulum in hips at risk [1]. Standard anteroposterior radiograms are used to assess the Reimers index (RI) which expresses the percent of epiphyseal ossific nucleus located outside the acetabular roof (Figure 1a); the hip is considered displaced if RI is greater than 0.3 [1]. While RI reflects the consequences, a biomechanical parameter - contact hip stress - may also elucidate the mechanism of hip dislocation. According to the mathematical model within the HIPSTRESS method, unfavorable stress distribution in the one-legged stance is characterized by a monotonous decrease of contact hip stress in the medial direction and by small functional angle of the weight bearing area. This is expressed by a positive hip stress gradient index (Gp) [2]. HIPSTRESS method requires as an input the geometrical parameters of pelvis and hips which can likewise be obtained from standard anteroposterior rentgenograms (Figure 1).
A 12 year old boy with a severe spastic diplegic cerebral palsy presented with a complaint of severe pain in his right hip. A radiogram showed dislocation of the right hip with moderate degenerative changes; the left hip appeared to be normal (RI was 21%) (Figure 1a). However, calculation of hip stress distribution with the HIPSTRESS model showed that the hip stress gradient index (Gp) in the left hip was positive. Unfavorable distribution of contact hip stress indicated a risk for dislocation in the one-legged stance, although RI did not show excessive migration of the femoral head. As the hip geometry before dislocation of the right hip was considered symmetric, the fact that the right hip underwent dislocation supports the indication that the geometry of these hips presents a risk for dislocation when standing on the leg. Assessment of hip stress can therefore be of help in planning the treatment. After the surgical treatment of the right hip the patient at age 20 uses a wheelchair but also stands and walks shorter distances (in the room) with support.
The geometrical parameters used for calculation of the hip stress distribution according to the HIPSTRESS method [2] were: interhip distance (l), pelvic height (H), pelvic width (C), position of the effective muscle attachment point on the greater trochanter (x and z) (Figure 1b), radius of the femoral head (r) and centre-edge angle (ϑCE) (Figure 1a), and the biomechanical parameters of the patient's left hip were: peak hip stress normalized to body weight pmax/Wb = 5907 m-2, position of the stress pole ( Θ = 38°) and normalized index of stress gradient Gp/Wb = 39400 m-3.