Journal of Family Medicine and Disease Prevention
Social Ecology and Diabetes Self-Management among Pacific Islanders in Arkansas
Pearl Anna McElfish1*, Ramey Moore2, David Woodring1, Rachel S. Purvis1, Gregory G. Maskarinec3, Williamina Ioanna Bing1, Jonell Hudson4, Peter O. Kohler5 and Peter A. Goulden6
1Office of Community Health and Research, University of Arkansas for Medical Sciences Northwest, USA
2Department of Anthropology, University of Arkansas, USA
3Family Medicine and Community Health, University of Hawai'i at Manoa, USA
4Pharmacy Practice, University of Arkansas for Medical Sciences Northwest, USA
5University of Arkansas for Medical Sciences Northwest, USA
6College of Medicine, University of Arkansas for Medical Sciences, USA
*Corresponding author: Pearl Anna McElfish, PhD, MBA, Assistant Professor, College of Medicine, Director of the Office of Community Health and Research, University of Arkansas for Medical Sciences Northwest, 1125 North College Ave, Fayetteville, AR 72703, USA, Tel: 479-713-8680, E-mail: pamcelfish@uams.edu
J Fam Med Dis Prev, JFMDP-2-026, (Volume 2, Issue 1), Research Article ; ISSN: 2469-5793
Received: February 02, 2016 | Accepted: March 10, 2016 | Published: March 14, 2016
Citation: McElfish PA, Moore R, Woodring D, Purvis RS, Maskarinec GG, et al. (2016) Social Ecology and Diabetes Self-Management among Pacific Islanders in Arkansas. J Fam Med Dis Prev 2:026. 10.23937/2469-5793/1510026
Copyright: © 2016 McElfish PA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Chronic diseases disproportionately affect ethnic and racial minorities. Pacific Islanders, including the Marshallese, experience some of the highest documented rates of type 2 diabetes. Northwest Arkansas is home to the largest population of Marshallese outside of the Republic of the Marshall Islands, and many migrants are employed by the local poultry industry. This migrant population continues to increase because of climate change, limited health care and educational infrastructure in the Marshall Islands, and the ongoing health effects of US nuclear testing. The US nuclear weapons testing program had extensive social, economic, and ecological consequences for the Marshallese and many of the health disparities they face are related to the nuclear fallout. Beginning in 2013, researchers using a community-based participatory (CBPR) approach began working with the local Marshallese community to address diabetes through the development and implementation of culturally appropriate diabetes self-management education in a family setting. Preliminary research captured numerous and significant environmental barriers that constrain self-management behaviors. At the request of our CBPR stakeholders, researchers have documented the ecological barriers faced by the Marshallese living in Arkansas through a series of qualitative research projects. Using the Social Ecological Model as a framework, this research provides an analysis of Marshallese health that expands the traditional diabetes self-management perspective. Participants identified barriers at the organizational, community, and policy levels that constrain their efforts to achieve diabetes self-management. We offer practice and policy recommendations to address barriers at the community, organizational, and policy level.
Keywords
Health disparities, Community-based participatory research, Pacific Islanders, Minority health, Diabetes type 2
Introduction
Chronic diseases, such as heart disease, overweight/obesity, and type 2 diabetes, disproportionately affect ethnic and racial minorities [1-3]. Pacific Islanders, including Marshallese from the Republic of the Marshall Islands, experience some of the highest documented rates of type 2 diabetes-ranging from 25% to 50% for Marshallese adults-compared to the total US population (8.6%) [4-6].
Springdale, Arkansas is home to the largest population of Marshallese migrants in the continental United States, and migration from the Republic of the Marshall Islands to the United States continues to grow due to climate change, limited health care and education infrastructure, and ongoing health effects from US nuclear testing in the Republic of the Marshall Islands [7,8]. The poultry industry in northwest Arkansas is the primary employer of Marshallese migrants, and access to poultry industry jobs encourages Marshallese migration to the area [9]. In order to explain the context of the diabetes epidemic in the Marshallese community, it is important to understand the historical relationship between the Republic of the Marshall Islands and the United States.
Between 1946 and 1958, the US military detonated 67 fission and thermonuclear devices on Marshall Island atolls, which were equivalent to 7,200 Hiroshima-sized bombs. The largest of these detonations-a single 15 megaton hydrogen bomb over 1,000 times the power of the Hiroshima bomb-occurred on Bikini Atoll, exposing Marshallese to widespread radioactive fallout [10,11]. The nuclear weapons testing program had extensive social, economic, and ecological consequences for the Marshallese. There are many health disparities related to the nuclear fallout, including disruptions in the native food supply and lifestyle [10,12]. After the nuclear testing, the United States sent high-calorie, low-nutrient, processed foods to the Republic of the Marshall Islands as food aid [13]. US food aid transformed the Marshallese diet and many Marshallese still rely on and prefer these unhealthy foods. In addition to nuclear testing, a growing body of literature suggests the prolonged and rising rates of obesity and diabetes among Pacific Islander populations are exacerbated by the adoption of Western lifestyles, and a lack of access to health care and to health education [14,15].
The United States had trusteeship of the Marshall Islands beginning in 1947, and in 1986, the Republic of the Marshall Islands became an independent nation through the signing of a Compact of Free Association (COFA). Under the COFA agreement, Marshallese from the Republic of the Marshall Islands are allowed to freely enter and work in the United States; however, their COFA migrant status limits their access to federal assistance programs, such as Medicaid.
The United States continues to derive numerous benefits from the COFA, including the use of 11 of the 97 islands of Kwajalein Atoll for military activity, which allows the US military to maintain control of approximately two million square miles of the Pacific. While the US military continues to benefit from the COFA, Marshallese migrants struggle to access basic health care services both in the United States and in the Republic of the Marshall Islands.
In 2013, researchers from the University of Arkansas for Medical Sciences Northwest campus began working with the Marshallese community using a community-based participatory research (CBPR) approach to address the health disparities affecting the Marshallese community. Marshallese stakeholders identified diabetes as a primary concern, and the lead researcher began working with community stakeholders to understand the epidemic of type 2 diabetes in the community [16]. In 2014, the lead researcher worked with CBPR stakeholders to adapt and implement culturally appropriate diabetes self-management education [14,17,18]. While the self-management study continues, preliminary research revealed numerous and significant environmental barriers that constrain self-management behaviors. CBPR stakeholders asked that ecological barriers be documented and discussed. At the request of CBPR stakeholders, this work highlights the environmental barriers faced by Marshallese living in Arkansas.
Diabetes self-management is an evidenced-based method for addressing type 2 diabetes that focuses on patient health behaviors [19]. While diabetes self-management has shown improvement in health outcomes, there is evidence that it is not accessible and effective for all populations [20,21]. Furthermore, diabetes self-management may over-emphasize personal responsibility, giving limited consideration to the community, organizational, and policy environments that also affect health outcomes [22]. Critics of the self-management and personal responsibility paradigm argue, "an overriding emphasis on personal responsibility blames the victim, by ignoring the social context in which the individual decision making and health-related action takes place [23]".
Theoretical Framework
Diabetes self-management requires access to a variety of resources beyond individual agency, and the Social Ecological Model considers the environmental factors that constrain or facilitate access to organizational, community, and policy resources [23]. The Social Ecological Model brings together multiple fields of research and provides a framework for examining participants' health in relationship with their natural and social environments. This multi-dimensional focus allows researchers to examine individual-environment interactions that affect access and use of resources and services [24]. Since effective self-management is contingent on both individual and environmental resources, systematic patterns of inequality may emerge at environmental levels.
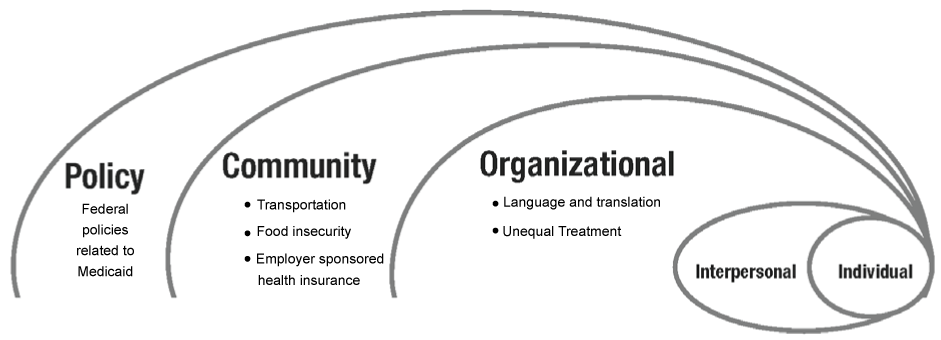
While much research has focused on individual-level barriers to diabetes self-management, an ecological perspective integrates both individual and environmental factors to examine health outcomes of individuals. Ecological models delineate the reciprocal relationships between individual/interpersonal factors and broader organizational, community, and policy determinants of health behaviors [22]. In contrast to perspectives that emphasize personal responsibility for disease self-management, this body of literature highlights the confluence of multiple environmental dimensions of health across the lifespan [24-26]. Examining individual and environmental determinants of health behaviors and outcomes allows for complex comprehension of the social and cultural contexts and situational factors that can affect efforts to manage one's health [24] (Figure 1).
Methods
Over a period of two and a half years, the CBPR team conducted several qualitative pilot projects to address diabetes disparities with research questions focused on: general beliefs about health and use of health care services, health beliefs regarding diabetes self-management behavior, and perceptions of family-model diabetes self-management (Table 1).
Twelve focus groups were conducted with Marshallese participants (n = 69). All focus group participants were recruited through CBPR partners: Arkansas Coalition of Marshallese, Gaps in Services to Marshallese Task Force, Marshallese pastors, and the local Republic of the Marshall Islands Consulate in Springdale, Arkansas. The research team worked with CBPR stakeholders to create culturally appropriate study announcements, and community partners provided potential participants with information about the research. All participants provided consent prior to data collection, were age 18 or older, and self-reported as Marshallese. A Marshallese community co-investigator was available at each focus group to provide translation if needed. Focus groups ranged from four to twelve participants. A semi-structured interview guide created by the CBPR team included open-ended questions that allowed participants to speak in-depth about their health beliefs and experiences. All focus groups were conducted in private community rooms to ensure participant confidentiality. The duration of each focus group was approximately one hour. Focus groups were recorded and transcribed verbatim. Participants received a $25 gift card as compensation for their time. Each of the study's procedures were reviewed and approved by the University of Arkansas for Medical Sciences Institutional Review Board (Table 1).
![]()
Table 1: Studies from which the data was drawn
View Table 1
Each of these projects focused on gathering data to answer study-specific research questions and concentrated on personal/interpersonal beliefs, experiences, and behavior. While research questions centered on describing general beliefs about health, with a focus on individual and interpersonal elements, there were a number of emergent themes that participants discussed during the course of the research projects described above that pointed to larger organizational, community, and policy barriers to health care. As a part of our commitment to a CBPR paradigm, a collective decision was made by the CBPR researchers and stakeholders to ensure participants' voices were heard regarding these environmental barriers.
Emergent themes were coded based upon the environmental barriers identified by participants. These emergent themes were organized into priori groups according to the Social Ecological Model's levels: organizational, community, and policy. A codebook was developed with the priori codes and emergent codes (Table 2).
![]()
Table 2: Themes and sub-themes.
View Table 2
Coding was conducted by four qualitative researchers with two primary coders and two confirmation coders. Researchers collaborated through the course of data analysis to ensure inter-coder reliability. Marshallese community co-investigators provided feedback throughout the research and writing process. The Marshallese community co-investigators' involvement helps reduce the risk of misinterpretation because of language barriers or cultural nuances in meaning, and helps ensure findings and discussion accurately reflected what Marshallese participants stated.
Results
The results are presented using the three environmental levels of the Social Ecological Model as an organizing template. The environmental levels are organizational, community, and policy. First, Marshallese informants report barriers to diabetes self-management at local health care organizations including issues with: (a) language and translation, and (b) unequal treatment. Second, participants report three barriers to diabetes self-management at the community level including: (a) transportation, (b) food insecurity, and (c) employment and employer sponsored health insurance. Finally, participants discuss barriers at the policy level, which is the macro-level of the social ecology of health. Participants identify federal policies related to Medicaid as a barrier to self-management of diabetes.
Organizational
Language and translation: Participants highlight a lack of translated materials (e.g. care instructions, patient forms, and information on medicines) as well as a lack of organizations that hire Marshallese translators. Marshallese participants discuss that "the language barrier is also a barrier to better health." Participants state that successful diabetes education for the community would include educational materials "translated into (the) Marshallese language."
Language barriers and the lack of translators affect Marshallese decisions about whether or not to seek care. Participants describe that when Marshallese patients have a doctor's appointment "they won't show up because of (the) language barrier." For the Marshallese, knowledge that they will likely not be provided care with a translator greatly reduces the choices that they have when seeking care, even in instances where they may be adequately covered by insurance.
Another participant notes that these issues go beyond merely providing translation of language, since many Marshallese often need additional translation of medical concepts. One participant states that "every time the receptionist would do the intake for the new patients, she would ask them, 'Do you have PCP (Primary Care Physician)?' They're like they don't know what PCP is, cause we don't have PCPs in our island...they wouldn't answer, or they just look at her."
Unequal treatment: Participants share concerns about the way that uninsured and underinsured Marshallese patients are treated by area doctors, clinics, and hospitals. Participants speak about the difficulties of receiving care with inadequate levels of insurance coverage. To be clear, Marshallese patients state that they are not waiting to seek medical care until they are at a crisis point, but that organizational policies limit their options. As one of the participants notes, "[A recent study] conclusion is that the Marshallese wait until they are very sick and seek medical attention...that is not true...we go and seek medical attention, (but the doctors and hospitals) don't give us attention".
Marshallese participants also discuss their experiences with unequal treatment at doctor's offices, clinics, and hospitals, which participants believe is based on their insurance status or Marshallese ethnicity. As one participant states:
If they don't have insurance, they go and see the doctor, [the doctor] always keep them until the last, because
they don't have the insurance. They wait there. They are very sick, and they've been waiting for them
(the doctor/doctor office staff) to call their names. Finally, they have to go to another place, because they
are really sick but they (the doctors) don't really take care of them.
For some patients, this may result in a last resort visit to the emergency room at a local hospital, where they have access to some form of care. However, participants report that even hospital visits can be fraught with obstructions stemming from insurance status. "It seems like some of the hospitals, they only take those that have insurance, not the ones that didn't have," notes one participant.
It is not just uninsured Marshallese that experience barriers to accessing health care. For a number of participants, even when they qualify for Medicaid, because they are US citizens, participants note that there are still issues with their care. One participant explains that after changing from private insurance to Medicaid their "(previous doctor) doesn't take anyone with Medicaid. A lot of doctors here in the United States are not taking Medicaid patients. They will take the people with good insurance. I mean, you go in there and present your Medicaid card, well, find someone else."
Community
Transportation: Public transportation is limited in northwest Arkansas, and participants report that transportation issues can make every aspect of diabetes self-management more difficult for Marshallese households. Many participants explain that it is necessary to have a car in order to meet basic needs, including access to employment, health care services, diabetes education, and healthy food. Importantly, access to a car is not the only requirement. Currently, the drivers' license test and testing materials are not available in Marshallese, and because many Marshallese do not read English well, they cannot pass the drivers' licensing exam. Without a driver's license, they have limited access to the doctor, work, pharmacy, and grocery store, and face deportation if they drive without a license. Participants note that:
As you... know that most of the Marshallese are being deported because they keep driving without license
because: one, they really want to bring their family needs (food, doctor, employment) and two, pick their children
from school. There may be one person in the household who knows how to drive but he or she does not
have a license but it is hard to ask somebody to drive for you to pick your child from school and also to get your
needs.
Food insecurity: A lack of access to adequate and healthy food is another important theme that participants identify as creating barriers to health and to diabetes self-management. Participants frequently say that "when (we) are educated... some of (us) will try to change what (we) eat, but the problem too is the cost of vegetables." Participants state that the affordability and ability to store and prepare healthy foods is an issue that cannot be addressed merely through diabetes education and self-management practices, which often assume that dietary choices are unfettered by cost and other constraints. "At the beginning of the week, I have healthy food, but after a few days, I don't have money to buy vegetables and meat and fruit. Then it is just Ramen". While traditional self-management programs recommend switching from sugar to the use of products, such as Splenda, there are issues where "most Marshallese . . . make little more than minimum wage and if you are going to buy Splenda compared to like regular sugar, the regular sugar is cheaper than (other options)," according to participants.
Employment and employer sponsored health insurance: Participants explain that their access to health care is constrained by the kinds of employment that the community can access. Participants state that most of the Marshallese are in jobs that pay low wages and are part-time, or have varying weekly hours, and this means they have to make the choice between everyday necessities, like food, shelter, and insurance premiums.
Even when employers offer health insurance plans, participants find these plans to be too costly for many families, even when these plans were partially subsidized by an employer. "The reason why most Marshallese don't buy in (to employer insurance plans) at work is because they can't afford it."
The prevalence of chronic illnesses in the community is confounded by issues with employer sponsored insurance. Marshallese focus group participants state that
(Marshallese people) don't have any insurance because they don't work for some reason...They disqualified
to be employed (due to health). That's not when you go to the employer, they will ask easily check. Then
(employers) will say, "Oh, you are sick. You are sick, you cannot do the job." That's why most of the Marshallese
been laid off from work, because of their ill condition.
Participants describe the lack of ability (or the employer's perception of employee's abilities) to perform job duties means that they cannot work. Participants also state that this renders insurance coverage beyond the financial capabilities of Marshallese households because employer sponsored health insurance is not an option if you cannot get hired. Lack of insurance limits a person's ability to manage chronic illnesses, therefore limiting their ability to become healthy enough for employment.
One Marshallese elder states that due to the health issues they developed as a result of nuclear radiation exposure they had to quit their job, and then could not afford their insurance premiums.
I was afraid that I'm gonna bleed while I'm on the line... [so], I would go into the bathroom every 20 minutes to
take care of that. I quit working. They told me that I was eligible for social security or disability or whatever, and
I've been trying to apply...I turned 60 yesterday. I don't have nothing. I lost my insurance. Whenever I quit
working, my insurance went up to $400.00 a month, which I couldn't afford. I dropped all that.
The precariousness of a full-time designation for some employees can make access to insurance programs fleeting. One participant describes that "now that they already cut (hours of employment) and I don't have (work for) 8 hours. But work 4 hours. I lost my insurance." Participants state that the difficulty of maintaining health coverage constrains their ability to manage their disease.
Policy
Current federal health policy limits access to insurance for the Marshallese COFA migrants residing in the United States. The passage of the Personal Responsibility and Work Opportunity Reconciliation Act of 1996 (PRWORA) made COFA migrants ineligible for federally-funded benefits programs, including Medicaid. PRWORA excluded COFA migrants from the category of "qualified immigrants [27]." Despite this, COFA migrants are still required to carry insurance through the Affordable Care Act (ACA). COFA migrants do qualify for income-dependent subsidies. However, these subsidies are based upon a higher income level than most Marshallese have and may not be enough to place insurance premiums within the financial means of most Marshallese households.
Throughout each focus group, participants discuss the lack of access to Medicaid and Medicaid Expansion. They stated that because of the lack of access to Medicaid and Medicaid Expansion under the ACA, many Marshallese residents of the United States do not have access to adequate insurance coverage or health care.
Focus group participants note that there are very few Marshallese who have consistent access to insurance, with some Marshallese estimating that only 20% to 30% of the community are covered by some form of insurance. This is discussed as a life-or-death issue for members of the community. One participant identifies that "we Marshallese have to figure out a way to better our lives because most of us have no medical insurance to seek medical care and I am one that have real high diabetes, I think I would have died (without some access to care)."
Discussion
The Marshallese community suffers from diabetes at rates that are more than 400% higher than the general US population [4-6], and the disease is poorly managed within the population. Most intervention efforts to improve diabetes self-management behaviors are focused on individual behaviors (individual level) [28]. Much research examines the efficacy of self-management interventions, and diabetes self-management education results in improved health outcomes and reduced costs [29], but improvements are not achieved equally in all populations [30]. The Social Ecological Model provides a framework for understanding environmental elements that affect a person's health at the organizational, community, and policy level. There is emerging evidence that ecological factors at the organizational, community, and policy levels can create systems of structural inequality for minority and low socioeconomic communities [31].
Through this research, participants identify barriers at organizational, community, and policy levels that constrain efforts to achieve diabetes self-management. For example, patients are instructed to eat nutritionally dense food and avoid processed carbohydrates and fatty meats. However, because the Marshallese are often employed at low-wage jobs, and one worker often supports many in the household, they cannot afford healthy foods. The foods they can afford and the ones provided at local food pantries are primarily processed carbohydrates and fatty, canned meats. To self-manage diabetes, patients are instructed to see their doctor regularly, take their medications as prescribed, and monitor their glucose twice per day. However, exclusion from Medicaid means many Marshallese are left without insurance. The lack of insurance means they cannot afford to see the doctor, purchase their medication, or obtain glucometer strips. Because of these barriers, many Marshallese patients report that they receive sporadic care. This lack of care may result in emergency room visits when chronic conditions reach a severe state.
Transportation issues, such as the lack of public transportation, the necessity to purchase a car, and the need to obtain a driver's license, affect all areas of self-management. Even for households that have access to a car, the driver's license test is not offered in Marshallese, and many Marshallese drivers are unable to pass the test. This leaves entire households without transportation to go to the store for healthy food or go to the doctor and pharmacy.
Language barriers remain for those who overcome transportation and insurance barriers. Marshallese speakers are often unable to understand treatment instructions because there are no staff members who speak Marshallese to translate the doctor's orders, and patient materials are also not provided in Marshallese. The participants also perceive their treatment by health care providers as being discriminatory and unequitable.
Employment issues for the Marshallese include limited access to both full-time employment and access to employer-subsidized insurance programs. Marshallese households experience barriers to health care due to part-time employment and variable weekly hours. This precludes workers, and their extended families, from accessing employer subsidized insurance, and from having funds necessary to pay for healthy food, doctors' visits, or medication.
These ecological factors create a web of barriers that prevent Marshallese diabetes self-management behavior. It is evident that to achieve improvement in diabetes self-management, we must move beyond individual-level interventions and address barriers at the community, organizational, and policy level.
Recommendations for practice and policy
At the organizational level, health care providers can offer translated patient materials in the Marshallese language and hire Marshallese health workers to provide oral translation. At the same time, it is important for health professionals to ensure culturally appropriate translations of medical concepts. Additionally, local health care providers should conduct internal reviews of policies regarding Marshallese patient experiences to find ways to improve patient care and experiences. Health care providers should also provide all employees with Marshallese cultural awareness training.
To address community level barriers, the inadequacy of transportation and healthy food options in the area must be addressed. It is necessary that local communities invest in public transit. In addition, agencies responsible for drivers' licensing and vehicle registration should translate policies and materials into Marshallese. Food pantries should implement healthy food donation polices, which would allow them to distribute healthier food choices. Employer-subsidized insurance plans should be made more accessible to Marshallese employees through increased options for consistent, full-time status. In addition, employers should also consider increasing insurance subsidies to ensure that Marshallese employees can afford insurance plans. Full-time employment would also provide other benefits to the community, such as income to purchase healthy foods and necessary medications for the household. Additionally, providing more education to employees concerning their health benefits, particularly translated into Marshallese, is also essential to facilitate Marshallese access to these programs.
At a policy level, Medicaid should be restored for COFA migrants through amendment of PRWORA to include them within the category of qualified immigrants. Marshallese were eligible for Medicaid when they agreed to the COFA; however, they were left out when PRWORA's definition of qualified immigrants did not include COFA migrants [32]. Bills have been introduced in the US House of Representatives and the US Senate to restore Medicaid coverage for COFA migrants lawfully residing in the United States by amending Title IV of the PRWORA. If approved, this would restore Medicaid for the Marshallese and provide other eligible COFA migrants with Medicaid (Table 3).
![]()
Table 3: Recommendation for Policy and Practice
View Table 3
Limitations and Strengths
The data for this study was derived from numerous focus groups where the primary purpose was the elicitation of information related to personal and interpersonal level beliefs and barriers to health care and diabetes self-management. The fact that these environmental level concerns emerged is both a strength and a limitation to the design. While the studies were not constructed to elicit information about the environmental context of health and diabetes self-management, the CBPR approach requires that we disseminate the full results of the focus groups. This study allows the voices of participants and their lived experiences to be documented and published. An additional limitation is the convenience sample, which reduces the generalizability of the results. Despite these limitations, this study provides insight into the environmental barriers to diabetes self-management for the Marshallese and provides recommendations for addressing those barriers.
Conclusion
Using the Social Ecological Model as a framework, this research provides an analysis of Marshallese health that expands the traditional diabetes self-management perspective. Understanding of environmental barriers is necessary to support patients in their self-management efforts. Researchers, health care providers, and policy makers have the challenge of addressing these environmental barriers, along with providing culturally appropriate self-management education in their efforts to reduce diabetes disparities within the Marshallese population.
Ethical Statement
Each of the study's procedures for the focus group were reviewed and approved by the University of Arkansas for Medical Sciences Institutional Review Board.
Acknowledgement
*Research was conducted at the University of Arkansas for Medical Sciences Northwest, 1125 North College Ave, Fayetteville, AR 72703, USA. Acknowledgements: This work was supported by the University of Arkansas for Medical Sciences Translational Research Institute (TRI) under Grant [UL1TR000039], which is funded through the NIH National Center for Research Resources and National Center for Advancing Translational Sciences.
Conflicts of Interest
The authors have no conflict of interest to disclose.
References
-
Center for Disease Control and Prevention (2013) CDC Health Disparities and Inequalities Report-United States, 2013.
-
Kurian AK, Cardarelli KM (2007) Racial and ethnic differences in cardiovascular disease risk factors: a systematic review. Ethn Dis 17: 143-152.
-
Rocca WA, Boyd CM, Grossardt BR, Bobo WV, Finney Rutten LJ, et al. (2014) Prevalence of multimorbidity in a geographically defined American population: patterns by age, sex, and race/ethnicity. Mayo Clin Proc 89: 1336-1349.
-
Yamada S, Dodd A, Soe T, Chen TH, Bauman K (2004) Diabetes mellitus prevalence in out-patient Marshallese adults on Ebeye Island, Republic of the Marshall Islands. Hawaii Med J 63: 45-51.
-
Aitaoto N, Ichiho HM (2013) Assessing the health care system of services for non-communicable diseases in the US-affiliated Pacific Islands: a Pacific regional perspective. Hawaii J Med Public Health 72: 106-114.
-
Blackwell DL, Lucas JW, Clarke TC (2014) Summary health statistics for U.S. adults: national health interview survey, 2012. Vital Health Stat 10: 1-161.
-
United States Census Bureau (2010) 2010 Census Interactive Population Search.
-
McElfish PA, Hallgren E, Yamada S (2015) Effect of US health policies on health care access for Marshallese migrants. Am J Public Health 105: 637-643.
-
Jimeno R (2013) A Profile of the Marshallese Community in Arkansas, Volume 3. In: Little Rock AR and Fayetteville AR, University of Arkansas.
-
Barker H (2012) Bravo for the Marshallese: Regaining Control in a Post-Nuclear, the case of Marshallese Post-Colonial World. (2nd ed), Cengage Learning.
-
Adams W, Heotis P, Scott W (1989) Medical Status of Marshallese Accidentally Exposed to 1954 Bravo Fallout Radiation: January 1985 through December 1987. Washington, DC: United States Department of Energy.
-
Reddy R, Shehata C, Smith G, Maskarinec GG (2005) Characteristics of Marshallese with Type 2 Diabetes on Oahu: A Pilot Study to Implement a Community-Based Diabetic Health Improvement Project. Calif J Health Promot 3: 36-47.
-
Yamada S, Palafox N (2001) On the biopsychosocial model: the example of political economic causes of diabetes in the Marshall Islands. Fam Med 33: 702-704.
-
Hallgren EA, McElfish PA, Rubon-Chutaro J (2015) Barriers and opportunities: a community-based participatory research study of health beliefs related to diabetes in a US Marshallese community. Diabetes Educ 41: 86-94.
-
Hodge AM, Dowse GK, Zimmet PZ, Collins VR (1995) Prevalence and secular trends in obesity in Pacific and Indian Ocean island populations. Obes Res 3 Suppl 2: 77s-87s.
-
McElfish PA, Kohler P, Smith C, Warmack S, Buron B, et al. (2015) Community-Driven Research Agenda to Reduce Health Disparities. ClinTranslSci 8: 690-695.
-
McElfish PA, Bridges MD, Hudson JS, Purvis RS, Bursac Z, et al. (2015) Family Model of Diabetes Education With a Pacific Islander Community. Diabetes Educ 41: 706-715.
-
McElfish PA, Hallgren E, Henry LJ, Ritok M, Rubon-Chutaro J, et al. (2016) Health Beliefs of Marshallese Regarding Type 2 Diabetes. Am J Health Behav 40: 248-257.
-
American Association of Diabetes Educators (2013) Technical Review: Diabetes Self-Management Education and Training (DSME/T) Outcomes and Measures.
-
Nagelkerk J, Reick K, Meengs L (2006) Perceived barriers and effective strategies to diabetes self-management. J AdvNurs 54: 151-158.
-
Rodriguez KM (2013) Intrinsic and extrinsic factors affecting patient engagement in diabetes self-management: perspectives of a certified diabetes educator. ClinTher 35: 170-178.
-
McLeroy KR, Bibeau D, Steckler A, Glanz K (1988) An ecological perspective on health promotion programs. Health Educ Q 15: 351-377.
-
Minkler M (1999) Personal responsibility for health? A review of the arguments and the evidence at century's end. Health EducBehav 26: 121-140.
-
Stokols D (1996) Translating social ecological theory into guidelines for community health promotion. Am J Health Promot 10: 282-298.
-
Glasgow RE (1995) A practical model of diabetes management and education. Diabetes Care 18: 117-126.
-
Sallis J, Owen N, Fisher E (2008) Ecological Models of Health Behavior. Health Behvaior and Health Education: Theory, Research, and Practice. John Wiley & Sons.
-
U.S. (1996) Government Printing Office. 104th Congress Public Law 193.
-
Funnell MM, Brown TL, Childs BP, Haas LB, Hosey GM, et al. (2009) National standards for diabetes self-management education. Diabetes Care 32 Suppl 1: S87-94.
-
Powers M, Bardsley J, Cypress M, Duker P, Funnell MM, et al. (2015) Diabetes self-management education and support in type 2 diabetes: A joint position statement of the American Diabetes Association, the American Association of Diabetes Educators, and the Academy of Nutrition and Dietetics. J AcadNutr Diet 115:1323-1334.
-
Anderson D, Christison-Lagay J (2008) Diabetes self-management in a community health center: Improving health behaviors and clinical outcomes for underserved patients. Clin Diabetes 26:22-27.
-
Geronimus AT (2000) To mitigate, resist, or undo: addressing structural influences on the health of urban populations. Am J Public Health 90: 867-872.
-
Singer A (2004) Welfare Reform and Immigrants: A Policy Review. In: Kretsedemans P, Aparicio A, eds. Immigrants, Welfare Reform, and the Poverty of Policy. Westport, CT: Praeger Publishers.