Evidences reveal that bellow half of asthma patients are adherent to their medications. Striving for improved adherence and asthma control is of vital concern in today's asthma management. In a recent document, the world health organization recognized lack of adherence as a major problem in management of chronic disease and concluded that improving adherence would have more beneficial impact on health outcome than improving specific treatment. But, study findings addressing its magnitude and associated factors are lacking in the country and hence current study was aimed to assess level of treatment adherence and factors affecting among asthmatic patients in Soddo Christian General hospital, from July to August, 2017.
A facility based cross-sectional study design was used. Data was collected through structured questionnaire to collect information on socio-demographic, socio-economic and information on medication adherence and disease related factors. Completeness of the data was checked every day and cleaned and analyzed. Descriptive analysis was computed as frequency, mean and standard deviation (SD) for continuous variables and for categorical data. The out puts of different study findings was presented using tables, graphs, & figures accordingly.
Among 106 patients participated in the study, 62 (59%) were males and majority of the respondents found within age range of 36-45, 36 (34%). It was found that 139 (59%) of asthmatic patients had poor adherence for which the most common factors affecting adherence were, forgetting to take the drug 25 (23.5%) and being busy with other tasks 18 (17%). Majority (79%) of asthmatic patients reported as they use alternative methods as means of treatment.
The level of adherence to asthma medication was relatively lower when compared to others studies done in developing countries. The major reasons for missing doses were simple forgetfulness, absences of clear drug information and being busy with other things. Hence, health care providers especially pharmacists should provide accessible information to patients on their treatment plan to ensure patients keep their regular follow up, improve their patient's confidence and to avoid drug abuse.
Adherence, Asthma, Christian hospital, Sodo
ADR: Adverse Drug Reaction; NIH: National Institutes of Health; SCGH: Christian General hospital; SNNPRS: South Nations Nationalities and People Region States; WHO: World Health Organization
As defined by the World Health Organization (WHO) "bronchial asthma is a respiratory disorder, characterized by recurrent attacks of breathlessness and wheezing, usually of allergic origin, which varies in severity from person to person". Asthma is a disease that is characterized by the spontaneous occurrence of attacks of breathlessness and wheezing, usually at night. The condition occurs with varying severity over a period of several years and sometimes throughout life. With good management the symptoms may diminish and even disappear [1-3].
Despite the availability of highly effective pharmacotherapy, poorly controlled asthma is reported in up to 70-95% of patients in developed and developing countries. Among other factors, poor compliance and knowledge of asthma medication and poor adherence towards regular control visits are explanations for this suboptimal control. Although, the most effective long-term control medicines available are inhaled corticosteroids, a recent national survey in USA showed that four out five people with chronic asthma are not using these medicines. Inadequate compliance with prescribed medication can lead to failure of treatment, excessive use of medication, unnecessary costs, life-threatening exacerbations, and ultimately death [4,5].
Adherence to treatment does not refer simply to the act of taking the medications; rather, it refers to how the person manages their treatment in relation to doses, times, frequency and duration. In the context of chronic illnesses, in which the people and their relatives are responsible for the greater part of the care, adherence must be seen as a joint activity in which the person not only follows medical advice, but understands, agrees with and adopts the regimen described. Adherence to long-term therapy refers to the extent to which a person's behavior - taking medication, following a diet, and/or executing lifestyle changes, corresponds with agreed recommendations from a health care provider [6,7].
Ordinarily, the word compliance refers to taking the correct dose of prescribed medication at the correct intervals. Compliance can be either unintentional or intentional. The reason for unintentional non-compliance may be inadequate instructions or a regimen that is too complex or time consuming. Inadequate training in inhalation technique often causes non-compliance despite the best intentions. Lack of understanding about the need for long-term preventive treatment is another important cause of non-compliance, especially when preventive medication does not produce immediate symptom relief. Compliance is used within the medical setting to define whether a patient follows a prescribed management plan in order to treat effectively an underlying illness or condition [8-10].
Despite various degrees of adherence, much of the literature continues reporting adherence as a dichotomous construct, in which patients are considered to be either adherent or not. Improved adherence to a treatment regimen for asthma in general and to inhaled corticosteroids in particular is recognized as an important factor in asthmatic patients' reduced morbidity, utilization of healthcare resources and mortality [11,12]. Studies have shown that less than 50% of asthma patients are adherent to their asthma medications. Striving for improved adherence and asthma control is of vital concern in today's asthma management. In a recent document, the world health organization recognized lack of adherence as a major problem in management of chronic disease and concluded that improving adherence would have more beneficial impact on health outcome than improving specific treatment [13].
The absence of adherence measures in health care contributes to costly asthma outcomes and poor quality control. Multiple studies have shown that medication adherence decreases as the number of medications prescribed, the dosing frequency, and the duration of treatment increase [14,15]. Therefore, current study was aimed to assess the level of medication adherence and to identify factors that affect it among asthmatic patients in Soddo Christian General hospital, Southern Ethiopia.
As revealed by the literatures, the success of any medical regimen prescribed for a particular patient often depends, in large part, on three factors: the patient's knowledge regarding the illness, which enables him/her to take appropriate action to control particular symptoms, the patient's attitude toward the illness, including his or her willingness to work with the physician to manage the disorder and the patient's confidence in his or her ability to contribute to the management of the illness. Many patients are reluctant to inform their providers that they did not follow medical instructions. Because no objective adherence measures are available for practicing physicians, clinicians must rely on the "honor system", which often leads to inaccurate diagnostic and therapeutic decisions. Without objective adherence measures, physicians must rely on a more detailed medication history to evaluate adherence. Short-term studies have documented that open ended communication, careful interviewing and active listening can improve medication use [16].
Therefore, the findings of this study can be used as an input for policy makers to up to date treatment guidelines and to provide trainings for healthcare professionals, will help to know the prevalence, factors affecting medication adherence among asthmatic patients, can point out areas need to be focused in health care plans of the hospital, and will serve as base line for further studies or serve as secondary data for other studies as there is lack of studies on this topic in the country in general and in Wolaita Zone in particular.
The study was carried out among patients with asthmatic patients at Soddo Christian General Hospital (SCGH). Soddo Christian General Hospital is found in Southern Nations Nationalities and People Region States (SNNPRS), Ethiopia. The hospital is located in Soddo town of Wolaita Zone, SNNPRS which is 380 km away from the national capital Addis Ababa and 170 km far from the regional capital Hawassa. The study was conducted from June to July, 2017.
Study design: A facility based cross-sectional study design was used.
Source population: All asthmatic patients who visit Soddo Christian General Hospital for their chronic care follow up.
Study population: Asthmatic patients who came to the hospital during data collection and who fulfill the inclusion criteria.
Inclusion criteria: Asthmatic patients who are on their follow up and have been using ant-asthmatic medications and age above 15 years.
Exclusion criteria: Unwilling, and patients with psychiatric problems were excluded from the study.
The adult asthmatic patients coming to the hospital for their regular following were approached for interview. Accordingly, there were 106 asthma patients on medication those interviewed during the specified data collection period.
Sampling procedure: The asthmatic patients who fulfil eligibility criteria were consecutively include in the study until the calculated sample size was attained.
Data collection procedures: Data was collected through structured questionnaire which will be translated to the local language for patient interview to collect information on socio-demographic, socio-economic and information on medication adherence.
Methods of data analysis: Completeness of the data was checked every day and cleaned and analyzed. Descriptive analysis was computed as frequency, mean and standard deviation (SD) for continuous variables and for categorical data. The out puts of different study findings was presented using tables, graphs, & figures accordingly.
Formal letter was obtained from Paradise Valley University and given to the hospital .There was also a written consent taken so that the patients agreed to give his/her medical information. Patients were assured that lack of willingness to involve in the study could not affect the service they get from the hospital. To ensure patient confidentiality, name and address of the patient was recorded in the data collection format. The patients was clearly informed that that his/her medical information would not be disclosed to any external subjects/media.
• Asthma: "Bronchial asthma is a respiratory disorder, characterized by recurrent attacks of breathlessness and wheezing, usually of allergic origin.
• Treatment adherence: Is defined as a manner in which a given patient takes his/her prescribed medications according to the instruction given by the health care provider.
• Comorbidity: Any chronic disease the patient has together with asthma for he/she is taking medications.
• Social drug use: Any habit of chewing chat, smoking cigarette, drinking alcohol.
Among 106 patients participated in the study, 62 (59%) were males and majority of the respondents found within age range of 36-45, 36 (34%) followed by 26-35, 25 (24%). It was also found that most of study participants were married 61 (57.6%), in case of their religion, they were protestant religion followers 46 (43%), and in ethnicity, there was Wolaita ethnicity predominance which accounted 61 (60%).
As per the respondents' educational status, majority attended secondary school, 40 (38%), followed by those who dropped out from elementary schools 27 (25.3%). Majority of study participants were found to be merchants 44 (41.3%) and employees which accounted 31 (29.2%).
The study has found that majority, 88 (83%) of asthma patients on follow up were urban dwellers.
More than one fourth, 34 (32%) of total asthmatic patients reported as they had family history of asthma (Table 1).
Table 1: Socio-demographic characteristics of asthmatic patients at Soddo Christian General Hospital, 2017 [N = 106]. View Table 1
As depicted in the figure below, this study also collected data on social drug use and found that 23 (21.6%) reported as they have habit of smoking cigarette, 30 (28.4%) chew chat. However, study participants those reported as drinking alcohol accounted a greater proportion which was 41 (38.6%) (Figure 1).
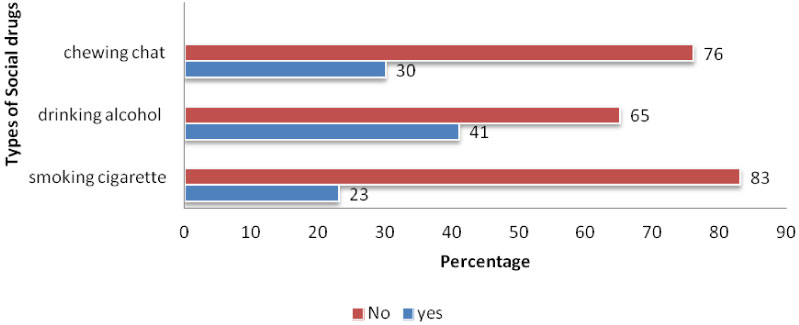 Figure 1: Prevalence of social drug use among study participants, June-July 2017, N = 106. View Figure 1
Figure 1: Prevalence of social drug use among study participants, June-July 2017, N = 106. View Figure 1
It was found that most of asthmatic patients reported that they have 5-10 years, 35 (33.1%) followed by those stayed for 1-5 years after starting the medication, 28 (26%).
Of the total participants, 64 (60.4%) responded as they were admitted due to asthma exacerbation while on treatment which could probably be a clear indication for low level of medication adherence among these populations.
Out of the total, infectious diseases, 25 (23.6%) were predominant comorbidities followed by hypertension, 20 (13%) which were the most frequent.
According to patients' knowledge on aggravating and relieving factors, the most common disease aggravating factors or conditions reported were smells, 23 (21.6), drugs 21 (19%), dusts and weather conditions, 41 (20.4%). Similarly, taking bronchodilator drugs, 64 (60%) was the major disease relieving factor at the time of exacerbation as reported by the respondents (Table 2).
Table 2: Disease related variables of asthmatic patients at Soddo Christian General Hospital, June-July 2017 [N = 106]. View Table 2
Data indicates that majority, 63 (62.7%) were using bronchodilators most commonly salbutamol followed by combination of bronchodilators with anti-inflammatory (corticosteroids) 22 (20.3%) (Figure 2). It was also found that anti invectives 27 (26%), cardiovascular drugs 20 (18%) and pain killers 26 (24.5%) were the most common concurrently taken medications by asthmatic patients at the hospital. Majority, 35 (34.8%) of patients were taking two pills per day and about 79% were using alternative treatment methods for asthma treatment along with modern drugs (Table 3).
Table 3: Medication related information asthmatic patients at Soddo Christian General Hospital, June-July 2017 [N = 106]. View Table 3
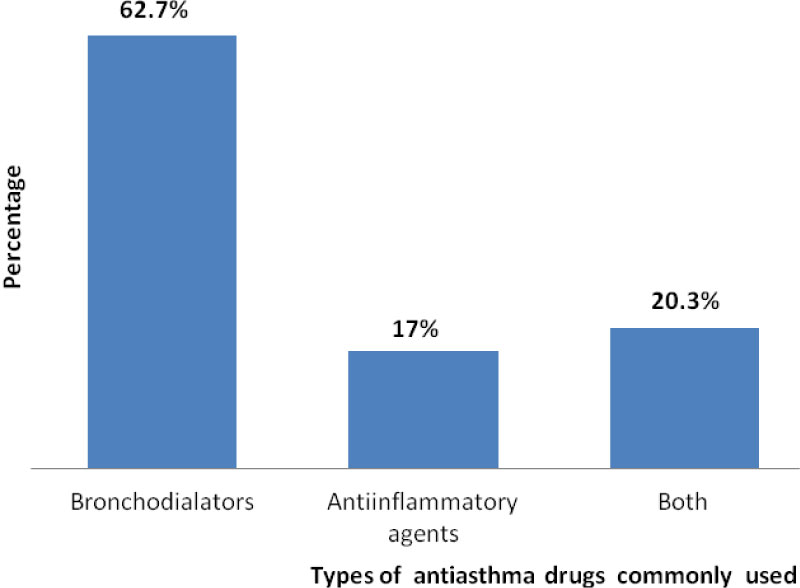 Figure 2: Types of antiasthma drugs commonly used among asthmatic patients at Soddo Christian General Hospital, June-July 2017 [N = 106]. View Figure 2
Figure 2: Types of antiasthma drugs commonly used among asthmatic patients at Soddo Christian General Hospital, June-July 2017 [N = 106]. View Figure 2
Additionally, treatments other than antiasthma drugs, about half of asthmatic patients reported as they use religious methods as means of alternative treatment (Table 3).
As depicted in the tables, more than half of the patients 60 (59.2%) reported that they missed their dose, indicating as there is non-adherence to their asthma treatment. For their non-adherence the most common factors affecting were, forgetting to take the drug 25 (23.5%), being busy with other tasks 18 (17%) and unclear information from the health care providers about the drugs and their side effects 14 (13.2%) (Table 4).
Table 4: Information on medication adherence and perceived reasons among asthmatic patients at Soddo Christian General Hospital, June-July 2017 [N = 106]. View Table 4
As indicated in Figure 3 above, majority of asthmatic patients were found to have poor medication adherence, 59% but only 11% of the patients identified as they have high adherence.
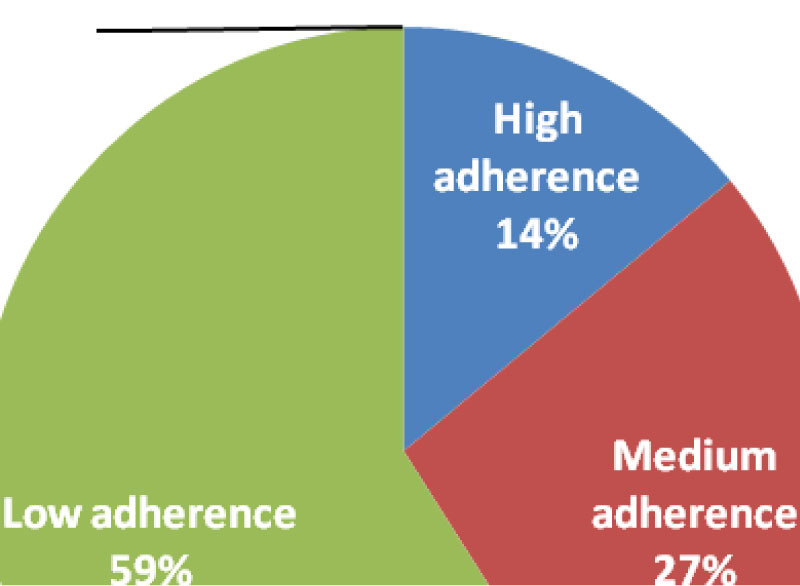 Figure 3: Level of Medication Adherence among asthmatic patients at SCGH, N = 106. View Figure 3
Figure 3: Level of Medication Adherence among asthmatic patients at SCGH, N = 106. View Figure 3
For adequate management of asthma, the use of multiple medications is required at different times during the course of the disease and hence increasing patients' medication adherence is vital to optimal asthma management. Good medication adherence levels optimize health outcomes and minimize unwanted drug effects, disease progression and health care costs. Non-compliance to treatment program is more common than usually suspected (20% to 80%) in patients with asthma and other chronic conditions [14]. Nevertheless, rates of noncompliance are hard to come by because patients do not accurately report and physicians often do not enquire critically.
In this study 62 (59%) were males and majority of the respondents found within age range of 36-45, 36 (34%) followed by 26-35, 25 (24%) which is similar with study conducted in India [17]. This study has found that majority of asthmatic patients had poor adherence, 139 (69%). This result is surprisingly consistent with adherence study by Gajanan S. Gaude in India. But it is much higher than the one conducted in Iran, with the possible reasons being difference in socio-economic status of the population, study design difference and the likes.
It was found that the most common factors affecting adherence were forgetting to take the drug 49 (24.5%), being busy with other tasks 38 (19%) and unclear information from the health care providers about the drugs and their side effects 29 (14.5%). This finding is in agreement with an adherence study in elsewhere which found that the main reasons for missing doses were forgot to take drugs 8 (36.4%), away from home 5 (22.7%) and being busy with other things 4 (18.2%) [15].
However, the overall adherence level in current study is much lower than that of the previous one which could possibly be due to sociocultural, economic, religious and other study design related differences. Additionally, absence of ward based clinical pharmacy service in the current hospital and absence of pharmacy drug counseling may also contribute to the high level of non-adherence among asthmatic population. The present study found that forgetfulness was the most frequently claimed reason for missing doses, which is similar with study findings reported in elsewhere in which the main (38%) reason for missing therapy were being busy and forgetting. Similarly, other studies reported that forgetting was the main reason for missing doses in addition to other reasons like being busy and away from the home [16,16].
Patient self-report was used and it is subject to recall bias and overestimate adherence level. Time and budget constraints may are also one hindering factors for the study. Because of cross-sectional nature of the study, it did not allow the cause-effect relationships between various factors and adherence to be addressed. Despite the limitation, this finding is useful for program managers to develop appropriate strategies to address the issue of adherence from both the clinician and the patient side in the hospital as well as the country at large.
In current study, the level of adherence to asthma medication was relatively lower when compared to others studies done in developing countries. This could alarm the health care providers of the hospital to give due attention in drug education and counseling. The major factors or reasons for missing doses were simple forgetfulness, absences of clear drug information and being busy with other things.
Based on the findings of the study, the following recommendations were forwarded to the hospital, health care providers, and other concerned bodies.
⇒ The hospital should construct a better care plan incorporating adequate drug education as main component of asthma management.
⇒ All health care providers taking care of asthma patients should monitor their adherence to prescribed medication in regular basis.
⇒ Health care providers especially pharmacists should provide accessible information to patients on their treatment plan to ensure patients keep their regular follow up, improve their patient's confidence and to avoid drug abuse.
⇒ The clinicians need to improve relationship with their patients and counsel their patients on the regular follow up of the appointments and avoiding drug abuse.
⇒ Finally, further study should be done with inclusion of different adherence measures and advanced statistical tests using large sample size.
None declared.
The authors are grateful to W/ro Birtukan Ermias, Blen Hailu and Grace Hailu, for their unreserved support throughout the study. Finally, Sodo Christian General hospital staffs and the study participants are also acknowledged for their cooperation during data collection.
TC participated in designing, conception and analysis of the paper as his partial fulfillment for requirement of his bachelor degree in Pharmacy. HC participated in designing, interpretation, analysis and writing up of the manuscript.