International Journal of Neurology and Neurotherapy
A Combinatory Therapy Continuously Improves Memory in a Case of Probable Alzheimer's Disease with Head Trauma for Nearly Two Years
Jing Shi#, Xuekai Zhang#, Mingqing Wei, Jingnian Ni, Ting Li Mphil and Jinzhou Tian*
BUCM Neurology Centre, Dongzhimen Hospital, Beijing University of Chinese Medicine, China
#Equally contributed
*Corresponding author:
Jinzhou Tian, MD, Ph.D, BUCM Neurology Centre, Dongzhimen Hospital, Beijing University of Chinese Medicine, Beijing 100700, China, E-mail: jztian@hotmail.com
Int J Neurol Neurother, IJNN-3-062, (Volume 3, Issue 6), Case Report; ISSN: 2378-3001
Received: August 10, 2016 | Accepted: November 28, 2016 | Published: December 05, 2016
Citation: Shi J, Zhang X, Wei M, Ni J, Mphil TL, et al. (2016) A Combinatory Therapy Continuously Improves Memory in a Case of Probable Alzheimer's Disease with Head Trauma for Nearly Two Years. Int J Neurol Neurother 3:062. 10.23937/2378-3001/3/6/1062
Copyright: © 2016 Shi J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Since the worldwide demographic ageing, prevalence of the most common cause of dementia in the elderly, Alzheimer's disease (AD), will increase dramatically. Although it has been intensively researched for many years, there are still limited treatments for AD. Currently approved pharmacotherapy is generally considered have symptom-relieving rather than disease processing modifying effects. Meanwhile, there are efficacy limits of such medicines, for example, donepezil efficacy starts to decline from the peak in 3 month and gradually drop below the baseline in 9 months in patients. Thus, how to improve cognitive function beyond this limitation is a worldwide challenge. With our clinical experience, we propose a combinatory therapy of ChEI and herbal medicines for it. Here is a report of a 65-year-old man with moderate probable AD with head trauma. He has been improved slowly by the combinatory therapy at cognitive function and global status nearly two years, from 18 scores on MMSE at his first visit to 21 scores at final visit.
Keywords
Alzheimer's disease, Combined therapy
Introduction
As the worldwide demographic ageing, prevalence of the most common cause of dementia in the elderly, Alzheimer's disease (AD), will increase dramatically. AD currently affects about 8.2/1000 person-years in China [1]. Although it has been intensively researched for many years, there are still limited treatments for AD. Currently approved pharmacotherapy include three cholinesterase inhibitors for mild to moderate patient and one N-methyl D-aspartate receptor antagonist for moderate to severe patient. These well studied treatments for AD are generally considered have symptom-relieving rather than disease processing modifying effects [2,3]. And there is a phenomenon that the single use of ChEI or the combined use ChEI and NMDA antagonist may reach peak effects in 3 months, while drop below the baseline in 9 months [4-5]. Although we still do not know whether this is the efficacy of the drug recession or the body's resistance build up to the inflection point [6], it is a kind of AD treatment bottleneck. Thus, we propose a hypothesis to break this bottleneck through a combinatory therapy of ChEI or/and NMDA receptor antagonist with herbal medicines included active ingredients associated with increase efficacy and anti-resistance. This hypothesis was evidenced by a large number of cases in our clinical practice. Following is a representative case treated by our combinatory therapy.
Patient Information
WQR a retired linguistic teacher, who was born on April 5th 1949. He was brought to our memory clinic on 2014 for consideration of gradual cognitive decline in three years, and deteriorated in two months after a head trauma (ID is 4442991 in our outpatients system). Since second half year of 2011, he insidiously got memory decline, which is characterized by asking the same question repeatedly, call the same person on the phone several times in a day, he also has difficulties in handling common daily life issues. He has been to hospital for the memory decline and took a herbal medicine with kidney boosting function for about half year, his memory got certain improvement. He got a sudden loss of consciousness when looking up, and fell down to the ground with head trauma on February 2nd 2014. He has had right side occipital bone fractures with soft tissue injury, brain contusion, subarachnoid hemorrhage, subdural hematoma, with careful brain dehydration and protection, as well as nutrition support treatment, he regain conscious after three days. However, he has had neuropsychological psychiatric and behavioral disturbances, like talk to himself, irritability, delusions as well hallucinations since then. He has no obvious personal and family history related to dementia. He also has no relevant sign in his physical examination and neurologic examination. No significant abnormality in his laboratory tests.
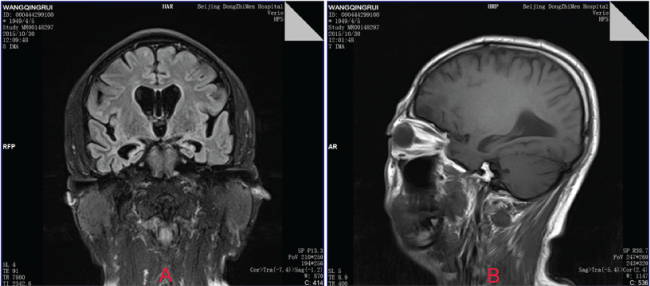
His cranial MRI showed severe atrophy of the bilateral hippocampal volume, and slight distended lateral ventricles (Figure 1).
.
Figure 1: MRI imaging findings.
Note: A) Coronal FLAIR showed severe atrophy of the bilateral hippocampal volume, and slight distended lateral ventricles, Right MTA = 4 Left MTA = 3, Global cortical atrophy (GCA) scale = 1. B) Sagittal FLAIR also showed atrophy of the bilateral hippocampal volume.
View Figure 1
His neuropsychological assessment in the first visit on April 17, 2014 revealed that he has significant decrease in global cognition, delayed episodic memory, severe decrease of daily living activities, anxiety, psychiatric and behavior symptoms, like irritability, delusions as well hallucinations. He has no obvious depression, (Table 1.). According to above information, the case was diagnosed as moderate dementia, probable Alzheimer disease with head trauma according to the AD criteria of International Working Group and the US National Institute on Aging-Alzheimer's Association).
![]()
Table 1: Neuropsychological assessments in two years time.
View Table 1
He received our combinatory therapy after diagnosis. The combined therapy include symptomatic medicines (Donepezil tablets 5 mg qd, po), TCM herbal therapy. The prescribed TCM herbal formula mainly include herbal decoction covering herbs with functions of boosting kidney, and clearing phlegm twice a day), which is the main ingredients of GAPT, a combination of eight herbal extracts with functions of boosting kidney, and clearing phlegm.
He got a continues improvement in cognition and steadily improvement in daily activities after nearly two years' combined therapy (Table 1). His latest neuropsychological assessment results showed that his global cognition and daily living activities were both in mild dementia. He has no obvious depression, anxiety, psychiatric and behavior symptoms. Overall results indicate he pertains to mild dementia at the moment. His psychiatric and behavioral symptoms, like talk to himself, irritability, delusions as well hallucinations was disappears. The good outcomes of receiving nearly two year's combined therapy after diagnosis was significantly higher than the expected decline of MMSE changes according to historical data (Figure 1).
.
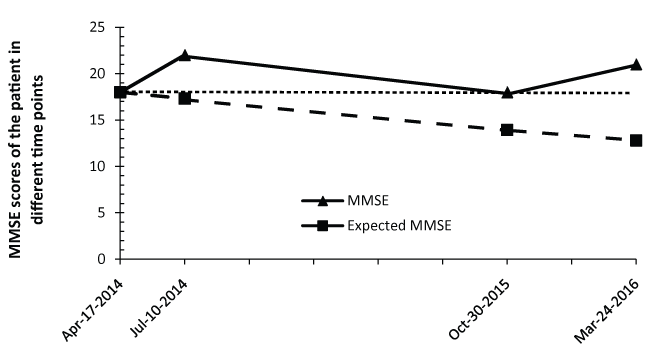
Figure 2: The MMSE changes from first visit and follow up in three, 18 and 23 months.
Note: There is a dramatic difference between observed MMSE changes and his expected decline according to a baseline-dependent mathematical MMSE prediction model published by Mendiondo, et al. His MMSE score improved to 21 [7].
View Figure 2
His neuropsychological assessment showed that his MMSE increased from 18 to 22 after three months combined therapy. Although the MMSE score fell back to 18 after 18 months, it improved steadily to 21 after 23 months. With the improvement of MMSE scores, his ADL scores also improved from 33 to 21 (The less score in ADL means better daily life activity function). His CDT improved from one to four after three months treatment. His CDR improved from three to one (The less score means slighter dementia degree). His NPI also improved from three to zero (The less score means less neuropsychological and behavioral disturbances, his severe agitation disappear after three months treatment). His performance on ISR, DSR, HAMD and HAMA kept relatively stable.
Discussion
As far as the diagnosis of the patient concerned, he was diagnosed as probable AD with head trauma for the following reasons. First, although the patient had deteriorated after head trauma, he had insidious and progressive cognitive decline before the head accident in three years without fluctuating character. Second, he has more than two domains of cognitive impairment (memory loss and decreased calculation, comprehension, judgment and clumsy response). His CDR was three and ADL score is 33, which is quite beyond the 16 (he cannot use household appliances and has difficulties in dressing, and need instructions in eating and grooming) and the cognitive impairment has interfered with her daily activities [7-8]. Third, his brain MRI showed severe atrophy of the bilateral hippocampal volume and slight distending of bilateral ventricles. Thus, he was finally diagnosed as moderate probable AD [9-11]. Other diseases that cause cognitive impairment were excluded by the patient's negative results of laboratory tests.
The good outcomes of receiving nearly two years combinatory therapy after diagnosis was quite beyond the expected decline of MMSE changes according to historical data [7]. Moreover, his psychiatric and behavioral symptoms also got significant improvement. Which may partially explained by evidences from our previous clinical trials or animal experiments of Donepezil and our herbal formula, GAPT, a combination of eight herbal extracts with functions of boosting kidney, and clearing phlegm. This GAPT have been found markedly enhance learning and memory of AD rat models induced by Aβ injection or transgenic mice of APPV717I and APPswe/PS1dE9 [12-16]. It might also indicate the complex pathogenic process of AD should be treated with multiple targets medicine or combination of multiple therapies. Well designed preclinical and clinical study may needed to investigate the effects of combinatory therapy in treating Alzheimer's disease.
References
-
Yuan J, Zhang Z, Wen H, Hong X, Hong Z, et al. (2016) Incidence of dementia and subtypes: A cohort study in four regions in China. Alzheimers Dement 12: 262-271.
-
Wilcock GK (2006) Disease-modifying treatments for Alzheimer's disease: a perspective based on experience with R-Flurbiprofen. Alzheimers Dement 2: 150-152.
-
Chalmers KA, Wilcock GK, Vinters HV, Perry EK, Perry R, et al. (2009) Cholinesterase inhibitors may increase phosphorylated tau in Alzheimer's disease. Journal of Neurology 256: 717-720.
-
Winblad B, Engedal K, Soininen H, Verhey F, Waldemar G, et al. (2001) A 1-year, randomized, placebo-controlled study of donepezil in patients with mild to moderate AD. Neurology 57: 489-495.
-
Tariot PN, Farlow MR, Grossberg GT, Graham SM, McDonald S, et al. (2004) Memantine treatment in patients with moderate to severe Alzheimer disease already receiving donepezil: a randomized controlled trial. JAMA 291: 317-324.
-
Dumas JA, Newhouse PA (2011) The cholinergic hypothesis of cognitive aging revisited again: cholinergic functional compensation. Pharmacology biochemistry and behavior 99: 254-261.
-
Mendiondo MS, Ashford JW, Kryscio RJ, Schmitt FA (2000) Modelling mini mental state examination changes in Alzheimer's disease. Statistics in medicine 19: 1607-1616.
-
Ni J, Shi J, Wei M, Tian J, Jian W, et al. (2015) Screening mild cognitive impairment by delayed story recall and instrumental activities of daily living. International Journal of Geriatric Psychiatry 30: 888-890.
-
Dubois B, Feldman HH, Jacova C, DeKosky ST, Barberger-Gateau P, et al. (2007) Research criteria for the diagnosis of Alzheimer's disease: revising the NINCDS-ADRDA criteria. The Lancet Neurology 6: 734-746.
-
McKhann GM, Knopman DS, Chertkow H, Hyman BT, Jack CR, et al. (2011) The diagnosis of dementia due to Alzheimer's disease: recommendations from the National Institute on Aging-Alzheimer's Association workgroups on diagnostic guidelines for Alzheimer's disease. Alzheimers Dement 7: 263-269.
-
Tian J Shi J WM, Zhang XK, Ni JN, Wang YY (2012) Chinese Characteristics of Clinical diagnostic criteria for Alzheimer 's disease 4: 2084-2087.
-
Tian J, Shi J, Zhang X, Wang Y (2010) Herbal therapy: a new pathway for the treatment of Alzheimer's disease. Alzheimer's research & therapy 2: 1-4.
-
Tian J, Shi J, Zhang L, Yin J, Hu Q, et al. (2009) GEPT extract reduces Abeta deposition by regulating the balance between production and degradation of Abeta in APPV717I transgenic mice. Current Alzheimer research 6: 118-131.
-
Shi J, Zhang X, Yin L, Wei M, Ni J, et al. (2016) Herbal formula GAPT prevents beta amyloid deposition induced Ca2+/Calmodulin-dependent protein kinase II and Ca2+/Calmodulin-dependent protein phosphatase 2B imbalance in APPV717I mice. BMC complementary and alternative medicine 16: 159.
-
Shi J, Tian J, Zhang X, Wei M, Yin L, et al. (2012) A combination extract of ginseng, epimedium, polygala, and tuber curcumae increases synaptophysin expression in APPV717I transgenic mice. Chinese medicine 7: 13.
-
Shi J, Tian J, Zhang X, Zeng C, Wei M, et al. (2013) A combination extract of Renshen (Panax Ginseng), Yinyanghuo (Herba Epimedii Brevicornus), Yuanzhi (Radix Palygalae) and Jianghuang (Rhizoma Curcumae Longae) decreases glycogen synthase kinase 3beta expression in brain cortex of APPV7171 transgenic mice. Journal of traditional Chinese medicine 33: 211-217.





