Leprosy or Hansen's disease is an infection by Mycobacterium leprae (M. leprae), whose prevalence has considerably decreased since the application of the new anti-leprosy strategies advocated since 1982 by the World Health Organization (WHO). However, in the endemic countries several cases of leprosy are reported annually. We report a clinical case of lepromatous leprosy revealed by disseminated maculopapular lesions simulating a Sweet syndrome highlighting the importance of knowing how to evoke this diagnosis in patients from endemic areas.
Lepromatous leprosy, Rash, Sweet syndrome
Lepromatous leprosy is generally manifested by non-inflammatory lesions, hypochromic macules, and progressive erythematous papulo-nodules. We report an observation of lepromatous leprosy in a 62-year-old patient from rural Morocco who was diagnosed with maculopapular lesions.
A 62-year-old patient having a history of prostate adenocarcinoma for one year, had consulted in dermatology for disseminated erythematous skin lesions affecting the face, trunk, upper limbs and lower limbs evolving for two months. Dermatological examination revealed erythematous macular erythematous lesions on the face, papulo-nodular lesions on the face, hands and forearms (Figure 1a and Figure 1b), infiltrated lesions in the left elbow as well as annular lesions in the abdomen (Figure 2a and Figure 2b). The neurological examination showed hypoesthesia in gloves and socks, with bilateral hypertrophy of the ulnar nerve. Acid-fast bacillus test showed bacillus with bacterial index (BI) of +6. Histology favored lepromatous leprosy (Figure 3). The electromyogram revealed a sensory-motor axon polyneuropathy of the lower limbs. A multidrug therapy combining dapsone (100 mg per day), rifampicin (600 mg per month) and clofazimine (50 mg per day) was recommended and followed for 12 months. The evolution was marked by the partial disappearance of the cutaneous lesions after of treatment for two months and almost total disappearance after five months (Figure 4).
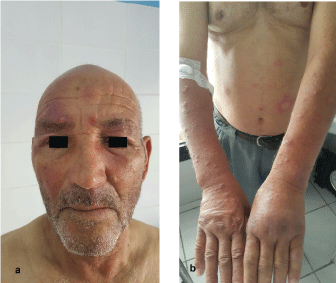 Figure 1: a) Maculopapular erythematous lesions of the face; b) Papulonodular erythematous lesions in forearms and hands. View Figure 1
Figure 1: a) Maculopapular erythematous lesions of the face; b) Papulonodular erythematous lesions in forearms and hands. View Figure 1
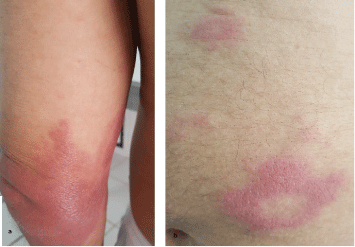 Figure 2: a) Erythematous plaque infiltrated on the left elbow; b) Annular erythematous lesions on the abdomen. View Figure 2
Figure 2: a) Erythematous plaque infiltrated on the left elbow; b) Annular erythematous lesions on the abdomen. View Figure 2
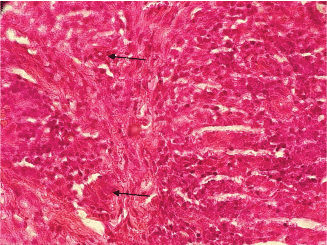 Figure 3: Inflammatory peri-adnexal and peri-nervous infiltrate in the deep dermis rich in foamy histiocytes (Hematoxylin-Eosin ×400). View Figure 3
Figure 3: Inflammatory peri-adnexal and peri-nervous infiltrate in the deep dermis rich in foamy histiocytes (Hematoxylin-Eosin ×400). View Figure 3
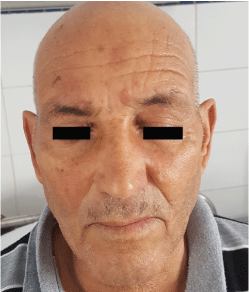 Figure 4: Total disappearance of erythematous lesions of the face after anti-bacillary treatment. View Figure 4
Figure 4: Total disappearance of erythematous lesions of the face after anti-bacillary treatment. View Figure 4
Leprosy is an infectious disease, transmissible by Mycobacterium leprae (M. leprae) or Hansen's bacillus that primarily affects skin, the mucous membranes, the peripheral nervous system, and eyes. Depending on the cellular immunity of the infected subject, different clinical forms manifest. Lepromatous leprosy, which is the multibacillary form, generally manifests by non-inflammatory lesions, hypochromic macules and normo-esthesic erythematous papulo-nodules, with progressive onset [1]. In addition to these cutaneous signs, nerves are damaged in the skin-neuritic form [2]. The search for Hansen's bacillus is by performing a skin smear examination: Tissue fluid and pulp is collected from the lobules of the ear or cutaneous lesions. That test is always positive in multibacillary forms [1,3]. The lepromatous infiltrate to the histology is generally dense respecting the papillary dermis with a peri-capillary, peri-adnexal and peri-nervous disposition. This infiltrate consists above all of foamy cytoplasm histiocytes and rare lymphocytes. Hansen's bacillus are numerous and often clustered in histiocytes and nerves [1]. Treatment requires multi-drug therapy consisting of dapsone, rifampicin and clofazimine [4].
In our patient, the diagnosis of leprosy was not obvious in front of this polymorphous clinical picture, so a paraneoplastic sweet syndrome was evoked in front of the presence of maculopapular erythematous lesions in the face and the upper limbs, seen the history of prostatic adenocarcinoma evolving for a year (cases of sweet syndrome secondary to neoplasia have been reported in the literature), nevertheless the presence of annular lesions at the abdominal level and the sensory neurological damage at the extremities made it possible to confirm the diagnosis of lepromatous leprosy. Histology confirmed the diagnosis.
This observation confirms the fact that this pathology is generally unknown in countries with low endemicity making diagnosis difficult. Interview and a complete clinical examination are crucial for early diagnosis and treatment, which is the only way to avoid long-term complications.
Leprosy is characterized by a clinical polymorphism. It is a pathology that is not yet eradicated, hence the need to discuss this diagnosis with medical personnel from endemic areas.